Abstract
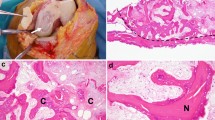
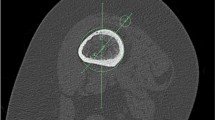
The objective of this study was to evaluate the bone mineral density (BMD) of the proximal tibia in the area adjacent to the fixation of the posterior cruciate ligament (PCL) and compare with the BMD in a similar area at the ideal site for anterior cruciate ligament fixation. Twenty healthy male subjects, undertaking similar daily physical activity were enrolled for this study. The mean age of the subjects was 22 years (range 20–24 years). The bone mineral density (BMD) at the proximal tibia was calculated using a quantitative CT scan of the dominant knee, and the data were recorded in Hounsfield units (HU). Two circular regions of interest, anterior and posterior, of identical diameters (10 mm) and thicknesses (5 mm) were studied. The results showed a significantly higher BMD in the anterior region (162.4±33.8 HU) than in the posterior one (104±24.6 HU) with a statistically significant difference (p=0.0001). The clinical implication of this finding is that the fixation should provide a firm construct for PCL reconstructions and be specifically designed for working in low bone quality areas such as the posterior proximal tibia.


Similar content being viewed by others
References
Brand JC, Pienkowski D, Steenlage E, Hamilton D, Johnson D, Caborn DNM (2000) Interference screw fixation strength of a quadrupled hamstring tendon graft is directly related to bone mineral density and insertion torque. Am J Sports Med 28:705–710
Brown GA, Peňa F, Gróntvedt T, Labadie D, Engebretsen L (1996) Fixation strength of interference screw fixation in bovine, young human and elderly human cadaver knees: influence of insertion torque, tunnel-bone block gap, and interference. Knee Surg Sports Traumatol Arthrosc 3:238–244
Butler JC, Branch TP, Hutton WC (1994) Optimal graft fixation-the effect of gap size and screw size on bone plug fixation in ACL reconstruction. Arthroscopy 10:524–529
Cann CE, Genant HK (1980) Precise measurement of vertebral mineral content using computer tomography. J Comput Assist Tomogr 4:493–500
Christensen P, Kiaer J, Melsen F, Nielsen HE, Sneppen O (1982) The subchondral bone of the proximal tibial epiphysis in osteoarthritis of the knee. Acta Orthop Scand 53:889–895
Ding M, Odgaard A, Linde F, Hvid I (2002) Age-related variations in the microstructure of human tibial cancellous bone. J Orthop Res 20:615–621
Eysel P, Schwitalle M, Oberstein A, Rompe J, Hopf C, Kullmer K (1998) Preoperative estimation of screw fixation strength in vertebral bodies. Spine 23:174–180
Fu FH, Bennett CH, Ma CB, Menetrey J, Lattermann C (2000) Current trends in anterior cruciate ligament reconstruction. Part II. Operative procedures and clinical correlations. Am J Sports Med 28:124–130
Greis PE, Burks RT, Bachus K, Luker MG (2001) The influence of tendon length and fit on the strength of a tendon-bone tunnel complex. A biomechanical and histologic study in the dog. Am J Sports Med 29:493–497
Höher J, Scheffler S, Weiler A (2003) Graft choice and graft fixation in PCL reconstruction. Knee Surg Sports Traumatol Arthrosc 11:297–306
Hopper K, Wang MP, Kunselman AR (2000) The use of clinical CT for baseline bone density assessment. J Comp Assist Tomogr 24:896–899
Johnson L, van Dijk N (1996) Metal and bioabsorbable interference screws: comparison of failure strength. Arthroscopy 13:177–182
Johnson LL (1998) Bone compaction techniques in knee ligament reconstruction. Techn Orthop 13:341–352
Kohn D, Rose C (1994) Primary stability of interference screw fixation. Am J Sports Med 22:334–338
Madsen OR, Scaadt O, Biddal H (1994) Bone mineral distribution of the proximal tibia in gonarthrosis assessed in vivo by photon absorption. Osteoarthritis Cartilage 2:141–147
Marti C, Imhoff AB, Bahrs C, Romero J (1997) Metal versus bioabsorbable interference screw for fixation of bone-patellar tendon-bone autograft in arthroscopic anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 5:217–221
Margheritini F, Rihn JA, Mauro CS, Stabile KJ, Woo SL-Y, Harner CD (2004) The effect of tibial fixation location on the biomechanics of posterior cruciate ligament reconstructed knee. Arthroscopy (in press)
