Abstract
Summary
Evaluation of 234 men referred for osteoporosis found many with undiagnosed secondary causes and multiple unrecognized risk factors.
Introduction
Studies in women with postmenopausal osteoporosis suggest that many have unrecognized disorders affecting bone. Men are considered more likely to have underlying, possibly correctable causes. We studied the prevalence of risk factors, secondary causes, and laboratory abnormalities in men with and without previously known causes for osteoporosis.
Methods
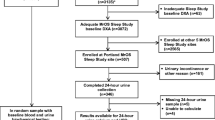
We reviewed the charts of 234 men with osteoporosis diagnosed by bone mineral density testing. In addition to screening chemistries, 25-hydroxyvitamin D, testosterone, luteinizing hormone, follicle-stimulating hormone, thyroid-stimulating hormone, and spot urinary calcium-to-creatinine ratio were measured.
Results
The mean age was 70.6 years and mean weight was 76.4 kg. The mean T-score for spine, femoral neck, and forearm was −2.2, −2.4, and −2.3, respectively. Evaluation revealed secondary osteoporosis in 75% overall including hypogonadism, vitamin D deficiency, hypercalciuria, subclinical hyperthyroidism, and hyperparathyroidism. In those men with known secondary osteoporosis at the time of dual energy X-ray absorptiometry testing, additional diagnoses were found in just over half. Vitamin D deficiency and insufficiency were very common, and other common risk factors for osteoporosis included age >65, current smoking, and prior fracture. Half of the subjects had ≥4 risk factors.
Conclusion
Evaluation revealed a specific cause in about half of men thought to have primary osteoporosis. Among men with known secondary osteoporosis, additional risk factors and secondary causes were frequently identified. In conclusion, a relatively modest evaluation of men with osteoporosis will often provide useful information.


Similar content being viewed by others
References
Jones G, Nguyen T, Sambrook PN, Kelly PJ, Gilbert C, Eisman JA (1994) Symptomatic fracture incidence in elderly men and women: the Dubbo Osteoporosis Epidemiology Study (DOES). Osteoporos Int 4:277–282
Cooper C, Atkinson EJ, Jacobsen SJ, O’Fallon WM, Melton LJ III (1993) Population-based study of survival after osteoporotic fractures. Am J Epidemiol 137:1001–1005
Sernbo I, Johnell O (1993) Consequences of a hip fracture: a prospective study over 1 year. Osteoporos Int 3:148–153
Kelepouris N, Harper KD, Gannon F, Kaplan FS, Haddad JG (1995) Severe osteoporosis in men. Ann Intern Med 123:452–460
Caplan GA, Scane AC, Francis RM (1994) Pathogenesis of vertebral crush fractures in women. J R Soc Med 87:200–202
Hanley DA, Brown JP, Tenenhouse A, Olszynski WP, Ioannidis G, Berger C, Prior JC, Pickard L, Murray RM, Anastassiades T, Kirkland S, Joyce C, Joseph L, Papaioannou A, Jackson SA, Poliquin S, Adachi JD, Canadian Multicentre Osteoporosis Study Research Group (2003) Association among disease conditions, bone mineral density, and prevalent vertebral deformities in men and women 50 years of age and older: cross-sectional results from the Canadian Multicentre Osteoporosis Study. J Bone Miner Res 18:784–790
Tannenbaum C, Clark J, Schwartzman K, Wallenstein S, Lapinski R, Meier D, Luckey M (2002) Yield of laboratory testing to identify secondary contributors to osteoporosis in otherwise healthy women. J Clin Endocrinol Metab 87:4431–4437
Adler RA, Tran MT, Petkov VI (2003) Performance of the osteoporosis self-assessment screening tool for osteoporosis in American men. Mayo Clin Proc 78:723–727
