Abstract
Introduction and hypothesis
Our aim was to identify predictors of postoperative voiding trial failure among patients who had a pelvic floor repair without a concurrent incontinence procedure in order to identify low-risk patients in whom postoperative voiding trials may be modified.
Methods
We conducted a retrospective cohort study of women who underwent pelvic floor repair without concurrent incontinence procedures at two institutions from 1 November 2011 through 13 October 2013 after abstracting demographic and clinical data from medical records. The primary outcome was postoperative retrograde voiding trial failure. We used modified Poisson regression to calculate the risk ratio (RR) and 95 % confidence interval (CI).
Results
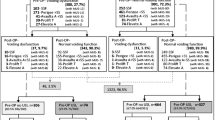
Of the 371 women who met eligibility criteria, 294 (79.2 %) had complete data on the variables of interest. Forty nine (16.7 %) failed the trial, and those women were less likely to be white (p = 0.04), more likely to have had an anterior colporrhaphy (p = 0.001), and more likely to have had a preoperative postvoid residual (PVR) ≥150 ml (p = 0.001). After adjusting for race, women were more likely to fail their voiding trial if they had a preoperative PVR of ≥150 ml (RR: 1.9; 95 % CI: 1.1–3.2); institution also was associated with voiding trial failure (RR: 3.0; 95 % CI: 1.6–5.4).
Conclusions
Among our cohort, postoperative voiding trial failure was associated with a PVR of ≥150 ml and institution at which the surgery was performed.
Similar content being viewed by others
References
Barron K, Savageau J, Young S, Labin L, Morse A (2006) Prediction of successful voiding immediately after outpatient mid-urethral sling. Int Urogynecol J Pelvic Floor Dysfunct 17:570–575
Chung S, Moon Y, Jeon M, Kim S, Bai S (2010) Risk factors associated with voiding dysfunction after anti-incontinence surgery. Int Urogynecol J 21:1505–1509
Wheeler T 2nd, Richter H, Greer W, Bowling C, Redden D, Varner R (2008) Predictors of success with postoperative voiding trials after a mid urethral sling procedure. J Urol 179:600–604
Partoll L (2002) Efficacy of tension-free vaginal tape with other pelvic reconstructive surgery. Am J Obstet Gynecol 186:1292–1295
Chung C, Kuehl T, Spoonts K, Martins D, Larsen W, Yandell P, Shull B (2013) Lack of preoperative predictors of the immediate return of postoperative bladder emptying after uterosacral ligament suspension. South Med J 106:267–9
Hakvoort R, Dijkgraaf M, Burger M, Emanuel M, Roovers J (2009) Predicting short-term urinary retention after vaginal prolapse surgery. Neurourol Urodyn 28:225–228
Park S, Kwon H, Park J, Moon Y, Kim S, Bai S (2011) Predicting risk factors of postoperative voiding dysfunction after abdominal sacrocolpopexy in the treatment of pelvic organ prolapse. Korean J Obstet Gynecol 54:93–98
Tan G, Chan S, Ho CK (2010) Is transurethral catheterization the ideal method of bladder drainage? A survey of patient satisfaction with indwelling transurethral urinary catheters. Asian J Surg 33:31–36
Geller E, Hankins K, Parnell B, Robinson B, Dunivan G (2011) Diagnostic accuracy of retrograde and spontaneous voiding trials for postoperative voiding dysfunction. Obstet Gynecol 118:637–642
Wu J, Vaugh C, Goode P, Redden D, Burgio K, Richter H, Markland A (2014) Prevalence and trends of symptomatic pelvic floor disorders in U.S. women. Obstet Gynecol 123:141–148
Smorgick N, DeLancey J, Patzkowsky K, Advincula A, Song A, As-Sanie S (2012) Risk factors for postoperative urinary retention after laparoscopic and robotic hysterectomy for benign indications. J Obstet Gynecol 120:581–586
Ghezzi F, Cromi A, Uccella S, Colombo G, Salvatore S, Tomera S, Bolis P (2007) Immediate Foley removal after laparoscopic and vaginal hysterectomy: determinants of postoperative urinary retention. J Minim Invasive Gynecol 14:706–711
Bodker B, Lose G (2003) Postoperative urinary retention in gynecologic patients. Int Urogynecol J Pelvic Floor Dysfunct 14:94–97
Kafy S, Huang J, Al-Sunaidi M, Wiener D, Tulandi T (2006) Audit of morbidity and mortality rates of 1792 hysterectomies. J Minim Invasive Gynecol 13:55–59
Zou G (2004) A modified poisson regression approach to prospective studies with binary data. Am J Epidemiol 159:702–706
Harris P, Taylor R, Thielke R, Payne J, Gonzalez N, Conde J (2009) Research electronic data capture (REDCap) - A metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42:377–381
Geller E (2014) Prevention and management of postoperative urinary retention after urogynecologic surgery. Int J Womens Health 6:829–838
Book N, Novi B, Novi J, Pulvino J (2012) Postoperative voiding dysfunction following posterior colporrhaphy. Female Pelvic Med Reconstr Surg 18:32–34
Duckett J, Patil A, Papanikolaou N (2008) Predicting early voiding dysfunction after tension-free vaginal tape. J Obstet Gynecol 28:89–92
Wang K, Wang K, Neimark M, Davila G (2002) Voiding dysfunction following TVT procedure. Int Urogynecol J Pelvic Floor Dysfunct 13:353–357
Kim J, du Moon G, Shin J, Bae J, Lee J, Oh M (2012) Predictors of voiding dysfunction after mid-urethral sling surgery for stress urinary incontinence. Int Neurourol J 16:30–36
Stromberg B, Reines D, Ackerly J (1991) Transderm scopolamine for the control of perioperative nausea. Am Surg 57:712–715
Turner L, Kantartzis K, Shepherd J (2014) Predictors of postoperative acute urinary retention in women undergoing minimally invasive sacral colpopexy. Female Pelvic Med Reconstr Surg 21:39–42
Zhang L, Zhu L, Xu T, Liang S, Lang J (2015) Postoperative voiding difficulty and mesh-related complications after Total Prolift System surgical repair for pelvic organ prolapse and predisposing factors. Menopause 22:885–92
Acknowledgments
We would like to thank Dr. Eman Elkadry for helpful comments on this manuscript. This work was conducted with support from Harvard Catalyst | The Harvard Clinical and Translational Science Center (National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health Award UL1 TR001102), and financial contributions from Harvard University and its affiliated academic healthcare centers.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Rui Wang and Sara Won contributed equally to this work.
Rights and permissions
About this article
Cite this article
Wang, R., Won, S., Haviland, M.J. et al. Voiding trial outcome following pelvic floor repair without incontinence procedures. Int Urogynecol J 27, 1215–1220 (2016). https://doi.org/10.1007/s00192-016-2975-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-016-2975-y