Abstract
Objectives
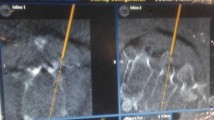
To investigate and illustrate a variation on the traditional percutaneous access to the vertebral body via a parapedicular approach.
Design
An effective parapedicular access technique that could safely and reliably guide the needle tip into the center of the vertebral body was developed from cadaver dissection observations for the purpose of clinical use.
Patients
A total of 102 vertebral compression fractures from T-4 to L-5 were treated via the parapedicular access at our institution between July 2005 and March 2006. There were 72 patients between the ages of 17 and 96 years (mean age: 68.2 years) who underwent treatment.
Results
The cadaver dissection revealed a relatively avascular and aneural portion of the vertebral body along the superior margin of the vertebral body-pedicle junction. A total 102 vertebral fractures were treated using the parapedicular access technique without any recognized clinical complications from the needle access or the instrumentation.
Conclusions
The thoracic and lumbar vertebral bodies may be safely, reliably, and reproducibly accessed using a percutaneous parapedicular access technique. The technique presented represents a relatively avascular and aneural approach to vertebral body.








Similar content being viewed by others
References
Galibert P, Deramond H, Rosat P, et. al. Preliminary note on the treatment of vertebral angioma by percutaneous acrylic vertebroplasty. Neurochirurgie 1987;33:166–8.
Barr JD, Barr MS, Lemly TJ, et. al. Percutaneous vertebroplasty for pain relief and spinal stabilization. Spine 2000;25:923–8.
Cotten A, Dewatre F, Cortet B, et. al. Percutaneous vertebroplasty for osteolytic metastases and myeloma: effects of the percentage of lesion filling and the leakage of methyl methacrylate at clinical follow-up. Radiology 1996;200:525–30.
Deramond H, Depriester C, Galibert P, et. al. Percutaneous vertebroplasty with polymethylmethacrylate. Radiol Clin N Am 1998;36:533–6.
Cooper C, Atkinson EJ, O’Fallon WM. Incidence of clinically diagnosed vertebral fractures: a population study based in Rochester, Minnesota, 1985–89. J Bone Miner Res 1992;7:221–7.
Vaccaro AR, Rizzolo SJ, Balderston RA, et al. Placement of pedicle screws I the thoracic spine. Part I: morphometric analysis of the thoracic vertebrae. J Bone Joint Surg [Am] 1995;77:1193–9.
Vaccaro AR, Rizzolo SJ, Balderston RA, et al. Placement of pedicle screws I the thoracic spine. Part II: an anatomical and radiographic assessment. J Bone Joint Surg [Am] 1995;77:1200–6.
Han KR, Kim C, Eun JS, Chung YS. Extrapedicular approach of percutaneous vertebroplasty in the treatment of upper and mid-thoracic vertebral compression fracture. Acta Radiol 2005;46:280–7.
Vaccaro AR, Yuan PS, Smith HE, Hott J, Sasso R, Papadopoulos S. An evaluation of image-guided technologies in the placement of anterior thoracic vertebral body screws in spinal trauma: a cadaver study. J Spinal Cord Med. 2005;28:308–13.
Chiras J, Deramond H. Complications des vertĕbroplasties. In: Saillants G, Laville C (eds) Echecs et complication de la chirurgie du rachis. Sauramps Medical, Montpellier, France 1995; pp 149–53.
Chiras J, Depriester C, Weill A, Sola Martinez M-T, Deramond H. Vertĕbroplasties percutanees, Technique et indications. J Neuroradiol 1997;24:45–59.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Beall, D.P., Braswell, J.J., Martin, H.D. et al. Technical strategies and anatomic considerations for parapedicular access to thoracic and lumbar vertebral bodies. Skeletal Radiol 36, 47–52 (2007). https://doi.org/10.1007/s00256-006-0192-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-006-0192-3