Abstract
Summary
Our study focused on the associations of metabolites with BMD and osteoporosis, finding that several metabolites are associated with BMD, and metabolites combined with bone turnover markers tend to be more sensitive in distinguishing osteoporosis in both males and postmenopausal females, which might be meaningful for the early diagnosis of osteoporosis.
Introduction
Our study aimed to evaluate the association of metabolites with bone, trying to find new metabolic markers that are distinguishing for low bone mineral density (BMD).
Methods
Our study recruited 320 participants, including 138 males and 182 postmenopausal females from the Shanghai area. Bone turnover markers (BTMs), including osteocalcin, PINP and β-CTX, and other biochemical traits were tested. BMD values of the lumber spine (L1–4), femoral neck and total hip were determined using dual-energy X-ray absorptiometry and the serum metabolome profiles including 221 metabolites from five groups (acylcarnitines, amino acids, biogenic amines, glycerophospholipids, sphingolipids and hexose) were assessed by mass spectrometry.
Results
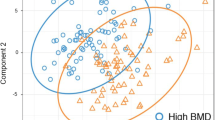
No visual separation in the metabolic profiles between different BMD groups was observed in principal component analysis (PCA) or partial least squares discriminant analysis (PLS-DA) models. We compared metabolites in three groups with different BMD levels in males and postmenopausal females separately and further filtering these metabolites via random forest-based feature selection, a commonly applied machine learning algorithm which could select the features with the greatest impact on osteoporosis, then metabolites with the highest importance (≥ 5%) (5 in males and 9 in postmenopausal females) were selected to construct better models for osteoporosis classification. After adding these selected metabolites to the model, the area under the curve (AUC) of receiver operating characteristic (ROC) curves increased significantly (BTMs: AUC 0.729, 95% CI 0.647–0.802, p < 0.0001, model 1: AUC = 0.828, 95% CI 0.754–0.888, p < 0.0001; model 1 versus model of BTMs: p = 0.0158) compared to the AUC of the BTM-only model in males. Similar results were also observed in postmenopausal females (BTMs: AUC = 0.638, 95% CI 0.562–0.708, p = 0.0025; model 2: AUC = 0.741, 95% CI 0.669–0.803, p < 0.0001; model 1 versus model of BTMs: p = 0.0182).
Conclusion
Metabolites combined with traditional BTMs tend to better markers for distinguishing osteoporosis in both males and postmenopausal females than BTMs alone.




Similar content being viewed by others
References
Svedbom A, Hernlund E, Ivergard M, Compston J, Cooper C, Stenmark J, McCloskey EV, Jonsson B, Kanis JA (2013) Osteoporosis in the European Union: a compendium of country-specific reports. Arch Osteoporos 8:137
Qu B, Ma Y, Yan M, Wu HH, Fan L, Liao DF, Pan XM, Hong Z (2014) The economic burden of fracture patients with osteoporosis in western China. Osteoporos Int 25:1853–1860
Rossini M, Adami S, Bertoldo F, Diacinti D, Gatti D, Giannini S, Giusti A, Malavolta N, Minisola S, Osella G, Pedrazzoni M, Sinigaglia L, Viapiana O, Isaia GC (2016) Guidelines for the diagnosis, prevention and management of osteoporosis. Reumatismo 68:1–39
Blake GM, Fogelman I (2007) The role of DXA bone density scans in the diagnosis and treatment of osteoporosis. Postgrad Med J 83:509–517
McCloskey EV, Johansson H, Oden A, Kanis JA (2009) From relative risk to absolute fracture risk calculation: the FRAX algorithm. Curr Osteoporos Rep 7:77–83
Leslie WD, Brennan SL, Lix LM, Johansson H, Oden A, McCloskey E, Kanis JA (2013) Direct comparison of eight national FRAX(R) tools for fracture prediction and treatment qualification in Canadian women. Arch Osteoporos 8:145
