Abstract
Introduction and hypothesis
Bladder outlet obstruction (BOO) is a common occurrence after midurethral sling (MUS) insertion and can result in acute or chronic urinary retention or de novo lower urinary tract symptoms (LUTS). However, the management of BOO after MUS is not standardised. The objective of this study was to compare two therapeutic strategies for suspected BOO after MUS.
Methods
Patients who had surgical revision for voiding dysfunction with a post-void residual (PVR) ≥100 ml after MUS in five centres between 2005 and 2020 were included in a retrospective study. Patients were divided into two groups: early sling loosening (EL) vs delayed section/excision of the sling (DS).
Results
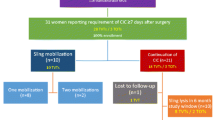
Seventy patients were included: 38 in the EL group and 32 in the DS group. The postoperative complication rate was comparable in both groups (10.5% vs 12.5%; p = 0.99). At 3 months, the rate of withdrawal from self-catheterisation was similar in the two groups (92.1% vs 100%; p = 0.25) as was the PVR (57.5 vs 63.5 ml; p = 0.09). After a median follow-up of 9 months, there were significantly more patients with resolved voiding dysfunction in the EL group (63.2% vs 31.3%; p = 0.01). The rate of persistent/recurrent stress urinary incontinence (SUI) was higher in the DS group (21% vs 43.7%; p = 0.04). In multivariate analysis, the main predictive factor of recurrent SUI was DS (OR 2.87, 95% CI 1.01–8.60, p = 0.048).
Conclusions
Early loosening of MUS in the case of postoperative voiding dysfunction offers better efficacy than DS of the sling, with a lower risk of recurrent/persistent SUI.

Similar content being viewed by others
Abbreviations
- BOO:
-
Bladder outlet obstruction
- CIC:
-
Clean intermittent catheterisation
- DS:
-
Delayed section/partial section
- EL:
-
Early loosening
- LUTS:
-
Lower urinary tract symptoms
- MUS:
-
Midurethral sling
- PVR:
-
Post-void residual
- Qmax:
-
Maximum urinary flow rate
- SUI:
-
Stress urinary incontinence
References
Aoki Y, Brown HW, Brubaker L, Cornu JN, Daly JO, Cartwright R. Urinary incontinence in women. Nat Rev Dis Primer. 2017;3:17042.
Kuhlmann-Capek MJ, Kilic GS, Shah AB, Diken ZM, Snyder RR, Phelps JY. Enmeshed in controversy: use of vaginal mesh in the current medicolegal environment. Female Pelvic Med Reconstr Surg. 2015;21(5):241–3.
Haylen BT, Lee JKS, Sivagnanam V, Cross A. What if there were no tapes? Neurourol Urodyn. 2018;37(6):2026–34.
Hermieu N, Hermieu J-F, Schoentgen N, et al. Évolution des pratiques après l’arrêté encadrant les bandelettes sous-urétrales : résultats d’une enquête nationale. Prog Urol. 2021. https://doi.org/10.1016/j.purol.2021.03.003.
Ngo YG, Huang K-H, Kung F-T, et al. The effects of “unilateral midurethral sling cut down” in women with voiding dysfunctions after anti-incontinence surgery. Int Urol Nephrol. 2019;51(9):1501–6.
Moksnes LR, Svenningsen R, Schiøtz HA, Moe K, Staff AC, Kulseng-Hanssen S. Sling mobilization in the management of urinary retention after mid-urethral sling surgery. Neurourol Urodyn. 2017;36(4):1091–6.
Fritel X, Campagne-Loiseau S, Cosson M, et al. Complications after pelvic floor repair surgery (with and without mesh): short-term incidence after 1873 inclusions in the French VIGI-MESH registry. BJOG. 2020;127(1):88–97.
Nguyen JK, Glowacki CA, Bhatia NN. Survey of voiding dysfunction and urinary retention after anti-incontinence procedures. Obstet Gynecol. 2001;98(6):1011–7.
Brennand EA, Tang S, Birch C, Robert M, Kim-Fine S. Early voiding dysfunction after midurethral sling surgery: comparison of two management approaches. Int Urogynecol J. 2017;28(10):1515–26.
