Abstract
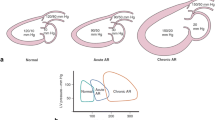
Pulmonary autograft replacement (Ross procedure) is used as an alternative to prosthetic aortic valve replacement patients with aortic valve disease. There are limited data on incidence and risk factors for dilatation and dysfunction of the neo-aortic after the Ross procedure. Ross procedure was performed in 100 patients at our institution between 1993 and 2011. In 76 patients, complete follow-up data were available. Their median age at surgery was 16 (0.4–58) years (76 % males; 95 % with congenital aortic valve disease). Median follow-up duration was 5.2 years (0.3–16.0 years). We analyzed their clinical and echocardiographic follow-up to identify possible risk factors for neo-aortic root dilatation and dysfunction. Ross procedure included reduction plasty of the native ascending aorta in 25 % of patients. During follow-up, 21 patients (28 %) developed neo-aortic root dilatation, 38 patients (50 %) dilatation oft the native ascending aorta and 7 patients (9 %) at least moderate neo-aortic regurgitation. Univariate risk factors for neo-aortic root dilatation were preoperative aortic regurgitation (p = 0.04), concomitant reduction plasty of the ascending aorta (p = 0.009) and a longer duration of follow-up (p = 0.005). Younger age at surgery was associated with dilatation of the ascending aorta (p = 0.03). Reoperation on the neo-aortic root because of severe dilatation was necessary in 6 patients (8 %), where 2 patients had at least moderate neo-aortic root regurgitation. Neo-aortic root and aortic dilatation are common after the Ross procedure. This is often combined with neo-aortic valve dysfunction. Close follow-up of these patients is mandatory.



Similar content being viewed by others
References
Brown JW, Ruzmetov M, Shahriari A et al (2009) Midterm results of Ross aortic valve replacement: a single-institution experience. Ann Thorac Surg 88:601–607 discussion 607–608
Stulak JM, Burkhart HM, Sundt TM 3rd et al (2010) Spectrum and outcome of reoperations after the Ross procedure. Circulation 122:1153–1158
Clark JB, Pauliks LB, Rogerson A et al (2011) The Ross operation in children and young adults: a fifteen-year, single-institution experience. Ann Thorac Surg 91:1936–1942
Takkenberg JJ, Kappetein AP, van Herwerden LA et al (2005) Pediatric autograft aortic root replacement: a prospective follow-up study. Ann Thorac Surg 80:1628–1633
Alhalees Z, Pieters F, Qadoura F et al (2002) The Ross procedure is the procedure of choice for congenital aortic valve disease. J Thorac Cardiovasc Surg 123:437–442
Sievers HH, Stierle U, Charitos EI et al (2010) Major adverse cardiac and cerebrovascular events after the Ross procedure: a report from the German–Dutch Ross registry. Circulation 122:S216–S223
Takkenberg JJ, Klieverik LM, Schoof PH et al (2009) The Ross procedure: a systematic review and meta-analysis. Circulation 119:222–228
Chiappini B, Absil B, Rubay J et al (2007) The Ross procedure: Clinical and echocardiographic follow-up in 219 consecutive patients. Ann Thorac Surg 83:1285–1289
Dave H, Kadner A, Bauersfeld U et al (2003) Early results of using the bovine jugular vein for right ventricular outflow reconstruction during the Ross procedure. Heart Surg Forum 6:390–392
Dave H, Mueggler O, Comber M et al (2011) Risk factor analysis of 170 single-institutional contegra implantations in pulmonary position. Ann Thorac Surg 91:195–302 discussion 202–193
Karamlou T, Ungerleider RM, Alsoufi B et al (2005) Oversizing pulmonary homograft conduits does not significantly decrease allograft failure in children. Eur J Cardio-Thorac Surg 27:548–553
Lang RM, Bierig M, Devereux RB et al (2005) Recommendations for chamber quantification: a report from the american society of echocardiography’s guidelines and standards committee and the chamber quantification writing group, developed in conjunction with the european association of echocardiography, a branch of the european society of cardiology. J Am Soc Echocardiogr 18:1440–1463
Quinones MA, Otto CM, Stoddard M et al (2002) Recommendations for quantification of doppler echocardiography: a report from the doppler quantification task force of the nomenclature and standards committee of the american society of echocardiography. J Am Soc Echocardiogr 15:167–184
Roman MJ, Devereux RB, Kramer-Fox R et al (1989) Two-dimensional echocardiographic aortic root dimensions in normal children and adults. Am J Cardiol 64:507–512
Bonow RO, Carabello BA, Chatterjee K et al (2006) ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the american college of cardiology/american heart association task force on practice guidelines (writing committee to revise the 1998 guidelines for the management of patients with valvular heart disease) developed in collaboration with the society of cardiovascular anesthesiologists endorsed by the society for cardiovascular angiography and interventions and the society of thoracic surgeons. J Am Coll Cardiol 48:e1–e148
Matura LA, Ho VB, Rosing DR et al (2007) Aortic dilatation and dissection in Turner syndrome. Circulation 116:1663–1670
Colan SD, McElhinney DB, Crawford EC et al (2006) Validation and re-evaluation of a discriminant model predicting anatomic suitability for biventricular repair in neonates with aortic stenosis. J Am Coll Cardiol 47:1858–1865
Valeske K, Muller M, Hijjeh N et al (2010) The fate of the pulmonary autograft in the aortic position: experience and results of 98 patients in twelve years. Thorac Cardiovasc Surg 58:334–338
Tan Tanny SP, Yong MS, d’Udekem Y et al (2013) Ross procedure in children: 17-year experience at a single institution. J Am Heart Assoc 2:e000153
Venkataraman R, Vaidyanathan KR, Sankar MN et al (2009) Late dissection of pulmonary autograft treated by valve-sparing aortic root replacement. J Card Surg 24:443–445
Niwa K, Perloff JK, Bhuta SM et al (2001) Structural abnormalities of great arterial walls in congenital heart disease: light and electron microscopic analyses. Circulation 103:393–400
Pees C, Laufer G, Michel-Behnke I (2013) Similarities and differences of the aortic root after arterial switch and Ross operation in children. Am J Cardiol 111:125–130
Arrington CB, Sower CT, Chuckwuk N et al (2008) Absence of TGFBR1 and TGFBR2 mutations in patients with bicuspid aortic valve and aortic dilation. Am J Cardiol 102:629–631
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Financial Support
This study received no specific Grant from any funding agency, commercial or non-for-profit sectors.
Rights and permissions
About this article
Cite this article
Zimmermann, C.A., Weber, R., Greutmann, M. et al. Dilatation and Dysfunction of the Neo-aortic Root and in 76 Patients After the Ross Procedure. Pediatr Cardiol 37, 1175–1183 (2016). https://doi.org/10.1007/s00246-016-1415-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-016-1415-6