Abstract
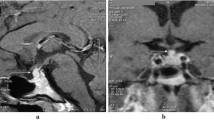
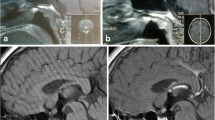
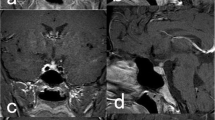
Langerhans cell histiocytosis (LCH) is a rare, systemic disease caused by monoclonal expansion of dendritic cells that shows a particular predilection for the hypothalamic–pituitary system (HPS). We studied the function (anterior and posterior pituitary hormonal secretion) and morphology using magnetic resonance imaging (MRI) of the HPS in 17 adult patients (seven males, median age 35 years, range 18–59 years) with multisystem LCH. We also evaluated the evolution of structural HPS abnormalities in relation to pituitary function and response to treatment in 12 of these patients during a median follow-up period of 3.75 years (range 1.5–10 years). Of the 17 patients, 14 (82%) had abnormal HPS imaging, and 12 (70%) had more than one area involved. Lack of the bright spot of the posterior pituitary lobe was typically found in all patients with the diagnosis of diabetes insipidus (DI). Eight patients (47%) had infundibular enlargement, six (35%) pituitary infiltration, four (24%) partially or completely empty sella, three (18%) hypothalamic involvement, and two (12%) infundibular atrophy. DI was found in 16 patients (94%) and anterior pituitary hormonal deficiency (APHD) in 10 patients (59%); two patients had single (12%) and 8 (47%) multiple APHD. During the follow-up period there was improvement of the initially demonstrated HPS pathology in seven (47%) patients, and five (33%) of them had received at least one form of treatment. APHD and DI persisted in all patients except in one in whom established gonadotrophin deficiency recovered. In summary, DI and APHD are very common in patients with multisystem LCH and are almost always associated with abnormal HPS imaging.




Similar content being viewed by others
References
Arceci RJ (1999) The histiocytoses: the fall of the Tower of Babel. Eur J Cancer 35:747–767
Arico M, Nichols K, Whitlock JA, et al (1999) Familial clustering of Langerhans cell histiocytosis. Br J Haematol 107:883–888
Carstensen H, Ornvold K (1993) The epidemiology of Langerhans cell histiocytosis in children in Denmark 1975–89. Med Pediatr Oncol 21:387–388
Broadbent V, Egeler RM, Nesbit ME (1994) Langerhans cell histiocytosis—clinical and epidemiological aspects. Br J Cancer 70 [Suppl XXIII]:S11–S16
Schmitz L, Favara BE (1998) Nosology and pathology of Langerhans cell histiocytosis. Hematol Oncol Clin North Am 12:221–246
Yu RC, Chu C, Buluwela L, Chu AC (1994) Clonal proliferation of Langerhans cells in Langerhans cell histiocytosis. Lancet 343:767–768
Broadbent V, Gadner H (1998) Current therapy for Langerhans cell histiocytosis. Hematol Oncol Clin North Am 12:327–338
Ceci A, de Terlizzi M, Colella R, et al (1993) Langerhans cell histiocytosis in childhood: results from the Italian Cooperative AIEOP-CNR-H.X ’83 study. Med Pediatr Oncol 21:259–264
Ceci A, de Terlizzi M, Colella R, et al (1988) Etoposide in recurrent childhood Langerhans’ cell histiocytosis: an Italian cooperative study. Cancer 62:2528–2531
Gadner H, Ladisch S, Arico M, et al (1994) VP-16 and the treatment of histiocytosis. Eur J Pediatr 153(5):389
Komp DM, Herson J, Starling KA, Vietti TJ, Hvizdala E (1981) A staging system for histiocytosis X: a Southwest Oncology Group Study. Cancer 47:798–800
Lahey E (1975) Histiocytosis x—an analysis of prognostic factors. J Pediatr 87:184–189
Arico M, Egeler R (1998) Clinical aspects of Langerhans cell histiocytosis. Hematol Oncol Clin North Am 12:247–258
Kaltsas GA, Powles TB, Evanson J, et al (2000) Hypothalamo-pituitary abnormalities in adult patients with Langerhans cell histiocytosis: clinical, endocrinological, and radiological features and response to treatment. J Clin Endocrinol Metab 85:1370–1376
Dunger DB, Broadbent V, Yeoman E, et al (1989) The frequency and natural history of diabetes insipidus in children with Langerhans-cell histiocytosis. N Engl J Med 321:1157–1162
