Abstract
Summary
Bisphosphonates have been associated with an increased risk of atrial fibrillation and may thus be associated with an increased risk of ischemic stroke. This would have substantial clinical and public health implications. We found no evidence of an association between bisphosphonate use and risk of ischemic stroke.
Introduction
Bisphosphonates have been associated with an increased risk of atrial fibrillation in some studies and may be associated with an increased risk of ischemic stroke. However, data regarding these possibilities are limited.
Methods
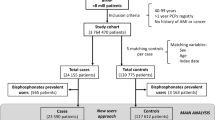
We conducted a population-based case–control study of 6,257 female cases of ischemic stroke and 31,285 age- and gender-matched population controls. Data on bisphosphonate use, other medication use, comorbidity, and ischemic stroke were obtained from medical databases. Current bisphosphonate use was defined as at least one redeemed prescription within 90 days before diagnosis/index date. We estimated the odds ratio (OR) of ischemic stroke among users and nonusers of bisphosphonates using conditional logistic regression, controlling for potential confounding factors.
Results
One hundred eighty-two (2.9%) cases and 901 (2.9%) controls were current users of bisphosphonates. Etidronate and alendronate were prescribed with similar frequency among cases and controls. The adjusted OR of ischemic stroke for bisphosphonate users compared with nonusers was 0.97 (95% confidence interval [CI], 0.82–1.15). New and continuing bisphosphonate users had adjusted ORs for ischemic stroke of 1.16 (95% CI, 0.69–1.96) and 0.97 (95% CI, 0.81–1.16), respectively. Excluding patients with known atrial fibrillation/flutter yielded an OR of 1.00 (95% CI, 0.85–1.19). The OR for ischemic stroke was 0.59 (95% CI, 0.32–1.09) among patients with a history of previous hospitalization for cardiovascular disease and 1.07 (95% CI, 0.88–1.18) among those without (P < 0.001). The OR for former users was 1.23 (95% CI, 1.01–1.49).
Conclusion
We found no evidence of an association of oral bisphosphonate use with the risk of ischemic stroke.
Similar content being viewed by others
References
Black DM, Delmas PD, Eastell R et al (2007) Once-yearly zoledronic acid for treatment of postmenopausal osteoporosis. N Engl J Med 356(18):1809–1822
Cummings SR, Schwartz AV, Black DM (2007) Alendronate and atrial fibrillation. N Engl J Med 356(18):1895–1896
Heckbert SR, Li G, Cummings SR, Smith NL, Psaty BM (2008) Use of alendronate and risk of incident atrial fibrillation in women. Arch Intern Med 168(8):826–831
Karam R, Camm J, McClung M (2007) Yearly zoledronic acid in postmenopausal osteoporosis. N Engl J Med 357(7):712–713
Lyles KW, Colón-Emeric CS, Magaziner JS et al (2007) HORIZON recurrent fracture trial. Zoledronic acid and clinical fractures and mortality after hip fracture. N Engl J Med 357(18):1799–1809
Sørensen HT, Christensen S, Mehnert F et al (2008) Use of bisphosphonates among women and risk of atrial fibrillation and flutter: population based case–control study. BMJ 336(7648):813–816
Wolf PA, Abbott RD, Kannel WB (1991) Atrial fibrillation as an independent risk factor for stroke: the Framingham study. Stroke 22(8):983–988
Grosso A, Douglas I, Hingorani A, MacAllister R, Smeeth L (2009) Oral bisphosphonates and risk of atrial fibrillation and flutter in women: a self-controlled case-series safety analysis. PLoS ONE 4(3):e4720
Frost L, Engholm G, Johnsen S, Moller H, Husted S (2000) Incident stroke after discharge from the hospital with a diagnosis of atrial fibrillation. Am J Med 108(1):36–40
Kaarisalo MM, Immonen-Räihä P, Marttila RJ et al (1997) Atrial fibrillation and stroke. Mortality and causes of death after the first acute ischemic stroke. Stroke 28(2):311–315
Sandercock P, Bamford J, Dennis M et al (1992) Atrial fibrillation and stroke: prevalence in different types of stroke and influence on early and long term prognosis (Oxfordshire community stroke project). BMJ 305(6867):1460–1465
Abrahamsen B, Eiken P, Brixen K (2009) Atrial fibrillation in fracture patients treated with oral bisphosphonates. J Intern Med 265(5):581–592
Suissa S (2008) Immeasurable time bias in observational studies of drug effects on mortality. Am J Epidemiol 168(3):329–335
Woolf AD, Akesson K (2003) Preventing fractures in elderly people. BMJ 327(7406):89–95
Poole KE, Loveridge N, Rose CM, Warburton EA, Reeve J (2007) A single infusion of zoledronate prevents bone loss after stroke. Stroke 38(5):1519–1525
Frank L (2000) Epidemiology. When an entire country is a cohort. Science 287(5462):2398–2399