Petros P. A constricted midurethral sling needs loosening within 48–72 hours. Int Urogynecol J. 2018;29(4):609–10.
Bazi T, Kerkhof MH, Takahashi SI, Abdel-Fattah M, IUGA Research and Development Committee. Management of post-midurethral sling voiding dysfunction. International Urogynecological Association research and development committee opinion. Int Urogynecol J. 2018;29(1):23–28.
Rautenberg O, Kociszewski J, Welter J, Kuszka A, Eberhard J, Viereck V. Ultrasound and early tape mobilization–a practical solution for treating postoperative voiding dysfunction. Neurourol Urodyn. 2014;33(7):1147–51.
Glavind K, Shim S. Incidence and treatment of postoperative voiding dysfunction after the tension-free vaginal tape procedure. Int Urogynecol J. 2015;26(11):1657–60.
Abraham N, Makovey I, King A, Goldman HB, Vasavada S. The effect of time to release of an obstructing synthetic mid-urethral sling on repeat surgery for stress urinary incontinence. Neurourol Urodyn. 2017;36(2):349–53.
Bailey C, Matharu G. Conservative management as an initial approach for post-operative voiding dysfunction. Eur J Obstet Gynecol Reprod Biol. 2012;160(1):106–9.
Dindo D, Demartines N, Clavien P-A. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240(2):205–13.
Elbadawi A, Yalla SV, Resnick NM. Structural basis of geriatric voiding dysfunction. IV. Bladder outlet obstruction. J Urol. 1993;150(5 Pt 2):1681–95.
Brading AF. A myogenic basis for the overactive bladder. Urology. 1997;50(6A Suppl):57–67; discussion 68–73. https://doi.org/10.1016/s0090-4295(97)00591-8
Thomas AW, Cannon A, Bartlett E, Ellis-Jones J, Abrams P. The natural history of lower urinary tract dysfunction in men: minimum 10-year urodynamic follow-up of untreated bladder outlet obstruction. BJU Int. 2005;96(9):1301–6.
Guven A, Onal B, Kalorin C, et al. Long term partial bladder outlet obstruction induced contractile dysfunction in male rabbits: a role for Rho-kinase. Neurourol Urodyn. 2007;26(7):1043–9.
Shaw J, Wohlrab K, Rardin C. Recurrence of stress urinary incontinence after midurethral sling revision: a retrospective cohort study. Female Pelvic Med Reconstr Surg. 2017;23(3):184–7.
Mishra VC, Mishra N, Karim OMA, Motiwala HG. Voiding dysfunction after tension-free vaginal tape: a conservative approach is often successful. Int Urogynecol J Pelvic Floor Dysfunct. 2005;16(3):210–4.
Paick J-S, Ku JH, Shin JW, Oh S-J, Kim SW. Complications associated with the tension-free vaginal tape procedure: the Korean experience. Int Urogynecol J Pelvic Floor Dysfunct. 2005;16(3):215–9.
Kim JW, Moon DG, Shin JH, Bae JH, Lee JG, Oh MM. Predictors of voiding dysfunction after mid-urethral sling surgery for stress urinary incontinence. Int Neurourol J. 2012;16(1):30–6.
Neuman M. Post tension-free vaginal tape voiding difficulties: prevention and management. J Pelvic Med Surg. 2004;10(1):19–21.
Author information
Authors and Affiliations
Contributions
Marion Pinsard collected and analysed data and wrote the manuscript; Sonia Guérin and Anis Gasmi helped with data collection; Arnaud Fauconnier, François D’Halluin, Pierre-Louis Broux, Jean-Philippe Harlicot, Vincent Lavoué, Jean Levêque, Andrea Manunta and Krystel Nyangoh Timoh helped to design and conduct the study, and have read and approved the final report; Benoît Peyronnet developed the study concept, made statistics and participated in analysing all the data and writing the article.
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pinsard, M., Fauconnier, A., D’Halluin, F. et al. Comparison of early loosening vs delayed section of mid-urethral slings for postoperative voiding dysfunction. Int Urogynecol J 34, 675–681 (2023). https://doi.org/10.1007/s00192-022-05095-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-022-05095-8