Abstract
Purpose
Aim of this study is to document if combined meniscal allograft transplantation (MAT) and ACL reconstruction can improve knee function, reduce pain and allow patients with meniscal defect and ACL lesion to resume sport activities.
Methods
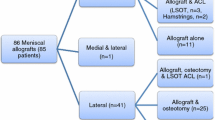
Fifty MAT, arthroscopically performed without bone plugs and combined with one-stage primary or revision ACL reconstruction, with or without high tibial osteotomy (HTO), were included. Patients (aged 38.2 ± 10.6 years, 87% males) were evaluated at a mean follow-up of 5 years with Lysholm, Tegner and VAS scores. Patient satisfaction was also recorded, together with complications and failures.
Results
VAS and Lysholm scores improved significantly (from 63.7 to 24.5 and from 60.6 to 82.7, respectively, p < 0.001), while the Tegner score did not reach pre-injury values (p < 0.001), but it improved significantly compared to pre-surgery values (from 2.8 to 4.6, p < 0.001). Medial MAT reported significantly better results compared to lateral MAT. Patients undergoing concomitant HTO reported a significantly higher decrease of VAS. Younger patients with higher pre-operative pain and lower activity level presented higher satisfaction. Eight patients needed a reoperation. Three patients were considered surgical failures while four were considered clinical failures, for a total of 15% failures.
Conclusions
Meniscal allograft transplantation combined with ACL reconstruction represents a safe and suitable treatment, which should be considered as a suitable option in the clinical practice. All evaluated patient profiles, ACL injury in a patient with post-meniscectomy syndrome, failed ACL reconstruction in patients with a meniscus defect, and ACL reconstruction in patients with malalignment due to meniscal defect, benefited from the combined MAT procedure at medium-term follow-up.
Level of evidence
IV.





Similar content being viewed by others
References
Alentorn-Geli E, Vazquez RS, Diaz PA, Cusco X, Cugat R (2010) Arthroscopic meniscal transplants in soccer players: outcomes at 2- to 5-year follow-up. Clin J Sport Med 20:340–343
Barber-Westin SD, Noyes FR (2018) Low-impact sports activities are feasible after meniscus transplantation: a systematic review. Knee Surg Sports Traumatol Arthrosc 26:1950–1958
Bulgheroni E, Grassi A, Bulgheroni P, Marcheggiani Muccioli GM, Zaffagnini S, Marcacci M (2015) Long-term outcomes of medial CMI implant versus partial medial meniscectomy in patients with concomitant ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 23:3221–3227
Chatain F, Adeleine P, Chambat P, Neyret P (2003) A comparative study of medial versus lateral arthroscopic partial meniscectomy on stable knees: 10-year minimum follow-up. Arthroscopy 19:842–849
Getgood A, LaPrade RF, Verdonk P, Gersoff W, Cole B, Spalding T (2016) International Meniscus Reconstruction Experts Forum (IMREF) 2015 consensus statement on the practice of meniscal allograft transplantation. Am J Sports Med. https://doi.org/10.1177/0363546516660064
Gonzalez-Lucena G, Gelber PE, Pelfort X, Tey M, Monllau JC (2010) Meniscal allograft transplantation without bone blocks: a 5- to 8-year follow-up of 33 patients. Arthroscopy 26:1633–1640
Hamrin Senorski E, Samuelsson K, Thomee C, Beischer S, Karlsson J, Thomee R (2017) Return to knee-strenuous sport after anterior cruciate ligament reconstruction: a report from a rehabilitation outcome registry of patient characteristics. Knee Surg Sports Traumatol Arthrosc 25:1364–1374
Heijink A, Gomoll AH, Madry H, Drobnic M, Filardo G, Espregueira-Mendes J et al (2012) Biomechanical considerations in the pathogenesis of osteoarthritis of the knee. Knee Surg Sports Traumatol Arthrosc 20:423–435
Mahmoud A, Young J, Bullock-Saxton J, Myers P (2018) Meniscal allograft transplantation: the effect of cartilage status on survivorship and clinical outcome. Arthroscopy 34:1871–1876 e1871
Marcacci M, Marcheggiani Muccioli GM, Grassi A, Ricci M, Tsapralis K, Nanni G et al (2014) Arthroscopic meniscus allograft transplantation in male professional soccer players: a 36-month follow-up study. Am J Sports Med 42:382–388
Marcacci M, Zaffagnini S, Bonanzinga T, Marcheggiani Muccioli GM, Bruni D, Iacono F (2012) Over-the-top double-bundle revision ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 20:1404–1408
Marcacci M, Zaffagnini S, Iacono F, Neri MP, Loreti I, Petitto A (1998) Arthroscopic intra- and extra-articular anterior cruciate ligament reconstruction with gracilis and semitendinosus tendons. Knee Surg Sports Traumatol Arthrosc 6:68–75
Marcacci M, Zaffagnini S, Marcheggiani Muccioli GM, Grassi A, Bonanzinga T, Nitri M et al (2012) Meniscal allograft transplantation without bone plugs: a 3-year minimum follow-up study. Am J Sports Med 40:395–403
