Abstract
Summary
Potassium bicarbonate was administrated to an already alkaline diet in seven male subjects during a 21-day bed rest study and was able to decrease bed rest induced increased calcium excretion but failed to prevent bed rest-induced bone resorption.
Introduction
Supplementation with alkali salts appears to positively influence calcium and bone metabolism and, thus, could be a countermeasure for population groups with an increased risk for bone loss. However, the extent to which alkalization counteracts acid-induced bone resorption or whether it merely has a calcium and bone maintenance effect is still not completely understood. In the present study, we hypothesized that additional alkalization to an already alkaline diet can further counteract bed rest-induced bone loss.
Methods
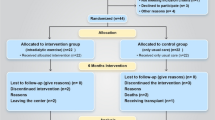
Seven healthy male subjects completed two parts of a crossover designed 21-day bed rest study: bed rest only (control) and bed rest supplemented with 90 mmol potassium bicarbonate (KHCO3) daily.
Results
KHCO3supplementation during bed rest resulted in a more alkaline status compared to the control intervention, demonstrated by the increase in pH and buffer capacity level (pH p = 0.023, HCO3p = 0.02, ABE p = 0.03). Urinary calcium excretion was decreased during KHCO3 supplementation (control 6.05 ± 2.74 mmol/24 h; KHCO3 4.87 ± 2.21 mmol/24 h, p = 0.03); whereas, bone formation was not affected by additional alkalization (bAP p = 0.58; PINP p = 0.60). Bone resorption marker UCTX tended to be lower during alkaline supplementation (UCTX p = 0.16).
Conclusions
The more alkaline acid-base status, achieved by KHCO3 supplementation, reduced renal calcium excretion during bed rest, but was not able to prevent immobilization-induced bone resorption. However, advantages of alkaline salts on bone metabolism may occur under acidic metabolic conditions or with respect to the positive effect of reduced calcium excretion within a longer time frame.
Trial registration
Trial number: NCT01509456



Similar content being viewed by others
References
Arnett T (2003) Regulation of bone cell function by acid-base balance. Proc Nutr Soc 62:511–520
Bushinsky DA (2001) Acid-base imbalance and the skeleton. Eur J Nutr 40:238–244
Bushinsky DA, Frick KK (2000) The effects of acid on bone. Curr Opin Nephrol Hypertens 9:369–379
Bushinsky DA, Gavrilov K, Stathopoulos VM, Krieger NS, Chabala JM, Levi-Setti R (1996) Effects of osteoclastic resorption on bone surface ion composition. Am J Phys 271:C1025–C1031
Krieger NS, Frick KK, Bushinsky DA (2004) Mechanism of acid-induced bone resorption. Curr Opin Nephrol Hypertens 13:423–436
Frassetto LA, Morris RC Jr, Sellmeyer DE, Sebastian A (2008) Adverse effects of sodium chloride on bone in the aging human population resulting from habitual consumption of typical American diets. J Nutr 138:419S–422S
Pizzorno J, Frassetto LA, Katzinger J (2010) Diet-induced acidosis: is it real and clinically relevant? Br J Nutr 103:1185–1194
Vormann J, Remer T (2008) Dietary, metabolic, physiologic, and disease-related aspects of acid-base balance: foreword to the contributions of the second International Acid-Base Symposium. J Nutr 138:413S–414S
Green J, Kleeman CR (1991) Role of bone in regulation of systemic acid-base balance. Kidney Int 39:9–26
Wynn E, Krieg MA, Lanham-New SA, Burckhardt P (2010) Postgraduate Symposium: positive influence of nutritional alkalinity on bone health. Proc Nutr Soc 69:166–173
Burckhardt P (2016) The role of low acid load in vegetarian diet on bone health: a narrative review. Swiss Med Wkly 146:w14277
Frings-Meuthen P, Baecker N, Heer M (2008) Low-grade metabolic acidosis may be the cause of sodium chloride-induced exaggerated bone resorption. J Bone Mineral Res 23:517–524
