Abstract
Purpose
Pulmonary ischemia–reperfusion is a pathological process seen in several clinical conditions, including lung transplantation, cardiopulmonary bypass, resuscitation for circulatory arrest, atherosclerosis, and pulmonary embolism. A better understanding of its molecular mechanisms is very important.
Methods
Rat left lung underwent in situ ischemia for 60 min, followed by 2 h of reperfusion. The gene expression profiles and Src protein tyrosine kinase (PTK) phosphorylation were studied over time, and PP2, an Src PTK inhibitor, was intravenously administered 10 min before lung ischemia to determine the role of Src PTK in lung injury.
Results
Reperfusion following ischemia significantly changed the expression of 169 genes, with Mmp8, Mmp9, S100a9, and S100a8 being the most upregulated genes. Ischemia alone only affected expression of 9 genes in the lung. However, Src PTK phosphorylation (activation) was increased in the ischemic lung, mainly on the alveolar wall. Src PTK inhibitor pretreatment decreased phosphorylation of Src PTKs, total protein tyrosine phosphorylation, and STAT3 phosphorylation. It increased phosphorylation of the p85α subunit of PI3 kinase, a signal pathway that can inhibit coagulation and inflammation. PP2 reduced leukocyte infiltration in the lung, apoptotic cell death, fibrin deposition, and severity of acute lung injury after reperfusion. Src inhibition also significantly reduced CXCL1 (GRO/KI) and CCL2 (MCP-1) chemokine levels in the serum.
Conclusion
During pulmonary ischemia, Src PTK activation, rather than alteration in gene expression, may play a critical role in reperfusion-induced lung injury. Src PTK inhibition presents a new prophylactic treatment for pulmonary ischemia–reperfusion-induced acute lung injury.
Similar content being viewed by others
Introduction
Pulmonary ischemia–reperfusion (IR) is associated with a wide range of clinical events, including lung transplantation, cardiopulmonary bypass, trauma, resuscitation for circulatory arrest, atherosclerosis, and pulmonary embolism [1]. It contributes to high morbidity and mortality in these patients [2]. In the case of lung transplantation (LTx), the warm ischemic period after cardiac arrest can cause cellular and tissue damage that often leads to lung injury [3]. Identifying molecular mechanisms associated with pulmonary IR-related lung injury may provide critical insight for the development of novel therapeutics.
Microarray-based technology provides a powerful tool to examine gene expression profiles of lungs at the genomic levels. It has been applied for gene expression profiling in IR-related tissue injury in the brain [4, 5], heart [6, 7], and kidney [8]. We have performed microarray studies on lung tissues collected during the cold IR process of rat [9] and human [10] LTx. Tyrosine phosphorylation is an important molecular mechanism related to acute inflammatory responses [11]. Particularly, activation of Src protein tyrosine kinase (PTK) has been identified as an essential mechanism for the recruitment and activation of monocytes, macrophages, and neutrophils [11]. It also plays a critical role in the regulation of vascular permeability [11, 12]. Src PTK activation is involved in ischemia- or IR-induced injury in the brain [13, 14], heart [15, 16], liver [17], and kidney [18, 19]. Src PTK inhibition prevented lipopolysaccharide (LPS)-induced acute lung injury [20, 21]. Protein tyrosine phosphorylation and Src PTK activity were altered over time during hypothermic IR processes in both clinically transplanted human lungs and experimentally transplanted rat lungs [22, 23].
In the present study, we performed gene profiling in rat lungs after pulmonary IR and investigated the effects of warm IR on Src PTK activation. Accordingly, a selective Src PTK inhibitor was employed to test the therapeutic potential of Src inhibition in preventing pulmonary IR-induced lung injury.
