Abstract
Background
Alzheimer’s disease is an age-related neurodegenerative disorder characterized clinically by a progressive loss of memory and cognitive functions resulting in severe dementia. Ipriflavone (IPRI) is a non-hormonal, semi-synthetic isoflavone, clinically used in some countries for the treatment and prevention of postmenopausal osteoporosis. Moreover, ipriflavone is a non-peptidomimetic small molecule AChE inhibitor with an improved bioavailability after systemic administration, due to its efficient blood-brain barrier permeability in comparison with peptidomimetic inhibitors.
Objective
The present study aimed to evaluate the possible enhancing effects of IPRI on memory impairments caused by scopolamine administration.
Methods
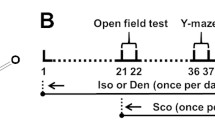
Male rats were administered IPRI (50 mg/kg, oral) 2 h before scopolamine injection (2 mg/kg, intraperitoneally injected) daily for 4 weeks. Effects of IPRI on acetylcholinesterase activity, amyloid-β precursor processing, and neuroplasticity in the rats’ hippocampus were investigated.
Results
Daily administration of IPRI reverted memory impairment caused by scopolamine as measured by the reduction of the escape latency. IPRI significantly alleviated the oxidative stress and restored the mRNA expression of both cAMP-response element-binding protein and brain-derived neurotrophic factor in the hippocampus. Furthermore, it significantly increased the expression of ADAM10 and ADAM17 (two putative α-secretase enzymes) and phosphorylated extracellular signal-regulated kinase 1/2 (pERK1/2) that associated with decreased expression of β-secretase (BACE) in the hippocampus. Finally, both the amyloid-β (Aβ) and Tau pathologies were reduced.
Conclusions
IPRI showed promising neuroprotective effects against scopolamine-induced memory dysfunction in rats. These findings contributed to the stimulation of α-secretase enzymes, the activation of MAPK/ERK1/2, and the alleviation of oxidative stress.











Similar content being viewed by others
References
Aid T, Kazantseva A, Piirsoo M, Palm K, Timmusk T (2007) Mouse and rat BDNF gene structure and expression revisited. J Neurosci Res 85:525–535
Ali SK, Hamed AR, Soltan MM, Hegazy UM, Elgorashi EE, El-Garf IA, Hussein AA (2013) In-vitro evaluation of selected Egyptian traditional herbal medicines for treatment of Alzheimer disease. BMC Complement Altern Med 13:121. doi:10.1186/1472-6882-13-121
Arjmandi BH, Juma S, Sohn E, Schaefer R, Goyal N, Getlinger MJ (1995) Effects of ovariectomy, estrogen, and ipriflavone on liver lipids and cholesterol in a rat model. J Am Diet Assoc 95(9):A9. doi:10.1016/S0002-8223(95)00387-8
Arjmandi BH, Khan DA, Juma SS, Svanborg A (1997) The ovarian hormone deficiency-induced hypercholesterolemia is reversed by soy protein and the synthetic isoflavone, ipriflavone. Nutr Res 17(5):885–894. doi:10.1016/S0271-5317(97)00055-9
Bachurin SO, Bovina EV, Ustyugov AA (2017) Drugs in clinical trials for Alzheimer’s disease: the major trends. Med Res Rev. doi:10.1002/med.21434
Bajda M, Guzior N, Ignasik M, Malawska B (2011) Multi-target-directed ligands in Alzheimer’s disease treatment. Curr Med Chem 18(32):4949–4975
Bakhshalian N, Johnson SA, Hooshmand S, Feresin RG, Elam ML, Soung do Y et al (2014) Dietary phosphorus exacerbates bone loss induced by cadmium in ovariectomized rats. Menopause 21(12):1292–1297. doi:10.1097/GME.0000000000000241
Belcavello L, Vencioneck Dutra JC, de Freitas JV, Aranha IP, do Carmo Pimentel Batitucci M (2012) Mutagenicity of ipriflavone in vivo and in vitro. Food Chem Toxicol 50(3–4):996–1000. doi:10.1016/j.fct.2011.12.013
