Abstract
Background
In order to assess relationships between thyroid hormone status and findings on brain MRI, a subset of babies was recruited to a multi-centre randomised, placebo-controlled trial of levothyroxine (LT4) supplementation for babies born before 28 weeks’ gestation (known as the TIPIT study, for Thyroxine supplementation In Preterm InfanTs). These infants were imaged at term-equivalence.
Materials and methods
Forty-five TIPIT participants had brain MRI using diffusion tensor imaging (DTI) to estimate white matter development by apparent diffusion coefficient (ADC), fractional anisotropy (FA) and tractography metrics of number and length of streamlines. We made comparisons between babies with the lowest and highest plasma FT4 concentrations during the initial 4 weeks after birth.
Results
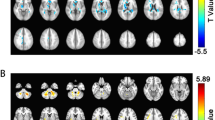
There were no differences in DTI metrics between babies who had received LT4 supplementation and those who had received a placebo. Among recipients of a placebo, babies in the lowest quartile of plasma-free thyroxine (FT4) concentrations had significantly higher apparent diffusion coefficient measurements in the posterior corpus callosum and streamlines that were shorter and less numerous in the right internal capsule. Among LT4-supplemented babies, those who had plasma FT4 concentrations in the highest quartile had significantly lower apparent diffusion coefficient values in the left occipital lobe, higher fractional anisotropy in the anterior corpus callosum and longer and more numerous streamlines in the anterior corpus callosum.
Conclusion
DTI variables were not associated with allocation of placebo or thyroid supplementation. Markers of poorly organised brain microstructure were associated with low plasma FT4 concentrations after birth. The findings suggest that plasma FT4 concentrations affect brain development in very immature infants and that the effect of LT4 supplementation for immature babies with low FT4 plasma concentrations warrants further study.


Similar content being viewed by others
References
Wood NS, Costeloe K, Gibson AT et al (2005) The EPICure study: associations and antecedents of neurological and developmental disability at 30 months of age following extremely preterm birth. Arch Dis Child Fetal Neonatal Ed 90:F134–F140
Den Ouden AL, Kok JH, Verkerk PH et al (1996) The relation between neonatal thyroxine levels and neurodevelopmental outcome at age 5 and 9 years in a national cohort of very preterm and/or very low birth weight infants. Pediatr Res 39:142–145
Leviton A, Paneth N, Reuss ML et al (1999) Hypothyroxinemia of prematurity and the risk of cerebral white matter damage. J Pediatr 134:706–711
Ng SM, Turner MA, Gamble C et al (2013) An explanatory randomised placebo controlled trial of levothyroxine supplementation for babies born <28 weeks’ gestation: results of the TIPIT trial. Trials 14:211
Schoonover CM, Seibel MM, Jolson DM et al (2004) Thyroid hormone regulates oligodendrocyte accumulation in developing rat brain white matter tracts. Endocrinology 145:5013–5020
Gupta RK, Bhatia V, Poptani H et al (1995) Brain metabolite changes on in vivo proton magnetic resonance spectroscopy in children with congenital hypothyroidism. J Pediatr 126:389–392
Jagannathan NR, Tandon N, Raghunathan P et al (1998) Reversal of abnormalities of myelination by thyroxine therapy in congenital hypothyroidism: localized in vivo proton magnetic resonance spectroscopy (MRS) study. Brain Res Dev Brain Res 109:179–186
Berman JI, Mukherjee P, Partridge SC et al (2005) Quantitative diffusion tensor MRI fiber tractography of sensorimotor white matter development in premature infants. Neuroimage 27:862–871
Nair G, Tanahashi Y, Low HP et al (2005) Myelination and long diffusion times alter diffusion-tensor-imaging contrast in myelin-deficient shiverer mice. Neuroimage 28:165–174
Van Wassenaer AG, Briet JM, van Baar A et al (2002) Free thyroxine levels during the first weeks of life and neurodevelopmental outcome until the age of 5 years in very preterm infants. Pediatrics 110:534–539
Oouchi H, Yamada K, Sakai K et al (2007) Diffusion anisotropy measurement of brain white matter is affected by voxel size: underestimation occurs in areas with crossing fibers. AJNR Am J Neuroradiol 28:1102–1106
Jiang H, van Zijl PC, Kim J et al (2006) DtiStudio: resource program for diffusion tensor computation and fiber bundle tracking. Comput Methods Programs Biomed 81:106–116
De Vries LS, Groenendaal F, van Haastert IC et al (1999) Asymmetrical myelination of the posterior limb of the internal capsule in infants with periventricular haemorrhagic infarction: an early predictor of hemiplegia. Neuropediatrics 30:314–319
Rutherford MA, Pennock JM, Counsell SJ et al (1998) Abnormal magnetic resonance signal in the internal capsule predicts poor neurodevelopmental outcome in infants with hypoxic-ischemic encephalopathy. Pediatrics 102:323–328
Jones DK (2010) Challenges and limitations of quantifying brain connectivity in vivo with diffusion MRI. Imaging Med 2:341–355
Correia S, Lee SY, Voorn T et al (2008) Quantitative tractography metrics of white matter integrity in diffusion-tensor MRI. Neuroimage 42:568–581
Partridge SC, Mukherjee P, Berman JI et al (2005) Tractography-based quantitation of diffusion tensor imaging parameters in white matter tracts of preterm newborns. J Magn Reson Imaging 22:467–474
Dudink J, Lequin M, van Pul C et al (2007) Fractional anisotropy in white matter tracts of very-low-birth-weight infants. Pediatr Radiol 37:1216–1223
Chau V, Brant R, Poskitt KJ et al (2012) Postnatal infection is associated with widespread abnormalities of brain development in premature newborns. Pediatr Res 71:274–279
Van Kooij BJ, de Vries LS, Ball G et al (2012) Neonatal tract-based spatial statistics findings and outcome in preterm infants. AJNR Am J Neuroradiol 33:188–194
Rose J, Butler EE, Lamont LE et al (2009) Neonatal brain structure on MRI and diffusion tensor imaging, sex, and neurodevelopment in very-low-birthweight preterm children. Dev Med Child Neurol 51:526–535
Acknowledgments
We would like to acknowledge the support of the Medical Research Council (Clinical Research Fellowship to Dr. Sze May Ng) and Newborn Appeal for funding, the Medicines for Children’s Research Network Clinical Trials Unit for information systems and data support, the Pharmacy Department of Liverpool Women’s Foundation NHS Trust, Wellcome Trust Clinical Research Facility, Royal Liverpool and Broadgreen University Hospitals NHS Trust for pharmaceutical support and the Biochemistry and Radiology departments of Alder Hey Children’s Hospital for their support in the trial. The research team also acknowledges the support of the National Institute for Health Research, through the Cheshire, Merseyside & North Wales Medicines for Children Local Research Network and the Greater Manchester, Lancashire and South Cumbria Medicines for Children Research Network.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ng, S.M., Turner, M.A., Gamble, C. et al. Effect of thyroxine on brain microstructure in extremely premature babies: magnetic resonance imaging findings in the TIPIT study. Pediatr Radiol 44, 987–996 (2014). https://doi.org/10.1007/s00247-014-2911-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-014-2911-6