Wiliams MI, Petkov VI, Biskobing DM, Adler RA (2004) The Osteoporosis Self-Assessment Tool (OST) leads to increased osteoporosis evaluation and therapy in men. American Society for Bone and Mineral Research Annual Meeting, #SU-482 (abstract)
Simonelli C, Adler RA, Blake GM, Caudill JP, Khan A, Leib E, Maricic M, Prior JC, Eis SR, Rosen C, Kendler DL (2008) Dual-energy X-ray absorptiometry technical issues: the 2007 ISCD official positions. J Clin Densitom 11:109–122
Qaseem A, Snow V, Shekelle P, Hopkins R Jr, Forciea MA, Owens DK, Clinical Efficacy Assessment Subcommittee of the American College of Physicians (2008) Screening for osteoporosis in men: a clinical practice guideline from the American College of Physicians. Ann Intern Med 148:680–684
Baillie SP, Davison CE, Johnson FJ, Francis RM (1992) Pathogenesis of vertebral crush fractures in men. Age Ageing 21:139–141
Pye SR, Adams KR, Halsey JP, Klimiuk P, Knight SM, Pal B, Selby PL, Stewart IM, Swinson DR, O’Neill TW (2003) Frequency and causes of osteoporosis in men. Rheumatology (Oxford) 42:811–812
Evans SF, Davie MW (2000) Vertebral fractures and bone mineral density in idiopathic, secondary and corticosteroid associated osteoporosis in men. Ann Rheum Dis 59:269–275
Dawson-Hughes B, Heaney RP, Holick MF, Lips P, Meunier PJ, Vieth R (2005) Estimates of optimal vitamin D status. Osteoporos Int 16:713–716
Dawson-Hughes B, Mithal A, Bonjour JP, Boonen S, Burckhardt P, Fuleihan GE, Josse RG, Lips P, Morales-Torres J, Yoshimura N (2010) IOF position statement: vitamin D recommendations for older adults. Osteoporosis Int 21:1151–1154
Luckey MM, Tannenbaum C (2003) Authors’ response: recommended testing in patients with low bone density. J Clin Endocrinol Metab 88:1405
Binkley N, Krueger D, Cowgill CS, Plum L, Lake E, Hansen KE, DeLuca HF, Drezner MK (2004) Assay variation confounds the diagnosis of hypovitaminosis D: a call for standardization. J Clin Endocrinol Metab 89:3152–3157
Levis S, Gomez A, Jimenez C, Veras L, Ma F, Lai S, Hollis B, Roos BA (2005) Vitamin D deficiency and seasonal variation in an adult South Florida population. J Clin Endocrinol Metab 90:1557–1562
Binkley N, Novotny R, Krueger D, Kawahara T, Daida YG, Lensmeyer G, Hollis BW, Drezner MK (2007) Low vitamin D status despite abundant sun exposure. J Clin Endocrinol Metab 92:2130–2135
Kumari M, Judd SE, Tangpricha V (2008) Vitamin D status in United States war veterans. Endocr Pract 14:127–128
Peris P, Guanabens N, Monegal A, Suris X, Alvarez L, Martinez de Osaba MJ, Hernandez MV, Munoz-Gomez J (1995) Aetiology and presenting symptoms in male osteoporosis. Br J Rheumatol 34:936–941
Perry HM III, Fallon MD, Bergfeld M, Teitelbaum SL, Avioli LV (1982) Osteoporosis in young men: a syndrome of hypercalciuria and accelerated bone turnover. Arch Intern Med 142:1295–1298
Pak CY, Kaplan R, Bone H, Townsend J, Waters O (1975) A simple test for the diagnosis of absorptive, resorptive and renal hypercalciurias. N Engl J Med 292:497–500
Stanley HL, Schmitt BP, Poses RM, Deiss WP (1991) Does hypogonadism contribute to the occurrence of a minimal trauma hip fracture in elderly men? J Am Geriatr Soc 39:766–771
Abbasi AA, Rudman D, Wilson CR, Drinka PJ, Basu SN, Mattson DE, Richardson TJ (1995) Observations on nursing home residents with a history of hip fracture. Am J Med Sci 310:229–234
Wang C, Neischlag E, Swerdloff R, Behre HM, Hellstrom WJ, Gooren LJ, Kaufman JM, Legros J-J, Lunenfeld B, Morales A, Morley JE, Schulman C, Thompson IM, Weidner W, Wu FCW (2009) Investigation, treatment, and monitoring of late-onset hypogonadism in males; ISA, ISSAM, EAU, EAA, and ASA recommendations. J Androl 30:1–9
