Abstract
Purpose
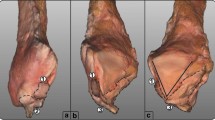
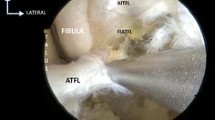
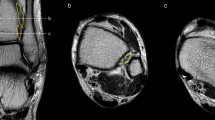
The purpose of this study was to determine the clinical utility of three bony tubercles: fibular obscure tubercle, talar obscure tubercle and tuberculum ligamenti calcaneofibularis, to serve as anatomical landmarks for defining the precise location of the origins and insertions of the anterior talofibular ligament (ATFL) and calcaneofibular ligament (CFL).
Methods
Twelve lower extremity cadaveric specimens were procured. The detectability of the tubercles was tested using palpation and fluoroscopy with subsequent confirmation after dissection. If the tubercles were present, then distances from the identified tubercles to the footprint centres and the intersection of the ATFL and CFL were measured to allow precise localization of the ATFL and CFL origin and intersection sites. Further, if the tubercles were not detectable, then an attempt to provide an alternative means of localizing ATFL and CFL origin and insertion sites was made by measuring distances between alternative landmarks and other important structures. All the measurements were performed by two researchers, and the results were averaged.
Results
The fibular obscure tubercle existed and was detectable in all specimens. It was located 1.3 mm proximal to the articular tip of the fibula, 2.7 mm to the intersection of the ATFL and CFL, 3.7 mm distal to the ATFL and 4.9 mm proximal to the CFL origins. The talar obscure tubercle existed 58 % of specimens and was detectable in 57 %. The talar obscure tubercle was located 1.4 mm to the ATFL. The ATFL insertion point was located 60 % of the distance from the inferolateral corner to the anterolateral corner of the of talar body along the anterior border of the talar lateral articular facet. The tuberculum ligamenti calcaneofibularis existed in 33 % of specimens and was detectable in 8 %. The CFL inserted 17 mm on a perpendicular projected line distal from the subtalar joint.
Conclusions
The fibular obscure tubercle was clinically relevant and reliable bony landmark of the ATFL and CFL origin location. However, the talar obscure tubercle was less reliable and the tuberculum ligamenti calcaneofibularis was rarely available and as such alternative landmarks for the ATFL and CFL insertion location should be utilized. The present study describes the utility of clinically relevant bony landmarks that may assist in identifying the origins and insertions of the ATFL and CFL to facilitate minimally invasive ankle stabilization surgery.






Similar content being viewed by others
Abbreviations
- FOT:
-
Fibular obscure tubercle
- TOT:
-
Talar obscure tubercle
- TLC:
-
Tuberculum ligamenti calcaneofibularis
- ATFL:
-
Anterior talofibular ligament
- CFL:
-
Calcaneofibular ligament
- CAI:
-
Chronic ankle instability
- MIS:
-
Minimally invasive ankle stabilization surgery
- AL:
-
Anterolateral
- IL:
-
Inferolateral
References
Acevedo JI, Mangone P (2015) Arthroscopic brostrom technique. Foot Ankle Int 36:465–473
Burks RT, Morgan J (1994) Anatomy of the lateral ankle ligaments. Am J Sports Med 22:72–77
Buzzi R, Todescan G, Brenner E, Segoni F, Inderster A, Aglietti P (1993) Reconstruction of the lateral ligaments of the ankle: an anatomic study with evaluation of isometry. J Sports Traumatol Relat Res 15:55–74
Clanton TO, Campbell KJ, Wilson KJ, Michalski MP, Goldsmith MT, Wijdicks CA, LaPrade RF (2014) Qualitative and quantitative anatomic investigation of the lateral ankle ligaments for surgical reconstruction procedures. J Bone Joint Surg Am 96:e98
