Abstract
Introduction
Brain herniations (BH) into arachnoid granulations (AG) in dural venous sinuses and calvarium have rarely been reported in the literature.
Methods
MRIs of 38 patients with BH into AG (BHAG) were retrospectively analyzed. Locations of BHAG, gyrus/lobe of the herniated brain, parenchymal abnormalities of the BH, and clinical and radiological conditions with raised intracranial pressure were recorded.
Results
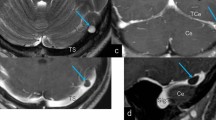
Sixty-eight BHAG were found, by order of frequency, in the occipital squama (OS), transverse sinus (TS), lateral lacuna of the superior sagittal sinus (LLSSS), and straight sinus (SS), with cerebellar tissue being the most frequently involved in BHAG (94.5 % of OS, 55 % of TS, 100 % SS BHAG). Multiple BHAG were found in 58 % of the patients (up to five per patient). Parenchymal signal and structural changes (SSCG) were observed in 46 % of BHAG (100 % were cerebellar). Three patients had pseudotumor cerebri (PTCS); one patient had only MRI signs of PTCS. Twenty-one percent of patients had intracranial conditions susceptible of increasing cerebrospinal fluid (CSF) pressure other than PTCS.
Conclusions
BHAG occurred in the OS, TS, LLSSS, and the SS. SSCG of the herniated cerebellum were frequent and possibly result from tethering/strangulation in the AG. No symptoms could be clearly attributed to BHAG, though in three cases of PTCS, TS BHAG could have contributed to sustaining the raised CSF pressure. Various factors are probably involved in the development of BHAG including normal pia-arachnoid bridges between the brain surface and the AG, hydrodynamic constrains on the brain and AG, and, in some cases, increased intracranial pressure.






Similar content being viewed by others
Abbreviations
- AG:
-
Arachnoid granulation
- BH:
-
Brain herniation
- BHAG:
-
Brain herniation into an AG
- ITG:
-
Inferior temporal gyrus
- ISL:
-
Inferior semilunar lobule
- L:
-
Left
- LLSSS:
-
Lateral lacunae of the SSS
- LOTG:
-
Lateral occipito-temporal gyrus
- NC-CT:
-
Non-contrast CT
- OS:
-
Occipital squama
- PC-CT:
-
Post-contrast CT
- PTCS:
-
Pseudotumor cerebri syndrome
- R:
-
Right
- SiS:
-
Sigmoid sinus
- SS:
-
Straight sinus
- SSCG:
-
Signal and structural changes
- SSL:
-
Superior semilunar lobule
- SSS:
-
Superior sagittal sinus
- TS:
-
Transverse sinus
References
Faivre EJ (1853) Les granulations méningiennes. Ecole de Médecine de Paris, Paris
Trolard P (1892) Les granulations de Pacchioni. Les lacunes veineuses de la dure-mère. J de l’anatomie et de la physiologie normales et pathologiques de l’homme et des animaux 28:28–57/172–210
Turner L (1961) The structure of arachnoid granulations with observations on their physiological and pathological significance. Ann R Coll Surg Engl 29:237–264
Basmajian JV (1952) The depressions for the arachnoid granulations as a criterion of age. Anat Rec 112(4):843–846
Le Gros Clark WE (1920) On the pacchionian bodies. J Anat 55:40–48
Trolard P (1890) Les veines méningées moyennes. Rev Sci Biol 485–499
Wolbach SB (1908) Multiple hernias of the cerebrum and cerebellum, due to intracranial pressure. J Med Res 19(1):153–174 157
Cooper ER (1958) Arachnoid granulations in man. Acta Anat (Basel) 34(3):187–200
Cooper ER (1960) Further studies of arachnoid granulations in man. Acta Anat (Basel) 42:88–104
Gailloud P, Muster M, Khaw N, Martin JB, Murphy KJ, Fasel JH, Rufenacht DA (2001) Anatomic relationship between arachnoid granulations in the transverse sinus and the termination of the vein of Labbe: an angiographic study. Neuroradiology 43(2):139–143
Grzybowski DM, Herderick EE, Kapoor KG, Holman DW, Katz SE (2007) Human arachnoid granulations part I: a technique for quantifying area and distribution on the superior surface of the cerebral cortex. Cerebrospinal Fluid Res 4:6. doi:10.1186/1743-8454-4-6
Grossman CB, Potts DG (1974) Arachnoid granulations: radiology and anatomy. Radiology 113(1):95–100. doi:10.1148/113.1.95
Branan R, Wilson CB (1976) Arachnoid granulations simulating osteolytic lesions of the calvarium. AJR Am J Roentgenol 127(3):523–525. doi:10.2214/ajr.127.3.523
Rosenberg AE, O’Connell JX, Ojemann RG, Plata MJ, Palmer WE (1993) Giant cystic arachnoid granulations: a rare cause of lytic skull lesions. Hum Pathol 24(4):438–441
