Abstract
Introduction and hypothesis
The interest of uterus-preserving surgery has been growing. Based on a nationwide database, we examined surgical procedures for uterine prolapse in Taiwan during the study period of 1997–2007, a total of 11 years.
Methods
The operations, either uterine suspension or hysterectomy, due to the diagnosis of uterine prolapse were indentified into the study. Data on several parameters were collected for analysis, i.e., the surgical type, patient factors (age and concomitant anti-incontinence surgery), surgeon factors (age and gender), and hospital factors (accreditation level and ownership). Data of this study were obtained from the inpatient expenditures by admission files of the National Health Insurance Research Database (NHIRD). The NHIRD was established by the National Health Research Institute with the aim of promoting research into current and emerging medical issues in Taiwan.
Results
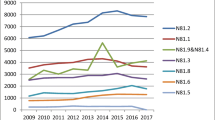
In total, 31,038 operations were identified for this study. There was a trend for increased use of uterine suspension with uterine preservation during the latter years, evidenced by joinpoint regression analyses. More women who were younger (<50 years) or had concomitant anti-incontinence surgery received uterine suspension. Younger surgeons (<50 years) and male surgeons tended to perform more uterine suspensions. As for hospital accreditation, more uterine suspension surgeries were performed in regional hospitals, followed by local hospitals and medical centers. As for hospital ownership, more uterine suspension surgeries were performed in private hospitals, followed by not-for-profit and government-owned hospitals.
Conclusions
There has been a considerable change in the surgical approach for uterine prolapse in Taiwan over the past 11 years. Patient age and concomitant anti-incontinence surgery, surgeon age and gender, and hospital accreditation and ownership may correlate with the choice of surgery for women with uterine prolapse.




Similar content being viewed by others
References
Hendrix SL, Clark A, Nygaard I, Aragaki A, Barnabei V, McTiernan A (2002) Pelvic organ prolapse in the Women’s Health Initiative: gravity and gravidity. Am J Obstet Gynecol 186:1160–1166
Swift SE, Tate SB, Nicholas J (2003) Correlation of symptoms with degree of pelvic organ support in a general population of women: what is pelvic organ prolapse? Am J Obstet Gynecol 189:372–377, discussion 377–379
Samuelsson EC, Victor FT, Tibblin G, Svardsudd KF (1999) Signs of genital prolapse in a Swedish population of women 20 to 59 years of age and possible related factors. Am J Obstet Gynecol 180:299–305
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89:501–506
Zucchi A, Lazzeri M, Porena M, Mearini L, Costantini E (2010) Uterus preservation in pelvic organ prolapse surgery. Nat Rev Urol 7:626–633
Barranger E, Fritel X, Pigne A (2003) Abdominal sacrohysteropexy in young women with uterovaginal prolapse: long-term follow-up. Am J Obstet Gynecol 189:1245–1250
Diwan A, Rardin CR, Strohsnitter WC, Weld A, Rosenblatt P, Kohli N (2006) Laparoscopic uterosacral ligament uterine suspension compared with vaginal hysterectomy with vaginal vault suspension for uterovaginal prolapse. Int Urogynecol J Pelvic Floor Dysfunct 17:79–83
Dietz V, Huisman M, de Jong JM, Heintz PM, van der Vaart CH (2008) Functional outcome after sacrospinous hysteropexy for uterine descensus. Int Urogynecol J Pelvic Floor Dysfunct 19:747–752
Diwan A, Rardin CR, Kohli N (2004) Uterine preservation during surgery for uterovaginal prolapse: a review. Int Urogynecol J Pelvic Floor Dysfunct 15:286–292
Feiner B, Jelovsek JE, Maher C (2009) Efficacy and safety of transvaginal mesh kits in the treatment of prolapse of the vaginal apex: a systematic review. BJOG 116:15–24
