Abstract
Background
Anatomical imaging findings indicating normal bowel rotation can be identified on cross-sectional imaging, including magnetic resonance imaging (MRI) performed for non-related indications.
Objective
The goal of our study was to assess whether non-targeted MRI can accurately assess intestinal malrotation.
Materials and methods
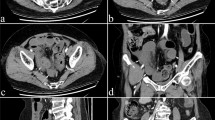
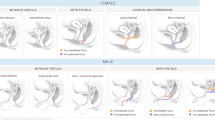
Four anatomical landmarks were assessed on MRIs of the chest, spine or abdomen performed from January 2006 to June 2014, on patients who also had upper gastrointestinal series (UGI) performed within 10 years of the MRI date: 1) retroperitoneal duodenum, 2) left upper quadrant duodenojejunal junction, 3) superior mesenteric artery to the left of the superior mesenteric vein, and 4) right lower quadrant cecum. Two attending radiologists, one pediatric and one abdominal radiologist, independently reviewed the MR images. The pediatric radiologist reviewed images from UGI (considered the gold standard) to determine the intestinal rotation for each case. Validation of the criteria was performed on new patients imaged through January 2016.
Results
The original cohort included 109 MRIs (15 chest, 41 spine and 53 abdomen) done on 109 patients (42% males, mean age: 10.2 years). If each of the 4 anatomical questions were answered “yes” (4-YES), specificity was 100% for each radiologist and malrotation was appropriately excluded. Using the 4-YES criteria, the pediatric radiologist excluded malrotation in 71 patients (65%) and the abdominal radiologist excluded it in 65 (60%), with concurrence for 57 patients. Validation of the 4-YES criteria in 23 new patients appropriately proved the 4-YES rule, with neither labeling the one new malrotation case 4-YES.
Conclusion
If a radiologist can confidently answer “yes” to the four questions evaluated in this study, then intestinal rotation can be safely considered normal. Normal bowel rotation should be commented upon in MRI reports when these four anatomical locations are imaged, thus helping patients avoid unnecessary UGI and radiation exposure.





Similar content being viewed by others
References
Applegate K (2009) Evidence-based diagnosis of malrotation and volvulus. Pediatr Radiol 39:S161–S163
Lampl B, Levin T, Berdon W et al (2009) Malrotation and midgut volvulus: a historical review and current controversies in diagnosis and management. Pediatr Radiol 39:359–366
Newman B, Koppolu R, Murphy D et al (2014) Heterotaxy syndromes and abnormal bowel rotation. Pediatr Radiol 44:542–551
Larson-Nath CM, Wagner AJ, Goday PS (2014) Use of upper gastrointestinal series before gastrostomy tube placement. J Pediatr Gastroenterol Nutr 58:613–615
Strouse P (2008) Malrotation. Semin Roentgenol 43:7–14
Yousefzadeh D (2009) The position of the duodenojejunal junction: the wrong horse to bet on in diagnosing or excluding malrotation. Pediatr Radiol 39:S172–S177
Emigh B, Gordon CL, Connolly BL et al (2013) Effective dose estimation for pediatric upper gastrointestinal examinations using an anthropomorphic phantom set and metal oxide semiconductor field-effect transistor (MOSFET) technology. Pediatr Radiol 43:1108–1116
Ritenour ER (2013) Answer to question #10655 submitted to “ask the experts.” Health Physics Society. https://hps.org/publicinformation/ate/q10655.html#. Accessed 18 Mar 2017
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Fay, J.S., Chernyak, V. & Taragin, B.H. Identifying intestinal malrotation on magnetic resonance examinations ordered for unrelated indications. Pediatr Radiol 47, 1477–1482 (2017). https://doi.org/10.1007/s00247-017-3903-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-017-3903-0