Bhat AH, Dar KB, Anees S, Zargar MA, Masood A, Sofi MA, Ganie SA (2015) Oxidative stress, mitochondrial dysfunction and neurodegenerative diseases; a mechanistic insight. Biomed Pharmacother 74:101–110. doi:10.1016/j.biopha.2015.07.025
Bihaqi SW, Singh AP, Tiwari M (2012) Supplementation of convolvulus pluricaulis attenuates scopolamine-induced increased Tau and amyloid precursor protein (AbetaPP) expression in rat brain. Indian J Pharmacol 44(5):593–598. doi:10.4103/0253-7613.100383
Bimonte-Nelson HA, Granholm AC, Nelson ME, Moore AB (2008) Patterns of neurotrophin protein levels in male and female Fischer 344 rats from adulthood to senescence: how young is “young” and how old is “old”? Exp Aging Res 34(1):13–26. doi:10.1080/03610730701761908
Blake MG, Krawczyk MC, Baratti CM, Boccia MM (2014) Neuropharmacology of memory consolidation and reconsolidation: insights on central cholinergic mechanisms. J Physiol Paris 108(4–6):286–291. doi:10.1016/j.jphysparis.2014.04.005
Budzynska B, Boguszewska-Czubara A, Kruk-Slomka M, Skalicka-Wozniak K, Michalak A, Musik I, Biala G (2015) Effects of imperatorin on scopolamine-induced cognitive impairment and oxidative stress in mice. Psychopharmacology 232(5):931–942. doi:10.1007/s00213-014-3728-6
Canerina-Amaro A, Hernandez-Abad LG, Ferrer I, Quinto-Alemany D, Mesa-Herrera F, Ferri C et al (2017) Lipid raft ER signalosome malfunctions in menopause and Alzheimer’s disease. Front Biosci (Schol Ed) 9:111–126
Castro A, Martinez A (2006) Targeting beta-amyloid pathogenesis through acetylcholinesterase inhibitors. Curr Pharm Des 12(33):4377–4387
Chen W, Cheng X, Chen J, Yi X, Nie D, Sun X et al (2014) Lycium barbarum Polysaccharides prevent memory and neurogenesis impairments in scopolamine-treated rats. PLoS One 9(2):e88076. doi:10.1371/journal.pone.0088076
Cheung ZH, Ip NY (2012) Cdk5: a multifaceted kinase in neurodegenerative diseases. Trends Cell Biol 22(3):169–175. doi:10.1016/j.tcb.2011.11.003
Chhetri J, King AE, Gueven N (2017) Alzheimer’s disease and NQO1: is there a link? Curr Alzheimer Res. doi:10.2174/1567205014666170203095802
Chiu DT, Stults FH, Tappel AL (1976) Purification and properties of rat lung soluble glutathione peroxidase. Biochim Biophys Acta 445(3):558–566
Cui J, Shen Y, Li R (2013) Estrogen synthesis and signaling pathways during aging: from periphery to brain. Trends Mol Med 19(3):197–209. doi:10.1016/j.molmed.2012.12.007
Delarmelina JM, Dutra JC, Batitucci Mdo C (2014) Antimutagenic activity of ipriflavone against the DNA-damage induced by cyclophosphamide in mice. Food Chem Toxicol 65:140–146. doi:10.1016/j.fct.2013.12.028
Deroo BJ, Korach KS (2006) Estrogen receptors and human disease. J Clin Invest 116(3):561–570. doi:10.1172/JCI27987
Doguc DK, Delibas N, Vural H, Altuntas I, Sutcu R, Sonmez Y (2012) Effects of chronic scopolamine administration on spatial working memory and hippocampal receptors related to learning. Behav Pharmacol 23(8):762–770. doi:10.1097/FBP.0b013e32835a38af
Dong HK, Gim JA, Yeo SH, Kim HS (2017) Integrated late onset Alzheimer’s disease (LOAD) susceptibility genes: cholesterol metabolism and trafficking perspectives. Gene 597:10–16. doi:10.1016/j.gene.2016.10.022
Duan Y, Dong S, Gu F, Hu Y, Zhao Z (2012) Advances in the pathogenesis of Alzheimer’s disease: focusing on Tau-mediated neurodegeneration. Transl Neurodegener 1(1):24. doi:10.1186/2047-9158-1-24
El-Khadragy MF, Al-Olayan EM, Abdel Moneim AE (2014) Neuroprotective effects of Citrus reticulata in scopolamine-induced dementia oxidative stress in rats. CNS Neurol Disord Drug Targets 13(4):684–690
