Abstract
Summary
Apparent modulus and failure stress of trabecular bone structure from 45 women with osteoporosis treated with bisphosphonates for varying durations were studied using finite element analyses and statistical modeling. Following adjustments for patient age and bone volume, increasing bisphosphonate treatment duration for up to 7.3 years was associated with treatment–time-dependent increases in bone apparent modulus and failure stress. Treatment durations exceeding 7.3 years were associated with time-dependent decreases in apparent modulus and failure stress from the peak values observed.
Introduction
The purpose of this study was to clarify the relationship between bisphosphonate (BP) treatment duration and human bone quality. This study quantified changes in the apparent modulus and failure stress of trabecular bone biopsied from patients with osteoporosis who were treated with BPs for widely varying durations.
Methods
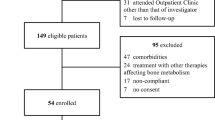
Forty-five iliac crest bone samples were obtained from women with osteoporosis who were continuously treated with oral BPs for varying periods of up to 16 years. Micro-CT imaging was used to develop three-dimensional virtual models of the trabecular bone from these samples. Apparent modulus and failure stress of these virtual models were determined using finite element analyses (FEA). Polynomial regression and cubic splines, adjusted for relevant (age and BV/TV) covariates, were used to statistically model the data and quantify the relationships between BP treatment duration and apparent modulus or failure stress.
Results
Second-order polynomial models were needed to relate apparent modulus or failure stress to BP treatment duration. These models showed that these bone quality parameters (a) increased with increasing BP treatment duration up to approximately 7.3 years, (b) reached a maximum at this (~7.3 years) time, and then (c) declined with BP treatment durations exceeding ~7.3 years. A similar result was obtained by modeling with cubic splines.
Conclusions
Changes in FEA-derived apparent stiffness and failure stress are attributable to changes in trabecular bone structure, which in turn are related to the duration of BP treatment. These relationships are evident even after adjustments are made in the statistical models for changes in age and BV/TV. According to these models, increases in trabecular bone apparent stiffness and failure stress linked to BPs cease and appear to reverse after approximately 7.3 years of treatment. Conclusions regarding optimal BP therapy duration await study of additional bone quality parameters.



Similar content being viewed by others
References
Schmidt GA, Horner KE, McDanel DL, Ross MB, Moores KG (2010) Risks and benefits of long-term bisphosphonate therapy. Am J Health Syst Pharm 67(12):994–1001
Chavassieux PM, Arlot ME, Reda C, Wei L, Yates AJ, Meunier PJ (1997) Histomorphometric assessment of the long-term effects of alendronate on bone quality and remodeling in patients with osteoporosis. J Clin Invest 100(6):1475–1480
Drake MT, Clarke BL, Khosla S (2008) Bisphosphonates: mechanism of action and role in clinical practice. Mayo Clin Proc 83(9):1032–1045
Plotkin LI, Weinstein RS, Parfitt AM, Roberson PK, Manolagas SC, Bellido T (1999) Prevention of osteocyte and osteoblast apoptosis by bisphosphonates and calcitonin. J Clin Invest 104(10):1363–1374
Liberman UA, Weiss SR, Broll J et al (1995) Effect of oral alendronate on bone mineral density and the incidence of fractures in postmenopausal osteoporosis. The Alendronate Phase III Osteoporosis Treatment Study Group. N Engl J Med 333(22):1437–1443
Cummings SR, Black DM, Thompson DE et al (1998) Effect of alendronate on risk of fracture in women with low bone density but without vertebral fractures: results from the Fracture Intervention Trial. JAMA 280(24):2077–2082
Harris ST, Watts NB, Genant HK et al (1999) Effects of risedronate treatment on vertebral and nonvertebral fractures in women with postmenopausal osteoporosis: a randomized controlled trial. Vertebral Efficacy with Risedronate Therapy (VERT) Study Group. JAMA 282(14):1344–1352
Bilezikian JP (2009) Efficacy of bisphosphonates in reducing fracture risk in postmenopausal osteoporosis. Am J Med 122(2 Suppl):S14–S21
Black DM, Schwartz AV, Ensrud KE et al (2006) Effects of continuing or stopping alendronate after 5 years of treatment: the Fracture Intervention Trial Long-term Extension (FLEX): a randomized trial. JAMA 296(24):2927–2938
