Abstract
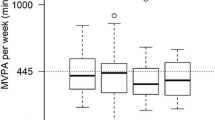
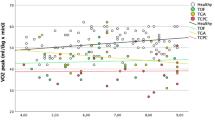
The aim of this study was to determine factors associated with physical fitness (PF) in children who underwent surgery for congenital heart disease (CHD). Sixty-six children (7–14 years) who underwent surgery for ventricular septal defect (n = 19), transposition of great arteries (n = 22), coarctation of aorta (n = 10), and tetralogy of Fallot (n = 15) were included. All children performed PF tests: cardiorespiratory fitness, upper- and lower-limb muscle strength, speed, balance, and flexibility. Cardiac evaluation was done via echocardiography and cardiopulmonary exercise test. Factors related to child’s characteristics, child’s lifestyle, physical activity motivators/barriers, and parental factors were assessed. Linear regression analyses were conducted. The results showed no significant differences in physical activity (PA) level by CHD type. Boys had better cardiorespiratory fitness (difference = 1.86 ml/kg/min [0.51;3.22]) and were more physically active (difference = 19.40 min/day [8.14;30.66]), while girls had better flexibility (difference = − 3.60 cm [− 7.07;− 0.14]). Physical activity motivators showed an association with four out of six PF components: cardiorespiratory fitness, coefficient = 0.063 [0.01;0.11]; upper-limb muscle strength, coefficient = 0.076 [0.01;0.14]; lower-limb muscle strength, coefficient = 0.598 [0.07;1.13]; and speed, coefficient = 0.03 [0.01;0.05]. Age, sex, and motivators together reached a maximum adjusted R2 = 0.707 for upper-limb strength. Adding other possible determinants did not significantly increase the explained variance. Apart from age and sex as non-modifiable determinants, the main target which might improve fitness would be the introduction of an intervention which increases the motivation to be active.

Similar content being viewed by others
References
Khairy P, Ionescu-Ittu R, Mackie AS, Abrahamowicz M, Pilote L, Marelli AJ (2010) Changing mortality in congenital heart disease. J Am Coll Cardiol 56:1149–1157
Ortega F, Ruiz J, Castillo M, Sjöström M (2008) Physical fitness in childhood and adolescence: a powerful marker of health. Int J Obes 32:1–11
Zaqout M, Vyncke K, Moreno LA, De Miguel-Etayo P, Lauria F, Molnar D, Lissner L, Hunsberger M, Veidebaum T, Tornaritis M (2016) Determinant factors of physical fitness in European children. Int J Public Health 61:573–582
Voss C, Duncombe SL, Dean PH, de Souza AM, Harris KC (2017) Physical activity and sedentary behavior in children with congenital heart disease. J Am Heart Assoc 6:e004665
Zaqout M, Vandekerckhove K, Michels N, Bove T, François K, De Wolf D (2017) Physical fitness and metabolic syndrome in children with repaired congenital heart disease compared with healthy children. J Pediatr 191:125–132
Longmuir PE, Brothers JA, de Ferranti SD, Hayman LL, Van Hare GF, Matherne GP, Davis CK, Joy EA, McCrindle BW (2013) Promotion of physical activity for children and adults with congenital heart disease. Circulation 127:2147–2159
Rosenblum O, Katz U, Reuveny R, Williams CA, Dubnov-Raz G (2015) Exercise performance in children and young adults after complete and incomplete repair of congenital heart disease. Pediatr Cardiol 36:1573–1581
Reybrouck T, Mertens L (2005) Physical performance and physical activity in grown-up congenital heart disease. Eur J Cardiovasc Prev Rehabil 12:498–502
Massin MM, Hövels-Gürich HH, Gérard P, Seghaye M-C (2006) Physical activity patterns of children after neonatal arterial switch operation. Ann Thorac Surg 81:665–670
Barbiero SM, Sica CDA, Schuh DS, Cesa CC, de Oliveira PR, Pellanda LC (2014) Overweight and obesity in children with congenital heart disease: combination of risks for the future? BMC Pediatr 14:271
