Abstract
Summary
Intake of plant-based protein and recommended protein intake are associated with a lower risk of osteosarcopenic adiposity (co-occurrence of osteopenia/osteoporosis, sarcopenia, and adiposity) in elderly Korean men.
Introduction
Osteosarcopenic adiposity (OSA) syndrome is defined as the concurrent presence of osteopenia/osteoporosis, sarcopenia, and adiposity and leads to negative functional and metabolic outcomes in late adulthood. This study aimed to investigate the association between OSA and protein intake in adults aged 50 or older.
Methods
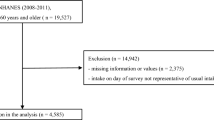
A population-based, cross-sectional survey was conducted using the Korea National Health and Nutrition Examination Survey 2008–2009 data and included 645 men and 706 women aged 50 or older. Subjects were classified into normal and OSA groups. Protein intake was analyzed using the 24-h recall method.
Results
There was no significant difference in the intake of total protein and animal-based protein between normal and OSA groups. However, in males, the intake of plant-based protein (p = 0.0031) was significantly lower in the OSA group than that in the normal group. Further, the protein intake in the OSA group was 0.96 g/kg/day, which was significantly lower than that in the normal group (1.06 g/kg/day; p = 0.0203). After adjusting for confounding factors, men over 65 years old who consumed less than the recommended nutrient intake (RNI) of 0.91 g/kg/day had 5.82 times higher risk of OSA compared with subjects consuming protein equal to or greater than the RNI amount (95% CI 1.81–18.66).
Conclusion
In conclusion, a protein intake of RNI or more is associated with a lower risk of OSA in Korean elderly men.
Similar content being viewed by others
Data availability
Data used in this study are from the Korean CDC (https://knhanes.cdc.go.kr/knhanes/index.do).
References
Kinsella K, Phillips DR (2005) Global aging: the challenge of success. Popul Bull 60:5–42
Statistics Korea (2018) 2018 elderly statistics. Statistics Korea Website. http://kostat.go.kr/portal/korea/kor_nw/1/1/index.board?bmode=read&aSeq=370779. Accessed 9 Jan 2020
NCD Risk Factor Collaboration (NCD-RisC) (2016) Trends in adult body-mass index in 200 countries from 1975 to 2014: a pooled analysis of 1698 population-based measurement studies with 19.2 million participants. Lancet 387:1377–1396. https://doi.org/10.1016/S0140-6736(16)30054-X
Boles A, Kandimalla R, Reddy PH (2017) Dynamics of diabetes and obesity: epidemiological perspective. Biochim Biophys Acta Mol basis Dis 1863:1026–1036. https://doi.org/10.1016/j.bbadis.2017.01.016
Zamboni M, Rubele S, Rossi AP (2019) Sarcopenia and obesity. Curr Opin Clin Nutr Metab Care 22:13–19. https://doi.org/10.1097/MCO.0000000000000519
Ilich JZ, Kelly OJ, Inglis JE (2016) Osteosarcopenic obesity syndrome: what is it and how can it be identified and diagnosed? Curr Gerontol Geriatr Res 2016:7325973–7325977. https://doi.org/10.1155/2016/7325973
Ilich JZ, Gilman JC, Cvijetic S, Boschiero D (2020) Chronic stress contributes to osteosarcopenic adiposity via inflammation and immune modulation: the case for more precise nutritional investigation. Nutrients 12:989. https://doi.org/10.3390/nu12040989
Perna S, Spadaccini D, Nichetti M, Avanzato I, Faliva MA, Rondanelli M (2018) Osteosarcopenic visceral obesity and osteosarcopenic subcutaneous obesity, two new phenotypes of sarcopenia: prevalence, metabolic profile, and risk factors. J Aging Res 2018:6147426–6147428. https://doi.org/10.1155/2018/6147426
Kelly OJ, Gilman JC, Boschiero D, Ilich JZ (2019) Osteosarcopenic obesity: current knowledge, revised identification criteria and treatment principles. Nutrients 11:747. https://doi.org/10.3390/nu11040747
Wallace TC, Frankenfeld CL (2017) Dietary protein intake above the current RDA and bone health: a systematic review and meta-analysis. J Am Coll Nutr 36:481–496. https://doi.org/10.1080/07315724.2017.1322924
Genaro Pde S, Martini LA (2010) Effect of protein intake on bone and muscle mass in the elderly. Nutr Rev 68:616–623. https://doi.org/10.1111/j.1753-4887.2010.00321.x
Solerte SB, Gazzaruso C, Bonacasa R, Rondanelli M, Zamboni M, Basso C, Locatelli E, Schifino N, Giustina A, Fioravanti M (2008) Nutritional supplements with oral amino acid mixtures increases whole-body lean mass and insulin sensitivity in elderly subjects with sarcopenia. Am J Cardiol 101:69E–77E. https://doi.org/10.1016/j.amjcard.2008.03.004