Schuit SC, van der Klift M, Weel AE et al (2004) Fracture incidence and association with bone mineral density in elderly men and women: the Rotterdam Study. Bone 34(1):195–202
Dell RM, Adams AL, Greene DF et al (2012) Incidence of atypical nontraumatic diaphyseal fractures of the femur. J Bone Miner Res 27(12):2544–2550
Shane E, Burr D, Ebeling PR et al (2010) Atypical subtrochanteric and diaphyseal femoral fractures: report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res 25(11):2267–2294
Meier RP, Perneger TV, Stern R, Rizzoli R, Peter RE (2012) Increasing occurrence of atypical femoral fractures associated with bisphosphonate use. Arch Intern Med 172(12):930–936
Whitaker M, Guo J, Kehoe T, Benson G (2012) Bisphosphonates for osteoporosis—where do we go from here? N Engl J Med 366(22):2048–2051
Adler RA, El-Hajj Fuleihan G, Bauer DC et al (2016) Managing osteoporosis in patients on long-term bisphosphonate treatment: report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res 31(1):16–35
Recker RR, Lewiecki EM, Miller PD, Reiffel J (2009) Safety of bisphosphonates in the treatment of osteoporosis. Am J Med 122(2 Suppl):S22–S32
Odvina CV, Zerwekh JE, Rao DS, Maalouf N, Gottschalk FA, Pak CY (2005) Severely suppressed bone turnover: a potential complication of alendronate therapy. J Clin Endocrinol Metab 90(3):1294–1301
Ott SM (2005) Long-term safety of bisphosphonates. J Clin Endocrinol Metab 90(3):1897–1899
Bala Y, Depalle B, Farlay D et al (2012) Bone micromechanical properties are compromised during long-term alendronate therapy independently of mineralization. J Bone Miner Res 27(4):825–834
Nazarian A, Stauber M, Zurakowski D, Snyder BD, Muller R (2006) The interaction of microstructure and volume fraction in predicting failure in cancellous bone. Bone 39(6):1196–1202
Karim L, Vashishth D (2011) Role of trabecular microarchitecture in the formation, accumulation, and morphology of microdamage in human cancellous bone. J Orthop Res 29(11):1739–1744
Turner CH (2002) Biomechanics of bone: determinants of skeletal fragility and bone quality. Osteoporos Int 13(2):97–104
Borah B, Dufresne TE, Chmielewski PA, Johnson TD, Chines A, Manhart MD (2004) Risedronate preserves bone architecture in postmenopausal women with osteoporosis as measured by three-dimensional microcomputed tomography. Bone 34(4):736–746
Pazianas M, van der Geest S, Miller P (2014) Bisphosphonates and bone quality. BoneKEy Rep 3:529
Pistoia W, van Rietbergen B, Lochmuller EM, Lill CA, Eckstein F, Ruegsegger P (2002) Estimation of distal radius failure load with micro-finite element analysis models based on three-dimensional peripheral quantitative computed tomography images. Bone 30(6):842–848
Chevalier Y, Pahr D, Allmer H, Charlebois M, Zysset P (2007) Validation of a voxel-based FE method for prediction of the uniaxial apparent modulus of human trabecular bone using macroscopic mechanical tests and nanoindentation. J Biomech 40(15):3333–3340
Macneil JA, Boyd SK (2008) Bone strength at the distal radius can be estimated from high-resolution peripheral quantitative computed tomography and the finite element method. Bone 42(6):1203–1213
Harrison NM, McDonnell P, Mullins L, Wilson N, O’Mahoney D, McHugh PE (2013) Failure modelling of trabecular bone using a non-linear combined damage and fracture voxel finite element approach. Biomech Model Mechanobiol 12(2):225–241
Zysset PK, Dall’ara E, Varga P, Pahr DH (2013) Finite element analysis for prediction of bone strength. BoneKEy Rep 2:386
Britton JM, Davie MW (1990) Mechanical properties of bone from iliac crest and relationship to L5 vertebral bone. Bone 11(1):21–28
Mosekilde L, Viidik A, Mosekilde L (1985) Correlation between the compressive strength of iliac and vertebral trabecular bone in normal individuals. Bone 6(5):291–295
Neo M, Herbst H, Voigt CF, Gross UM (1998) Temporal and spatial patterns of osteoblast activation following implantation of beta-TCP particles into bone. J Biomed Mater Res 39(1):71–76
Malluche HH, Monier–Faugere MC (1997) In: Avioli LV, Krane SM (eds) Bone biopsies: a modern approach in metabolic bone disease, 3rd edn. WB Saunders Co, Philadelphia, pp 237–273
Malluche HHMH, Monier-Faugere MC (2008) Bone biopsy in patients with osteoporosis. Curr Osteoporos Rep 5(4):146–152
Malluche HH M-FM (1986) Atlas of mineralized bone histology. Karger