Pinto NM, Marino BS, Wernovsky G, De Ferranti SD, Walsh AZ, Laronde M, Hyland K, Dunn SO, Cohen MS (2007) Obesity is a common comorbidity in children with congenital and acquired heart disease. Pediatrics 120:e1157–e1164
Shustak RJ, McGuire SB, October TW, Phoon CK, Chun AJ (2012) Prevalence of obesity among patients with congenital and acquired heart disease. Pediatr Cardiol 33:8–14
Chung S, Hong B, Patterson L, Petit C, Ham J (2016) High overweight and obesity in Fontan patients: a 20-year history. Pediatr Cardiol 37:192–200
Stefan MA, Hopman WM, Smythe JF (2005) Effect of activity restriction owing to heart disease on obesity. Arch Pediatr Adolesc Med 159:477–481
Moola F, Faulkner GE, Kirsh JA, Kilburn J (2008) Physical activity and sport participation in youth with congenital heart disease: perceptions of children and parents. Adapt Phys Act Q 25:49–70
Norozi K, Gravenhorst V, Hobbiebrunken E, Wessel A (2005) Normality of cardiopulmonary capacity in children operated on to correct congenital heart defects. Arch Pediatr Adolesc Med 159:1063–1068
Ruiz JR, Castro-Piñero J, España-Romero V, Artero EG, Ortega FB, Cuenca MM, Jimenez-Pavón D, Chillón P, Girela-Rejón MJ, Mora J (2010) Field-based fitness assessment in young people: the alpha health-related fitness test battery for children and adolescents. Br J Sports Med. bjsports75341
Artero E, Espana-Romero V, Castro-Pinero J, Ortega F, Suni J, Castillo-Garzon M, Ruiz J (2011) Reliability of field-based fitness tests in youth. Int J Sports Med 32:159–169
Cole TJ, Lobstein T (2012) Extended international (IOTF) body mass index cut-offs for thinness, overweight and obesity. Pediatr Obes 7:284–294
Lanfer A, Hebestreit A, Ahrens W, Krogh V, Sieri S, Lissner L, Eiben G, Siani A, Huybrechts I, Loit H (2011) Reproducibility of food consumption frequencies derived from the children’s eating habits questionnaire used in the IDEFICS study. Int J Obes 35:S61–S68
Lanfer A, Knof K, Barba G, Veidebaum T, Papoutsou S, De Henauw S, Soos T, Moreno L, Ahrens W, Lissner L (2012) Taste preferences in association with dietary habits and weight status in European children: results from the IDEFICS study. Int J Obes 36:27–34
Evenson KR, Catellier DJ, Gill K, Ondrak KS, McMurray RG (2008) Calibration of two objective measures of physical activity for children. J Sports Sci 26:1557–1565
http://www.kindl.org National sleep foundation (2011) Children and sleep—information on sleep health and safety
Goodman R, Meltzer H, Bailey V (1998) The strengths and difficulties questionnaire: a pilot study on the validity of the self-report version. Eur Child Adolesc Psychiatry 7:125–130
Tucker CM, Rice KG, Desmond FF, Hou W, Kaye LB, Smith TM (2012) The youth form of the motivators of and barriers to health-smart behaviors inventory. Psychol Assess 24:490
Vandekerckhove K, Coomans I, De Bruyne E, De Groote K, Panzer J, De Wolf D, Boone J, De Bruyne R (2016) Evaluation of exercise performance, cardiac function, and quality of life in children after liver transplantation. Transplantation 100:1525–1531
Leger LA, Mercier D, Gadoury C, Lambert J (1988) The multistage 20 metre shuttle run test for aerobic fitness. J Sports Sci 6:93–101
De Miguel-Etayo P, Gracia-Marco L, Ortega F, Intemann T, Foraita R, Lissner L, Oja L, Barba G, Michels N, Tornaritis M (2014) Physical fitness reference standards in European children: the IDEFICS study. Int J Obes 38:S57–S66
Banks L, Rosenthal S, Manlhiot C, Fan C-PS, McKillop A, Longmuir PE, McCrindle BW (2017) Exercise capacity and self-efficacy are associated with moderate-to-vigorous intensity physical activity in children with congenital heart disease. Pediatr Cardiol 38:1206–1214
