Abstract
Purpose
The purpose of the current study was to comprehensively evaluate occupational radiation exposure to all intraoperative and perioperative personnel involved in radioguided surgical procedures utilizing 18F-fluorodeoxyglucose (18F-FDG).
Methods
Radiation exposure to surgeon, anesthetist, scrub technologist, circulating nurse, preoperative nurse, and postoperative nurse, using aluminum oxide dosimeters read by optically stimulated luminescence technology, was evaluated during ten actual radioguided surgical procedures involving administration of 18F-FDG.
Results
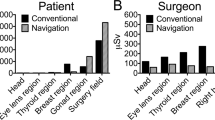
Mean patient dosage of 18F-FDG was 699 ± 181 MBq (range 451–984). Mean time from 18F-FDG injection to initial exposure of personnel to the patient was shortest for the preoperative nurse (75 ± 63 min, range 0–182) followed by the circulating nurse, anesthetist, scrub technologist, surgeon, and postoperative nurse. Mean total time of exposure of the personnel to the patient was longest for the anesthetist (250 ± 128 min, range 69–492) followed by the circulating nurse, scrub technologist, surgeon, postoperative nurse, and preoperative nurse. Largest deep dose equivalent per case was received by the surgeon (164 ± 135 μSv, range 10–580) followed by the anesthetist, scrub technologist, postoperative nurse, circulating nurse, and preoperative nurse. Largest deep dose equivalent per hour of exposure was received by the preoperative nurse (83 ± 134 μSv/h, range 0–400) followed by the surgeon, anesthetist, postoperative nurse, scrub technologist, and circulating nurse.
Conclusion
On a per case basis, occupational radiation exposure to intraoperative and perioperative personnel involved in 18F-FDG radioguided surgical procedures is relatively small. Development of guidelines for monitoring occupational radiation exposure in 18F-FDG cases will provide reassurance and afford a safe work environment for such personnel.
Similar content being viewed by others
References
Desai D, Arnold M, Saha S, Hinkle G, Soble D, Fry J, et al. Intraoperative gamma detection of FDG distribution in colorectal cancer. Clin Positron Imaging 1999;2:325.
Desai DC, Arnold M, Saha S, Hinkle G, Soble D, Fry J, et al. Correlative whole-body FDG-PET and intraoperative gamma detection of FDG distribution in colorectal cancer. Clin Positron Imaging 2000;3:189–96.
Zervos EE, Desai DC, DePalatis LR, Soble D, Martin EW. 18F-labeled fluorodeoxyglucose positron emission tomography-guided surgery for recurrent colorectal cancer: a feasibility study. J Surg Res. 2001;97:9–13.
Essner R, Hsueh EC, Haigh PI, Glass EC, Huynh Y, Daghighian F. Application of an [(18)F]fluorodeoxyglucose-sensitive probe for the intraoperative detection of malignancy. J Surg Res. 2001;96:120–6.
Essner R, Daghighian F, Giuliano AE. Advances in FDG PET probes in surgical oncology. Cancer J. 2002;8:100–8.
Carrera D, Fernandez A, Estrada J, Martin-Comin J, Gamez C. [Detection of occult malignant melanoma by 18F-FDG PET-CT and gamma probe]. Rev Esp Med Nucl. 2005;24:410–13, [Spanish].
Franc BL, Mari C, Johnson D, Leong SP. The role of a positron- and high-energy gamma photon probe in intraoperative localization of recurrent melanoma. Clin Nucl Med. 2005;30:787–91.
Kraeber-Bodéré F, Cariou B, Curtet C, Bridji B, Rousseau C, Dravet F, et al. Feasibility and benefit of fluorine 18-fluoro-2-deoxyglucose-guided surgery in the management of radioiodine-negative differentiated thyroid carcinoma metastases. Surgery 2005;138:1176–82.
Meller B, Sommer K, Gerl J, von Hof K, Surowiec A, Richter E, et al. High energy probe for detecting lymph node metastases with 18F-FDG in patients with head and neck cancer. Nuklearmedizin 2006;45:153–9.
Gulec SA, Daghighian F, Essner R. PET-Probe: Evaluation of Technical Performance and Clinical Utility of a Handheld High-Energy Gamma Probe in Oncologic Surgery. Ann Surg Oncol 2006;Jul 24; [Epub ahead of print]; doi:10.1245/ASO.2006.05.047.
Sarikaya I, Povoski SP, Al-Saif OH, Kocak E, Bloomston M, Marsh S, et al. Combined use of preoperative 18F FDG-PET imaging and intraoperative gamma probe detection for accurate assessment of tumor recurrence in patients with colorectal cancer. World J Surg Oncol. 2007;5:80.
Sun D, Bloomston M, Hinkle G, Al-Saif OH, Hall NC, Povoski SP, et al. Radioimmunoguided surgery (RIGS), PET/CT image-guided surgery, and fluorescence image-guided surgery: past, present, and future. J Surg Oncol. 2007;96:297–308.
