Abstract
Summary
Cutaneous adverse reactions are reported for many treatments including antiosteoporotic agents. This position paper includes an algorithm for their recognition. With early recognition and proper management, including immediate and permanent withdrawal of the culprit agent, accompanied by hospitalization, rehydration, and systemic corticosteroids, if necessary, the prognosis is good.
Introduction
Cutaneous adverse reactions are reported for many therapeutic agents and observed in between 0% and 8% of treated patients depending on the drug. The antiosteoporotic agents are reputed to be safe in terms of cutaneous effects; however, there have been a number of case reports of cutaneous adverse reactions, which merit consideration. This was the subject of a Working Group meeting of the European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis in April 2009, to focus on the impact of cutaneous adverse reactions and drug-induced hypersensitivity in the management of postmenopausal osteoporosis. We prepared this position paper following these discussions, and include an algorithm for their recognition.
Methods
We reviewed cutaneous adverse reactions observed with antiosteoporotic agents, including information from case reports, regulatory documents, and pharmacovigilance.
Results
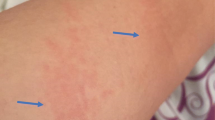
The cutaneous adverse reactions range from benign reactions including exanthematous or maculopapular eruption (drug rash), photosensitivity, and urticaria to the severe and potentially life-threatening reactions, angioedema, drug rash with eosinophilia and systemic symptoms (DRESS), Stevens Johnson syndrome (SJS), and toxic epidermal necrolysis (TEN). Review of available evidence shows that cutaneous adverse reactions occur with all commonly used antiosteoporotic agents. Notably, there are reports of SJS and TEN for bisphosphonates, and of DRESS and TEN for strontium ranelate. These severe reactions remain very rare (<1 in 10,000 cases).
Conclusion
With early recognition and proper management, including immediate and permanent withdrawal of the culprit agent, accompanied by hospitalization and rehydration and systemic corticosteroids if necessary, the prognosis is good.


Similar content being viewed by others
References
Edwards IR, Aronson JK (2000) Adverse drug reactions: definitions, diagnosis, and management. Lancet 356:1255–59
Hunziker T, Kunzi UP, Braunschweig S, Zehnder D, Hoigne R (1997) Comprehensive hospital drug monitoring (CHDM): adverse skin reactions, a 20-year survey. Allergy 52:388–93
Bigby M (2001) Rates of cutaneous reactions to drugs. Arch Dermatol 137:765–70
US Food and Drugs Administration (2009) Pharmapendium
Gomes ER, Demoly P (2005) Epidemiology of hypersensitivity drug reactions. Curr Opin Allergy Clin Immunol 5:309–16
Hung SI, Chung WH, Liou LB, Chu CC, Lin M, Huang HP, Lin YL, Lan JL, Yang LC, Hong HS, Chen MJ, Lai PC, Wu MS, Chu CY, Wang KH, Chen CH, Fann CS, Wu JY, Chen YT (2005) HLA-B*5801 allele as a genetic marker for severe cutaneous adverse reactions caused by allopurinol. Proc Natl Acad Sci U S A 102:4134–39
Chung WH, Hung SI, Hong HS, Hsih MS, Yang LC, Ho HC, Wu JY, Chen YT (2004) Medical genetics: a marker for Stevens Johnson syndrome. Nature 428:486
Mallal S, Phillips E, Carosi G, Molina JM, Workman C, Tomazic J, Jagel-Guedes E, Rugina S, Kozyrev O, Cid JF, Hay P, Nolan D, Hughes S, Hughes A, Ryan S, Fitch N, Thorborn D, Benbow A (2008) HLA-B*5701 screening for hypersensitivity to abacavir. N Engl J Med 358:568–79
Mockenhaupt M (2007) Epidemiology and causes of severe cutaneous adverse reactions to drugs, pp 18–31
Eshki M, Allanore L, Musette P, Milpied B, Grange A, Guillaume JC, Chosidow O, Guillot I, Paradis V, Joly P, Crickx B, Ranger-Rogez S, Descamps V (2009) Twelve-year analysis of severe cases of drug reaction with eosinophilia and systemic symptoms: a cause of unpredictable multiorgan failure. Arch Dermatol 145:67–72
Roujeau JC (2005) Clinical heterogeneity of drug hypersensitivity. Toxicology 209:123–29