Biver E, Chopin F, Coiffier G, Brentano TF, Bouvard B, Garnero P, Cortet B (2012) Bone turnover markers for osteoporotic status assessment? A systematic review of their diagnosis value at baseline in osteoporosis. Joint Bone Spine 79:20–25
Nielsen J, Oliver S (2005) The next wave in metabolome analysis. Trends Biotechnol 23:544–546
Hirayama A, Kami K, Sugimoto M, Sugawara M, Toki N, Onozuka H, Kinoshita T, Saito N, Ochiai A, Tomita M, Esumi H, Soga T (2009) Quantitative metabolome profiling of colon and stomach cancer microenvironment by capillary electrophoresis time-of-flight mass spectrometry. Cancer Res 69:4918–4925
Zhang Y, Hu C, Hong J, Zeng J, Lai S, Lv A, Su Q, Dong Y, Zhou Z, Tang W, Zhao J, Cui L, Zou D, Wang D, Li H, Liu C, Wu G, Shen J, Zhu D, Wang W, Shen W, Ning G, Xu G (2014) Lipid profiling reveals different therapeutic effects of metformin and glipizide in patients with type 2 diabetes and coronary artery disease. Diabetes Care 37:2804–2812
Yang G, Zhang H, Chen T, Zhu W, Ding S, Xu K, Xu Z, Guo Y, Zhang J (2016) Metabolic analysis of osteoarthritis subchondral bone based on UPLC/Q-TOF-MS. Anal Bioanal Chem 408:4275–4286
Ma B, Liu J, Zhang Q, Ying H, A J SJ, Wu D, Wang Y, Li J, Liu Y (2013) Metabolomic profiles delineate signature metabolic shifts during estrogen deficiency-induced bone loss in rat by GC-TOF/MS. PLoS One 8:e54965
Miyamoto T, Hirayama A, Sato Y, Koboyashi T, Katsuyama E, Kanagawa H, Miyamoto H, Mori T, Yoshida S, Fujie A, Morita M, Watanabe R, Tando T, Miyamoto K, Tsuji T, Funayama A, Nakamura M, Matsumoto M, Soga T, Tomita M, Toyama Y (2017) A serum metabolomics-based profile in low bone mineral density postmenopausal women. Bone 95:1–4
Wang J, Yan D, Hou X, Chen P, Sun Q, Bao Y, Hu C, Zhang Z, Jia W (2017) Association of adiposity indices with bone density and bone turnover in the Chinese population. Osteoporos Int 28:2645–2652
Cheng XG, Yang DZ, Zhou Q, Zhuo TJ, Zhang HC, Xiang J, Wang HF, Ou PZ, Liu JL, Xu L, Huang GY, Huang QR, Barden HS, Weynand LS, Faulkner KG, Meng XW (2007) Age-related bone mineral density, bone loss rate, prevalence of osteoporosis, and reference database of women at multiple centers in China. J Clin Densitom 10:276–284
Abraham A, Pedregosa F, Eickenberg M, Gervais P, Mueller A, Kossaifi J, Gramfort A, Thirion B, Varoquaux G (2014) Machine learning for neuroimaging with scikit-learn. Front Neuroinform 8:14
Touw WG, Bayjanov JR, Overmars L, Backus L, Boekhorst J, Wels M, van Hijum SA (2013) Data mining in the life sciences with random Forest: a walk in the park or lost in the jungle? Brief Bioinform 14:315–326
Colucci S, Mori G, Vaira S, Brunetti G, Greco G, Mancini L, Simone GM, Sardelli F, Koverech A, Zallone A, Grano M (2005) L-carnitine and isovaleryl L-carnitine fumarate positively affect human osteoblast proliferation and differentiation in vitro. Calcif Tissue Int 76:458–465
Aubin I, Adams CP, Opsahl S, Septier D, Bishop CE, Auge N, Salvayre R, Negre-Salvayre A, Goldberg M, Guénet JL, Poirier C (2005) A deletion in the gene encoding sphingomyelin phosphodiesterase 3 (Smpd3) results in osteogenesis and dentinogenesis imperfecta in the mouse. Nat Genet 37:803–805
Farina EK, Kiel DP, Roubenoff R, Schaefer EJ, Cupples LA, Tucker KL (2012) Plasma phosphatidylcholine concentrations of polyunsaturated fatty acids are differentially associated with hip bone mineral density and hip fracture in older adults: the Framingham osteoporosis study. J Bone Miner Res 27:1222–1230
Liu Z, Jeppesen PB, Gregersen S, Chen X, Hermansen K (2008) Dose- and glucose-dependent effects of amino acids on insulin secretion from isolated mouse islets and clonal INS-1E Beta-cells. Rev Diabet Stud 5:232–244
Yang J, Hu X, Zhang Q, Cao H, Wang J, Liu B (2012) Homocysteine level and risk of fracture: A meta-analysis and systematic review. Bone 51:376–382
