Abstract
Purpose
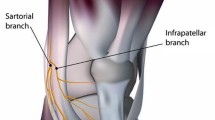
To determine how the incision technique for hamstring tendon (HT) harvest in anterior cruciate ligament (ACL) reconstruction affects the risk of injury to the IPBSN and clinical outcome.
Methods
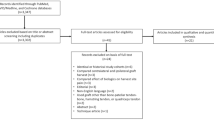
A systematic literature search of the MEDLINE/Pubmed, Cochrane Central Register of Controlled Trials (CENTRAL) and EBSCOhost electronic databases and clinicaltrials.gov for unpublished studies was performed to identify comparative studies investigating injury to the IPBSN after HT ACL reconstruction by comparing at least two different incision techniques. Data were extracted for the number of patients with evidence of any neurologic deficit corresponding to injury to the IPBSN, area of sensory deficit, the Lysholm score and patient satisfaction. The mean difference (MD) in study outcome between incision groups was assessed. The relative risk (RR) and the number needed to treat (NNT) were calculated. The Chi-square and Higgins’ I2 tests were applied to test heterogeneity. Data were pooled using a Mantel–Haenszel random-effects model if the statistical heterogeneity was > 50% and a fixed-effects model if the statistical heterogeneity was < 50%. The risk of bias was evaluated according to the Cochrane Database questionnaire and the quality of evidence was graded according to the Grading of Recommendations Assessment, Development and Evaluation (GRADE) guidelines.
Results
A total of eight studies (three randomized controlled trials (RCTs) and five comparative studies) were included, of which six compared vertical and oblique incisions, one horizontal and vertical incisions, and one compared all three techniques. HT harvest was performed through a vertical incision in 329 patients, through an oblique incision in 195 patients and through a horizontal incision in 151 patients. Considering the meta-analysis of the RCTs, the performance of a vertical incision significantly increased the risk of causing IPBSN deficiency compared with both oblique and horizontal incision [RR 1.65 (CI 1.10–2.49, p = 0.02) and RR 2.45 (CI 1.73–3.47, p < 0.0001), respectively]. A significantly larger area of sensory deficit was found with vertical incisions compared with oblique ones, with an MD of 22.91 cm2 (95% CI 7.73–38.08; p = 0.04). No significant differences were found between the incision techniques in relation to patient-reported outcomes. The same trend was obtained after the performing a meta-analysis of all eight included studies. The quality of evidence in this meta-analysis was determined as “low” to “moderate”, mostly due to inadequate methods of randomization and high heterogeneity among the included studies.
Conclusion
The performance of a vertical incision to harvest HTs for ACL reconstruction significantly increased the risk of iatrogenic injury to the IPBSN compared with both oblique and horizontal incisions.
Level of evidence
Level I–III, meta-analysis of comparative studies.










Similar content being viewed by others
References
Arthornthurasook A, Gaew-Im K (1990) The sartorial nerve: its relationship to the medial aspect of the knee. Am J Sports Med 18:41–42
Balshem H, Helfand M, Schunemann HJ, Oxman AD, Kunz R, Brozek J et al (2011) GRADE guidelines: 3. Rating the quality of evidence. J Clin Epidemiol 64:401–406
Figueroa D, Calvo R, Vaisman A, Campero M, Moraga C (2008) Injury to the infrapatellar branch of the saphenous nerve in ACL reconstruction with the hamstrings technique: clinical and electrophysiological study. Knee 15:360–363
Gianotti SM, Marshall SW, Hume PA, Bunt L (2009) Incidence of anterior cruciate ligament injury and other knee ligament injuries: a national population-based study. J Sci Med Sport 12:622–627
Hedges LV, Vevea JL (1998) Fixed-and random-effects models in meta-analysis. Psychological methods 3:486
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. Bmj 327:557–560
Higgins JPT, Green S (2011) Cochrane handbook for systematic reviews of intervention version 5.1.0. The Cochrane Collaboration. http://handbook.cochrane.org
Hunter LY, Louis DS, Ricciardi JR, O’Connor GA (1979) The saphenous nerve: its course and importance in medial arthrotomy. Am J Sports Med 7:227–230
Jameson S, Emmerson K (2007) Altered sensation over the lower leg following hamstring graft anterior cruciate ligament reconstruction with transverse femoral fixation. Knee 14:314–320
Kaczmarczyk J, Sergiew M, Adamcewicz F, Kruczynski J (2007) Lower limb dysaesthesia after anterior cruciate ligament reconstructions with hamstring tendons. A comparison of vertical versus oblique harvest site incisions. Chir Narzadow Ruchu Ortop Pol 72:247–248
Kalthur SG, Sumalatha S, Nair N, Pandey AK, Sequeria S, Shobha L (2015) Anatomic study of infrapatellar branch of saphenous nerve in male cadavers. Ir J Med Sci 184:201–206