Materials and methods
Reagents and antibodies
A selective Src PTK inhibitor, 4-amino-5-(4-chlorophenyl)-7-(t-butyl)-pyrazolo [3,4-d] pyrimidine (PP2), was from Biomol International LP (Plymouth Meeting, PA). Antibodies for phosphorylated-Src (Tyr416), phoshporylated-p85 (Tyr199), STAT3, and phosphorylated-STAT3 (Tyr705) were from Cell Signaling Technology (Beverly, MA). Antibodies for p-Hck (Tyr411) and glyceraldehyde 3-phosphate dehydrogenase (GAPDH) were from Santa Cruz Biotechnology (Santa Cruz, CA). Antibodies for Src (GD11), p85α, and phosphotyrosine (4G10) were from Upstate Biotechnology Inc. (Lake Placid, NY). T6Rat IL-6 ELISA kit was from BD Biosciences (San Jose, CA). ELISA kits for CXCL1 (GRO/KC) and CCL2 (MCP-1) were from R&D Systems (Minneapolis, MN) and Invitrogen Inc. (Burlington, ON, Canada), respectively.
Animals
Male Sprague–Dawley rats, weighing from 300 to 350 g, were purchased from Charles River (Montreal, Canada). The experimental protocol was approved by the Toronto General Research Institute Animal Care and Use Committee. All animals received care in compliance with the Principles of Laboratory Animal Care formulated by the National Society for Medical Research, the Guide for the Care and Use of Laboratory Animals (NIH publication No. 85-23, Revised 1985, U.S. Government Printing Office, Washington, DC), and the Guide to the Care and Use of Experimental Animals formulated by the Canadian Council on Animal Care.
Rat lung IR model
Rats were anesthetized by intraperitoneal administration of ketamine (100 mg/kg) and xylazine (10 mg/kg). Atropine (0.2 mg) was injected intramuscularly. Animals were tracheotomized, intubated with a 12-gauge intravenous catheter, and ventilated using a model 683 ventilator (Harvard Apparatus Canada, Saint-Laurent, QC, Canada) with a tidal volume of 10 ml/kg with 2 cmH2O positive end-expiratory pressure (PEEP). Fraction of inspired oxygen (FiO2) and respiratory rate were kept at 0.6 and 70 cycles/min, respectively. A 24-gauge intravenous catheter was inserted into left jugular vein for injection. Anesthesia was maintained by administering one-third of the initial anesthetic dose in normal saline at 1 ml/h as a continuous infusion using a syringe pump (KDS100, KD Scientific Inc., Holliston, MA). Animals were placed on their right side and lateral thoracotomy was performed at the fifth left intercostal space. To achieve tissue ischemia, the left lung hilum was clamped at the end-expiration with two non-clash microclips (Sugita® Aneurysm Clip 07-940-88, Mizuho, Tokyo, Japan) 5 min after administration of an intravenous heparin bolus (50 IU/animal). The tidal volume was reduced to 6 ml/kg during the left lung hilum clamping. The lung was covered with a plastic wrap to prevent unnecessary evaporation. The clips were removed after 60 min and the thoracic cavity was sutured closed. Animals were placed in the supine position for 30 min or 120 min under mechanical ventilation in the same condition as before lung ischemia. In the Src PTK inhibition study, PP2 was dissolved with 20% dimethyl sulfoxide (DMSO) in normal saline. On the basis of literature precedent [24] and our pilot studies, PP2 (0.2 mg/kg) solution was injected into left jugular vein 10 min before lung ischemia with 20% DMSO as vehicle control.
Arterial blood gas analysis
At the end of 120 min reperfusion, animals were laparotomized to expose the thoracic and abdominal cavities. The right main bronchus and pulmonary vessels were occluded. Animals were ventilated with tidal volume of 6 ml/kg, 2 cmH2O of PEEP, 100% FiO2, and 70 breaths/min for 5 min. Blood samples for arterial blood gas analysis were obtained by puncturing the ascending aorta.
Histological studies
The pulmonary vasculature was flushed from the right ventricle with 20 ml of normal saline. The lung was injected with 10% formalin through the airway at 20 cmH2O of pressure. The tissues were dehydrated, embedded in paraffin, cut into 4-μm sections, and mounted. After rehydration by paraffin removal, the tissues were stained with hematoxylin and eosin [25]. Infiltrated leukocytes were counted in a blinded fashion. Martius Scarlet Blue staining was performed for alveolar fibrin deposition [26–28]. Cell death was assessed by terminal transferase dUTP nick end labeling (TUNEL) staining [27, 29, 30]. All images were acquired with a Nikon Eclipse 80i microscope.