Malluche HH, Porter DS, Monier-Faugere MC, Mawad H, Pienkowski D (2012) Differences in bone quality in low- and high-turnover renal osteodystrophy. J Am Soc Nephrol 23(3):525–532
van Rietbergen B, Weinans H, Huiskes R, Odgaard A (1995) A new method to determine trabecular bone elastic properties and loading using micromechanical finite-element models. J Biomech 28(1):69–81
Waarsing JH, Day JS, Weinans H (2004) An improved segmentation method for in vivo micro-CT imaging. J Bone Miner Res 19(10):1640–1650
Ruegsegger P, Koller B, Muller R (1996) A microtomographic system for the nondestructive evaluation of bone architecture. Calcif Tissue Int 58(1):24–29
Ding M, Odgaard A, Hvid I (1999) Accuracy of cancellous bone volume fraction measured by micro-CT scanning. J Biomech 32(3):323–326
Wilkerson LT (2012) Finite element analysis of cancellous bone. Theses and Dissertations: Mechanical Engineering, University of Kentucky
Burkhart TA, Andrews DM, Dunning CE (2013) Finite element modeling mesh quality, energy balance and validation methods: a review with recommendations associated with the modeling of bone tissue. J Biomech 46(9):1477–1488
Polly BJ, Yuya PA, Akhter MP, Recker RR, Turner JA (2012) Intrinsic material properties of trabecular bone by nanoindentation testing of biopsies taken from healthy women before and after menopause. Calcif Tissue Int 90(4):286–293
Bevill G, Keaveny TM (2009) Trabecular bone strength predictions using finite element analysis of micro-scale images at limited spatial resolution. Bone 44(4):579–584
Un K, Bevill G, Keaveny TM (2006) The effects of side-artifacts on the elastic modulus of trabecular bone. J Biomech 39(11):1955–1963
Wood S (2006) Generalized additive models: an introduction with R, 1st edn. Chapman & Hall/CRC, New York
Wahba G (1990) Spline models for observational data, 1st edn. SIAM, Philadelphia
Ruppert D, Wand M, Carrol RJ (2003) Semiparametric regression, 1st edn. Cambridge University Press, New York
Borah B, Dufresne TE, Ritman EL et al (2006) Long-term risedronate treatment normalizes mineralization and continues to preserve trabecular architecture: sequential triple biopsy studies with micro-computed tomography. Bone 39(2):345–352
Day JS, Ding M, Bednarz P et al (2004) Bisphosphonate treatment affects trabecular bone apparent modulus through micro-architecture rather than matrix properties. J Orthop Res 22(3):465–471
Keaveny TM, Hoffmann PF, Singh M et al (2008) Femoral bone strength and its relation to cortical and trabecular changes after treatment with PTH, alendronate, and their combination as assessed by finite element analysis of quantitative CT scans. J Bone Miner Res 23(12):1974–1982
Imai K, Ohnishi I, Matsumoto T, Yamamoto S, Nakamura K (2009) Assessment of vertebral fracture risk and therapeutic effects of alendronate in postmenopausal women using a quantitative computed tomography-based nonlinear finite element method. Osteoporos Int 20(5):801–810
Lewiecki EM, Keaveny TM, Kopperdahl DL et al (2009) Once-monthly oral ibandronate improves biomechanical determinants of bone strength in women with postmenopausal osteoporosis. J Clin Endocrinol Metab 94(1):171–180
Burghardt AJ, Kazakia GJ, Sode M, de Papp AE, Link TM, Majumdar S (2010) A longitudinal HR-pQCT study of alendronate treatment in postmenopausal women with low bone density: relations among density, cortical and trabecular microarchitecture, biomechanics, and bone turnover. J Bone Miner Res 25(12):2558–2571
What is Osteoporosis? [website]. http://nof.org/articles/7, 2014
Borah B, Dufresne TE, Chmielewski PA, Gross GJ, Prenger MC, Phipps RJ (2002) Risedronate preserves trabecular architecture and increases bone strength in vertebra of ovariectomized minipigs as measured by three-dimensional microcomputed tomography. J Bone Miner Res 17(7):1139–1147
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Research support
This study was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases of the National Institutes of Health under award number R01 AR061578 and the Kentucky Nephrology Research Trust. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Ward, J., Wood, C., Rouch, K. et al. Stiffness and strength of bone in osteoporotic patients treated with varying durations of oral bisphosphonates. Osteoporos Int 27, 2681–2688 (2016). https://doi.org/10.1007/s00198-016-3661-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-016-3661-0