Piert M, Burian M, Meisetschläger G, Stein HJ, Ziegler S, Nährig J, et al. Positron detection for the intraoperative localisation of cancer deposits. Eur J Nucl Med Mol Imaging 2007;34:1534–44.
Piert M, Carey J, Clinthorne N. Probe-guided localization of cancer deposits using [18F]fluorodeoxyglucose. Q J Nucl Med Mol Imaging 2008;52:37–49.
Gulec SA, Hoenie E, Hostetter R, Schwartzentruber D. PET probe-guided surgery: applications and clinical protocol. World J Surg Oncol. 2007;5:65.
Gulec SA. PET probe-guided surgery. J Surg Oncol. 2007;96:353–7.
Hall NC, Povoski SP, Murrey DA, Knopp MV, Martin EW. Combined approach of perioperative 18F-FDG PET/CT imaging and intraoperative 18F-FDG handheld gamma probe detection for tumor localization and verification of complete tumor resection in breast cancer. World J Surg Oncol. 2007;5:143.
Povoski SP, Hall NC, Martin EW, Walker MJ. Multimodality approach of perioperative 18F-FDG PET/CT imaging, intraoperative 18F-FDG handheld gamma probe detection, and intraoperative ultrasound for tumor localization and verification of resection of all sites of hypermetabolic activity in a case of occult recurrent metastatic melanoma. World J Surg Oncol. 2008;6:1.
Schober O, Lottes G. [Positron emission tomography and radiation exposure]. Nuklearmedizin 1994;33:174–7, [German].
Benatar NA, Cronin BF, O'Doherty MJ. Radiation dose rates from patients undergoing PET: implications for technologists and waiting areas. Eur J Nucl Med. 2000;27:583–9.
Linemann H, Will E, Beuthien-Baumann B. [Investigations of radiation exposure of the medical personnel during F-18-FDG PET studies]. Nuklearmedizin 2000;39:77–81, [German].
White S, Binns D, Johnston VV, Fawcett M, Greer B, Ciavarella F, et al. Occupational exposure in nuclear medicine and PET. Clin Positron Imaging 2000;3:127–9.
Biran T, Weininger J, Malchi S, Marciano R, Chisin R. Measurements of occupational exposure for a technologist performing 18F FDG PET scans. Health Phys. 2004;87:539–44.
Roberts FO, Gunawardana DH, Pathmaraj K, Wallace A, U PL, Mi T, et al. Radiation dose to PET technologists and strategies to lower occupational exposure. J Nucl Med Technol. 2005;33:44–7.
Guillet B, Quentin P, Waultier S, Bourrelly M, Pisano P, Mundler O. Technologist radiation exposure in routine clinical practice with 18F-FDG PET. J Nucl Med Technol. 2005;33:175–9.
Robinson CN, Young JG, Wallace AB, Ibbetson VJ. A study of the personal radiation dose received by nuclear medicine technologists working in a dedicated PET center. Health Phys. 2005;88(2 Suppl):S17–S21.
Seierstad T, Stranden E, Bjering K, Evensen M, Holt A, Michalsen HM, et al. Doses to nuclear technicians in a dedicated PET/CT centre utilising 18F fluorodeoxyglucose (FDG). Radiat Prot Dosimetry. 2007;23:246–9.
Heckathorne E, Dimock C, Dahlbom M, Daghighian F. Radiation dose to surgical staff from PET-based localization and radiosurgery of tumors. Health Phys. 2007;93:S45.
Andersen PA, Chakera AH, Klausen TL, Binderup T, Grossjohann HS, Friis E, et al. Radiation exposure to surgical staff during F-18-FDG-guided cancer surgery. Eur J Nucl Med Mol Imaging 2008;35:624–9.
Curtet C, Carlier T, Mirallié E, Bodet-Milin C, Rousseau C, Barbet J, et al. Prospective comparison of two gamma probes for intraoperative detection of 18F-FDG: in vitro assessment and clinical evaluation in differentiated thyroid cancer patients with iodine-negative recurrence. Eur J Nucl Med Mol Imaging 2007;34:1556–62.
ICRP, Publication 60. The1990 Recommendations of the International Commission on Radiological Protection. Ann ICRP. 1991;21(1–3):1–201.
ICRP, Publication 103. The 2007 Recommendations of the International Commission on Radiological Protection (Chapters 5 and 6). Ann ICRP. 2007;37(2–4):81–123.
Acknowledgements
The authors would like to thank Deborah Hurley of the Nuclear Medicine Department for her ongoing efforts in the coordination and management of these and many other radioguided surgical procedures involving 18F-FDG administration. The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Povoski, S.P., Sarikaya, I., White, W.C. et al. Comprehensive evaluation of occupational radiation exposure to intraoperative and perioperative personnel from 18F-FDG radioguided surgical procedures. Eur J Nucl Med Mol Imaging 35, 2026–2034 (2008). https://doi.org/10.1007/s00259-008-0880-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-008-0880-4