Immunohistochemistry staining of phosphorylated Src
The paraffin-embedded lung sections were deparaffinized, followed by antigen retrieval in boiling 0.01 M citrate buffer (pH 6) for 20 min. The slides were then blocked with 3% H2O2 for 5 min, avidin and biotin (Vector Labs Inc., Burlington, Canada) for 15 min, and 5% goat serum in serum-free blocking reagent (Dako Inc., Burlington, Canada) for 1 h. The slides were incubated with a polyclonal anti-phosphorylated-Src (Tyr416) antibody (Abcam, Cambridge, MA) at 1:100 dilution overnight at 4°C. After washing with PBS (containing 0.1% Tween 20), the sections were incubated with goat anti-rabbit antibody (Vector Labs Inc.) for 30 min and developed with a DAB substrate kit (Zymed Labs, San Francisco, CA), followed by hematoxylin counterstaining. Images were scanned at 40× with a ScanScope, and the positive pixels per square millimeter were quantified and normalized with a Positive Pixel Count Algorithm program (Aperio, Vista, CA).
Microarray and data analysis
Total RNA was extracted [9, 31]. Equal amounts of RNA from three animals in each group were used for microarray. Rat Gene ST 1.0 chips from Affymetrix (Santa Clara, CA) were used. Probe-based analysis, background reduction, and quantile data normalization were performed in MAS 5.0 (Affymetrix). Scaled values were analyzed in Genespring (http://www.silicongenetics.com). Gene expression data were further filtered on the basis of raw intensity values. To identify differentially expressed genes, normalized data were imported into R (Statistical Package for Microarray Analysis, http://www.statistik.lmu.de/strimmer/notes/rexpress.html), analyzed using the Linear Models for Microarray Data library (LIMMA) of the Bioconductor package (http://www.bioconductor.org), and confirmed using Significance Analysis of Microarray (SAM, http://www-stat.stanford.edu/tibs/SAM). JMP version 5.0.1J (SAS Institute Inc., Cary, NC) was used for hierarchical cluster analysis. Functional networks induced by pulmonary IR were analyzed with Ingenuity Pathway Analysis (Ingenuity Systems, Inc. Redwood City, CA) [32].
Immunoblotting
Immunoblotting was performed as previously described [22, 23, 33]. In brief, 40 μg of protein was separated by SDS-PAGE and transferred to nitrocellulose membranes (Schleicher & Schuell, Whatman, Middlesex, UK). The membranes were incubated with designated antibodies. The proteins of interests were detected with an enhanced chemiluminescence detection kit (ECL) (Amersham Pharmacia Biotech, Little Chalfort, UK) on X-ray film.
Enzyme-linked immunosorbent assay (ELISA)
The inflammatory cytokine IL-6 levels in the lung lysates and serum levels of CXCL1 (GRO/KC) and CCL2 (MCP-1) were measured with ELISA, following the standard procedure.
Serum cytokine/chemokine analysis
Serum samples from 3 rats/group were tested for cytokines/chemokines levels with a multiplex magnetic beads assay (MILLIPLEX MAG Rat Cytokine/Chemokine Magnetic Bead Panel—Premixed 23 Plex, Millipore, Billerica, MA), following the company’s instructions.
Statistical analyses
Statistical analyses were performed using the statistical software JMP version 5.0.1J (SAS Institute Inc., Cary, NC). Results were expressed as the mean ± standard error of the mean (SEM). A Student’s t test was applied for comparison between two groups, whereas one-way ANOVA followed by Tukey–Kramer HSD tests were used for multiple groups. Differences are considered significant when the P value is no greater than 0.05.