Corte-Real NM, Moreira RM (2009) Arthroscopic repair of chronic lateral ankle instability. Foot Ankle Int 30:213–217
Cottom JM, Rigby RB (2013) The “all inside” arthroscopic brostrom procedure: a prospective study of 40 consecutive patients. J Foot Ankle Surg 52:568–574
Freeman MA (1965) Instability of the foot after injuries to the lateral ligament of the ankle. J Bone Joint Surg Br 47:669–677
Glazebrook M, Stone J, Matsui K, Guillo S, Takao M (2016) Percutaneous ankle reconstruction of lateral ligaments (Perc-Anti RoLL). Foot Ankle Int 37:659–664
Guillo S, Archbold P, Perera A, Bauer T, Sonnery-Cottet B (2014) Arthroscopic anatomic reconstruction of the lateral ligaments of the ankle with gracilis autograft. Arthrosc Tech 3:e593–e598
Guillo S, Cordier G, Sonnery-Cottet B, Bauer T (2014) Anatomical reconstruction of the anterior talofibular and calcaneofibular ligaments with an all-arthroscopic surgical technique. Orthop Traumatol Surg Res 100:S413–S417
Guillo S, Bauer T, Lee JW, Takao M, Kong SW, Stone JW, Mangone PG, Molloy A, Perera A, Pearce CJ, Michels F, Tourne Y, Ghorbani A, Calder J (2013) Consensus in chronic ankle instability: aetiology, assessment, surgical indications and place for arthroscopy. Orthop Traumatol Surg Res 99:S411–S419
Kelikian A, Sarrafian S (2011) Sarrafian’s anatomy of the foot and ankle: descriptive, topographic, functional. Lippincott, Williams & Wilkins, Wolters Kluwer, Philadelphia, pp 40–119, 163–222
Kerkhoffs Gino MMJ, Handoll Helen HG, de Bie R, Rowe Brian H, Struijs Peter AA (2007) Surgical versus conservative treatment for acute injuries of the lateral ligament complex of the ankle in adults. Cochrane Database Syst Rev 18:CD000380
Kim ES, Lee KT, Park JS, Lee YK (2011) Arthroscopic anterior talofibular ligament repair for chronic ankle instability with a suture anchor technique. Orthopedics 34:273
Kim HN, Dong Q, Hong DY, Yoon YH, Park YW (2014) Percutaneous Lateral ankle ligament reconstruction using a split peroneus longus tendon free graft: technical tip. Foot Ankle Int 35:1082–1086
Laidlaw PP (1904) The varieties of the Os Calcis. J Anat Physiol 38:133–143
Lui TH (2015) Modified arthroscopic Brostrom procedure. Foot Ankle Surg 21:216–219
Lui TH (2007) Arthroscopic-assisted lateral ligamentous reconstruction in combined ankle and subtalar instability. Arthrosc J Arthroscopic Relat Surg 23:554.e1–554.e5
Matsui K, Burgesson B, Takao M, Stone J, Guillo S, ESSKA AFAS Ankle Instability Group, Glazebrook M (2016) Minimally invasive surgical treatment of chronic ankle instability: a systematic review. Knee Surg Sports Traumatol Arthrosc 24:1040–1048
Matsui K, Takao M, Miyamoto W, Matsushita T (2016) Early recovery after arthroscopic repair compared to open repair of the anterior talofibular ligament for lateral instability of the ankle. Arch Orthop Trauma Surg 136:93–100
Matsui K, Takao M, Miyamoto W, Innami K, Matsushita T (2014) Arthroscopic Brostrom repair with Gould augmentation via an accessory anterolateral port for lateral instability of the ankle. Arch Orthop Trauma Surg 134:1461–1467
Michels F, Cordier G, Burssens A, Vereecke E, Guillo S (2016) Endoscopic reconstruction of CFL and the ATFL with a gracilis graft: a cadaveric study. Knee Surg Sports Traumatol Arthrosc 24:1007–1014
Miyamoto W, Takao M, Yamada K, Matsushita T (2014) Accelerated versus traditional rehabilitation after anterior talofibular ligament reconstruction for chronic lateral instability of the ankle in athletes. Am J Sports Med 42:1441–1447
