Abstract
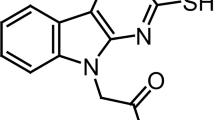
Hyperglycemia is considered a key risk factor for development of diabetic complications including neuropathy. There is strong scientific evidence showing a primary role of aldose reductase, the first enzyme of the polyol pathway, in the cascade of metabolic imbalances responsible for the detrimental effects of hyperglycemia. Aldose reductase is thus considered a significant drug target. We investigated the effects of cemtirestat, a novel aldose reductase inhibitor, in the streptozotocin-induced rat model of uncontrolled type 1 diabetes in a 4-month experiment. Markedly increased sorbitol levels were recorded in the erythrocytes and the sciatic nerve of diabetic animals. Osmotic fragility of red blood cells was increased in diabetic animals. Indices of thermal hypoalgesia were significantly increased in diabetic rats. Tactile allodynia, recorded in diabetic animals in the early stages, turned to mechanical hypoalgesia by the end of the experiment. Treatment of diabetic animals with cemtirestat (i) reduced plasma triglycerides and TBAR levels; (ii) did not affect the values of HbA1c and body weights; (iii) reversed erythrocyte sorbitol accumulation to near control values, while sorbitol in the sciatic nerve was not affected; (iv) ameliorated indices of the erythrocyte osmotic fragility; and (v) attenuated the symptoms of peripheral neuropathy more significantly in the middle of the experiment than at the end of the treatment. Taking into account the lipid metabolism as an interesting molecular target for prevention or treatment of diabetic peripheral neuropathy, the triglyceride-lowering effect of cemtirestat should be considered in future studies. The most feasible mechanisms of triglyceride-lowering action of cemtirestat were suggested.




Similar content being viewed by others
Abbreviations
- HbA1c:
-
Glycated hemoglobin
- LPL:
-
Lipoprotein lipase
- MCF:
-
Median corpuscular fragility
- RBC:
-
Red blood cells
- STZ:
-
Streptozotocin
- TBA:
-
Thiobarbituric acid
- TBAR:
-
Thiobarbituric acid reactive substances
- PPARs:
-
Peroxisome proliferator-activated receptors
- ZDF rat:
-
Zucker diabetic fatty rat
References
Adeli K, Taghibiglou C, Van Iderstine SC, Lewis GF (2001) Mechanisms of hepatic very low-density lipoprotein overproduction in insulin resistance. Trends Cardiovasc Med 11(5):170–176
Alexiou P, Pegklidou K, Chatzopoulou M, Nicolaou I, Demopoulos VJ (2009) Aldose reductase enzyme and its implication to major health problems of the 21(st) century. Curr Med Chem 16:734–752
Ali G, Subhan F, Abbas M, Zeb J, Shahid M, Sewell RD (2015) A streptozotocin-induced diabetic neuropathic pain model for static or dynamic mechanical allodynia and vulvodynia: validation using topical and systemic gabapentin. Naunyn Schmiedeberg’s Arch Pharmacol 388(11):1129–1140. https://doi.org/10.1007/s00210-015-1145-y
Balendiran GK, Rajkumar B (2005) Fibrates inhibit aldose reductase activity in the forward and reverse reactions. Biochem Pharmacol 70(11):1653. https://doi.org/10.1016/j.bcp.2005.06.029
Behling-Kelly E, Collins-Cronkright R (2014) Increases in beta-lipoproteins in hyperlipidemic and dyslipidemic dogs are associated with increased erythrocyte osmotic fragility. Vet Clin Pathol 43(3):405–415. https://doi.org/10.1111/vcp12155
Biessels GJ, Bril V, Calcutt NA et al (2014) Phenotyping animal models of diabetic neuropathy: a consensus statement of the diabetic neuropathy study group of the EASD (Neurodiab). J Peripher Nerv Syst 19(2):77–87. https://doi.org/10.1111/jns5.12072
