Abstract
Purpose
A new CR TKA design with concave medial and convex lateral tibial polyethylene bearing components was introduced recently to improve functional outcomes. This study aimed to investigate in-vivo articular contact kinematics in unilateral asymmetrical tibial polyethylene geometry CR TKA patients during strenuous knee flexion activities.
Methods
Fifteen unilateral CR TKA patients (68.4 ± 5.8 years; 6 male/9 female) were evaluated for both knees during sit-to-stand, single-leg deep lunges and step-ups using validated combined computer tomography and dual fluoroscopic imaging system. Medial and lateral condylar contact positions were quantified during weight-bearing flexion activities. The Wilcoxon signed-rank test was performed to determine if there is a significant difference in articular contact kinematics during strenuous flexion activities between CR TKA and the non-operated knees.
Results
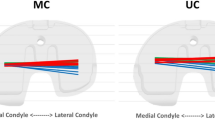
Contact excursions of the lateral condyle in CR TKAs were significantly more anteriorly located than the contralateral non-operated knee during sit-to-stand (3.7 ± 4.8 mm vs − 7.8 ± 4.3 mm) and step-ups (− 1.5 ± 3.2 mm vs − 6.3 ± 5.8 mm). Contact excursions of the lateral condyle in CR TKAs were significantly less laterally located than the contralateral non-operated knee during sit-to-stand (21.4 ± 2.8 mm vs 24.5 ± 4.7 mm) and single-leg deep lunges (22.6 ± 4.4 mm vs 26.2 ± 5.7 mm, p < 0.05). Lateral condyle posterior rollback was not fully restored in CR TKA patients during sit-to-stand (9.8 ± 6.7 mm vs 12.9 ± 8.3 mm) and step-ups (8.1 ± 4.8 mm vs 12.2 ± 6.4 mm). Lateral pivoting patterns were observed in 80%, 73% and 69% of patients during sit-to-stand, step-ups and single-leg deep lunges respectively.
Conclusion
Although lateral femoral rollback and lateral pivoting patterns were observed during strenuous functional daily activities, asymmetric contact kinematics still persisted in unilateral CR TKA patients. This suggests the specific investigated contemporary asymmetrical tibial polyethylene geometry CR TKA design evaluated in this study does not fully replicate healthy knee contact kinematics during strenuous functional daily activities.
Level of evidence
III.








Similar content being viewed by others
Data availablity
Data are available upon request. Only standard software was used for analysis.
References
Arauz P, Klemt C, Limmahakhun S, An S, Kwon Y-M (2018) Stair climbing and high knee flexion activities in bi-cruciate retaining total knee arthroplasty. In vivo kinematics and articular contact analysis. J Arthroplasty 34:570–576
Arauz P, Peng Y, An S, Kwon Y-M (2018) In-vivo analysis of sliding distance and cross-shear in Bi-cruciate retaining total knee arthroplasty. J Biomech 77:8–15
Bingham J, Li G (2006) An optimized image matching method for determining in-vivo TKA kinematics with a dual-orthogonal fluoroscopic imaging system. J Biomech Eng 128:588–595
Bonner BE, Castillo TN, Fitz DW, Zhao JZ, Klemt C, Kwon Y-M (2019) Preoperative opioid use negatively affects patient-reported outcomes after primary total hip arthroplasty. J Am Acad Orthop Surg 27:1016–1020
Cates HE, Komistek RD, Mahfouz MR, Schmidt MA, Anderle M (2008) In vivo comparison of knee kinematics for subjects having either a posterior stabilized or cruciate retaining high-flexion total knee arthroplasty. J Arthroplasty 23:1057–1067
DeFrate LE, Gill TJ, Li G (2004) In vivo function of the posterior cruciate ligament during weightbearing knee flexion. Am J Sports Med 32:1923–1928
Defrate LE, Papannagari R, Gill TJ, Moses JM, Pathare NP, Li G (2006) The 6 degrees of freedom kinematics of the knee after anterior cruciate ligament deficiency: an in vivo imaging analysis. Am J Sports Med 34:1240–1246
Dimitriou D, Tsai T-Y, Park KK, Hosseini A, Kwon Y-M, Rubash HE, Li G (2016) Weight-bearing condyle motion of the knee before and after cruciate-retaining TKA: in-vivo surgical transepicondylar axis and geometric center axis analyses. J Biomech 49:1891–1898
Grieco TF, Sharma A, Dessinger GM, Cates HE, Komistek RD (2018) In vivo kinematic comparison of a bicruciate stabilized total knee arthroplasty and the normal knee using fluoroscopy. J Arthroplasty 33:565–571
Grieco TF, Sharma A, Komistek RD, Cates HE (2016) Single versus multiple-radii cruciate-retaining total knee arthroplasty: an in vivo mobile fluoroscopy study. J Arthroplasty 31:694–701
Horiuchi H, Akizuki S, Tomita T, Sugamoto K, Yamazaki T, Shimizu N (2012) In vivo kinematic analysis of cruciate-retaining total knee arthroplasty during weight-bearing and non-weight-bearing deep knee bending. J Arthroplasty 27:1196–1202
