Abstract
Introduction and hypothesis
The purpose of this study is to examine the inter-observer reliability of the pelvic organ prolapse quantification (POP-Q) system in left lateral position.
Methods
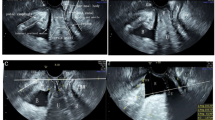
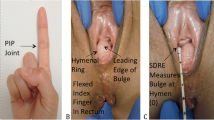
Women attending urogynaecology outpatient clinics were examined in the left lateral position using a digital examination and POP-Q. This was repeated separately by a second blinded clinician. The inter-observer agreement was calculated using the Cohen’s kappa coefficient. The POP-Q examination was then performed with a woman lying in dorsal lithotomy position. The POP-Q findings in the two positions were compared.
Results
Two hundred and eighteen women were recruited. The digital examination had a moderate inter-observer reliability with a kappa value of 0.54. The POP-Q showed a high degree of reliability (0.88). There was a high degree of correlation between the POP-Q findings in left lateral and lithotomy position (rho > 0.95, p < 0.001).
Conclusion
The POP-Q in the left lateral position is reliable, easy to perform, acceptable for patients, and is not a time-consuming examination.
Similar content being viewed by others
References
Swift SE, Pound T, Dias JK (2001) Case-control study of etiologic factors in the development of severe pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct 12(3):187–192
Swift SE (2000) The distribution of pelvic organ support in a population of female subjects seen for routine gynecologic health care. Am J Obstet Gynecol 183(2):277–285
Kapoor DS, Sultan AH, Thakar R, Abulafi MA, Swift RI, Ness W (2008) Management of complex pelvic floor disorders in a multidisciplinary pelvic floor clinic. Colorectal Dis 10(2):118–123
Bump RC, Mattiasson A, Bo K, Brubaker LP, DeLancey JO, Klarskov P et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Silva WA, Kleeman S, Segal J, Pauls R, Woods SE, Karram MM (2004) Effects of a full bladder and patient positioning on pelvic organ prolapse assessment. Obstet Gynecol 104(1):37–41
Barber MD, Lambers A, Visco AG, Bump RC (2000) Effect of patient position on clinical evaluation of pelvic organ prolapse. Obstet Gynecol 96:18–22
Swift SE, Herring M (1998) Comparison of pelvic organ prolapse in the dorsal lithotomy compared with the standing position. Obstet Gynecol 91:961–964
Swift S, Morris S, McKinnie V, Freeman R, Petri E, Scotti RJ, Dwyer P (2006) Validation of a simplified technique for using the POPQ pelvic organ prolapse classification system. Int Urogynecol J Pelvic Floor Dysfunct 17(6):615–620
Poston GJ, Joseph AE, Riddle PR (1983) The accuracy of ultrasound in the measurement of changes in bladder volume. Br J Urol 55:361–363
Digesu GA, Khullar V, Cardozo L, Robinson D (2008) Inter-observer reliability of digital vaginal examination using a four-grade scale in different patient positions. Int Urogynecol J Pelvic Floor Dysfunct 19(9):1303–1307
Altman DG (1999) Practical statistics for medical research. Chapman & Hall/CRC, Boca Raton
Nunnally JC (1978) Psychometric Theory. McGraw Hill, New York
Carmines E, Zeller R (1979) Reliability and validity assessment: quantitative applications in the social science. Sage, Beverley Hills, California
Hall AF, Theofrastous JP, Cundiff GW, Harris RL, Hamilton LF, Swift SE et al (1996) Interobserver and intraobserver reliability of the proposed international continence society, society of gynecologic surgeons, and American urogynecologic society pelvic organ prolapse classification system. Am J Obstet Gynecol 175:1467–1470
Grody MHT (1997) Posterior compartment defects. In: Rock J, Thompson T (eds) Telinde’s operative gynecology, 8th edn. Lippincott-Raven Press, Philadelphia, pp 1044–1056
Walters MD, Karram MM (1992) Enterocele. American urogynecologic society quarterly report. American Urogynecologic Society, Chicago, 10
Auwad W, Freeman RM, Swift S (2004) Is the pelvic organ prolapse quantification system (POPQ) being used? A survey of members of the international continence society (ICS) and the American urogynecologic society (AUGS). Int Urogynecol J Pelvic Floor Dysfunct 15(5):324–327
Conflicts of interest
The authors declare the following for research, consultancy, and/or advisory work. Linda Cardozo: Astellas, Lilly, UCB, Pharma, Pfizer, Gynecare, Plethora, Cook, Organon, and Bioxell; Vik Khullar: Astellas, Lilly, Allergan, Pfizer, Gynecare, Cook, and Bioxell; G.A. Digesu: Astellas and Bioxell; Stavros Athanasiou: Astellas, Pfizer, and Gynecare; Simon Hill: Pfizer, Astellas, Ardana, and UCB Pharma.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Digesu, G.A., Athanasiou, S., Cardozo, L. et al. Validation of the pelvic organ prolapse quantification (POP-Q) system in left lateral position. Int Urogynecol J 20, 979–983 (2009). https://doi.org/10.1007/s00192-009-0884-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-009-0884-z