El-Sherbiny DA, Khalifa AE, Attia AS, Eldenshary Eel D (2003) Hypericum perforatum extract demonstrates antioxidant properties against elevated rat brain oxidative status induced by amnestic dose of scopolamine. Pharmacol Biochem Behav 76(3–4):525–533
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82(1):70–77
Ellman GL, Courtney KD, Andres V Jr, Feather-Stone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95
Fassbender K, Simons M, Bergmann C, Stroick M, Lutjohann D, Keller P et al (2001) Simvastatin strongly reduces levels of Alzheimer’s disease beta-amyloid peptides Abeta 42 and Abeta 40 in vitro and in vivo. Proc Natl Acad Sci U S A 98(10):5856–5861. doi:10.1073/pnas.081620098
Ghareeb DA, Newairy AA, El-Rashidy FH, Hussein HM, Ali AN (2010) Efficacy of natural extracts of Ginkgo biloba and berberry and a synthetic derivative of Genistein (ipriflavone), as acetylcholinesterase inhibitors, comparative study with Aricept® effect. J Biochem Biotechnol 1(1):5–11
Gillies GE, McArthur S (2010) Estrogen actions in the brain and the basis for differential action in men and women: a case for sex-specific medicines. Pharmacol Rev 62(2):155–198. doi:10.1124/pr.109.002071
Habig WH, Pabst MJ, Jakoby WB (1974) Glutathione S-transferases. The first enzymatic step in mercapturic acid formation. J Biol Chem 249(22):7130–7139
Haughey NJ, Bandaru VV, Bae M, Mattson MP (2010) Roles for dysfunctional sphingolipid metabolism in Alzheimer’s disease neuropathogenesis. Biochim Biophys Acta 1801(8):878–886. doi:10.1016/j.bbalip.2010.05.003
Hernández-Zimbrón LF, Gorostieta-Salas E, Díaz-Hung M-L, Pérez-Garmendia R, Gevorkian G, Quiroz-Mercado H (2016) Beta amyloid peptides: extracellular and intracellular mechanisms of clearance in Alzheimer’s disease
Hong IS, Lee HY, Kim HP (2014) Anti-oxidative effects of rooibos tea (Aspalathus linearis) on immobilization-induced oxidative stress in rat brain. PLoS One 9(1):e87061. doi:10.1371/journal.pone.0087061
Kalaria RN, Maestre GE, Arizaga R, Friedland RP, Galasko D, Hall K, World Federation of Neurology Dementia Research Group (2008) Alzheimer’s disease and vascular dementia in developing countries: prevalence, management, and risk factors. Lancet Neurol 7(9):812–826. doi:10.1016/S1474-4422(08)70169-8
Kim EK, Choi EJ (2010) Pathological roles of MAPK signaling pathways in human diseases. Biochim Biophys Acta 1802(4):396–405. doi:10.1016/j.bbadis.2009.12.009
Kojro E, Gimpl G, Lammich S, Marz W, Fahrenholz F (2001) Low cholesterol stimulates the nonamyloidogenic pathway by its effect on the alpha-secretase ADAM 10. Proc Natl Acad Sci U S A 98(10):5815–5820. doi:10.1073/pnas.081612998
Konar A, Shah N, Singh R, Saxena N, Kaul SC, Wadhwa R, Thakur MK (2011) Protective role of Ashwagandha leaf extract and its component withanone on scopolamine-induced changes in the brain and brain-derived cells. PLoS One 6(11):e27265. doi:10.1371/journal.pone.0027265
Kulkarni KS, Kasture SB, Mengi SA (2010) Efficacy study of Prunus amygdalus (almond) nuts in scopolamine-induced amnesia in rats. Indian J Pharmacol 42(3):168–173. doi:10.4103/0253-7613.66841
Lee B, Park J, Kwon S, Park MW, Oh SM, Yeom MJ et al (2010) Effect of wild ginseng on scopolamine-induced acetylcholine depletion in the rat hippocampus. J Pharm Pharmacol 62(2):263–271. doi:10.1211/jpp.62.02.0015
Lee B, Sur B, Shim I, Lee H, Hahm DH (2012) Phellodendron amurense and its major alkaloid compound, berberine ameliorates scopolamine-induced neuronal impairment and memory dysfunction in rats. Korean J Physiol Pharmacol 16(2):79–89. doi:10.4196/kjpp.2012.16.2.79