Frings-Meuthen P, Buehlmeier J, Baecker N, Stehle P, Fimmers R, May F, Kluge G, Heer M (2011) High sodium chloride intake exacerbates immobilization-induced bone resorption and protein losses. J Appl Physiol 111(1985):537–542
Lambert H, Frassetto L, Moore JB, Torgerson D, Gannon R, Burckhardt P, Lanham-New S (2015) The effect of supplementation with alkaline potassium salts on bone metabolism: a meta-analysis. Osteoporosis international : a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA 26:1311–1318
Bushinsky DA (1996) Metabolic alkalosis decreases bone calcium efflux by suppressing osteoclasts and stimulating osteoblasts. Am J Phys 271:F216–F222
Wynn E, Krieg MA, Aeschlimann JM, Burckhardt P (2009) Alkaline mineral water lowers bone resorption even in calcium sufficiency: alkaline mineral water and bone metabolism. Bone 44:120–124
Sebastian A, Harris ST, Ottaway JH, Todd KM, Morris RC Jr (1994) Improved mineral balance and skeletal metabolism in postmenopausal women treated with potassium bicarbonate. N Engl J Med 330:1776–1781
Buclin T, Cosma M, Appenzeller M, Jacquet AF, Decosterd LA, Biollaz J, Burckhardt P (2001) Diet acids and alkalis influence calcium retention in bone. Osteoporos Int 12:493–499
Gregory NS, Kumar R, Stein EM, Alexander E, Christos P, Bockman RS, Rodman JS (2015) Potassium citrate decreases bone resorption in postmenopausal women with osteopenia: a randomized, double-blind clinical trial. Endocr Pract 21:1380–1386
New SA, MacDonald HM, Campbell MK, Martin JC, Garton MJ, Robins SP, Reid DM (2004) Lower estimates of net endogenous non-carbonic acid production are positively associated with indexes of bone health in premenopausal and perimenopausal women. Am J Clin Nutr 79:131–138
Remer T, Krupp D, Shi L (2014) Dietary protein’s and dietary acid load’s influence on bone health. Crit Rev Food Sci Nutr 54:1140–1150
Jehle S, Hulter HN, Krapf R (2013) Effect of potassium citrate on bone density, microarchitecture, and fracture risk in healthy older adults without osteoporosis: a randomized controlled trial. J Clin Endocrinol Metab 98:207–217
Smith SM, Heer MA, Shackelford LC, Sibonga JD, Ploutz-Snyder L, Zwart SR (2012) Benefits for bone from resistance exercise and nutrition in long-duration spaceflight: evidence from biochemistry and densitometry. J Bone Mineral Res 27:1896–1906
Baecker N, Tomic A, Mika C, Gotzmann A, Platen P, Gerzer R, Heer M (2003) Bone resorption is induced on the second day of bed rest: results of a controlled crossover trial. J Appl Physiol 95(1985):977–982
Jost PD (2008) Simulating human space physiology with bed rest. Hippokratia 12(Suppl 1):37–40
Biolo G, Heer M, Narici M, Strollo F (2003) Microgravity as a model of ageing. Curr Opin Clin Nutr Metab Care 6:31–40
Vernikos J, Schneider VS (2010) Space, gravity and the physiology of aging: parallel or convergent disciplines? A mini-review. Gerontology 56:157–166
Remer T, Manz F (1994) Estimation of the renal net acid excretion by adults consuming diets containing variable amounts of protein. Am J Clin Nutr 59:1356–1361
Tucker KL, Hannan MT, Chen H, Cupples LA, Wilson PW, Kiel DP (1999) Potassium, magnesium, and fruit and vegetable intakes are associated with greater bone mineral density in elderly men and women. Am J Clin Nutr 69:727–736
Prynne CJ, Mishra GD, O'Connell MA, Muniz G, Laskey MA, Yan L, Prentice A, Ginty F (2006) Fruit and vegetable intakes and bone mineral status: a cross sectional study in 5 age and sex cohorts. Am J Clin Nutr 83:1420–1428
Macdonald HM, Black AJ, Aucott L, Duthie G, Duthie S, Sandison R, Hardcastle AC, Lanham New SA, Fraser WD, Reid DM (2008) Effect of potassium citrate supplementation or increased fruit and vegetable intake on bone metabolism in healthy postmenopausal women: a randomized controlled trial. Am J Clin Nutr 88:465–474