Bobek P, Chorvathova V, Ozdin L (1981) Kinetics of plasma triglycerides in rats with streptozotocin diabetes. Physiol Bohemoslov 30:35–40
Buege JA, Aust SD (1978) Microsomal lipid. Methods Enzymol 52:302–310. https://doi.org/10.1016/S0076-6879(78)52032-6
Calabek B, Callaghan B, Feldman EL (2014) Therapy for diabetic neuropathy: an overview. Chapter 22. In: Zochodne DW, Malik RA (eds) Handbook of clinical neurology. Elsevier, 126:317–333. https://doi.org/10.1016/B978-0-444-53480-4.00022-9
Calcutt NA, Freshwater JD, Mizisin AP (2004) Prevention of sensory disorders in diabetic Sprague-Dawley rats by aldose reductase inhibition or treatment with ciliary neurotrophic factor. Diabetologia 47(4):718–724. https://doi.org/10.1007/s00125-004-1354-2
Chalk C, Benstead TJ, Moore F (2007) Aldose reductase inhibitors for the treatment of diabetic polyneuropathy. Cochrane Database Syst Rev 4:CD004572. https://doi.org/10.1002/14651858CD004572pub2
Chaplan SR, Bach FW, Pogrel JW, Chung JM, Yaksh TL (1994) Quantitative assessment of tactile allodynia in the rat paw. J Neurosci Methods 53(1):55–63
Dewanjee S, Das S, Das AK, Bhattacharjee N, Dihingia A, Dua TK, Kalita J, Manna P (2018) Molecular mechanism of diabetic neuropathy and its pharmacotherapeutic targets. Eur J Pharmacol 15(833):472–523. https://doi.org/10.1016/jejphar201806034
Drel VR, Pacher P, Vareniuk I, Pavlov I, Ilnytska O, Lyzogubov VV, Tibrewala J, Groves JT, Obrosova IG (2007) A peroxynitrite decomposition catalyst counteracts sensory neuropathy in streptozotocin-diabetic mice. Eur J Pharmacol 13 569(1–2):48–58
Eleazu CO, Eleazu KC, Chukwuma S, Essien UN (2013) Review of the mechanism of cell death resulting from streptozotocin challenge in experimental animals, its practical use and potential risk to humans. J Diabetes Metab Disord 12(1):60–67
Espejo EF, Mir D (1993) Structure of the rat’s behaviour in the hot plate test. Behav Brain Res. 56(2):171–176
Feldman EL, Nave KA, Jensen TS, Bennett DLH (2017) New horizons in diabetic neuropathy: mechanisms, bioenergetics, and pain. Neuron 93(6):1296–1313. https://doi.org/10.1016/jneuron201702005
Gajdosík A, Gajdosíková A, Stefek M, Navarová J, Hozová R (1999) Streptozotocin-induced experimental diabetes in male Wistar rats. Gen Physiol Biophys 18:54–62
Grewal AS, Bhardwaj S, Pandita D, Lather V, Sekhon BS (2016) Updates on aldose reductase inhibitors for management of diabetic complications and non-diabetic diseases. Mini Rev Med Chem 16(2):120–162
Hinder LM, Vincent AM, Hayes JM, McLean LL, Feldman EL (2013) Apolipoprotein E knockout as the basis for mouse models of dyslipidemia-induced neuropathy. Exp Neurol 239:102–110. https://doi.org/10.1016/jexpneurol201210002
Hirano T (2018) Pathophysiology of diabetic dyslipidemia. J Atheroscler Thromb 25(9):771–782. https://doi.org/10.5551/jatRV17023
Hirano T, Mamo JC, Takeuchi H, Nagano S, Takahashi T (1991) Correlation of insulin deficiency and hypertriglyceridemia in diabetic rats. Diabetes Res Clin Pract 12(3):173–180
Ilnytska O, Lyzogubov VV, Stevens MJ, Drel VR, Mashtalir N, Pacher P, Yorek MA, Obrosova IG (2006) Poly (ADP-ribose) polymerase inhibition alleviates experimental diabetic sensory neuropathy. Diabetes 55(6):1686–1694
Klemin S, Calvo RY, Bond S, Dingess H, Rajkumar B, Perez R, Chow L, Balendiran GK (2006) WY 14,643 inhibits human aldose reductase activity. J Enzyme Inhib Med Chem 21(5):569–573. https://doi.org/10.1080/14756360600720887
Kyselova Z, Gajdosik A, Gajdosikova A, Ulicna O, Mihalova D, Karasu C, Stefek M (2005) Effect of the pyridoindole antioxidant stobadine on development of experimental diabetic cataract and on lens protein oxidation in rats: comparison with vitamin E and BHT. MolVis 11:56–65