Lee B, Sur B, Shim J, Hahm DH, Lee H (2014) Acupuncture stimulation improves scopolamine-induced cognitive impairment via activation of cholinergic system and regulation of BDNF and CREB expressions in rats. BMC Complement Altern Med 14:338. doi:10.1186/1472-6882-14-338
Lee JS, Kim HG, Lee HW, Han JM, Lee SK, Kim DW et al (2015) Hippocampal memory enhancing activity of pine needle extract against scopolamine-induced amnesia in a mouse model. Sci Rep 5:9651. doi:10.1038/srep09651
Lenz RA, Baker JD, Locke C, Rueter LE, Mohler EG, Wesnes K et al (2012) The scopolamine model as a pharmacodynamic marker in early drug development. Psychopharmacology 220(1):97–107. doi:10.1007/s00213-011-2456-4
Li W, He QZ, Wu CQ, Pan XY, Wang J, Tan Y et al (2015) PFOS disturbs BDNF-ERK-CREB Signalling in association with increased MicroRNA-22 in SH-SY5Y cells. Biomed Res Int 2015:302653. doi:10.1155/2015/302653
Lin J, Huang L, Yu J, Xiang S, Wang J, Zhang J et al (2016) Fucoxanthin, a marine carotenoid, reverses scopolamine-induced cognitive impairments in mice and inhibits acetylcholinesterase in vitro. Mar Drugs 14(4). doi:10.3390/md14040067
Liu Z, Li T, Li P, Wei N, Zhao Z, Liang H et al (2015) The ambiguous relationship of oxidative stress, Tau hyperphosphorylation, and autophagy dysfunction in Alzheimer’s disease. Oxidative Med Cell Longev 2015:352723. doi:10.1155/2015/352723
Lowry OH, Rosenbrough NJ, Farr A, Randall RJ (1951) Protein measurement with Folinphenol reagent. J Biol Chem 193:265–275
Mancuso C, Bates TE, Butterfield DA, Calafato S, Cornelius C, De Lorenzo A et al (2007) Natural antioxidants in Alzheimer’s disease. Expert Opin Investig Drugs 16(12):1921–1931. doi:10.1517/13543784.16.12.1921
Mantamadiotis T, Lemberger T, Bleckmann SC, Kern H, Kretz O, Martin Villalba A et al (2002) Disruption of CREB function in brain leads to neurodegeneration. Nat Genet 31(1):47–54. doi:10.1038/ng882
Melis GB, Paoletti AM, Cagnacci A, Bufalino L, Spinetti A, Gambacciani M, Fioretti P (1992) Lack of any estrogenic effect of ipriflavone in postmenopausal women. J Endocrinol Investig 15(10):755–761
Melo A, Monteiro L, Lima RM, Oliveira DM, Cerqueira MD, El-Bacha RS (2011) Oxidative stress in neurodegenerative diseases: mechanisms and therapeutic perspectives. Oxidative Med Cell Longev 2011:467180. doi:10.1155/2011/467180
Mendiola-Precoma J, Berumen LC, Padilla K, Garcia-Alcocer G (2016) Therapies for prevention and treatment of Alzheimer’s disease. Biomed Res Int 2016:2589276. doi:10.1155/2016/2589276
Mietelska-Porowska A, Wasik U, Goras M, Filipek A, Niewiadomska G (2014) Tau protein modifications and interactions: their role in function and dysfunction. Int J Mol Sci 15(3):4671–4713. doi:10.3390/ijms15034671
Mitchell JH, Gardner PT, McPhail DB, Morrice PC, Collins AR, Duthie GG (1998) Antioxidant efficacy of phytoestrogens in chemical and biological model systems. Arch Biochem Biophys 360(1):142–148. doi:10.1006/abbi.1998.0951
Montgomery H, Dymock J (1961) The determination of nitrite in water. Analyst 86:414–416
Morrison JH, Brinton RD, Schmidt PJ, Gore AC (2006) Estrogen, menopause, and the aging brain: how basic neuroscience can inform hormone therapy in women. J Neurosci 26(41):10332–10348. doi:10.1523/JNEUROSCI.3369-06.2006
Nalivaeva NN, Fisk LR, Belyaev ND, Turner AJ (2008) Amyloid-degrading enzymes as therapeutic targets in Alzheimer’s disease. Curr Alzheimer Res 5(2):212–224
Nasir I, Linse S, Cabaleiro-Lago C (2015) Fluorescent filter-trap assay for amyloid fibril formation kinetics in complex solutions. ACS Chem Neurosci 6(8):1436–1444. doi:10.1021/acschemneuro.5b00104
