Abstract
Purpose
Exposure to prenatal opioids may adversely impact the developing brain networks. The aim of this pilot study was to evaluate alterations in amygdalar functional connectivity in human infants with prenatal opioid exposure.
Methods
In this prospective IRB approved study, we performed resting state functional MRI (rs-fMRI) in 10 infants with prenatal opioid exposure and 12 infants without prenatal drug exposure at < 48 weeks corrected gestational age. Following standard preprocessing, we performed seed-based functional connectivity analysis with the right and left amygdala as the regions of interest after correcting for maternal depression and infant sex. We compared functional connectivity of the amygdala network between infants with and without prenatal opioid exposure.
Results
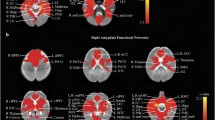
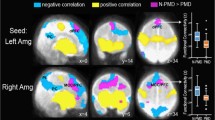
There were significant differences in connectivity of the amygdala seed regions to the several cortical regions including the medial prefrontal cortex in infants who had prenatal opioid exposure when compared with opioid naïve infants.
Conclusion
This finding of increased amygdala functional connectivity in infants with in utero opioid exposure suggests a potential role of maternal opioid exposure on infants’ altered amygdala function. This association with prenatal exposure needs to be replicated in future larger studies.



Similar content being viewed by others
References
Desai RJ, Hernandez-Diaz S, Bateman BT, Huybrechts KF (2014) Increase in prescription opioid use during pregnancy among Medicaid-enrolled women. Obstet Gynecol 123(5):997–1002
Patrick SW, Davis MM, Lehmann CU, Cooper WO (2015) Increasing incidence and geographic distribution of neonatal abstinence syndrome: United States 2009 to 2012. J Perinatol 35(8):650–655
Patrick SW et al (2012) Neonatal abstinence syndrome and associated health care expenditures: United States, 2000-2009. JAMA 307(18):1934–1940
Ross EJ, Graham DL, Money KM, Stanwood GD (2015) Developmental consequences of fetal exposure to drugs: what we know and what we still must learn. Neuropsychopharmacology 40(1):61–87
Romanowicz M, Vande Voort JL, Shekunov J, Oesterle TS, Thusius NJ, Rummans TA, Croarkin PE, Karpyak VM, Lynch BA, Schak KM (2019) The effects of parental opioid use on the parent-child relationship and children’s developmental and behavioral outcomes: a systematic review of published reports. Child Adolesc Psychiatry Ment Health 13:5. https://doi.org/10.1186/s13034-019-0266-3
Nygaard E, Slinning K, Moe V, Due-Tønnessen P, Fjell A, Walhovd KB (2018) Neuroanatomical characteristics of youths with prenatal opioid and poly-drug exposure. Neurotoxicol Teratol 68:13–26
Mayes LC, Granger RH, Bornstein MH, Zuckerman B (1992) The problem of prenatal cocaine exposure. A rush to judgment. JAMA 267(3):406–408
Upton MN, Smith GD, McConnachie A, Hart CL, Watt GCM (2004) Maternal and personal cigarette smoking synergize to increase airflow limitation in adults. Am J Respir Crit Care Med 169(4):479–487
Stroud LR, Paster RL, Goodwin MS, Shenassa E, Buka S, Niaura R, Rosenblith JF, Lipsitt LP (2009) Maternal smoking during pregnancy and neonatal behavior: a large-scale community study. Pediatrics 123(5):e842–e848
Treit S, Lebel C, Baugh L, Rasmussen C, Andrew G, Beaulieu C (2013) Longitudinal MRI reveals altered trajectory of brain development during childhood and adolescence in fetal alcohol spectrum disorders. J Neurosci 33(24):10098–10109
Grewen K, Salzwedel AP, Gao W (2015) Functional connectivity disruption in neonates with prenatal marijuana exposure. Front Hum Neurosci 9:601
Salzwedel AP, Grewen KM, Vachet C, Gerig G, Lin W, Gao W (2015) Prenatal drug exposure affects neonatal brain functional connectivity. J Neurosci 35(14):5860–5869
Walhovd KB, Watts R, Amlien I, Woodward LJ (2012) Neural tract development of infants born to methadone-maintained mothers. Pediatr Neurol 47(1):1–6