Results
Pulmonary IR-induced lung injury
The severity of lung injury was determined by assessment of lung histology and oxygenation function. Compared to the non-ischemic right lung and the lungs in the sham group, the left lung appeared hyperemic following 60 min ischemia. Gross pathological changes were consistent with the congestion and hemorrhage. Hyperemic changes were further exacerbated after 120 min reperfusion (Fig. 1a top panel). Histological assessments confirmed the development of interstitial edema and alveolar hemorrhage in the ischemic lungs, which was further enhanced after reperfusion (Fig. 1a lower panel). Oxygenation function of the left lungs (PaO2/FiO2, ratio of the partial pressure of arterial oxygen to FiO2) was significantly decreased after reperfusion (I60/R120, Fig. 1b). Ischemia for 60 min followed by 120 min reperfusion caused acute lung injury.
Pulmonary IR-induced lung injury in rats. a Ischemia and IR resulted in diffuse alveolar damage in the left lung. Alveolar hemorrhage and interstitial edema were found in damaged left lung following ischemia and further enhanced after reperfusion. b Pulmonary IR (60 min ischemia and 120 min reperfusion) significantly reduced oxygenation function of the left lung (mean ± SEM, n = 6 in each group, *P < 0.05)
Gene expression profile after pulmonary ischemia and IR
To determine transcriptional changes associated with pulmonary ischemia and/or IR, we performed microarray analysis. Three conditions (I60, I60/R30, and I60/R120) were studied in comparison with the sham control. Of 27,342 expressed sequence tags spotted on the chip, 196 genes significantly changed during IR (Fig. 2a). Among them, 27 genes were significantly regulated after ischemia, of which only 9 genes were ischemia-specific, with 2 upregulated and 7 downregulated (Fig. 2b). In contrast, there were 169 genes differentially expressed primarily after reperfusion (Fig. 2b). Significant changes in gene expression were noted as early as with 30 min reperfusion (I60/R30). Most expression changes became more pronounced (further increased or decreased in the same direction) after 120 min reperfusion (I60/R120) (Fig. 2a). Specific trends can be seen from the top 40 upregulated (Table 1) and top 40 downregulated (Table 2) genes. In an unsupervised hierarchical cluster analysis, the sham and I60 groups were clustered together and separated from the reperfusion (I60/R30 and I60/R120) groups. A small group of genes is shown in Fig. 2c to illustrate the clustering distribution among these four groups.
Pulmonary IR-induced changes of gene expression. a Fold change of 196 genes expressed in log 2 scale. b Venn diagram shows the number of ischemia- or IR-specific genes. c Unsupervised hierarchical clustering analysis demonstrates gene expression patterns. Each column corresponds to one animal, and each row corresponds to a particular gene. The matrix represents the expression level of an individual gene in each sample, with red and green indicating gene expression levels above or below the reference RNA, respectively. Sham sham control animal, I60 60 min ischemia, I60/R30 60 min ischemia and 30 min reperfusion, I60/R120 60 min ischemia and 120 min reperfusion
To elucidate the molecular features of IR-induced lung injury, we used Ingenuity Pathway Analysis (http://www.ingenuity.com/) to search for enrichment in predicted functions amongst genes that were significantly altered in the IR group. “inflammatory response” was the top biological function, whereas the top molecular and cellular function was “cellular movement” (Supplementary Table 1). Indeed, most of the genes in the top network (network 1) are related to “cellular movement, hematological system development and function, immune cell trafficking”. These genes are connected to ERK, p38MAPK, PI3K, and PKCs, the signal transduction proteins that can be activated by and are involved in inflammatory responses (Fig. 3).
The top network of genes after pulmonary IR at 2 h. Ingenuity Pathway Analysis was performed on genes significantly changed after I60/R120 (ischemia 60 min and reperfusion 120 min). Signal network related to inflammatory response shows that ERK, p38MAPK, PI3K, and PKCs are located at the center of the network
We were surprised by the fact that only nine genes changed their expression levels after ischemia. These genes are not known to play a role in inflammation or tissue damage. This suggested that the major effects of pulmonary ischemia on lung tissues are not the alteration of gene expression, thus, we further examined the inflammatory response and changes of signal transduction.
