Abstract
Purpose
Smoking cessation has been shown to normalize the coronary endothelial dysfunction in healthy young smokers. However, its effect has not been explored in middle-aged smokers with a longer history of smoking. Therefore, we compared the effects of smoking cessation on coronary vasomotor response between both young and middle-aged smokers and identified the predictor for its improvement.
Methods
This study investigated 14 young healthy smokers (age 25.2 ± 2.3 years), 13 middle-aged smokers (age 42.0 ± 6.5 years) and 10 non-smokers. Myocardial blood flow (MBF) was measured by using 15O-water positron emission tomography (PET).
Results
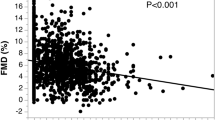
At baseline, the ratio of MBF during the cold pressor test (CPT) to that at rest (MBFCPT/rest), the index of coronary endothelial function, was significantly decreased in both young and middle-aged smokers compared to non-smokers (1.24 ± 0.20 and 1.10 ± 0.39 vs 1.53 ± 0.18, p < 0.05 and p < 0.001, respectively). The ratio of MBF during adenosine triphosphate infusion to that at rest was significantly decreased in middle-aged smokers compared to young smokers and non-smokers (3.34 ± 1.52 vs 4.43 ± 0.92 and 4.69 ± 1.25, p < 0.05, respectively). MBFCPT/rest at 1 month after smoking cessation significantly increased in young smokers, but not in middle-aged smokers. By multivariate analysis, baseline serum malondialdehyde-modified low-density lipoprotein (MDA-LDL) was an independent predictor for the changes in MBFCPT/rest after smoking cessation (β = –0.45, p < 0.05).
Conclusion
Coronary endothelial dysfunction was reversible by short-term smoking cessation in young smokers, but not in middle-aged smokers, which was associated with serum MDA-LDL levels. Long-term smoking exposure could lead to more advanced coronary endothelial dysfunction and atherosclerosis possibly via oxidative stress.


Similar content being viewed by others
Abbreviations
- ATP:
-
Adenosine triphosphate
- BP:
-
Blood pressure
- CPT:
-
Cold pressor test
- HDL:
-
High-density lipoprotein
- LDL:
-
Low-density lipoprotein
- MBF:
-
Myocardial blood flow
- MBFATP/rest :
-
Ratio of myocardial blood flow during adenosine triphosphate infusion to that at rest
- MBFCPT/rest :
-
Ratio of myocardial blood flow during the cold pressor test to that at rest
- MDA:
-
Malondialdehyde
- PET:
-
Positron emission tomography
- RPP:
-
Rate-pressure product
References
Schindler TH, Nitzsche EU, Munzel T, Olschewski M, Brink I, Jeserich M, et al. Coronary vasoregulation in patients with various risk factors in response to cold pressor testing: contrasting myocardial blood flow responses to short- and long-term vitamin C administration. J Am Coll Cardiol 2003;42:814–22.
Kaufmann PA, Gnecchi-Ruscone T, di Terlizzi M, Schäfers KP, Lüscher TF, Camici PG. Coronary heart disease in smokers: vitamin C restores coronary microcirculatory function. Circulation 2000;102:1233–8.
Iwado Y, Yoshinaga K, Furuyama H, Ito Y, Noriyasu K, Katoh C, et al. Decreased endothelium-dependent coronary vasomotion in healthy young smokers. Eur J Nucl Med Mol Imaging 2002;29:984–90.
Morita K, Tsukamoto T, Naya M, Noriyasu K, Inubushi M, Shiga T, et al. Smoking cessation normalizes coronary endothelial vasomotor response assessed with 15O-water and PET in healthy young smokers. J Nucl Med 2006;47:1914–20.
Tani S, Watanabe I, Anazawa T, Kawamata H, Tachibana E, Furukawa K, et al. Effect of pravastatin on malondialdehyde-modified low-density lipoprotein levels and coronary plaque regression as determined by three-dimensional intravascular ultrasound. Am J Cardiol 2005;96:1089–94.
Holvoet P, Collen D, Van de Werf F. Malondialdehyde-modified LDL as a marker of acute coronary syndromes. JAMA 1999;281:1718–21.
Katoh C, Morita K, Shiga T, Kubo N, Nakada K, Tamaki N. Improvement of algorithm for quantification of regional myocardial blood flow using 15O-water with PET. J Nucl Med 2004;45:1908–16.
Zeiher AM, Drexler H, Wollschlaeger H, Saurbier B, Just H. Coronary vasomotion in response to sympathetic stimulation in humans: importance of the functional integrity of the endothelium. J Am Coll Cardiol 1989;14:1181–90.
Tsukamoto T, Morita K, Naya M, Katoh C, Inubushi M, Kuge Y, et al. Myocardial flow reserve is influenced by both coronary artery stenosis severity and coronary risk factors in patients with suspected coronary artery disease. Eur J Nucl Med Mol Imaging 2006;33:1150–6.