Kerver AL, Leliveld MS, den Hartog D, Verhofstad MH, Kleinrensink GJ (2013) The surgical anatomy of the infrapatellar branch of the saphenous nerve in relation to incisions for anteromedial knee surgery. J Bone Joint Surg Am 95:2119–2125
Kjaergaard J, Fauno LZ, Fauno P (2008) Sensibility loss after ACL reconstruction with hamstring graft. Int J Sports Med 29:507–511
Lai CC, Ardern CL, Feller JA, Webster KE (2017) Eighty-three per cent of elite athletes return to preinjury sport after anterior cruciate ligament reconstruction: a systematic review with meta-analysis of return to sport rates, graft rupture rates and performance outcomes. Br J Sports Med. https://doi.org/10.1136/bjsports-2016-096836
Lefevre N, Klouche S, Mirouse G, Herman S, Gerometta A, Bohu Y (2017) Return to sport after primary and revision anterior cruciate ligament reconstruction: a prospective comparative study of 552 patients from the FAST cohort. Am J Sports Med 45:34–41
Leite ML, Cunha FA, Costa BQ, Andrade RM, Diniz Junior JH, Temponi EF (2016) Relationship between peri-incisional dysesthesia and the vertical and oblique incisions on the hamstrings harvest in anterior cruciate ligament reconstruction. Rev Bras Ortop 51:667–671
Luo H, Yu JK, Ao YF, Yu CL, Peng LB, Lin CY et al (2007) Relationship between different skin incisions and the injury of the infrapatellar branch of the saphenous nerve during anterior cruciate ligament reconstruction. Chin Med J (Engl) 120:1127–1130
Marder RA, Raskind JR, Carroll M (1991) Prospective evaluation of arthroscopically assisted anterior cruciate ligament reconstruction. Patellar tendon versus semitendinosus and gracilis tendons. Am J Sports Med 19:478–484
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 62:1006–1012
Mohtadi NG, Chan DS, Dainty KN, Whelan DB (2011) Patellar tendon versus hamstring tendon autograft for anterior cruciate ligament rupture in adults. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD005960.pub2Cd005960
Pagnani MJ, Warner JJ, O’Brien SJ, Warren RF (1993) Anatomic considerations in harvesting the semitendinosus and gracilis tendons and a technique of harvest. Am J Sports Med 21:565–571
Papastergiou SG, Voulgaropoulos H, Mikalef P, Ziogas E, Pappis G, Giannakopoulos I (2006) Injuries to the infrapatellar branch(es) of the saphenous nerve in anterior cruciate ligament reconstruction with four-strand hamstring tendon autograft: vertical versus horizontal incision for harvest. Knee Surg Sports Traumatol Arthrosc 14:789–793
Parkkari J, Pasanen K, Mattila VM, Kannus P, Rimpela A (2008) The risk for a cruciate ligament injury of the knee in adolescents and young adults: a population-based cohort study of 46,500 people with a 9 year follow-up. Br J Sports Med 42:422–426
Portland GH, Martin D, Keene G, Menz T (2005) Injury to the infrapatellar branch of the saphenous nerve in anterior cruciate ligament reconstruction: comparison of horizontal versus vertical harvest site incisions. Arthroscopy 21:281–285
Sabat D, Kumar V (2013) Nerve injury during hamstring graft harvest: a prospective comparative study of three different incisions. Knee Surg Sports Traumatol Arthrosc 21:2089–2095
Samuelsen BT, Webster KE, Johnson NR, Hewett TE, Krych AJ (2017) Hamstring autograft versus patellar tendon autograft for ACL reconstruction: is there a difference in graft failure rate? A meta-analysis of 47,613 patients. Clin Orthop Relat Res. https://doi.org/10.1007/s11999-017-5278-9
Sanders B, Rolf R, McClelland W, Xerogeanes J (2007) Prevalence of saphenous nerve injury after autogenous hamstring harvest: an anatomic and clinical study of sartorial branch injury. Arthroscopy 23:956–963
Sipahioglu S, Zehir S, Sarikaya B, Levent A (2017) Injury of the infrapatellar branch of the saphenous nerve due to hamstring graft harvest. J Orthop Surg (Hong Kong) 25:2309499017690995
Spicer DD, Blagg SE, Unwin AJ, Allum RL (2000) Anterior knee symptoms after four-strand hamstring tendon anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 8:286–289
Tavakoli Darestani R, Bagherian Lemraski MM, Hosseinpour M, Kamrani-Rad A (2013) Electrophysiological assessment of injury to the infra-patellar branch(es) of the saphenous nerve during anterior cruciate ligament reconstruction using medial hamstring auto-grafts: vertical versus oblique harvest site incisions. Arch Trauma Res 2:118–123
Warren LF, Marshall JL (1979) The supporting structures and layers on the medial side of the knee: an anatomical analysis. J Bone Joint Surg Am 61:56–62
Funding
No funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study formal consent is not required.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Grassi, A., Perdisa, F., Samuelsson, K. et al. Association between incision technique for hamstring tendon harvest in anterior cruciate ligament reconstruction and the risk of injury to the infra-patellar branch of the saphenous nerve: a meta-analysis. Knee Surg Sports Traumatol Arthrosc 26, 2410–2423 (2018). https://doi.org/10.1007/s00167-018-4858-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-4858-x