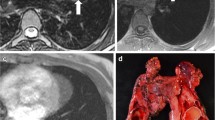
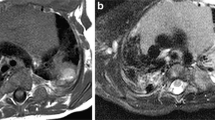
Abstract
The mediastinum, the central anatomical space of the thorax, is divided by anatomical landmarks but not by physical boundaries. The mediastinum is a conduit, a space through which cranial nerves, important nerve branches, the sympathetic chain, vascular structures, and visceral structures, the trachea and esophagus pass. This arrangement allows contiguous extension or communication of disease along facial planes and through potential spaces to and from the head and neck or cervical spine, to and from the superior mediastinum, between superior and inferior mediastinal levels, and between inferior mediastinal spaces into the intra- and retroperitoneal spaces. Magnetic resonance imaging (MRI) of the mediastinum in children poses technical challenges, in particular cardiac and respiratory motion, and diagnostic challenges, including a broad range of tissue types and possible diagnoses. In this paper we review mediastinal anatomy, MRI sequences and protocol choices and include a short discussion of features and MRI findings of some of the congenital and acquired pathologies that are most often encountered in the pediatric mediastinum.















Similar content being viewed by others
References
Aquino SL, Duncan G, Taber KH et al (2001) Reconciliation of the anatomic, surgical, and radiographic classifications of the mediastinum. J Comput Assist Tomogr 25:489–492
Nason LK, Walker CM, McNeeley MF et al (2012) Imaging of the diaphragm: anatomy and function. Radiographics 32:E51–E70
Wang J, Li J, Liu G, Deslauriers J (2011) Nerves of the mediastinum. Thoac Surg Clin 21:139–322
Ackman JB (2015) MR imaging of mediastinal masses. Magn Reson Imaging Clin N Am 23:141–164
Chavhan GB (2016) Appropriate selection of MRI sequences for common scenarios in clinical practice. Pediatr Radiol 46:740–747
Krishnamurthy R, Malone L, Lyons K et al (2016) Body MR angiography in children: how we do it. Pediatr Radiol 46:748–763
Pokorney A, Chia J, Bardo DME et al (2017) Non-gadolinium-contrast relaxation-enhanced MR angiography in children with an inversion recovery and T2-prepared 3D mDIXON gradient-echo technique: preliminary experience. Presented at the 25th annual meeting and exhibition of the International Society for Magnetic Resonance in Medicine, Honolulu
Berrocal T, Madrid C, Novo S et al (2004) Congenital anomalies of the tracheobronchial tree, lung, and mediastinum: embryology, radiology, and pathology. Radiographics 24:e17
Sharma S, Nezakatgoo N, Sreenivasan P et al (2009) Foregut cystic developmental malformation: new taxonomy and classification — unifying embryopathological concepts. Indian J Pathol Microbiol 52:461–472
Som PM, Grapin-Botton A (2016) The current embryology of the foregut and its derivatives. Neurographics 6:43–63
McAdams HP, Kirejczyk WM, Rosado-de-Christenson ML, Matsumoto S (2000) Bronchogenic cyst: imaging features with clinical and histopathologic correlation. Radiology 217:441–446
Jeung MY, Gasser B, Gangi A et al (2002) Imaging of cystic masses of the mediastinum. Radiographics 22:S79–S93
Inaoka T, Takahashi K, Mineta M et al (2007) Thymic hyperplasia and thymus gland tumors: differentiation with chemical shift MR imaging. Radiology 243:869–876
Ackman JB, Wu CC (2010) MRI of the thymus. AJR Am J Roentgenol 19:W15–W20
Tomiyama N, Honda O, Tsubamoto M et al (2009) Anterior mediastinal tumors: diagnostic accuracy of CT and MRI. Eur J Radiol 69:280–288
Lonergan GJ, Schwab CM, Suarez ES, Carlson CL (2002) Neuroblastoma, ganglioneuroblastoma, and ganglioneuroma: radiologic-pathologic correlation. Radiographics 22:911–934
Maitra A (2014) Diseases of infancy and childhood. In: Kumar V, Abbas AK, Fausto N, Aster JC (eds) Robbins and Cotran pathologic basis of disease, 9th edn. W.B. Saunders, Philadelphia, pp 451–482