Lenzen S (2008) The mechanisms of alloxan- and streptozotocin-induced diabetes. Diabetologia 51(2):216–226
Lupachyk S, Shevalye H, Maksimchyk Y, Drel VR, Obrosova IG (2011) PARP inhibition alleviates diabetes-induced systemic oxidative stress and neural tissue 4-hydroxynonenal adduct accumulation: correlation with peripheral nerve function. Free Radic Biol Med 50(10):1400–1409. https://doi.org/10.1016/j.freeradbiomed.2011.01.037
Maccari R, Ottanà R (2015) Targeting aldose reductase for the treatment of diabetes complications and inflammatory diseases: new insights and future directions. J Med Chem 58:2047–2067. https://doi.org/10.1021/jm500907a
Majekova M, Ballekova J, Prnova M, Stefek M (2017) Structure optimization of tetrahydropyridoindole-based aldose reductase inhibitors improved their efficacy and selectivity. Bioorg & Med Chem. 25:6353–6360. https://doi.org/10.1016/j.bmc.2017.10.005
Murase T, Tanaka K, Iwamoto Y, Akanuma Y, Kosaka K (1981) Reciprocal changes, caused by insulin and glucagon, of adipose tissue lipoprotein lipase in rats in vitro. Horm Metab Res 13:212–213
Oates PJ (2008) Aldose reductase, still a compelling target for diabetic neuropathy. Curr Drug Targets 9(1):14–36
Obrosova IG (2002) How does glucose generate oxidative stress in peripheral nerve? Int Rev Neurobiol 50:3–35. https://doi.org/10.1016/S0074-7742(02)50071-4
Obrosova IG (2009) Diabetic painful and insensate neuropathy: pathogenesis and potential treatments. Neurotherapeutics 6(4):638–647. https://doi.org/10.1016/jnurt200907004
Obrosova IG, Xu W, Lyzogubov VV, Ilnytska O, Mashtalir N, Vareniuk I, Pavlov IA, Zhang J, Slusher B, Drel VR (2008) PARP inhibition or gene deficiency counteracts intraepidermal nerve fiber loss and neuropathic pain in advanced diabetic neuropathy. Free Radic Biol Med 44(6):972–981
Pertovaara A, Wei H, Kalmari J, Ruotsalainen M (2001) Pain behavior and response properties of spinal dorsal horn neurons following experimental diabetic neuropathy in the rat: modulation by nitecapone, a COMT inhibitor with antioxidant properties. Exp Neurol 167(2):425–434
Pritchard KA Jr, Patel ST, Karpen CW, Newman HA, Panganamala RV (1986) Triglyceride-lowering effect of dietary vitamin E in streptozocin-induced diabetic rats. Increased lipoprotein lipase activity in livers of diabetic rats fed high dietary vitamin E. Diabetes 35(3):278–281
Prnova MS, Ballekova J, Majekova M, Stefek M (2015) Antioxidant action of 3-mercapto-5H-1,2,4-triazino[5,6-b]indole-5-acetic acid, an efficient aldose reductase inhibitor, in a 1,1′-diphenyl-2-picrylhydrazyl assay and in the cellular system of isolated erythrocytes exposed to tert-butyl hydroperoxide. Redox Rep 20(6):282–288. https://doi.org/10.1179/1351000215Y0000000019
Qiu L, Wu X, Chau JF, Szeto IY, Tam WY, Guo Z, Chung SK, Oates PJ, Chung SS, Yang JY (2008) Aldose reductase regulates hepatic peroxisome proliferator-activated receptor alpha phosphorylation and activity to impact lipid homeostasis. J Biol Chem 283(25):17175–17183. https://doi.org/10.1074/jbcM801791200
Qiu L, Lin J, Xu F, Gao Y, Zhang C, Liu Y, Luo Y, Yang JY (2012) Inhibition of aldose reductase activates hepatic peroxisome proliferator-activated receptor-α and ameliorates hepatosteatosis in diabetic db/db mice. Exp Diabetes Res 2012:789730. https://doi.org/10.1155/2012/789730
Ramirez MA, Borja NL (2008) Epalrestat: an aldose reductase inhibitor for the treatment of diabetic. Pharmacotherapy 28(5):646–655. https://doi.org/10.1592/phco285646