Masferrer-Pino A, Monllau JC, Ibanez M, Erquicia JI, Pelfort X, Gelber PE (2018) Capsulodesis versus bone trough technique in lateral meniscal allograft transplantation: graft extrusion and functional results. Arthroscopy 34:1879–1888
McCormick F, Harris JD, Abrams GD, Hussey KE, Wilson H, Frank R et al (2014) Survival and reoperation rates after meniscal allograft transplantation: analysis of failures for 172 consecutive transplants at a minimum 2-year follow-up. Am J Sports Med 42:892–897
Musahl V, Rahnemai-Azar AA, Costello J, Arner JW, Fu FH, Hoshino Y et al (2016) The influence of meniscal and anterolateral capsular injury on knee laxity in patients with anterior cruciate ligament injuries. Am J Sports Med 44:3126–3131
Paxton ES, Stock MV, Brophy RH (2011) Meniscal repair versus partial meniscectomy: a systematic review comparing reoperation rates and clinical outcomes. Arthroscopy 27:1275–1288
Roldan E, Reeves ND, Cooper G, Andrews K (2017) In vivo mechanical behaviour of the anterior cruciate ligament: a study of six daily and high impact activities. Gait Posture 58:201–207
Rueff D, Nyland J, Kocabey Y, Chang HC, Caborn DN (2006) Self-reported patient outcomes at a minimum of 5 years after allograft anterior cruciate ligament reconstruction with or without medial meniscus transplantation: an age-, sex-, and activity level-matched comparison in patients aged approximately 50 years. Arthroscopy 22:1053–1062
Saltzman BM, Bajaj S, Salata M, Daley EL, Strauss E, Verma N et al (2012) Prospective long-term evaluation of meniscal allograft transplantation procedure: a minimum of 7-year follow-up. J Knee Surg 25:165–175
Saltzman BM, Meyer MA, Weber AE, Poland SG, Yanke AB, Cole BJ (2017) Prospective clinical and radiographic outcomes after concomitant anterior cruciate ligament reconstruction and meniscal allograft transplantation at a mean 5-year follow-up. Am J Sports Med 45:550–562
Sekiya JK, Giffin JR, Irrgang JJ, Fu FH, Harner CD (2003) Clinical outcomes after combined meniscal allograft transplantation and anterior cruciate ligament reconstruction. Am J Sports Med 31:896–906
Shelbourne KD, Gray T (2000) Results of anterior cruciate ligament reconstruction based on meniscus and articular cartilage status at the time of surgery. Five- to fifteen-year evaluations. Am J Sports Med 28:446–452
Spalding T, Getgood A (2016) Defining outcome after meniscal allograft transplantation: is buying time a valid measure of success? Knee Surg Sports Traumatol Arthrosc 24:1424–1426
Spang JT, Dang AB, Mazzocca A, Rincon L, Obopilwe E, Beynnon B et al (2010) The effect of medial meniscectomy and meniscal allograft transplantation on knee and anterior cruciate ligament biomechanics. Arthroscopy 26:192–201
van Arkel ER, de Boer HH (2002) Survival analysis of human meniscal transplantations. J Bone Jt Surg Br 84:227–231
van de Pol GJ, Arnold MP, Verdonschot N, van Kampen A (2009) Varus alignment leads to increased forces in the anterior cruciate ligament. Am J Sports Med 37:481–487
Verdonk PC, Verstraete KL, Almqvist KF, De Cuyper K, Veys EM, Verbruggen G et al (2006) Meniscal allograft transplantation: long-term clinical results with radiological and magnetic resonance imaging correlations. Knee Surg Sports Traumatol Arthrosc 14:694–706
Waterman BR, Rensing N, Cameron KL, Owens BD, Pallis M (2016) Survivorship of meniscal allograft transplantation in an athletic patient population. Am J Sports Med 44:1237–1242
Wu WH, Hackett T, Richmond JC (2002) Effects of meniscal and articular surface status on knee stability, function, and symptoms after anterior cruciate ligament reconstruction: a long-term prospective study. Am J Sports Med 30:845–850
Zaffagnini S, Bonanzinga T, Grassi A, Marcheggiani Muccioli GM, Musiani C, Raggi F et al (2013) Combined ACL reconstruction and closing-wedge HTO for varus angulated ACL-deficient knees. Knee Surg Sports Traumatol Arthrosc 21:934–941
Zaffagnini S, Grassi A, Marcheggiani Muccioli GM, Benzi A, Roberti di Sarsina T, Signorelli C et al (2016) Is sport activity possible after arthroscopic meniscal allograft transplantation? Midterm results in active patients. Am J Sports Med 44:625–632
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for- profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Stefano Zaffagnini, Alberto Grassi, Iacopo Romandini, Maurilio Marcacci, Giuseppe Filardo declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors. For this type of study formal consent is not required.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Zaffagnini, S., Grassi, A., Romandini, I. et al. Meniscal allograft transplantation combined with anterior cruciate ligament reconstruction provides good mid-term clinical outcome. Knee Surg Sports Traumatol Arthrosc 27, 1914–1923 (2019). https://doi.org/10.1007/s00167-018-5078-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-5078-0