Abstract
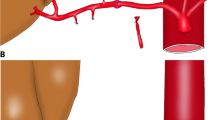
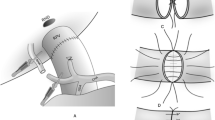
Use of operative microscopy (OM) has dramatically reduced the incidence of hepatic artery thrombosis (HAT) in children undergoing segmental liver transplantation. We used OM (12–16×) in our early experience. We changed to high power loupe magnification (6×) after 14 cases. We examined our experience with microvascular hepatic artery reconstruction in 28 consecutive children (<18 years) who underwent living donor (LDLT) or split liver transplantation (SLT). Reconstructions were done with interrupted, end-to-end anastomoses with 8–0 polypropylene using microvascular techniques. Group 1 consisted of 14 children who underwent LDLT employing OM for the hepatic artery anastomosis. Group 2 consisted of the subsequent 14 children (11 LDLT, 3 SLT) in whom 6× loupe optics were used for the arterial anastomosis. Grafts included 25 left lateral segments, 2 left lobes, and 1 right lobe. Recipients’ median age was 1.0 years (range 3 months to 17 years). The mean follow-up time was 27.1 months. There were no cases of HAT. Variables of age, sex, graft type, number of Doppler ultrasound exams (DUS), and biliary complications were similar between groups. Microvascular hepatic artery reconstruction in children with 6× loupe magnification can yield results as good as operative microscopy.



Similar content being viewed by others
References
Broelsch CE, Emond JC, Thistlethwaite JR, et al. Liver transplantation, including the concept of reduced size liver transplants in children. Ann Surg 1988; 208:410.
Tanaka K, Uemoto S, Tokunaga Y, et al. Surgical techniques and innovations in living related liver transplantation. Ann Surg 1993; 217:82.
Furuta S, Ikegami T, Nakazawa Y, et al. Hepatic artery reconstruction in living donor liver transplantation from the microsurgeon’s point of view. Liver Transpl Surg 1997; 3:388.
Uchiyama H, Hashimoto K, Hiroshige S, et al. Hepatic artery reconstruction in living-donor liver transplantation: a review of its techniques and complications. Surgery 2002; 131:S200.
Mori K, Nagata I, Yamagata I, et al. The introduction of microvascular surgery to hepatic artery reconstruction in living-donor liver transplantation: it’s surgical advantages compared with conventional procedures. Transplantation 1992; 54:263.
Saing H, Fan ST, Chan KL, et al. Liver transplantation in children: the experience of Queen Mary Hospital, Hong Kong. J Pediatr Surg 1997; 32:80.
Millis JM, Cronin DC, Brady LM, et al. Primary living donor transplantation at the University of Chicago: technical aspects of the first 104 recipients. Ann Surg 2000; 232:104.
Mori K, Nishizawa H, Sasaki S, et al. Hepatic artery reconstruction under microvascular surgery in partial liver transplantation from living donor. Transplant Proc 1993; 25:1093.
Inomoto T, Nishizawa F, Sasaki H, et al. Experiences of 120 microsurgical reconstructions of hepatic artery in living related liver transplantation. Surgery 1996; 119:20.
Acknowledgement
The Authors thank N. Erlich Lapid for her editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was presented at the biennial meeting of the International Association for the Study of the Liver, April, 2002, Madrid, Spain
About this article
Cite this article
Guarrera, J.V., Sinha, P., Lobritto, S.J. et al. Microvascular hepatic artery anastomosis in pediatric segmental liver transplantation: microscope vs loupe. Transpl Int 17, 585–588 (2004). https://doi.org/10.1007/s00147-004-0782-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00147-004-0782-8