Yuan Q et al (2014) Do maternal opioids reduce neonatal regional brain volumes? A pilot study. J Perinatol 34(12):909–913
Bier JB, Finger AS, Bier BA, Johnson TA, Coyle MG (2015) Growth and developmental outcome of infants with in-utero exposure to methadone vs buprenorphine. J Perinatol 35(8):656–659
Jenkinson M, Beckmann CF, Behrens TEJ, Woolrich MW, Smith SM (2012) Fsl. Neuroimage 62(2):782–790
Smith SM (2002) Fast robust automated brain extraction. Hum Brain Mapp 17(3):143–155
Chao-Gan Y, Yu-Feng Z (2010) DPARSF: a MATLAB toolbox for “pipeline” data analysis of resting-state fMRI. Front Syst Neurosci 4:13
Andersson J, Skare S (2003) How to correct susceptibility distortions in spin-echo echo-planar images: application to diffusion tensor imaging. NeuroImage 20:870–888
Jenkinson M, Bannister P, Brady M, Smith S (2002) Improved optimization for the robust and accurate linear registration and motion correction of brain images. NeuroImage 17:825–841
Power JD, Barnes KA, Snyder AZ, Schlaggar BL, Petersen SE (2012) Spurious but systematic correlations in functional connectivity MRI networks arise from subject motion. Neuroimage 59(3):2142–2154
Shi F, Yap PT, Wu G, Jia H, Gilmore JH, Lin W, Shen D (2011) Infant brain atlases from neonates to 1- and 2-year-olds. PLoS One 6(4):e18746
Avants B et al (2011) A reproducible evaluation of ANTs similarity metric performance in brain image registration. Neuroimage 54:2033–2044
Biswal B, Zerrin Yetkin F, Haughton VM, Hyde JS (1995) Functional connectivity in the motor cortex of resting human brain using echo-planar MRI. Magn Reson Med 34(4):537–541
Simons LE, Pielech M, Erpelding N, Linnman C, Moulton E, Sava S, Lebel A, Serrano P, Sethna N, Berde C, Becerra L, Borsook D (2014) The responsive amygdala: treatment-induced alterations in functional connectivity in pediatric complex regional pain syndrome. Pain 155(9):1727–1742
Sakaki M, Nga L, Mather M (2013) Amygdala functional connectivity with medial prefrontal cortex at rest predicts the positivity effect in older adults' memory. J Cogn Neurosci 25(8):1206–1224
Konijnenberg C, Melinder A (2015) Executive function in preschool children prenatally exposed to methadone or buprenorphine. Child Neuropsychol 21(5):570–585
Schweitzer JB, Riggins T, Liang X, Gallen C, Kurup PK, Ross TJ, Black MM, Nair P, Salmeron BJ (2015) Prenatal drug exposure to illicit drugs alters working memory-related brain activity and underlying network properties in adolescence. Neurotoxicol Teratol 48:69–77
Graham AM, Rasmussen JM, Entringer S, Ben Ward E, Rudolph MD, Gilmore JH, Styner M, Wadhwa PD, Fair DA, Buss C (2019) Maternal cortisol concentrations during pregnancy and sex-specific associations with neonatal amygdala connectivity and emerging internalizing behaviors. Biol Psychiatry 85(2):172–181
Graham AM, Rasmussen JM, Rudolph MD, Heim CM, Gilmore JH, Styner M, Potkin SG, Entringer S, Wadhwa PD, Fair DA, Buss C (2018) Maternal systemic interleukin-6 during pregnancy is associated with newborn amygdala phenotypes and subsequent behavior at 2 years of age. Biol Psychiatry 83(2):109–119
Rotem-Kohavi N et al (2019) Hub distribution of the brain functional networks of newborns prenatally exposed to maternal depression and SSRI antidepressants. Depress Anxiety
Funding
RR was supported by the American Roentgen Ray Scholarship Award 2018 and Radiological Society of North America Seed Grant 2018. SS and RR were supported by the Eunice Kennedy Shriver National Institute of Child Health & Human Development of the National Institutes of Health under Award, R01HD096800 (PI: Sadhasivam). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study. For minor participants, informed consent was obtained from the guardian.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Radhakrishnan, R., Elsaid, N.M.H., Sadhasivam, S. et al. Resting state functional MRI in infants with prenatal opioid exposure—a pilot study. Neuroradiology 63, 585–591 (2021). https://doi.org/10.1007/s00234-020-02552-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-020-02552-3