Mistrangelo E, Mancuso S, Nadalini C, Lijoi D, Costantini S (2007) Rising use of synthetic mesh in transvaginal pelvic reconstructive surgery: a review of the risk of vaginal erosion. J Minim Invasive Gynecol 14:564–569
Wu MP, Huang KH, Long CY, Huang KF, Yu KJ, Tang CH (2008) The distribution of different surgical types for female stress urinary incontinence among patients’ age, surgeons’ specialties and hospital accreditations in Taiwan: a descriptive 10-year nationwide study. Int Urogynecol J Pelvic Floor Dysfunct 19:1639–1646
Kim HJ, Fay MP, Feuer EJ, Midthune DN (2000) Permutation tests for joinpoint regression with applications to cancer rates. Stat Med 19:335–51
Miskry T, Magos A (2004) A national survey of senior trainees surgical experience in hysterectomy and attitudes to the place of vaginal hysterectomy. BJOG 111:877–879
Wu MP, Huang KH, Long CY, Tsai EM, Tang CH (2010) Trends in various types of surgery for hysterectomy and distribution by patient age, surgeon age, and hospital accreditation: 10-year population-based study in Taiwan. J Minim Invasive Gynecol 17:612–619
Babalola EO, Bharucha AE, Melton LJ 3rd, Schleck CD, Zinsmeister AR, Klingele CJ et al (2008) Utilization of surgical procedures for pelvic organ prolapse: a population-based study in Olmsted County, Minnesota, 1965–2002. Int Urogynecol J Pelvic Floor Dysfunct 19:1243–1250
Saini J, Kuczynski E, Gretz HF 3rd, Sills ES (2002) Supracervical hysterectomy versus total abdominal hysterectomy: perceived effects on sexual function. BMC Womens Health 2:1
Miner PB Jr (2004) Economic and personal impact of fecal and urinary incontinence. Gastroenterology 126:S8–S13
Brubaker L, Cundiff GW, Fine P, Nygaard I, Richter HE, Visco AG et al (2006) Abdominal sacrocolpopexy with Burch colposuspension to reduce urinary stress incontinence. N Engl J Med 354:1557–1566
Rogers RG (2006) The vexing problem of hidden incontinence. N Engl J Med 354:1627–1629
Altman D, Granath F, Cnattingius S, Falconer C (2007) Hysterectomy and risk of stress-urinary-incontinence surgery: nationwide cohort study. Lancet 370:1494–1499
Liang CC, Chang YL, Chang SD, Lo TS, Soong YK (2004) Pessary test to predict postoperative urinary incontinence in women undergoing hysterectomy for prolapse. Obstet Gynecol 104:795–800
Maher C, Baessler K, Glazener CM, Adams EJ, Hagen S (2007) Surgical management of pelvic organ prolapse in women. Cochrane Database Syst Rev 3:CD004014
Eckert M, Cuadrado D, Steele S, Brown T, Beekley A, Martin M (2010) The changing face of the general surgeon: national and local trends in resident operative experience. Am J Surg 199:652–656
Goldstone J, Wong V (2006) New training paradigms and program requirements. Semin Vasc Surg 19:168–171
Griffiths JM, Black NA, Pope C, Stanley J, Bowling A, Abel PD (1998) What determines the choice of procedure in stress incontinence surgery? The use of multilevel modeling. Int J Technol Assess Health Care 14:431–445
Hagen S, Stark D, Maher C, Adams E (2006) Conservative management of pelvic organ prolapse in women. Cochrane Database Syst Rev 4:CD003882
Acknowledgments
We are appreciative of the grant support from Chang Gung Memorial Hospital, Kaohsiung Medical Center, CMRPG870821, and Chi Mei Foundation Hospital, CMNCKU9806. We thank Dr. Yu-Tung Huang of Chang Gung University of Science and Technology, for the assistance of statistical analysis for the trend test.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Dr. Tang and Dr. Liang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Wu, MP., Long, CY., Huang, KH. et al. Changing trends of surgical approaches for uterine prolapse: an 11-year population-based nationwide descriptive study. Int Urogynecol J 23, 865–872 (2012). https://doi.org/10.1007/s00192-011-1647-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-011-1647-1