Harman SM, Metter EJ, Tobin JD, Pearson J, Blackman MR (2001) Longitudinal effects of aging on serum total and free testosterone levels in healthy men. Baltimore Longitudinal Study of Aging. J Clin Endocrinol Metab 86:724–731
Snyder PJ, Peachey H, Hannoush P, Berlin JA, Loh L, Holmes JH, Diewati A, Santanna RCJ, Strom BL (1999) Effect of testosterone treatment on bone mineral density in men over 65 years of age. J Clin Endocrinol Metab 84:1966–1972
Snyder PJ (2004) Hypogonadism in elderly men—what to do until the evidence comes. N Engl J Med 350:440–442
Kaufman JM, Vermeulen A (2005) The decline of androgen levels in elderly men and its clinical and therapeutic implications. Endocr Rev 26:833–876
Kelleher S, Conway AJ, Handelsman DJ (2004) Blood testosterone threshold for androgen deficiency syndromes. J Clin Endocrinol Metab 89:2813–3817
Koh LK, Sedrine WB, Torralba TP, Kung A, Fujiwara S, Chan SP, Huang QR, Rajatanavin R, Tsai KS, Park HM, Reginster JY, Osteoporosis Self-Assessment Tool for Asians (OSTA) Research Group (2001) A simple tool to identify Asian women at increased risk of osteoporosis. Osteoporos Int 12:699–705
Edwards BJ, Langman CB, Bunta AD, Vicuna M, Favus M (2008) Secondary contributors to bone loss in osteoporosis related hip fractures. Osteoporos Int 19:991–999
Dumitrescu B, van Helden S, ten Broeke R, Nieuwenhuijzen-Kruseman A, Wyers C, Udrea G, van der Linden S, Geusens P (2008) Evaluation of patients with a recent clinical fracture and osteoporosis, a multidisciplinary approach. BMC Musculoskelet Disord 9:109
Johnson SL, Petkov VI, Williams MI, Via PS, Adler RA (2005) Improving osteoporosis management in patients with fractures. Osteoporos Int 16:1079–1085
Papaioannu A, Kennedy CC, Cranney A, Hawker G, Brown JP, Kaiser SM, Leslie WD, O’Brien CJM, Sawka AM, Khan A, Siminoski K, Tarulli G, Webster D, McGowan J, Adachi JD (2009) Risk factors for low BMD in healthy men age 50 years or older: a systematic review. Osteoporos Int 20:507–518
Thomas-John M, Codd MB, Manne S, Watts NB, Mongey AB (2009) Risk factors for the development of osteoporosis and osteoporotic fractures among older men. J Rheumatol 36:1947–1952
Trimpou P, Landin-Wilhelmsen K, Oden A, Rosengren A, Wilhelmsen L (2010) Male risk factors for hip fracture—a 30-year follow-up study in 7, 495 men. Osteoporos Int 21:409–416
Adler RA (1992) Clinical review 33: clinically important effects of alcohol on endocrine function. J Clin Endocrinol Metab 74:957–960
Felson DT, Kiel DP, Anderson JJ, Kannel WB (1988) Alcohol consumption and hip fractures: the Framingham Study. Am J Epidemiol 128:1102–1110
Poor G, Atkinson EJ, O’Fallon WM, Melton LJ III (1995) Predictors of hip fractures in elderly men. J Bone Miner Res 10:1900–1907
Kanis JA, Oden A, Johansson H, Borgstrom F, Strom O, McCloskey E (2009) FRAX® and its application to clinical practice. Bone 44:734–743
Conflicts of interest
RAA has received research support from Genentech, Novartis, Eli Lilly, Amgen, and Merck and is a consultant for Eli Lilly, Merck, and GTX, Inc. CSR and VIP have indicated they have nothing to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ryan, C.S., Petkov, V.I. & Adler, R.A. Osteoporosis in men: the value of laboratory testing. Osteoporos Int 22, 1845–1853 (2011). https://doi.org/10.1007/s00198-010-1421-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-010-1421-0