Ischemia-induced inflammatory response and Src PTK activation
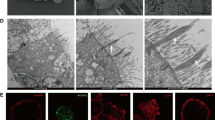
The tissue levels of IL-6 increased markedly after 60 min of ischemia (Fig. 4a), even though its gene expression levels remained unchanged as determined by the microarray assay. The total Src protein levels did not change during the IR period. In contrast, the phosphorylation of Src at tyrosine 416, a sign of Src activation, was increased in the ischemic lungs and decreased in a time-dependent fashion during the reperfusion period (Fig. 4b). The total protein tyrosine phosphorylation level was lower in sham and ischemic lungs but higher after reperfusion (Fig. 4b), suggesting that other PTKs and/or protein tyrosine phosphatases may be also involved in the regulation of protein tyrosine phosphorylation during the pulmonary IR process. We then performed immunohistochemistry staining to determine the distribution of activated Src PTK with an anti-pSrcY416 antibody. In the sham control group, phosphorylated Src (brown staining) was very low in the lung (Fig. 4c, left panel). The staining clearly increased on the alveolar septa after 60 min ischemia (Fig. 4c, middle panel), whereas scattered staining was observed in the infiltrated cells in the I60R120 group (Fig. 4c, right panel). The intensity of Src phosphorylation was quantified (Fig. 4d). The increased phosphorylation (activation) of Src PTK after ischemia may prime the lung tissue cells to subsequent inflammatory responses during reperfusion.
Changes of IL-6 protein levels and Src PTK tyrosine phosphorylation after pulmonary ischemia and IR. a IL-6 in the left lung lysate was increased after pulmonary ischemia and maintained at significantly higher levels after reperfusion (mean ± SEM, n = 3 in each group, *P < 0.05 compared with sham group). b Src Tyr 416-phosphorylation was increased after ischemia but decreased after reperfusion (top panel). Total Src protein levels did not change, whereas total protein tyrosine phosphorylation was higher after reperfusion (bottom panel). c Distribution of phosphorylated Src Tyr416 in the lung tissues. In sham group, pSrcTyr416 staining was very weak in the alveolar space. Ischemia increased the pSrcTyr416 in the alveolar wall (arrows). After 2 h reperfusion, pSrcTyr416 was seen mainly in infiltrated cells (arrowhead), and non-specific staining was found in the proteins that leaked into the alveolar space (asterisk). d The pSrcTyr416 staining density was quantified from four rats per group. *P < 0.01 compared with other groups; # P < 0.05 compared with Sham group
Src PTK inhibition before ischemia reduced pulmonary IR-induced lung injury
To determine the involvement of Src PTK activation in the pulmonary IR-induced lung injury, we administrated a chemical Src inhibitor, PP2, 10 min before ischemia through the jugular vein. In comparison with 20% DMSO (the organic solvent for PP2)-treated animals, PP2 pretreatment inhibited phosphorylation of Src Tyr-416 and phosphorylation of Hck, another Src PTK family member, at Tyr-411 during the ischemia period (Fig. 5a), leading to significantly reduced total protein tyrosine phosphorylation (Fig. 5b). In LPS-induced lung injury, STAT3 has been identified as a downstream signal of Src PTK [20]. STAT3 phosphorylation in the lung tissue was significantly decreased by PP2 pretreatment (Fig. 5c). Since Src PTK family is also involved in the PI3 kinase signal pathway [34], we then examined tyrosine phosphorylation of the p85α subunit of PI3K. Surprisingly, it was increased by PP2 pretreatment (Fig. 5d), suggesting an indirect effect of Src PTK on its phosphorylation. PI3 kinase activation suppresses coagulation and inflammation in endotoxemic mice [35].