Jaggers J, Balsara K (2004) Mediastinal masses in children. Semin Thorac Cardiovasc Surg 16:201–208
Franco A, Mody NS, Meza MP (2005) Imaging evaluation of pediatric mediastinal masses. Radiol Clin N Am 43:325–353
Vermoolen MA, Kersten MJ, Fijnheer R et al (2011) Magnetic resonance imaging of malignant lymphoma. Expert Rev Hematol 4:161–171
Manson DE (2016) Magnetic resonance imaging of the mediastinum, chest wall and pleura in children. Pediatr Radiol 46:902–915
Shahrzad M, Le TSM, Silva M et al (2014) Anterior mediastinal masses. AJR Am J Roentgenol 203:W128–W138
Ueno T, Tanaka YO, Nagata M et al (2004) Spectrum of germ cell tumors: from head to toe. Radiographics 24:387–404
Patel IJ, Hsiao E, Ahmad AH et al (2013) AIRP best cases in radiologic-pathologic correlation: mediastinal mature cystic teratoma. Radiographics 33:797–801
Reali A, Mortellaro G, Allis S et al (2013) A case of primary mediastinal Ewing’s sarcoma/primitive neuroectodermal tumor presenting with initial compression of superior vena cava. Ann Thorac Med 8:121–123
Murphey MD, Senchak LT, Mambalam PK et al (2013) From the radiologic pathology archives: Ewing sarcoma family of tumors: radiologic-pathologic correlation. Radiographics 33:803–831
McCarville MB (2016) What MRI can tell us about neurogenic tumors and rhabdomyosarcoma. Pediatr Radiol 46:881–890
Mautner VF, Asuagbor FA, Dombi E et al (2008) Assessment of benign tumor burden by whole-body MRI in patients with neurofibromatosis 1. Neuro Oncol 10:593–598
Wasa J, Nishida Y, Tsukushi S et al (2010) MRI feature in the differentiation of malignant peripheral nerve sheath tumors and neurofibromas. AJR Am J Roentgenol 194:1568–1574
Castellote A, Vazquez E, Vera J et al (1999) Cervicothoracic lesions in infants and children. Radiographics 19:583–600
Wassef M, Blei F, Adams D et al (2014) Vascular Anomalies classification: recommendations from the International Society for the Study of Vascular Anomalies. Pediatrics 136:e203–e214
Elluru RG, Balakrishnan K, Padua HM (2014) Lymphatic malformations: diagnosis and management. Semin Pediatr Surg 23:178–185
White CL, Olivieri B, Restrepo R et al (2016) Low-flow vascular malformation pitfalls: from clinical examination to practical imaging evaluation — part 1, lymphatic malformation mimickers. AJR Am J Roentgenol 206:940–951
Sjogren PP, Arnold RW, Skirko JR, Grimmer JF (2017) Anatomic distribution of cervicofacial lymphatic malformations based on lymph node groups. Int J Pediatr Otorhinolaryngol 97:72–75
Johnson OW, Chick JFB, Chauhan NR et al (2016) The thoracic duct: clinical importance, anatomic variation, imaging, and embolization. Eur Radiol 26:2482–2493
Kumar S, Kumar A, Pawar DK (2004) Thoracoscopic management of thoracic duct injury: is there a place for conservatism? J Postgrad Med 50:57–59
Krishnamurthy R, Hernandez A, Kavuk S et al (2014) Imaging the central conducting lymphatics: initial experience with dynamic MR lymphangiography. Radiology 274:871–878
Henry Gray (2017) (1821–1865). Anatomy of the human body. 1918. 3c. The veins of the upper extremity and thorax. Bartleby.com. http://www.bartleby.com/107/172.html. Accessed 08 Sept 2017
Ko S, Huang C, Ng S et al (2008) Imaging of the brachiocephalic vein. AJR Am J Roentgenol 191:897–907
Arnoldsussen CWKP, Strijkers RHW, Lambregts DMJ et al (2014) Feasibility of identifying deep vein thrombosis characteristics with contrast enhanced MR-venography. Phlebol J Ven Dis 29:119–124
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Bardo, D.M.E., Biyyam, D.R., Patel, M.C. et al. Magnetic resonance imaging of the pediatric mediastinum. Pediatr Radiol 48, 1209–1222 (2018). https://doi.org/10.1007/s00247-018-4112-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4112-1