Abstract
Purpose
Primary repair of the anterior cruciate ligament (ACL) is regaining popularity. Long-term results are lacking. The purpose of the current study was to determine the survival of the primarily repaired ACL after dynamic intraligamentary stabilization.
Methods
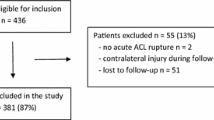
Between 2011 and 2013, 57 patients with acute proximal ACL ruptures underwent DIS repair within 3 weeks from injury and were available for final follow-up at least 5 years postoperatively. Failure as an end point was defined as conversion to ACL reconstruction, failure to restore stability with persisting laxity side-to-side laxity of > 5 mm or a late-traumatic re-rupture or loss of stability. Kaplan–Meier survival analysis was performed.
Results
Kaplan–Meier survival analysis demonstrated an overall survival of 70.0% (standard error SE 6.6%) at 74 months follow-up. Patients performing competitive sports prior to injury demonstrated an inferior long-term ACL survival of 56.4% (SE 11.6%). Patients performing recreational sport activities demonstrated a survival rate of 79.2% (SE 7.7%). The one factor demonstrating a direct influence on failure after adjustment was a high-pre-injury level of physical (odds ratio 4.0 confidence interval 1.0–15.8, p = 0.04).
Conclusion
The minimum 5 years survival rate after primary ACL repair using this technique was 70%. This value dropped to 56% in highly active patients performing competitive sports. Patients not suffering failure of repair demonstrated adequate restoration of knee laxity and high satisfaction. This study not only underlines the potential of ACL repair, but also highlights the danger of the procedure if strict patient selection is not appreciated.
Level of evidence
Level IV.


Similar content being viewed by others
References
Ahmad SS, Difelice GS, van der List JP, Ateschrang A, Hirschmann MT (2019) Primary repair of the anterior cruciate ligament: real innovation or reinvention of the wheel? Knee Surg Sports Traumatol Arthrosc 27:1–2
Ahmad SS, Meyer JC, Krismer AM, Ahmad SS, Evangelopoulos DS, Hoppe S et al (2017) Outcome measures in clinical ACL studies: an analysis of highly cited level I trials. Knee Surg Sports Traumatol Arthrosc 25:1517–1527
Ahmad SS, Schreiner AJ, Hirschmann MT, Schroter S, Dobele S, Ahrend MD et al (2019) Dynamic intraligamentary stabilization for ACL repair: a systematic review. Knee Surg Sports Traumatol Arthrosc 27:13–20
Crawford SN, Waterman MBR, Lubowitz JH (2013) Long-term failure of anterior cruciate ligament reconstruction. Arthroscopy 29:1566–1571
DiFelice GS, van der List JP (2018) Clinical outcomes of arthroscopic primary repair of proximal anterior cruciate ligament tears are maintained at mid-term follow-up. Arthroscopy 34:1085–1093
Feagin JA, Curl WW (1976) Isolated tear of the anterior cruciate ligament: 5-year follow-up study. Am J Sports Med 4:95–100
Hefti E, Müller W, Jakob R, Stäubli H-U (1993) Evaluation of knee ligament injuries with the IKDC form. Knee Surg Sports Traumatol Arthrosc 1:226–234
Henle P, Röder C, Perler G, Heitkemper S, Eggli S (2015) Dynamic Intraligamentary Stabilization (DIS) for treatment of acute anterior cruciate ligament ruptures: case series experience of the first three years. BMC Musculoskelet Disord 16:27
Irrgang JJ, Anderson AF, Boland AL, Harner CD, Kurosaka M, Neyret P et al (2001) Development and validation of the international knee documentation committee subjective knee form. Am J Sports Med 29:600–613
Kohl S, Evangelopoulos DS, Ahmad SS, Kohlhof H, Herrmann G, Bonel H et al (2014) A novel technique, dynamic intraligamentary stabilization creates optimal conditions for primary ACL healing: a preliminary biomechanical study. Knee 21:477–480
Kohl S, Evangelopoulos DS, Schar MO, Bieri K, Muller T, Ahmad SS (2016) Dynamic intraligamentary stabilisation: initial experience with treatment of acute ACL ruptures. Bone Jt J 98-b:793–798
Krismer AM, Gousopoulos L, Kohl S, Ateschrang A, Kohlhof H, Ahmad SS (2017) Factors influencing the success of anterior cruciate ligament repair with dynamic intraligamentary stabilisation. Knee Surg Sports Traumatol Arthrosc 25:3923–3928
Leiter JRS, Gourlay R, McRae S, de Korompay N, MacDonald PB (2014) Long-term follow-up of ACL reconstruction with hamstring autograft. Knee Surg Sports Traumatol Arthrosc 22:1061–1069
Lysholm J, Gillquist J (1982) Evaluation of knee ligament surgery results with special emphasis on use of a scoring scale. Am J Sports Med 10:150–154
Meister M, Koch J, Amsler F, Arnold MP, Hirschmann MT (2018) ACL suturing using dynamic intraligamentary stabilisation showing good clinical outcome but a high reoperation rate: a retrospective independent study. Knee Surg Sports Traumatol Arthrosc 26:655–659
Sherman MF, Lieber L, Bonamo JR, Podesta L, Reiter I (1991) The long-term followup of primary anterior cruciate ligament repair: defining a rationale for augmentation. Am J Sports Med 19:243–255
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res 198:43–49
van der List JP, DiFelice GS (2017) Primary repair of the anterior cruciate ligament: a paradigm shift. Surgeon 15:161–168
Weaver JK, Derkash RS, Freeman JR, Kirk RE, Oden RR, Matyas J (1985) Primary knee ligament repair—revisited. Clin Orthop Relat Res 199:185–191
Funding
No funding was received for the conduction of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
The study was performed according to its approval by the ethical commission of the canton of Bern, Switzerland (KEK-BE 253/2014).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ahmad, S.S., Schürholz, K., Liechti, E.F. et al. Seventy percent long-term survival of the repaired ACL after dynamic intraligamentary stabilization. Knee Surg Sports Traumatol Arthrosc 28, 594–598 (2020). https://doi.org/10.1007/s00167-019-05749-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-019-05749-z