Attebring M, Herlitz J, Berndt AK, Karlsson T, Hjalmarson A. Are patients truthful about their smoking habits? A validation of self-report about smoking cessation with biochemical markers of smoking activity amongst patients with ischaemic heart disease. J Intern Med 2001;249:145–51.
Naya M, Tsukamoto T, Morita K, Katoh C, Furumoto T, Fujii S, et al. Olmesartan, but not amlodipine, improves endothelium-dependent coronary dilation in hypertensive patients. J Am Coll Cardiol 2007;50:1144–9.
Prior JO, Schindler TH, Facta AD, Hernandez-Pampaloni M, Campisi R, Dahlbom M, et al. Determinants of myocardial blood flow response to cold pressor testing and pharmacologic vasodilation in healthy humans. Eur J Nucl Med Mol Imaging 2007;34:20–7.
Naya M, Tsukamoto T, Morita K, Katoh C, Furumoto T, Fujii S, et al. Plasma interleukin-6 and tumor necrosis factor-alpha can predict coronary endothelial dysfunction in hypertensive patients. Hypertens Res 2007;30:541–8.
Valenta I, Quercioli A, Vincenti G, Nkoulou R, Dewarrat S, Rager O, et al. Structural epicardial disease and microvascular function are determinants of an abnormal longitudinal myocardial blood flow difference in cardiovascular risk individuals as determined with PET/CT. J Nucl Cardiol 2010; in press.
Gould KL, Nakagawa Y, Nakagawa K, Sdringola S, Hess MJ, Haynie M, et al. Frequency and clinical implications of fluid dynamically significant diffuse coronary artery disease manifest as graded, longitudinal, base-to-apex myocardial perfusion abnormalities by noninvasive positron emission tomography. Circulation 2000;101:1931–9.
Zeiher AM, Drexler H, Saurbier B, Just H. Endothelium-mediated coronary blood flow modulation in humans. Effects of age, atherosclerosis, hypercholesterolemia, and hypertension. J Clin Invest 1993;92:652–62.
Barua RS, Ambrose JA, Srivastava S, DeVoe MC, Eales-Reynolds LJ. Reactive oxygen species are involved in smoking-induced dysfunction of nitric oxide biosynthesis and upregulation of endothelial nitric oxide synthase: an in vitro demonstration in human coronary artery endothelial cells. Circulation 2003;107:2342–7.
Campisi R, Czernin J, Schöder H, Sayre JW, Schelbert HR. L-Arginine normalizes coronary vasomotion in long-term smokers. Circulation 1999;99:491–7.
Tracy RP, Psaty BM, Macy E, Bovill EG, Cushman M, Cornell ES, et al. Lifetime smoking exposure affects the association of C-reactive protein with cardiovascular disease risk factors and subclinical disease in healthy elderly subjects. Arterioscler Thromb Vasc Biol 1997;17:2167–76.
Mazzone A, Cusa C, Mazzucchelli I, Vezzoli M, Ottini E, Ghio S, et al. Cigarette smoking and hypertension influence nitric oxide release and plasma levels of adhesion molecules. Clin Chem Lab Med 2001;39:822–6.
Heitzer T, Ylä-Herttuala S, Luoma J, Kurz S, Münzel T, Just H, et al. Cigarette smoking potentiates endothelial dysfunction of forearm resistance vessels in patients with hypercholesterolemia. Role of oxidized LDL. Circulation 1996;93:1346–53.
Schindler TH, Nitzsche EU, Schelbert HR, Olschewski M, Sayre J, Mix M, et al. Positron emission tomography-measured abnormal responses of myocardial blood flow to sympathetic stimulation are associated with the risk of developing cardiovascular events. J Am Coll Cardiol 2005;45:1505–12.
Rosenberg L, Kaufman DW, Helmrich SP, Shapiro S. The risk of myocardial infarction after quitting smoking in men under 55 years of age. N Engl J Med 1985;313:1511–4.
Petruzzelli S, Tavanti LM, Pulerà N, Fornai E, Puntoni R, Celi A, et al. Effects of nicotine replacement therapy on markers of oxidative stress in cigarette smokers enrolled in a smoking cessation program. Nicotine Tob Res 2000;2:345–50.
Acknowledgement
This study was supported in part by the Grants-in-Aid for Young Scientists (20790871) from the Ministry of Education, Culture, Sports, Science and Technology, Japan (MN), in part by The Mochida Memorial Foundation for Medical and Pharmaceutical Research, Japan (MN), and in part by the Smoking Research Foundation, Japan (NT).
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Naya, M., Morita, K., Yoshinaga, K. et al. Long-term smoking causes more advanced coronary endothelial dysfunction in middle-aged smokers compared to young smokers. Eur J Nucl Med Mol Imaging 38, 491–498 (2011). https://doi.org/10.1007/s00259-010-1647-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-010-1647-2