Markolf KL, Slauterbeck JR, Armstrong KL, Shapiro MS, Finermann GAM (1997) A biomechanical study of replacement of the posterior cruciate ligament with a graft. Part I. Isometry, pre-tension of the graft, and anterior posterior laxity. J Bone Joint Surg Am 79:375–379
Matthews LS, Parks BG, Sabbagh RC (1988) Determination of fixation strength of large-diameter interference screw. Arthroscopy 14:70–74
Morrison JB (1969) Function of knee joint and various activities. Biomed Eng 5:573–580
Nurmi JT, Järvinen TLN, Kannus P, Sievänen H, Toukosalo J, Järvinen M (2002) Compaction versus extraction drilling for fixation of the hamstring tendon graft in anterior cruciate ligament reconstruction. Am J Sports Med 30:67–173
Nurmi JT, Kannus P, Sievänen H, Järvinen M, Järvinen TLN (2003) Compaction drilling does not increase the initial fixation strength of the hamstring tendon graft in anterior cruciate ligament reconstruction in a cadaver model. Am J Sports Med 31:353–358
Nurmi JT, Kannus P, Sievänen H, Järvelä T, Järvinen M, Järvinen TLN (2004) Interference screw fixation of soft tissue grafts in anterior cruciate ligament reconstruction. Part 1. Effect of tunnel compaction by serial dilators versus extraction drilling on the initial fixation strength. Am J Sports Med 32:411–417
Peňa F, Gróntvedt T, Brown GA, Aune A, Engebretsen L (1996) Comparison of failure strength between metallic and absorbable interference screws. Am J Sports Med 24:329–334
Pomeroy G, Baltz M, Pierz K, Nowak M, Post W, Fulkerson JP (1998) The effects of bone plug length and screw diameter on the holding strength of bone-tendon-bone grafts. Arthroscopy 14:148–152
Rittmeister M, Noble P, Bocell JR Jr, Alexander JW, Conditt MA, Kohl HW III (2001) Interactive effects of tunnel dilation on the mechanical properties of hamstring grafts fixed in the tibia with interference screws. Knee Surg Sports Traumatol Arthrosc 9:267–271
Shapiro JD, Jackson DW, Aberman HM, Lee TQ, Simon TM (1995) Comparison of pullout strength for seven and nine millimeter diameter interference screw size as used in ACL reconstruction. Arthroscopy 11:596–599
Sievänen H, Koskue V, Rauhio A, Kannus P, Heinonen A, Vuori I (1998) Peripheral quantitative computer tomography in human long bones: evaluation of in vitro and in vivo precision. J Bone Miner Res 13:871–882
Singhatat W, Lawhorn KW, Howell SM, Hull ML (2002) How four weeks of implantation affect the strength and stiffness of a tendon graft in bone tunnel. Am J Sports Med 30:506–513
Snyder BD, Zaltz I, Hall JE, Emans JB (1995) Predicting the integrity of vertebral bone screw fixation in anterior spinal instrumentation. Spine 20:1568–1574
Steenlage E, Brand JC Jr, Johnson DL, Caborn DNM (2002) Correlation of bone tunnel diameter with quadrupled hamstring graft fixation strength using a biodegradable interference screw. Arthroscopy 18:901–907
Tsuji T, Kitano K, Yamano Y, Sato T, Koike T (2001) Distribution of bone mineral density in the proximal tibia in mid-teens. J Bone Miner Metab 19:324–328
Wang CJ, Chen HH, Chen HS, Huang T (2002) Effects of knee position, graft tension, and mode of fixation in posterior cruciate ligament reconstruction: a cadaveric knee study. Arthroscopy 18:496–501
Weiler A, Hoffmann RFG, Stähelin AC, Bail HJ, Siepe CJ, Südkamp NP (1998) Hamstring tendon fixation using interference screws: a biomechanical study in calf tibial bone. Arthroscopy 14:29–37
Wittenberg RH, Shea M, Swartz DE, Lee KS, White AA III, Hayes WC (1991) Importance of bone mineral density in instrumented spine fusions. Spine 16:647–652
Zheng Y, Lu W, Zhu Q, Qin L, Zhong S, Leong J (2000) Variation in bone mineral density of the sacrum in young adults and its significance for sacral fixation. Spine 25:353–357
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mariani, P.P., Margheritini, F. & Bellelli, A. Bone mineral density of the proximal metaphysis of tibia: clinical relevance in posterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 13, 263–267 (2005). https://doi.org/10.1007/s00167-004-0564-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-004-0564-y