Grois N, Favara B, Mostbeck H, Prayer D (1998) Central nervous disease in Langerhans cell histiocytosis. Hematol Oncol Clin North Am 12:287–305
Malpas J (1998) Langerhans cell histiocytosis in adults. Hematol Oncol Clin North Am 12:259–268
Willis B, Ablin A, Weinberg V, et al (1996) Disease course and late sequelae of Langerhans’ cell histiocytosis: 25-year experience at the University of California, San Francisco. J Clin Oncol 14:2073–2082
Braier J, Chantada G, Rosso D, et al (1999) Langerhans cell histiocytosis: retrospective evaluation of 123 patients at a single institution. Pediatr Hematol Oncol 16:377–385
The French Langerhans’ Cell Histiocytosis Study Group (1996) A multicentre retrospective survey of Langerhans’ cell histiocytosis: 348 cases observed between 1983 and 1993. Arch Dis Child 75:17–24
Howarth DM, Gilchrist GS, Mullan BP, et al (1999) Langerhans cell histiocytosis: diagnosis, natural history, management, and outcome. Cancer 85:2278–2290
Arico M, Girschikofsky M, Genereau T, et al (2003) Langerhans cell histiocytosis in adults. Report from the International Registry of the Histiocyte Society. Eur J Cancer 39:2341–2348
Braunstein GD, Kohler PO (1972) Pituitary function in Hand-Schuller Christian disease. N Engl J Med 286:1225–1229
Hanna CE, LaFranchi SH (1983) Evolving hypopituitarism in children with central nervous system lesions. Pediatrics 72:65–70
Ahmed M (1993) Endocrine abnormalities in patients with Langerhans cell histiocytosis (abstract). Proceedings of the 75th Annual Meeting of the Endocrine Society, p 73
Broadbent V, Dunger D, Yeomans E, Kendall B (1993) Anterior pituitary function and computed tomography/magnetic resonance imaging in patients with Langerhans cell histiocytosis and diabetes insipidus. Med Pediatr Oncol 21:649–654
Grois N, Prayer D, Prosch H, et al (2004) Course and clinical impact of magnetic resonance imaging findings in diabetes insipidus associated with Langerhans cell histiocytosis. Pediatr Blood Cancer 43:59–65
Maghnie M, Villa A, Arico M, et al (1992) Correlation between magnetic resonance imaging of posterior pituitary and neurohypophyseal function in children with diabetes insipidus. J Clin Endocrinol Metab 74:795–800
Mootha SL, Barkovich AJ, Grumbach MM, et al (1997) Idiopathic hypothalamic diabetes insipidus, pituitary stalk thickening, and the occult intracranial germinoma in children and adolescents. J Clin Endocrinol Metab 82:1362–1367
Tien R, Newton HT, McDermott MW, Dillon WP, Kucharsky J (1990) Thickened pituitary stalk on MR images in patients with diabetes insipidus and Langerhans cell histiocytosis. AJNR Am J Neuroradiol 11:703–708
Hartman ML, Crowe BJ, Biller BM, et al (2002) Which patients do not require a GH stimulation test for the diagnosis of adult GH deficiency? J Clin Endocrinol Metab 87:477–485
Elster AD (1993) Modern imaging of the pituitary. Radiology 187:1–14
Gardner H, Heitger A, Grois N, Gatterer-Menz I, Ladisch S (1994) Treatment strategy for disseminated Langerhans cell histiocytosis. Med Pediatr Oncol 23:72–80
Maghnie M, Genovese E, Arico M, et al (1994) Evolving pituitary hormone deficiency is associated with pituitary vasculopathy: dynamic MR study in children with hypopituitarism, diabetes insipidus and Langerhans cell histiocytosis. Radiology 193:493–499
Scherbaum WA, Wass JA, Besser GM, Bottazo GF, Doniach D (1986) Autoimmune cranial diabetes insipidus: its association with other endocrine diseases and with histiocytosis X. Clin Endocrinol (Oxf) 25:411–420
Kilpatrick SE, Wenger DE, Gilchrist GS, et al (1995) Langerhans’ cell histiocytosis (histiocytosis X) of bone. Cancer 76:2471–2484
LCH-A1 Study Committee (2004) Langerhans cell histiocytosis in adults: treatment protocol of the first international study
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Makras, P., Samara, C., Antoniou, M. et al. Evolving radiological features of hypothalamo-pituitary lesions in adult patients with Langerhans cell histiocytosis (LCH). Neuroradiology 48, 37–44 (2006). https://doi.org/10.1007/s00234-005-0011-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-005-0011-x