Svensson CK, Cowen EW, Gaspari AA (2001) Cutaneous drug reactions. Pharmacol Rev 53:357–79
Aberer W, Kranke B (2008) Clinical manifestations and mechanisms of skin reactions after systemic drug administration. Drug Discovery Today 5:e237–e247
Valeyrie-Allanore L, Sassolas B, Roujeau JC (2007) Drug-induced skin, nail and hair disorders. Drug Saf 30:1011–30
Morison WL (2004) Clinical practice. Photosensitivity. N Engl J Med 350:1111–17
Wolf R, Orion E, Marcos B, Matz H (2005) Life-threatening acute adverse cutaneous drug reactions. Clin Dermatol 23:171–81
Bocquet H, Bagot M, Roujeau JC (1996) Drug-induced pseudolymphoma and drug hypersensitivity syndrome (drug rash with eosinophilia and systemic symptoms: DRESS). Semin Cutan Med Surg 15:250–257
Shiohara T, Takahashi R, Kano Y (2007) Drug-induced hypersensitivity syndrome and viral reactivation, pp. 251-266
Borchers AT, Lee JL, Naguwa SM, Cheema GS, Gershwin ME (2008) Stevens-Johnson syndrome and toxic epidermal necrolysis. Autoimmun Rev 7:598–605
Mockenhaupt M, Viboud C, Dunant A, Naldi L, Halevy S, Bouwes Bavinck JN, Sidoroff A, Schneck J, Roujeau JC, Flahault A (2008) Stevens-Johnson syndrome and toxic epidermal necrolysis: assessment of medication risks with emphasis on recently marketed drugs. The EuroSCAR-study. J Invest Dermatol 128:35–44
Ghislain PD, Roujeau JC (2002) Treatment of severe drug reactions: Stevens-Johnson syndrome, toxic epidermal necrolysis and hypersensitivity syndrome. Dermatol Online J 8:5
Allanore L, Roujeau JC (2007) Clinic and pathogenesis of severe bullous skin reactions: Stevens-Johnson Syndrome, Toxic Epidermal Necrolysis, pp. 267–277
Shiohara T, Inaoka M, Kano Y (2006) Drug-induced hypersensitivity syndrome (DIHS): a reaction induced by a complex interplay among herpesviruses and antiviral and antidrug immune responses. Allergol Int 55:1–8
Viard I, Wehrli P, Bullani R, Schneider P, Holler N, Salomon D, Hunziker T, Saurat JH, Tschopp J, French LE (1998) Inhibition of toxic epidermal necrolysis by blockade of CD95 with human intravenous immunoglobulin. Science 282:490–493
Faye O, Roujeau JC (2005) Treatment of epidermal necrolysis with high-dose intravenous immunoglobulins (IV Ig): clinical experience to date. Drugs 65:2085–90
European Medicines Agency (2008) Alendronate. Summary of product characteristics
Kimura M, Kawada A, Murayama Y, Murayama M (2003) Drug eruption due to alendronate sodium hydrate. Contact Dermatitis 48:116
Kontoleon P, Ilias I, Stavropoulos PG, Papapetrou PD (2000) Urticaria after administration of alendronate. Acta Derm Venereol 80:398
Biswas PN, Wilton LV, Shakir SA (2003) Pharmacovigilance study of alendronate in England. Osteoporos Int 14:507–14
High WA, Cohen JB, Wetherington W, Cockerell CJ (2003) Superficial gyrate erythema as a cutaneous reaction to alendronate for osteoporosis. J Am Acad Dermatol 48:945–46
Brinkmeier T, Kugler K, Lepoittevin JP, Frosch PJ (2007) Adverse cutaneous drug reaction to alendronate. Contact Dermatitis 57:123–25
Lazarov A, Moss K, Plosk N, Cordoba M, Baitelman L (2002) Alendronate-induced lichen planus. Isr Med Assoc J 4:389–90
US Food and Drugs Administration (2002) Risedronate. Description
(2009) Vidal 2009. Le Dictionnaire, 85th ed
Barrera BA, Wilton L, Harris S, Shakir SA (2005) Prescription-event monitoring study on 13, 164 patients prescribed risedronate in primary care in England. Osteoporos Int 16:1989–98
Belhadjali H, Slim R, Aouam K, Youssef M, Zili J (2008) Cutaneous vasculitis induced by risedronate. Allergy 63:1405
European Medicines Agency (2007) Ibandronate. Summary of product characteristics
European Medicines Agency (2008) Zoledronic acid. Summary of product characteristics
Rizos EC, Milionis HJ, Elisaf MS (2006) Fever with rash following zolendronic acid administration. Clin Exp Rheumatol 24:455
European Medicines Agency (2008) Strontium ranelate. Summary of product characteristics
Groves C (2008) Interstitial granulomatous reaction to strontium ranelate. Arch Dermatol 144:268–69