Jennings A, MacGregor A, Spector T, Cassidy A (2016) Amino acid intakes are associated with bone mineral density and prevalence of low bone mass in women: evidence from discordant monozygotic twins. J Bone Miner Res 31:326–335
MacDonell R, Hamrick MW, Isales CM (2016) Protein/amino-acid modulation of bone cell function. Bonekey Rep 5:827
Chevalley T, Rizzoli R, Manen D, Caverzasio J, Bonjour JP (1998) Arginine increases insulin-like growth factor-I production and collagen synthesis in osteoblast-like cells. Bone 23:103–109
Yamaguchi T, Kanatani M, Yamauchi M, Kaji H, Sugishita T, Baylink DJ, Mohan S, Chihara K, Sugimoto T (2006) Serum levels of insulin-like growth factor (IGF); IGF-binding proteins-3, −4, and −5; and their relationships to bone mineral density and the risk of vertebral fractures in postmenopausal women. Calcif Tissue Int 78:18–24
Lee WC, Guntur AR, Long F, Rosen CJ (2017) Energy metabolism of the osteoblast: implications for osteoporosis. Endocr Rev 38:255–266
Cabral HW, Andolphi BF, Ferreira BV, Alves DC, Morelato RL, Chambo AF, Borges LS (2016) the use of biomarkers in clinical osteoporosis. Rev Assoc Med Bras (1992) 62:368–376
Zaitseva OV, Shandrenko SG, Veliky MM (2015) Biochemical markers of bone collagen type I metabolism. Ukr Biochem J 87:21–32
Engelen MP, Com G, Deutz NE (2014) Increased whole body hydroxyproline production as assessed by a new stable isotope technique is associated with hip and spine bone mineral loss in cystic fibrosis. Clin Nutr 33:1117–1121
Lv H, Jiang F, Guan D, Lu C, Guo B, Chan C, Peng S, Liu B, Guo W, Zhu H, Xu X, Lu A, Zhang G (2016) Metabolomics and its application in the development of discovering biomarkers for osteoporosis research. Int J Mol Sci 17: (12)
Garnero P, Mulleman D, Munoz F, Sornay-Rendu E, Delmas PD (2003) Long-term variability of markers of bone turnover in postmenopausal women and implications for their clinical use: the OFELY study. J Bone Miner Res 18:1789–1794
You YS, Lin CY, Liang HJ, Lee SH, Tsai KS, Chiou JM, Chen YC, Tsao CK, Chen JH (2014) Association between the metabolome and low bone mineral density in Taiwanese women determined by (1)H NMR spectroscopy. J Bone Miner Res 29:212–222
Hernandez-Rauda R, Martinez-Garcia S (2004) Osteoporosis-related life habits and knowledge about osteoporosis among women in El Salvador: a cross-sectional study. BMC Musculoskelet Disord 5:29
Acknowledgements
We thank the participants of the research study. We are grateful for the assistance of the nursing and medical staff at the Shanghai Clinical Centre for Diabetes.
Funding
This work was supported by National Key Research and Development Project of China [2016YFC0903303]; National Natural Science Foundation of China grants [81570713, 91649112]; Outstanding Academic Leaders of Shanghai Health System [2017BR008]; the National Program for Support of Top-notch Young Professionals; Yangtze River Scholar.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics statement
This study was approved by the institutional review board of The Shanghai Jiao Tong University Affiliated Sixth People’s Hospital with the approval number 2015-KY-002(T). It was conducted in accordance with the principles of the Second Revision of the Declaration of Helsinki, and written informed consent was signed by every participant.
Conflicts of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 23 kb)
Rights and permissions
About this article
Cite this article
Wang, J., Yan, D., Zhao, A. et al. Discovery of potential biomarkers for osteoporosis using LC-MS/MS metabolomic methods. Osteoporos Int 30, 1491–1499 (2019). https://doi.org/10.1007/s00198-019-04892-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-04892-0