Src inhibitor PP2 pretreatment reduced inflammation-related signaling. PP2 pretreatment inhibited phosphorylation of Src Tyr-416 and Hck Tyr-411 (a), total protein tyrosine phosphorylation (b), STAT3 phosphorylation (c), but increased tyrosine phosphorylation of PI3 kinase p85α subunit (d). N = 3 animals/group. *P ≤ 0.05
Lung injury at the end of 120 min reperfusion was reduced in PP2-pretreated animals compared with 20% DMSO-treated ones. Alveolar hemorrhage and interstitial edema were reduced (Fig. 6a). The number of infiltrated leukocytes in the alveolar space was significantly decreased in the PP2-treated group (Fig. 6b). The apoptotic cell death, as determined by TUNEL staining, was significantly reduced in the PP2 group (Fig. 6c, d). Fibrin deposition (seen in the DMSO group) was clearly reduced in the PP2 group (Fig. 6e). The oxygenation function was improved by the PP2 pretreatment, as PaO2/FiO2 was significantly higher in PP2-pretreated animals (Fig. 6f).
Src inhibitor PP2 pretreatment reduced pulmonary IR-induced lung injury. PP2 pretreatment reduced lung injury (a), infiltration of leukocytes in the alveolar space (b), TUNEL positive cell death (c and d), alveolar fibrin deposition (revealed by Martius Scarlet Blue staining, pink) (e), and significantly improved oxygenation function of the left lungs (f) after 60 min ischemia and 120 min reperfusion. N = 4 animals/group. *P < 0.05
We also examined the cytokine and chemokine levels in the serum. Among the 23 cytokines/chemokines tested, 8 of them showed measurable concentrations. Upon PP2 treatment, the levels of CXCL1 (GRO/KC) and CCL2 (MCP-1) were significantly decreased (Table 3). These results were validated with ELISA. The serum levels of CXCL1 (GRO/KC) decreased from 10,034 ± 1,378 to 1,724 ± 216 pg/ml (P = 0.004), and CCL2 (MCP-1) levels decreased from 752 ± 114 to 251 ± 34 pg/ml (P = 0.01). However, the mRNA levels of these two chemokines in the lung tissue lysates were not altered by PP2 treatment, indicating a systemic effect of PP2 on them. We conclude that Src PTK inhibition before ischemia is protective against pulmonary IR-induced lung injury.
Discussion
In the present study, we investigated pulmonary IR-induced gene expression profiles using a microarray/bioinformatics approach. Expression of many genes was significantly altered after reperfusion. Many of these upregulated genes are related to inflammatory responses (Table 1; Fig. 3). The top ranked genes include those associated with matrix metalloproteinases (Mmp8, Mmp9), chemotactic factors (S100a8, S100a9, and Fpr1), and inflammatory cytokine receptors (Il1r2, Il8rb). Proteins encoded by these genes are involved in inflammatory responses. Mmp9, Il1r2, S100a8, and S100a9 were also found in the top listed genes after 24 h hypothermic preservation followed by 2 h reperfusion in a rat LTx model [9]. Increased expression of these genes may reflect leukocyte infiltration. However, lung stromal cells, such as lung epithelial cells, may also contribute to the inflammatory responses [36].
Although ischemia for 60 min alone did not lead to dramatic changes in gene expression, formalin fixation of the ischemic left lung showed dark color, and IL-6 levels increased significantly. Tyrosine phosphorylation (activation) of c-Src was increased. PP2 pretreatment reduced Src and Hck PTK activation. Hck is another Src PTK family member, mainly expressed in granulocytes, monocytes, and macrophages. PP2 also reduced total protein tyrosine phosphorylation, phosphorylation of STAT3, a downstream signal of cytokine receptors [37, 38]. More interestingly, PP2 increased tyrosine phosphorylation of p85α subunits of PI3 kinase, suggesting that under IR conditions, Src PTK may affect p85α tyrosine phosphorylation through both direct and indirect mechanisms. Nonetheless, PI3 kinase pathway activation suppressed coagulation and inflammation in endotoxemic mice [35]. This may explain reduced cell death, fibrin deposition, and inflammatory cytokines in the present study.
More importantly, Src inhibition reduced lung injury, reduced leukocyte infiltration in the lung, apoptotic cell death, fibrin deposition, and prevented deterioration of oxygenation function of the IR lung. CXCL1 (GRO/KC) is an important chemokine for neutrophile recruitment, whereas CCL2 (MCP-1) is important for monocyte recruitment. Their serum levels were significantly reduced by PP2 pretreatment. Therefore, Src PTK activation in ischemic lung could be a critical mechanism which contributes to IR-induced lung injury.