Kweon S, Kim Y, Jang MJ, Kim Y, Kim K, Choi S, Chun C, Khang YH, Oh K (2014) Data resource profile: the Korea National Health and Nutrition Examination Survey (KNHANES). Int J Epidemiol 43:69–77. https://doi.org/10.1093/ije/dyt228
Willett W (2013) Nutritional epidemiology, 3rd (ed). Oxford University Press, New York
Kanis JA (1994) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis: synopsis of a WHO report. WHO Study Group. Osteoporos Int 4:368–381. https://doi.org/10.1007/bf01622200
Kim YS, Lee Y, Chung YS, Lee DJ, Joo NS, Hong D, Song GE, Kim HJ, Choi YJ, Kim KM (2012) Prevalence of sarcopenia and sarcopenic obesity in the Korean population based on the Fourth Korean National Health and Nutritional Examination Surveys. J Gerontol A Biol Sci Med Sci 67:1107–1113. https://doi.org/10.1093/gerona/gls071
American Council on Exercise. Percent body fat norms for men and women. https://www.acefitness.org/education-and-resources/lifestyle/tools-calculators/percent-body-fat-calculator/. Accessed 2 June 2020
National Rural Resources Development Institute (2006) Korean food composition table, 7th (ed). Rural Development Administration, Kyonggi
Ministry of Health and Welfare & The Korean Nutrition Society (2015) Dietary reference intakes for Koreans 2015. Korean Nutrition Society Website. http://www.kns.or.kr/FileRoom/FileRoom_view.asp?idx=79&BoardID=Kdr. Accessed 9 Jan 2020
Kelly OJ, Gilman JC, Kim Y, Ilich JZ (2017) Macronutrient intake and distribution in the etiology, prevention and treatment of osteosarcopenic obesity. Curr Aging Sci 10:83–105. https://doi.org/10.2174/1874609809666160509122558
Kelly OJ, Gilman JC, Kim Y, Ilich JZ (2016) Micronutrient intake in the etiology, prevention and treatment of osteosarcopenic obesity. Curr Aging Sci 9:260–278. https://doi.org/10.2174/1874609809666160509122001
Cosman F, de Beur SJ, LeBoff MS, Lewiecki EM, Tanner B, Randall S, Lindsay R (2014) Clinician’s guide to prevention and treatment of osteoporosis. Osteoporos Int 25:2359–2381. https://doi.org/10.1007/s00198-014-2794-2
Rom O, Kaisari S, Aizenbud D, Reznick AZ (2012) Lifestyle and sarcopenia-etiology, prevention, and treatment. Rambam Maimonides Med J 3:e0024. https://doi.org/10.5041/RMMJ.10091
Li Z, Heber D (2012) Sarcopenic obesity in the elderly and strategies for weight management. Nutr Rev 70:57–64. https://doi.org/10.1111/j.1753-4887.2011.00453.x
JafariNasabian P, Inglis JE, Kelly OJ, Ilich JZ (2017) Osteosarcopenic obesity in women: impact, prevalence, and management challenges. Int J Women's Health 9:33–42. https://doi.org/10.2147/IJWH.S106107
Kim J, Lee Y, Kye S, Chung YS, Kim JH, Chon D, Lee KE (2017) Diet quality and osteosarcopenic obesity in community-dwelling adults 50 years and older. Maturitas 104:73–79. https://doi.org/10.1016/j.maturitas.2017.08.007
Granic A, Mendonça N, Sayer AA, Hill TR, Davies K, Adamson A, Siervo M, Mathers JC, Jagger C (2018) Low protein intake, muscle strength and physical performance in the very old: the Newcastle 85+ study. Clin Nutr 37:2260–2270. https://doi.org/10.1016/j.clnu.2017.11.005
Issa RI, Griffin TM (2012) Pathobiology of obesity and osteoarthritis: integrating biomechanics and inflammation. Pathobiol Aging Age Relat Dis 2:17470. https://doi.org/10.3402/pba.v2i0.17470
Churchward-Venne TA, Murphy CH, Longland TM, Phillips SM (2013) Role of protein and amino acids in promoting lean mass accretion with resistance exercise and attenuating lean mass loss during energy deficit in humans. Amino Acids 45:231–240. https://doi.org/10.1007/s00726-013-1506-0
Oh C, Jeon BH, Reid Storm SN, Jho S, No JK (2017) The most effective factors to offset sarcopenia and obesity in the older Korean: physical activity, vitamin D, and protein intake. Nutrition 33:169–173. https://doi.org/10.1016/j.nut.2016.06.004
Kristensen MD, Bendsen NT, Christensen SM, Astrup A, Raben A (2016) Meals based on vegetable protein sources (bean and peas) are more satiating than meals based on animal protein sources (veal and pork)- a randomized cross-over meal test study. Food Nutr Res 60:32634. https://doi.org/10.3402/fnr.v60.32634
Bernstein AM, Sun Q, Hu FB, Stampfer MJ, Manson JE, Willett WC (2010) Major dietary protein sources and risk of coronary heart disease in women. Circulation 122:876–883. https://doi.org/10.1161/CIRCULATIONAHA.109.915165
Food and Agricultural Organization (FAO) (2013) Dietary protein quality evaluation in human nutrition: report of an FAO export consultation; FAO food and nutrition paper 92; Food and Agricultural Organization (FAO). Rome