Reaven EP, Reaven GM (1974) Mechanisms for development of diabetic hypertriglyceridemia in streptozotocin-treated rats effect of diet and duration of insulin deficiency. J Clin Invest 54(5):1167–1178. https://doi.org/10.1172/JCI107860
Schemmel KE, Padiyara RS, D’Souza JJ (2010) Aldose reductase inhibitors in the treatment of diabetic peripheral neuropathy: review. J Diabetes Complicat 24(5):354–360. https://doi.org/10.1016/jjdiacomp200907005
Shaikh AS, Somani RS (2010) Animal models and biomarkers of neuropathy in diabetic rodents. Indian J Pharmacol 42:129–134. https://doi.org/10.4103/0253-7613.66833
Shakeel M (2015) Recent advances in understanding the role of oxidative stress in diabetic neuropathy. Diabetes Metab Syndr 9(4):373–378. https://doi.org/10.1016/jdsx201404029
Singh R, Kishore L, Kaur N (2014) Diabetic peripheral neuropathy: current perspective and future. Directions Pharmacol Res 80:21–35. https://doi.org/10.1016/jphrs201312005
Soltesova Prnova M, Ballekova J, Gajdosikova A, Gajdosik A, Stefek M (2015a) A novel carboxymethylated mercaptotriazinoindole inhibitor of aldose reductase interferes with the polyol pathway in streptozotocin-induced diabetic rats. Physiol Res 64(4):587–591
Soltesova Prnova M, Majekova M, Milackova I, Díez-Dacal B, Pérez-Sala D, Ceyhan MS, Banerjee S, Stefek M (2015b) [5-(Benzyloxy)-1H-indol-1-yl] acetic acid, an aldose reductase inhibitor and PPARγ ligand. Acta Biochim Pol 62(3):523–528. https://doi.org/10.18388/abp2014953
Soltesova Prnova M, Svik K, Bezek S, Kovacikova L, Karasu C, Stefek M (2019) 3-Mercapto-5H-1,2,4-triazino[5,6-b]indole-5-acetic acid (cemtirestat) alleviates symptoms of peripheral diabetic neuropathy in Zucker diabetic fatty (ZDF) rats: a role of aldose reductase. Neurochem Res 44(5):1056–1064. https://doi.org/10.1007/s11064-019-02736-1
Stefek M, Soltesova Prnova M, Majekova M, Rechlin C, Heine A, Klebe G (2015) Identification of novel aldose reductase inhibitors based on carboxymethylated mercaptotriazinoindole scaffold. J Med Chem 58(6):2649–2657. https://doi.org/10.1021/jm5015814
Stefek M, Soltesova Prnova M, Ballekova J, Majekova M (2016) Cemtirestat, a novel aldose reductase inhibitor and antioxidant, in multitarget pharmacology of diabetic complications. Int J Adv Sci Eng Technol 4(3):41–44
Stefek M, Milackova I, Díez-Dacal B, Pérez-Sala D, Soltesova Prnova M (2017) Use of 5-carboxymethyl-3-mercapto-1,2,4-triazino-[5,6-b] indoles and their pharmaceutical composition. Slovak Patent No 288508
Tesfaye S, Selvarajah D (2009) The Eurodiab study: what has this taught us about diabetic peripheral neuropathy? Curr Diab Rep 9(6):432–434
Tomlinson DR, Gardiner NJ (2008) Glucose neurotoxicity. Nat Rev Neurosci 9(1):36–45. https://doi.org/10.1038/nrn2294
Travis SF, Morrison AD, Clements RS Jr, Winegrad AI, Oski FA (1971) Metabolic alterations in the human erythrocyte produced by increases in glucose concentration. The role of the polyol pathway. J Clin Invest 50(10):2104–2112. https://doi.org/10.1172/JCI106704
Tsutsumi K, Inoue Y, Shima A, Murase T (1995) Correction of hypertriglyceridemia with low high-density lipoprotein cholesterol by the novel compound NO-1886, a lipoprotein lipase-promoting agent, in STZ-induced diabetic rats. Diabetes 44(4):414–417
Uydu HA, Yıldırmıs S, Orem C et al (2012) The effects of atorvastatin therapy on rheological characteristics of erythrocyte membrane, serum lipid profile and oxidative status in patients with dyslipidemia. J Membr Biol 245:697–705. https://doi.org/10.1007/s00232-012-9441-7