Takken T, Giardini A, Reybrouck T, Gewillig M, Hövels-Gürich H, Longmuir P, McCrindle B, Paridon S, Hager A (2012) Recommendations for physical activity, recreation sport, and exercise training in paediatric patients with congenital heart disease: a report from the exercise, basic & translational research section of the European association of cardiovascular prevention and rehabilitation, the European congenital heart and lung exercise group, and the association for European paediatric cardiology. Eur J Prev Cardiol 19:1034–1065
Seghers J, De Baere S, Verloigne M, Cardon G (2018) Results from Flanders’ 2018 report card on physical activity for children and youth. J Phys Act Health 15:S357–S359
Wang T, Chen L, Yang T, Huang P, Wang L, Zhao L, Zhang S, Ye Z, Chen L, Zheng Z (2019) Congenital heart disease and risk of cardiovascular disease: a meta-analysis of cohort studies. J Am Heart Assoc 8:e012030
Giannakoulas G, Dimopoulos K (2010) Exercise training in congenital heart disease: should we follow the heart failure paradigm? Elsevier, Amsterdam
Duppen N, Etnel JR, Spaans L, Takken T, van den Berg-Emons RJ, Boersma E, Schokking M, Dulfer K, Utens EM, Helbing W (2015) Does exercise training improve cardiopulmonary fitness and daily physical activity in children and young adults with corrected tetralogy of Fallot or Fontan circulation? A randomized controlled trial. Am Heart J 170:606–614
Morrison M, Sands A, McCusker C, McKeown P, McMahon M, Gordon J, Grant B, Craig B, Casey F (2013) Exercise training improves activity in adolescents with congenital heart disease. Heart 99:1122–1128
Malina RM, Bouchard C, Bar-Or O (2004) Growth, maturation, and physical activity. Human Kinetics, Champaign
Rhodes J, Curran TJ, Camil L, Rabideau N, Fulton DR, Gauthier NS, Gauvreau K, Jenkins KJ (2006) Sustained effects of cardiac rehabilitation in children with serious congenital heart disease. Pediatrics 118:e586–e593
Duppen N, Takken T, Hopman M, ten Harkel AD, Dulfer K, Utens EM, Helbing WA (2013) Systematic review of the effects of physical exercise training programmes in children and young adults with congenital heart disease. Int J Cardiol 168:1779–1787
Dean PN, Gillespie CW, Greene EA, Pearson GD, Robb AS, Berul CI, Kaltman JR (2015) Sports participation and quality of life in adolescents and young adults with congenital heart disease. Congenit Heart Dis 10:169–179
WH Organization (2011) Global recommendations on physical activity for health: 5–17 years old. World Health Organization, Geneva
Acknowledgements
We would like to express our gratitude to Ilse Coomans from the Pediatric cardiology department for supervising cardiopulmonary exercise test and Lisa Vynckier from the Public health department for field work assistance.
Funding
The authors received no specific funding for this work.
Author information
Authors and Affiliations
Contributions
MZ conceptualized and designed the study, analyzed and interpreted the data, and drafted the initial manuscript; NM and DDW contributed to study conception and design, acquisition of data, interpretation of data, and review and revision of the manuscript. KV, JP, KF, TB, and SDH contributed to study conception and design, interpretation of data, and detailed review and revision of the manuscript, and all authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zaqout, M., Vandekerckhove, K., De Wolf, D. et al. Determinants of Physical Fitness in Children with Repaired Congenital Heart Disease. Pediatr Cardiol 42, 857–865 (2021). https://doi.org/10.1007/s00246-021-02551-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-021-02551-y