Nery C, Raduan F, Del Buono A, Asaumi ID, Cohen M, Maffulli N (2011) Arthroscopic-assisted Brostrom-Gould for chronic ankle instability: a long-term follow-up. Am J Sports Med 39:2381–2388
Neuschwander TB, Indresano AA, Hughes TH, Smith BW (2013) Footprint of the lateral ligament complex of the ankle. Foot Ankle Int 34:582–586
Pijnenburg AC, Bogaard K, Krips R, Marti RK, Bossuyt PM, Dijk CN (2003) Operative and functional treatment of rupture of the lateral ligament of the ankle. J Bone Joint Surg Br 85:525–530
Sindel M (1998) Anatomy of the lateral ankle ligaments. Turk J Med Sci 28:53–56
Takao M, Glazebrook M, Stone J, Guillo S (2015) Ankle arthroscopic reconstruction of lateral ligaments (Ankle Anti-ROLL). Arthrosc Tech 4:e595–e600
Takao M, Matsui K, Stone JW, Glazebrook MA, Kennedy JG, Guillo S, Calder JD, Karlsson J, Ankle Instability Group (2016) Arthroscopic anterior talofibular ligament repair for lateral instability of the ankle. Knee Surg Sports Traumatol Arthrosc 24:1003–1006
Takao M, Miyamoto W, Matsui K, Sasahara J, Matsushita T (2012) Functional treatment after surgical repair for acute lateral ligament disruption of the ankle in athletes. Am J Sports Med 40:447–451
Taser F, Shafiq Q, Ebraheim NA (2006) Anatomy of lateral ankle ligaments and their relationship to bony landmarks. Surg Radiol Anat 28:391–397
Thès A, Klouche S, Ferrand M, Hardy P, Bauer T (2016) Assessment of the feasibility of arthroscopic visualization of the lateral ligament of the ankle: a cadaveric study. Knee Surg Sports Traumatol Arthrosc 24:985–990
Vega J, Golano P, Pellegrino A, Rabat E, Pena F (2013) All-inside arthroscopic lateral collateral ligament repair for ankle instability with a knotless suture anchor technique. Foot Ankle Int 34:1701–1709
Wang B, Xu X- (2013) Minimally invasive reconstruction of lateral ligaments of the ankle using semitendinosus autograft. Foot Ankle Int 34:711–715
Wenny R, Duscher D, Meytap E, Weninger P, Hirtler L (2015) Dimensions and attachments of the ankle ligaments: evaluation for ligament reconstruction. Anat Sci Int 90:161–171
Xu X, Hu M, Liu J, Zhu Y, Wang B (2014) Minimally invasive reconstruction of the lateral ankle ligaments using semitendinosus autograft or tendon allograft. Foot Ankle Int 35:1015–1021
Youn H, Kim YS, Lee J, Choi WJ, Lee JW (2012) Percutaneous lateral ligament reconstruction with allograft for chronic lateral ankle instability. Foot Ankle Int 33:99–104
Acknowledgments
We thank Prof. Mariano Monzo and his Surgical Skills Lab at University of Barcelona for support in this study.
European Society of Sports Traumatolgy, Knee surgery and Arthroscopy Ankle and Foot Associates Ankle Instability Group
Jorge Batista, Thomas Bauer, James Calder, Woo Jin Choi, Ali Ghorbani, Mark Glazebrook, Stéphane Guillo, Siu Wah Kong, Jon Karlsson, Jin Woo Lee, Peter G. Mangone, Frederick Michels, Andy Molloy, Caio Nery, Satoru Ozeki, Christopher Pearce, Anthony Perera, Hélder Pereira, Bas Pijnenburg, Fernando Raduan, James W. Stone, Masato Takao, Yves Tourné.
Author information
Authors and Affiliations
Consortia
Corresponding author
Rights and permissions
About this article
Cite this article
Matsui, K., Oliva, X.M., Takao, M. et al. Bony landmarks available for minimally invasive lateral ankle stabilization surgery: a cadaveric anatomical study. Knee Surg Sports Traumatol Arthrosc 25, 1916–1924 (2017). https://doi.org/10.1007/s00167-016-4218-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-016-4218-7