Van Dam PS, Van Asbeck BS, Bravenboer B, Van Oirschot JF, Marx JJ, Gispen WH (1999) Nerve conduction and antioxidant levels in experimentally diabetic rats: effects of streptozotocin dose and diabetes duration. Metabolism 48(4):442–447
Vergès B (2011) Lipid disorders in type 1 diabetes, type 1 diabetes - complications, pathogenesis, and alternative treatments, Chih-Pin Liu, IntechOpen. https://doi.org/10.5772/20869. Available from: https://www.intechopen.com/books/type-1-diabetes-complications-pathogenesis-and-alternative-treatments/lipid-disorders-in-type-1-diabetes
Vincent AM, Russell JW, Low P, Feldman EL (2004) Oxidative stress in the pathogenesis of diabetic neuropathy. Endocr Rev 25(4):612. https://doi.org/10.1210/er2003-0019
Vincent AM, Callaghan BC, Smith AL, Feldman EL (2011) Diabetic neuropathy: cellular mechanisms as therapeutic targets. Nat Neurol 7(10):573–583. https://doi.org/10.1038/nrneurol2011137
Wiggin TD, Sullivan KA, Pop-Busui R, Amato A, Sima AA, Feldman EL (2009) Elevated triglycerides correlate with progression of diabetic neuropathy. Diabetes 58(7):1634–1640. https://doi.org/10.2337/db08-1771
Winterbourn CC (1990) Oxidative reactions of hemoglobin. Meth Enzymol 186:265–272. https://doi.org/10.1016/0076-6879(90)86118-F
Wu KK, Huan Y (2008) Streptozotocin-induced diabetic models in mice and rats. Curr Protoc Pharmacol 40:5.47.1–5.47.14. https://doi.org/10.1002/0471141755.ph0547s40
Yoshino G, Matsushita M, Maeda E, Nagata K, Morita M, Matsuba K, Tani T, Horinuki R, Kimura Y, Kazumi T (1991) Effect of probucol on triglyceride turnover in streptozotocin-diabetic rats. Atherosclerosis 88(1):69–75. https://doi.org/10.1016/0021-9150(91)90258-5
Zhan JY, Ma K, Zheng QC, Yang GH, Zhang HX (2019) Exploring the interactional details between aldose reductase (AKR1B1) and 3-Mercapto-5H-1,2,4-triazino[5,6-b]indole-5-acetic acid through molecular dynamics simulations. J Biomol Struct Dyn 37(7):1724. https://doi.org/10.1080/07391102.2018.1465851
Zhou Q, Bao Y, Zhang X, Zeng L, Wang L, Wang J, Jiang W (2014) Optimal interval for hot water immersion tail-flick test in rats. Acta Neuropsychiatr 26(4):218–222. https://doi.org/10.1017/neu.2013.57
Acknowledgments
This work was supported by VEGA 2/0005/2018, Slovak Research and Development Agency, under the contract NO. APVV-15-0455, SAS-Tubitak JRP 2015/7 and TUBITAK Project No: 215S19.
Author contribution statement
MSP, LK, CK, and MS designed and performed research including behavioral and biochemical assays; participated in the interpretation of the results, writing and review of the manuscript. KS, SB and ZE performed behavioral and biochemical assays. All authors read and approved the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the Ethics Committee of the Institute of Experimental Pharmacology and Toxicology, CEM, SAS, and the State Veterinary and Food Administration of the Slovak Republic, and it was performed in accordance with the Principles of Laboratory Animal Care (NIH publication 83-25, revised 1985) and the Slovak law regulating animal experiments (Decree 289, Part 139, July 9, 2003).
Conflict of interest
The authors declare that they have no conflict of interest
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Prnova, M.S., Kovacikova, L., Svik, K. et al. Triglyceride-lowering effect of the aldose reductase inhibitor cemtirestat—another factor that may contribute to attenuation of symptoms of peripheral neuropathy in STZ-diabetic rats. Naunyn-Schmiedeberg's Arch Pharmacol 393, 651–661 (2020). https://doi.org/10.1007/s00210-019-01769-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-019-01769-1