Sørensen HT (1997) Regional administrative health registers as a resource in clinical epidemiology. A study of options, strengths, limitations and data quality provided with examples of use. Int J Risk Saf Med 10:1–22
Rothman KJ, Greenland S (1998) Modern epidemiology, 2nd edn. Lippincott Williams & Wilkins, Philadelphia
Gaist D, Sørensen HT, Hallas J (1997) The Danish prescription registries. Dan Med Bull 44(4):445–448
Ray WA (2003) Evaluating medication effects outside of clinical trials: new-user designs. Am J Epidemiol 158(9):915–920
Sørensen HT, Lash TL, Rothman KJ (2006) Beyond randomized controlled trials: a critical comparison of trials with nonrandomized studies. Hepatology 44(5):1075–1082
Concato J, Shah N, Horwitz RI (2000) Randomized, controlled trials, observational studies, and the hierarchy of research designs. N Engl J Med 342(25):1887–1892
Johnsen SP, Overvad K, Sørensen HT, Tjønneland A, Husted SE (2002) Predictive value of stroke and transient ischemic attack discharge diagnoses in the Danish National Registry of Patients. J Clin Epidemiol 55(6):602–607
Krarup LH, Boysen G, Janjua H, Prescott E, Truelsen T (2007) Validity of stroke diagnoses in a national register of patients. Neuroepidemiology 28(3):150–154
Law MR, Hackshaw AK (1997) A meta-analysis of cigarette smoking, bone mineral density and risk of hip fracture: recognition of a major effect. BMJ 315(7112):841–846
Lawes CM, Bennett DA, Feigin VL, Rodgers A (2004) Blood pressure and stroke: an overview of published reviews. Stroke 35(3):776–785
Shinton R, Beevers G (1989) Meta-analysis of relation between cigarette smoking and stroke. BMJ 298(6676):789–794
Tanko LB, Christiansen C, Cox DA, Geiger MJ, McNabb MA, Cummings SR (2005) Relationship between osteoporosis and cardiovascular disease in postmenopausal women. J Bone Miner Res 20(11):1912–1920
Rexrode KM, Hennekens CH, Willett WC et al (1997) A prospective study of body mass index, weight change, and risk of stroke in women. JAMA 277(19):1539–1545
Burger H, de Laet CE, van Daele PL et al (1998) Risk factors for increased bone loss in an elderly population: the Rotterdam study. Am J Epidemiol 147(9):871–879
Fiore CE, Pennisi P, Pulvirenti I, Francucci CM (2009) Bisphosphonates and atherosclerosis. J Endocrinol Investig 32(4 Suppl):38–43
Nordström A, Eriksson M, Stegmayr B, Gustafson Y, Nordström P (2010) Low bone mineral density is an independent risk factor for stroke and death. Cerebrovasc Dis 29(2):130–136
Acknowledgments
This study was funded by the Danish Medical Research Council (grant 271-05-0511) and the Clinical Epidemiological Research Foundation, Denmark.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
ICD and ATC codes
Hospital Diagnoses (ICD-8 and ICD-10 codes)
Cardiovascular diseases
-
ICD-8: 393–398 (Chronic rheumatic heart disease, valve disorders), 410–414 (Ischemic heart disease), 427.09, 427.10, 427.19 (Heart failure)
-
ICD-10: I05–I09 (Chronic rheumatic heart disease, valve disorders), I20–I25 (Ischemic heart diseases), I50 (Heart failure)
Atrial fibrillation/flutter
-
ICD-8: 427.93, 427.94
-
ICD-10: I48.9
Renal failure
-
ICD-8: 581–584
-
ICD-10: N17–N19
Diabetes
-
ICD-8: 249.01–249.09, 250.00
-
ICD-10: E10, E11
Pulmonary diseases
-
ICD-8: 073, 471, 490–492, 480–486
-
ICD-10: A481, A709, J12–J18, J40–J44
Cancer
-
ICD-8: 140–149, 150, 151, 152, 153, 154, 155–159, 160, 161, 163, 162, 170–173, 174, 180–184, 185–187, 188–189, 190–194, 195–199, 200–207, 275.59
-
ICD-10: C00–C26, C30–C34, C37–C39, C40–C41, C43–C58, C60–C85, C88, C90–C96
Osteoporosis
-
ICD-8: 723.09
-
ICD-10: M80–M82
Hip or wrist fractures
-
ICD-8: 813.21, 820–821
-
ICD-10: S52.5, S52.6, S72.0, S72.1, S72.2
Liver disease
-
ICD-8: 577.10, 571.11, 571.19, 571.90, 571.92, 571.93, 571.99
-
ICD-10: A48.1, A70.9, B18, I85, J12–J18, K70.0, K70.3, K71.7, K73, K74, K74.3, K74.4, K74.5, K74.6, K76.0
Obesity
-
ICD-8: 277
-
ICD-10: E65–E68
Alcoholism
-
ICD-8: 291, 303, 571.09, 571.10, 577.10
-
ICD-10: F10 (except F10.0), G31.2, G62.1, G72.1, I42.6, K29.2, K86.0, Z72.1
-
AND/OR
-
Previous prescriptions of disulfiram (ATC: N07BB01)
Drug Use (ATC codes)
Cardiovascular drugs
-
ACE-inhibitors C09
-
Beta-blockers C07
-
Low-dose aspirin N02BA01
-
Statins B04AB01, C10AA
-
Calcium antagonists C08D
-
Diuretics C03
-
Nitrates C01D, C01DA
-
Antihypertensives C02
Postmenopausal hormone replacement therapy
-
G03C, G03F
Respiratory drugs
-
R03
Oral glucocorticoids
-
H02AB04, H02AB06
Antidiabetics
-
A10A, A10B
Rights and permissions
About this article
Cite this article
Christensen, S., Mehnert, F., Chapurlat, R.D. et al. Oral bisphosphonates and risk of ischemic stroke: a case–control study. Osteoporos Int 22, 1773–1779 (2011). https://doi.org/10.1007/s00198-010-1395-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-010-1395-y