Boada A, Carrascosa J, Leal L, Ferrandiz C (2009) Generalized cutaneous drug eruption due to strontium ranelate. J Eur Acad Dermatol Venereol 0 (in press)
Pernicova I, Middleton ET, Aye M (2008) Rash, strontium ranelate and DRESS syndrome put into perspective. European Medicine Agency on the alert. Osteoporos Int 19:1811–12
Jonville-Bera AP, Crickx B, Aaron L, Hartingh I, utret-Leca E (2009) Strontium ranelate-induced DRESS syndrome: first two case reports. Allergy
Lee HY, Lie D, Lim KS, Thirumoorthy T, Pang SM (2009) Strontium ranelate-induced toxic epidermal necrolysis in a patient with post-menopausal osteoporosis. Osteoporos Int 20:161–62
Grosso A, Douglas I, Hingorani A, MacAllister R, Smeeth L (2008) Post-marketing assessment of the safety of strontium ranelate; a novel case-only approach to the early detection of adverse drug reactions. Br J Clin Pharmacol 66:689–94
European Medicines Agency (2008) Raloxifene. Summary of product characteristics
Layton D, Clarke A, Wilton LV, Shakir SA (2005) Safety profile of raloxifene as used in general practice in England: results of a prescription-event monitoring study. Osteoporos Int 16:490–500
European Medicines Agency (2008) Teriparatide. Summary of product characteristics
European Medicines Agency (2007) Parathyroid hormone. Summary of product characteristics
Burnett-Bowie SA (2008) Is twice-yearly denosumab beneficial in postmenopausal women with osteopenia but no history of fracture? Nat Clin Pract Endocrinol Metab 4:660–661
McClung MR, Lewiecki EM, Cohen SB, Bolognese MA, Woodson GC, Moffett AH, Peacock M, Miller PD, Lederman SN, Chesnut CH, Lain D, Kivitz AJ, Holloway DL, Zhang C, Peterson MC, Bekker PJ (2006) Denosumab in postmenopausal women with low bone mineral density. N Engl J Med 354:821–31
Center JR, Nguyen TV, Schneider D, Sambrook PN, Eisman JA (1999) Mortality after all major types of osteoporotic fracture in men and women: an observational study. Lancet 353:878–82
Bliuc D, Nguyen ND, Milch VE, Nguyen TV, Eisman JA, Center JR (2009) Mortality risk associated with low-trauma osteoporotic fracture and subsequent fracture in men and women. JAMA 301:513–21
Schnyder B, Pichler WJ (2009) Mechanisms of drug-induced allergy. Mayo Clin Proc 84:268–72
Conflicts of interest
Professor P. Musette is a consultant/advisor for Servier.
Professor M-L Brandi has no conflict of interest for this manuscript.
Professor P. Cacoub has disclosed that he has been the recipient of research grants from Schering Plough, Roche, Servier, and Gilead; that he has received honoraria from Roche, Servier, Bristol Myers Squibb, Sanofi Aventis, Gilead, and Schering Plough; and that he is a consultant/advisor to Roche, Servier, Bristol Myers Squibb, Sanofi Aventis, and Gilead Schering Plough.
Doctor J-M Kaufman has no conflict of interest.
Doctor R. Rizzoli has disclosed that he is a consultant/advisor to Merck, Roche, Servier, Danone, Nycomed, Eli Lilly, and Amgen; and that he is on the Speakers' Bureau for Roche, Novartis, Servier, and Amgen.
Professor J-Y Reginster has disclosed that he has been the recipient of research grants from Bristol Myers Squibb, Merck Sharp and Dohme, Rottapharm, Teva, Lilly, Novartis, Roche, GlaxoSmithKline, Amgen, and Servier; that he is a consultant/advisor to Servier, Novartis, Negma, Lilly, Wyeth, Amgen, GlaxoSmithKline, Roche, Merckle, Nycomed, NPS, Theramex, and UCB; and that he has been the recipient of lecture fees for speaking at meetings on behalf of Merck Sharp and Dohme, Lilly, Rottapharm, IBSA, Genevrier, Novartis, Servier, Roche, GlaxoSmithKline, Teijin, Teva, Ebewee Pharma, Zodiac, Analis, Theramex, Nycomed, and NovoNordisk.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Musette, P., Brandi, M.L., Cacoub, P. et al. Treatment of osteoporosis: recognizing and managing cutaneous adverse reactions and drug-induced hypersensitivity. Osteoporos Int 21, 723–732 (2010). https://doi.org/10.1007/s00198-009-1097-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-009-1097-5