Esposito G, Della Pepa GM, Sturiale CL, Gaudino S, Anile C, Pompucci A (2011) Hypertrophic arachnoid granulation of the occipital bone: neuroradiological differential diagnosis. Clin Neuroradiol 21(4):239–243. doi:10.1007/s00062-011-0059-4
Tural Emon S, Orakdogen M, Akpinar E, Hakan T, Zafer Berkman M (2012) Arachnoid granulations: a rare cause of lytic occipital bone lesion. Neurol Neurochir Pol 46(6):603–606
Alonso RC, de la Pena MJ, Caicoya AG, Rodriguez MR, Moreno EA, de Vega Fernandez VM (2013) Spontaneous skull base meningoencephaloceles and cerebrospinal fluid fistulas. Radiographics 33(2):553–570. doi:10.1148/rg.332125028
Connor SE (2010) Imaging of skull-base cephalocoeles and cerebrospinal fluid leaks. Clin Radiol 65(10):832–841. doi:10.1016/j.crad.2010.05.002
San Millan D, Kohler R (2014) Enlarged CSF spaces in pseudotumor cerebri. AJR Am J Roentgenol 203(4):W457–W458. doi:10.2214/AJR.14.12787
Owler BK, Parker G, Halmagyi GM, Johnston IH, Besser M, Pickard JD, Higgins JN (2005) Cranial venous outflow obstruction and pseudotumor cerebri syndrome. Adv Tech Stand Neurosurg 30:107–174
Kollar C, Johnston I, Parker G, Harper C (1998) Dural arteriovenous fistula in association with heterotopic brain nodule in the transverse sinus. AJNR Am J Neuroradiol 19(6):1126–1128
Liang L, Korogi Y, Sugahara T, Ikushima I, Shigematsu Y, Takahashi M, Provenzale JM (2002) Normal structures in the intracranial dural sinuses: delineation with 3D contrast-enhanced magnetization prepared rapid acquisition gradient-echo imaging sequence. AJNR Am J Neuroradiol 23(10):1739–1746
Karatag O, Cosar M, Kizildag B, Sen HM (2013) Dural sinus filling defect: intrasigmoid encephalocele. BMJ Case Rep. doi:10.1136/bcr-2013-201616
Chan WC, Lai V, Wong YC, Poon WL (2011) Focal brain herniation into giant arachnoid granulation: a rare occurrence. Eur Radiol Radiol Extra 78:e111–e113
Kocyigit A, Herek D, Balci YI (2015) Focal herniation of cerebral parenchyma into transverse sinus. J Neuroradiol 42(2):126–127. doi:10.1016/j.neurad.2014.05.009
Battal B, Castillo M (2014) Brain herniations into the dural venous sinuses or calvarium: MRI of a recently recognized entity. Neuroradiol J 27(1):55–62
Coban G, Yildirim E, Horasanli B, Cifci BE, Agildere M (2013) Unusual cause of dizziness: occult temporal lobe encephalocele into transverse sinus. Clin Neurol Neurosurg 115(9):1911–1913. doi:10.1016/j.clineuro.2013.05.032
Asadi H, Morokoff A, Gaillard F (2015) Occult temporal lobe encephalocoele into the transverse sinus. J Clin Neurosci 22(7):1202–1204. doi:10.1016/j.jocn.2015.01.020
Battal B, Hamcan S, Akgun V, Sari S, Oz O, Tasar M, Castillo M (2015) Brain herniations into the dural venous sinus or calvarium: MRI findings, possible causes and clinical significance. Eur Radiol. doi:10.1007/s00330-015-3959-x
Tokiguchi S, Kurashima A, Ito J, Takahashi H, Shimbo Y (1988) Fat in the dural sinus—CT and anatomical correlations. Neuroradiology 30(1):78–80
Browder J, Browder A, Kaplan HA (1972) Benign tumors of the cerebral dural sinuses. J Neurosurg 37(5):576–579. doi:10.3171/jns.1972.37.5.0576
Trolard P (1890) De quelques particularités de la dure mère. Journal de l’anatomie et de la physiologie normales et pathologiques de l’homme et des animaux 26:407–418
Saavalainen T, Jutila L, Mervaala E, Kalviainen R, Vanninen R, Immonen A (2015) Temporal anteroinferior encephalocele: an underrecognized etiology of temporal lobe epilepsy? Neurology 85(17):1467–1474. doi:10.1212/WNL.0000000000002062
Durcan FJ, Corbett JJ, Wall M (1988) The incidence of pseudotumor cerebri. Population studies in Iowa and Louisiana. Arch Neurol 45(8):875–877
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
We declare that while all patients gave informed consent for imaging studies, due to the retrospective nature of this work, Institutional Review Board approval was not required.
Conflict of interest
We declare that we have no conflict of interest.
Rights and permissions
About this article
Cite this article
Malekzadehlashkariani, S., Wanke, I., Rüfenacht, D.A. et al. Brain herniations into arachnoid granulations: about 68 cases in 38 patients and review of the literature. Neuroradiology 58, 443–457 (2016). https://doi.org/10.1007/s00234-016-1662-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-016-1662-5