Dawson-Hughes B, Harris SS, Palermo NJ, Castaneda-Sceppa C, Rasmussen HM, Dallal GE (2009) Treatment with potassium bicarbonate lowers calcium excretion and bone resorption in older men and women. J Clin Endocrinol Metab 94:96–102
Wynn E, Lanham-New SA, Krieg MA, Whittamore DR, Burckhardt P (2008) Low estimates of dietary acid load are positively associated with bone ultrasound in women older than 75 years of age with a lifetime fracture. J Nutr 138:1349–1354
Edelstein SL, Barrett-Connor E (1993) Relation between body size and bone mineral density in elderly men and women. Am J Epidemiol 138:160–169
Segal NA, Torner JC, Yang M, Curtis JR, Felson DT, Nevitt MC (2008) Muscle mass is more strongly related to hip bone mineral density than is quadriceps strength or lower activity level in adults over age 50 year. J Clin Densitom 11:503–510
Lubran MM (1995) Renal function in the elderly. Ann Clin Lab Sci 25:122–133
Lemann J Jr, Gray RW, Pleuss JA (1989) Potassium bicarbonate, but not sodium bicarbonate, reduces urinary calcium excretion and improves calcium balance in healthy men. Kidney Int 35:688–695
Ceglia L, Harris SS, Abrams SA, Rasmussen HM, Dallal GE, Dawson-Hughes B (2009) Potassium bicarbonate attenuates the urinary nitrogen excretion that accompanies an increase in dietary protein and may promote calcium absorption. J Clin Endocrinol Metab 94:645–653
Whitson PA, Pietrzyk RA, Pak CY (1997) Renal stone risk assessment during space shuttle flights. J Urol 158:2305–2310
Whitson PA, Pietrzyk RA, Pak CY, Cintron NM (1993) Alterations in renal stone risk factors after space flight. J Urol 150:803–807
Pietrzyk RA, Jones JA, Sams CF, Whitson PA (2007) Renal stone formation among astronauts. Aviat Space Environ Med 78:A9–A13
Whitson PA, Pietrzyk RA, Morukov BV, Sams CF (2001) The risk of renal stone formation during and after long duration space flight. Nephron 89:264–270
Whitson PA, Pietrzyk RA, Jones JA, Nelman-Gonzalez M, Hudson EK, Sams CF (2009) Effect of potassium citrate therapy on the risk of renal stone formation during spaceflight. J Urol 182:2490–2496
Zerwekh JE, Odvina CV, Wuermser LA, Pak CY (2007) Reduction of renal stone risk by potassium-magnesium citrate during 5 weeks of bed rest. J Urol 177:2179–2184
Scales CD Jr, Smith AC, Hanley JM, Saigal CS (2012) Prevalence of kidney stones in the United States. Eur Urol 62:160–165
Acknowledgments
Firstly, we are very grateful to the test subjects and the study management team at DLR, who took care of the subjects in the laboratory. We are also grateful to H. Soll and P. Goerke, who performed the psychological evaluations of the test subjects. G. Kraus, I. Schrage, and E. Huth are acknowledged for the biochemical analysis. The authors thank Karina Marshall-Goebel for her assistance in the preparation of this manuscript.
M. Heer has recently moved from DLR, Cologne, Germany to University of Bonn, Germany.
N. Baecker has recently moved from DLR, Cologne, Germany to University of Bonn, Germany.
J. Buehlmeier has recently moved from DLR, Cologne, Germany to the University Hospital Essen, University of Duisburg-Essen, Germany.
G. Bernhardt has recently moved to Novartis, Basel Switzerland as a freelancer.
Grants
The study 2 was funded by the European Space Agency (ESA) as part of the “Microgravity Applications Programme” (contract number: 21381/08/NL/VJ) and by institutional funding of the German Aerospace Center (DLR Space Programme).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Frings-Meuthen, P., Bernhardt, G., Buehlmeier, J. et al. The negative effect of unloading exceeds the bone-sparing effect of alkaline supplementation: a bed rest study. Osteoporos Int 30, 431–439 (2019). https://doi.org/10.1007/s00198-018-4703-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-018-4703-6