Pachauri SD, Tota S, Khandelwal K, Verma PR, Nath C, Hanif K et al (2012) Protective effect of fruits of Morinda citrifolia L. on scopolamine induced memory impairment in mice: a behavioral, biochemical and cerebral blood flow study. J Ethnopharmacol 139(1):34–41. doi:10.1016/j.jep.2011.09.057
Paglia E, Valentine N (1967) Studies on the quantitative and qualitative characterization of erythrocyte glutathione peroxidase. J Lab Med 70:158–169
Park HR, Lee H, Park H, Cho WK, Ma JY (2016) Fermented Sipjeondaebo-tang alleviates memory deficits and loss of hippocampal neurogenesis in scopolamine-induced amnesia in mice. Sci Rep 6:22405. doi:10.1038/srep22405
Perez E, Liu R, Yang SH, Cai ZY, Covey DF, Simpkins JW (2005) Neuroprotective effects of an estratriene analog are estrogen receptor independent in vitro and in vivo. Brain Res 1038(2):216–222. doi:10.1016/j.brainres.2005.01.026
Persson T, Popescu BO, Cedazo-Minguez A (2014) Oxidative stress in Alzheimer’s disease: why did antioxidant therapy fail? Oxidative Med Cell Longev 2014:427318. doi:10.1155/2014/427318
Pike CJ (2017) Sex and the development of Alzheimer’s disease. J Neurosci Res 95(1–2):671–680. doi:10.1002/jnr.23827
Pike CJ, Carroll JC, Rosario ER, Barron AM (2009) Protective actions of sex steroid hormones in Alzheimer’s disease. Front Neuroendocrinol 30(2):239–258. doi:10.1016/j.yfrne.2009.04.015
Prasad MR, Lovell MA, Yatin M, Dhillon H, Markesbery WR (1998) Regional membrane phospholipid alterations in Alzheimer’s disease. Neurochem Res 23(1):81–88
Prior M, Dargusch R, Ehren JL, Chiruta C, Schubert D (2013) The neurotrophic compound J147 reverses cognitive impairment in aged Alzheimer’s disease mice. Alzheimers Res Ther 5(3):25. doi:10.1186/alzrt179
Qin W, Ho L, Wang J, Peskind E, Pasinetti GM (2009) S100A7, a novel Alzheimer’s disease biomarker with non-amyloidogenic alpha-secretase activity acts via selective promotion of ADAM-10. PLoS One 4(1):e4183. doi:10.1371/journal.pone.0004183
Reitz C, Mayeux R (2014) Alzheimer disease: epidemiology, diagnostic criteria, risk factors and biomarkers. Biochem Pharmacol 88(4):640–651. doi:10.1016/j.bcp.2013.12.024
Sadigh-Eteghad S, Sabermarouf B, Majdi A, Talebi M, Farhoudi M, Mahmoudi J (2015) Amyloid-beta: a crucial factor in Alzheimer’s disease. Med Princ Pract 24(1):1–10. doi:10.1159/000369101
Saxena G, Singh SP, Agrawal R, Nath C (2008) Effect of donepezil and tacrine on oxidative stress in intracerebral streptozotocin-induced model of dementia in mice. Eur J Pharmacol 581(3):283–289. doi:10.1016/j.ejphar.2007.12.009
Simpkins JW, Perez E, Wang X, Yang S, Wen Y, Singh M (2009) The potential for estrogens in preventing Alzheimer’s disease and vascular dementia. Ther Adv Neurol Disord 2(1):31–49. doi:10.1177/1756285608100427
Smith DG, Cappai R, Barnham KJ (2007) The redox chemistry of the Alzheimer’s disease amyloid beta peptide. Biochim Biophys Acta 1768(8):1976–1990. doi:10.1016/j.bbamem.2007.02.002
Song WJ, Son MY, Lee HW, Seo H, Kim JH, Chung SH (2015) Enhancement of BACE1 activity by p25/Cdk5-mediated phosphorylation in Alzheimer’s disease. PLoS One 10(8):e0136950. doi:10.1371/journal.pone.0136950
Tamagno E, Guglielmotto M, Giliberto L, Vitali A, Borghi R, Autelli R et al (2009) JNK and ERK1/2 pathways have a dual opposite effect on the expression of BACE1. Neurobiol Aging 30(10):1563–1573. doi:10.1016/j.neurobiolaging.2007.12.015
Tamagno E, Guglielmotto M, Monteleone D, Tabaton M (2012) Amyloid-beta production: major link between oxidative stress and BACE1. Neurotox Res 22(3):208–219. doi:10.1007/s12640-011-9283-6
Tappel AL, Zalkin H (1959) Inhibition of lipid peroxidation in mitochondria by vitamin E. Arch Biochem Biophys 80:333–333