Wang F, Zheng J, Yang B, Jiang J, Fu Y, Li D (2015) Effects of vegetarian diets on blood lipids: a systematic review and meta-analysis of randomized controlled trials. J Am Heart Assoc 4:e002408. https://doi.org/10.1161/JAHA.115.002408
Park KB, Park HA, Kang JH, Kim K, Cho YG, Jang J (2018) Animal and plant protein intake and body mass index and waist circumference in a Korean elderly population. Nutrients 10:E577. https://doi.org/10.3390/nu10050577
Jennings A, MacGregor A, Spector T, Cassidy A (2016) Amino acid intakes are associated with bone mineral density and prevalence of low bone mass in women: evidence from discordant monozygotic twins. J Bone Miner Res 31:326–335. https://doi.org/10.1002/jbmr.2703
Shams-White MM, Chung M, Fu Z, Insogna KL, Karlsen MC, LeBoff MS, Shapses SA, Sackey J, Shi J, Wallace TC, Weaver CM (2018) Animal versus plant protein and adult bone health: a systematic review and meta-analysis from the National Osteoporosis Foundation. PLoS One 13:e0192459. https://doi.org/10.1371/journal.pone.0192459
Darling AL, Manders RJF, Sahni S, Zhu K, Hewitt CE, Prince RL, Millward DJ, Lanham-New SA (2019) Dietary protein and bone health across the life-course: an updated systematic review and meta-analysis over 40 years. Osteoporos Int 30:741–761. https://doi.org/10.1007/s00198-019-04933-8
Ilich JZ, Inglis JE, Kelly OJ, McGee DL (2015) Osteosarcopenic obesity is associated with reduced handgrip strength, walking abilities, and balance in postmenopausal women. Osteoporos Int 26:2587–2595. https://doi.org/10.1007/s00198-015-3186-y
Santarpia L, Contaldo F, Pasanisi F (2017) Dietary protein content for an optimal diet: a clinical view. J Cachexia Sarcopenia Muscle 8:345–348. https://doi.org/10.1002/jcsm.12176
Park HA (2018) Adequacy of protein intake among Korean elderly: an analysis of the 2013-2014 Korea National Health and Nutrition Examination Survey Data. Korean J Fam Med 39:130–134. https://doi.org/10.4082/kjfm.2018.39.2.130
Chung JH, Hwang HJ, Shin HY, Han CH (2016) Association between sarcopenic obesity and bone mineral density in middle-aged and elderly Korean. Ann Nutr Metab 68:77–84. https://doi.org/10.1159/000442004
Jeng C, Zhao LJ, Wu K, Zhou Y, Chen T, Deng HW (2018) Race and socioeconomic effect on sarcopenia and sarcopenic obesity in the Louisiana Osteoporosis Study (LOS). JCSM Clin Rep 3:e00027
Yun S, Kim HJ, Oh K (2017) Trends in energy intake among Korean adults, 1998-2015: results from the Korea National Health and Nutrition Examination Survey. Nutr Res Pract 11:147–154. https://doi.org/10.4162/nrp.2017.11.2.147
Kim BK, Park DJ, Oh S (2019) Application of dairy food processing technology supplemented with enriched nutrients for the elderly: I. Nutritional conditions and care-foods for the elderly. J Milk Sci Biotechnol 37:69–80. https://doi.org/10.22424/jmsb.2019.37.1.69
Seo MH, Lee WY, Kim SS, Kang JH, Kang JH, Kim KK, Kim BY, Kim YH, Kim WJ, Kim EM, Kim HS, Shin YA, Shin HJ, Lee KR, Lee KY, Lee SY, Lee SK, Lee JH, Lee CB, Chung S, Cho YH, Choi KM, Han JS, Yoo SJ, Committee of Clinical Practice Guidelines, Korean Society for the Study of Obesity (KSSO) (2019) 2018 Korean Society for the Study of obesity guideline for the management of obesity in Korea. J Obes Metab Syndr 28:40–45. https://doi.org/10.7570/jomes.2019.28.1.40
Park S, Na W, Sohn C (2018) Relationship between osteosarcopenic obesity and dietary inflammatory index in postmenopausal Korean women: 2009 to 2011 Korea National Health and Nutrition Examination Surveys. J Clin Biochem Nutr 63:211–216. https://doi.org/10.3164/jcbn.18-10
Bae YJ (2020) Fruit intake and osteosarcopenic obesity in Korean postmenopausal women aged 50-64 years. Maturitas 134:41–46. https://doi.org/10.1016/j.maturitas.2020.02.003
Funding
This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Ministry of Science, ICT & Future Planning (Grant number: 2017R1C1B5017636).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethics approval
The KNHANES was reviewed and approved by the Ethics Committee of the Korea Centers for Disease Control and Prevention (KNHANES).
Consent to participate
All participants in the KNHANES survey provided informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Choi, MK., Bae, YJ. Protein intake and osteosarcopenic adiposity in Korean adults aged 50 years and older. Osteoporos Int 31, 2363–2372 (2020). https://doi.org/10.1007/s00198-020-05529-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-020-05529-3