Klemt C, Tirumala V, Oganesyan R, Xiong L, den van Kieboom J, Kwon Y-M (2020) Single-stage revision of the infected total knee arthroplasty is associated with improved functional outcomes: a Propensity Score Matched Cohort Study. J Arthroplasty 20:883–5403
Kozanek M, Hosseini A, Liu F, Van de Velde SK, Gill TJ, Rubash HE, Li G (2009) Tibiofemoral kinematics and condylar motion during the stance phase of gait. J Biomech 42:1877–1884
Li G, Van de Velde SK, Bingham JT (2008) Validation of a non-invasive fluoroscopic imaging technique for the measurement of dynamic knee joint motion. J Biomech 41:1616–1622
Li G, Wuerz TH, DeFrate LE (2004) Feasibility of using orthogonal fluoroscopic images to measure in vivo joint kinematics. J Biomech Eng 126:314–318
Lin H, Wang S, Tsai T-Y, Li G, Kwon Y-M (2013) In-vitro validation of a non-invasive dual fluoroscopic imaging technique for measurement of the hip kinematics. Med Eng Phys 35:411–416
Mendez JH, Mehrani A, Randolph P, Stagg S (2019) Throughput and resolution with a next-generation direct electron detector. IUCrJ 6:1007–1013
Mikashima Y, Tomatsu T, Horikoshi M, Nakatani T, Saito S, Momohara S, Banks SA (2010) In vivo deep-flexion kinematics in patients with posterior-cruciate retaining and anterior-cruciate substituting total knee arthroplasty. Clin Biomech 25:83–87
Most E, Li G, Sultan PG, Park SE, Rubash HE (2005) Kinematic analysis of conventional and high-flexion cruciate-retaining total knee arthroplasties: an in vitro investigation. J Arthroplasty 20:529–535
Nabeyama R, Matsuda S, Miura H, Kawano T, Nagamine R, Mawatari T, Tanaka K, Iwamoto Y (2003) Changes in anteroposterior stability following total knee arthroplasty. J Orthop Sci 8:526–531
Nosrati M, Dey D, Mehrani A, Strassler SE, Zelinskaya N, Hoffer ED, Stagg SM, Dunham CM, Conn GL (2019) Functionally critical residues in the aminoglycoside resistance-associated methyltransferase RmtC play distinct roles in 30S substrate recognition. J Biol Chem 294:17642–17653
Nozaki H, Banks SA, Suguro T, Hodge WA (2002) Observations of femoral rollback in cruciate-retaining knee arthroplasty. Clin Orthop Relat Res 404:308–314
Peng Y, Arauz P, An S, Limmahakhun S, Klemt C, Kwon Y-M (2019) Does component alignment affect patient reported outcomes following bicruciate retaining total knee arthroplasty? An in vivo three-dimensional analysis. J Knee Surg 33:798–803
Peng Y, Arauz P, Desai P, Byers A, Klemt C, Kwon Y-M (2019) In vivo kinematic analysis of patients with robotic-assisted total hip arthroplasty during gait at 1-year follow-up. Int J Med Robot 15:2021–2027
Qi W, Hosseini A, Tsai T-Y, Li J-S, Rubash HE, Li G (2013) In vivo kinematics of the knee during weight bearing high flexion. J Biomech 46:1576–1582
Simmons S, Lephart S, Rubash H, Pifer GW, Barrack R (1996) Proprioception after unicondylar knee arthroplasty versus total knee arthroplasty. Clin Orthop Relat Res 331:179–184
Tsai T-Y, Li J-S, Wang S, Lin H, Malchau H, Li G, Rubash H, Kwon Y-M (2013) A novel dual fluoroscopic imaging method for determination of THA kinematics: in-vitro and in-vivo study. J Biomech 46:1300–1304
Victor J, Banks S, Bellemans J (2005) Kinematics of posterior cruciate ligament-retaining and -substituting total knee arthroplasty: a prospective randomised outcome study. J Bone Joint Surg Br 87:646–655
Yoshiya S, Matsui N, Komistek RD, Dennis DA, Mahfouz M, Kurosaka M (2005) In vivo kinematic comparison of posterior cruciate-retaining and posterior stabilized total knee arthroplasties under passive and weight-bearing conditions. J Arthroplasty 20:777–783
Zambianchi F, Fiacchi F, Lombari V, Venturelli L, Marcovigi A, Giorgini A, Catani F (2018) Changes in total knee arthroplasty design affect in-vivo kinematics in a redesigned total knee system: a fluoroscopy study. Clin Biomech 54:92–102
Funding
The study did not receive any funding.
Author information
Authors and Affiliations
Contributions
CK: data collection, analysis, write-up; JD: data collection, analysis, write-up; VT: data collection, analysis; Y-MK: analysis, write-up.
Corresponding author
Ethics declarations
Conflict of interest
All authors report no conflict of interest or financial disclosures.
Ethical approval
This study was approved by the internal Institutional Review Board at Massachusetts General Hospital/Harvard Medical School (ID: 2013P000821).
Informed consent
All patients provided written consent prior to enrolment into the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Klemt, C., Drago, J., Tirumala, V. et al. Asymmetrical tibial polyethylene geometry-cruciate retaining total knee arthroplasty does not fully restore in-vivo articular contact kinematics during strenuous activities. Knee Surg Sports Traumatol Arthrosc 30, 652–660 (2022). https://doi.org/10.1007/s00167-020-06384-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-06384-9