Tarozzi A, Bartolini M, Piazzi L, Valgimigli L, Amorati R, Bolondi C et al (2014) From the dual function lead AP2238 to AP2469, a multi-target-directed ligand for the treatment of Alzheimer’s disease. Pharmacol Res Perspect 2(2):e00023. doi:10.1002/prp2.23
Turner AJ, Fisk L, Nalivaeva NN (2004) Targeting amyloid-degrading enzymes as therapeutic strategies in neurodegeneration. Ann N Y Acad Sci 1035:1–20. doi:10.1196/annals.1332.001
Weitz JC (1995) Detection of fecal Cryptosporidium parvum antigens using an ELISA technique. Rev Med Chil 123(3):330–333
Weitzner DS, Engler-Chiurazzi EB, Kotilinek LA, Ashe KH, Reed MN (2015) Morris water maze test: optimization for mouse strain and testing environment. J Vis Exp 100:e52706. doi:10.3791/52706
Williams TL, Serpell LC (2011) Membrane and surface interactions of Alzheimer’s Abeta peptide—insights into the mechanism of cytotoxicity. FEBS J 278(20):3905–3917. doi:10.1111/j.1742-4658.2011.08228.x
Wise PM, Suzuki S, Brown CM (2009) Estradiol: a hormone with diverse and contradictory neuroprotective actions. Dialogues Clin Neurosci 11(3):297–303
Wolozin B (2004) Cholesterol and the biology of Alzheimer’s disease. Neuron 41(1):7–10
Xiao Z, Huang C, Wu J, Sun L, Hao W, Leung LK, Huang J (2013) The neuroprotective effects of ipriflavone against H(2)O(2) and amyloid beta induced toxicity in human neuroblastoma SH-SY5Y cells. Eur J Pharmacol 721(1–3):286–293. doi:10.1016/j.ejphar.2013.09.023
Xiong H, Callaghan D, Jones A, Walker DG, Lue LF, Beach TG et al (2008) Cholesterol retention in Alzheimer’s brain is responsible for high beta- and gamma-secretase activities and Abeta production. Neurobiol Dis 29(3):422–437. doi:10.1016/j.nbd.2007.10.005
Xu J, Rong S, Xie B, Sun Z, Deng Q, Wu H et al (2010) Memory impairment in cognitively impaired aged rats associated with decreased hippocampal CREB phosphorylation: reversal by procyanidins extracted from the lotus seedpod. J Gerontol A Biol Sci Med Sci 65(9):933–940. doi:10.1093/gerona/glq094
Xu XW, Shi C, He ZQ, Ma CM, Chen WH, Shen YP et al (2008) Effects of phytoestrogen on mitochondrial structure and function of hippocampal CA1 region of ovariectomized rats. Cell Mol Neurobiol 28(6):875–886. doi:10.1007/s10571-008-9265-2
Yi KD, Perez E, Yang S, Liu R, Covey DF, Simpkins JW (2011) The assessment of non-feminizing estrogens for use in neuroprotection. Brain Res 1379:61–70. doi:10.1016/j.brainres.2010.11.058
Zhu F, Wu F, Ma Y, Liu G, Li Z, Sun Y, Pei Z (2011) Decrease in the production of beta-amyloid by berberine inhibition of the expression of beta-secretase in HEK293 cells. BMC Neurosci 12:125
Zimmermann M, Borroni B, Cattabeni F, Padovani A, Di Luca M (2005) Cholinesterase inhibitors influence APP metabolism in Alzheimer disease patients. Neurobiol Dis 19(1–2):237–242. doi:10.1016/j.nbd.2005.01.002
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
Experiments were performed following the ethical standards according to the Guide for the Care and Use of Laboratory Animals of the National Institutes of Health (Institute of Laboratory Animal Resources 1996) in Faculty of Medicine, Alexandria University, Egypt.
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
This research is supported by a core grant from Science and Technology Development Fund (STDF) in Egypt with grant number 4479.
Rights and permissions
About this article
Cite this article
Hafez, H.S., Ghareeb, D.A., Saleh, S.R. et al. Neuroprotective effect of ipriflavone against scopolamine-induced memory impairment in rats. Psychopharmacology 234, 3037–3053 (2017). https://doi.org/10.1007/s00213-017-4690-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-017-4690-x