The finding that Src inhibition reduced pulmonary IR-induced acute lung injury implicates its clinical application. PP2 has been shown to reduce organ injury in multiple animal models for different clinical situations [14, 15, 19, 20, 24]. However, PP2 is a hydrophobic chemical and cannot be dissolved directly in aqueous solution. Recently, a nano-formula has been developed for PP2, which is safe and effective in vivo to reduce LPS-induced lung injury [21]. Therefore, PP2, as well as many other hydrophobic chemicals which are effective in animal models, could be used clinically in the future, using nanoparticle-based drug delivery systems.
In conclusion, the results from the present study suggest that activation of Src PTK during the ischemic period may sensitize the lung to reperfusion-induced injury, which is associated with changes of genes related to inflammatory responses. Blocking Src activation before ischemia may represent a novel therapy to reduce pulmonary IR-induced lung injury.
References
den Hengst WA, Gielis JF, Lin JY, Van Schil PE, De Windt LJ, Moens AL (2010) Lung ischemia-reperfusion injury: a molecular and clinical view on a complex pathophysiological process. Am J Physiol Heart Circ Physiol 299:H1283–H1299
Phua J, Badia JR, Adhikari NK, Friedrich JO, Fowler RA, Singh JM, Scales DC, Stather DR, Li A, Jones A, Gattas DJ, Hallett D, Tomlinson G, Stewart TE, Ferguson ND (2009) Has mortality from acute respiratory distress syndrome decreased over time? A systematic review. Am J Respir Crit Care Med 179:220–227
Loehe F, Mueller C, Annecke T, Minor T, Bittmann I, Krombach F, Messmer K (2002) Tissue damage of non-heart-beating donor lungs after long-term preservation: evaluation of histologic alteration, bronchoalveolar lavage, and energy metabolism. Shock 17:502–507
Jin K, Mao XO, Eshoo MW, Nagayama T, Minami M, Simon RP, Greenberg DA (2001) Microarray analysis of hippocampal gene expression in global cerebral ischemia. Ann Neurol 50:93–103
Buttner F, Cordes C, Gerlach F, Heimann A, Alessandri B, Luxemburger U, Tureci O, Hankeln T, Kempski O, Burmester T (2009) Genomic response of the rat brain to global ischemia and reperfusion. Brain Res 1252:1–14
Stegall MD, Park WD, Kim DY, Covarrubias M, Khair A, Kremers WK (2002) Changes in intragraft gene expression secondary to ischemia reperfusion after cardiac transplantation. Transplantation 74:924–930
Amberger A, Schneeberger S, Hernegger G, Brandacher G, Obrist P, Lackner P, Margreiter R, Mark W (2002) Gene expression profiling of prolonged cold ischemia and reperfusion in murine heart transplants. Transplantation 74:1441–1449
Yoshida T, Kurella M, Beato F, Min H, Ingelfinger JR, Stears RL, Swinford RD, Gullans SR, Tang SS (2002) Monitoring changes in gene expression in renal ischemia-reperfusion in the rat. Kidney Int 61:1646–1654
Yamane M, Liu M, Kaneda H, Uhlig S, Waddell TK, Keshavjee S (2005) Reperfusion-induced gene expression profiles in rat lung transplantation. Am J Transplant 5:2160–2169
Anraku M, Cameron MJ, Waddell TK, Liu M, Arenovich T, Sato M, Cypel M, Pierre AF, de Perrot M, Kelvin DJ, Keshavjee S (2008) Impact of human donor lung gene expression profiles on survival after lung transplantation: a case-control study. Am J Transplant 8:2140–2148
Okutani D, Lodyga M, Han B, Liu M (2006) Src protein tyrosine kinase family and acute inflammatory responses. Am J Physiol Lung Cell Mol Physiol 291:L129–L141
Thomas SM, Brugge JS (1997) Cellular functions regulated by Src family kinases. Annu Rev Cell Dev Biol 13:513–609
Paul R, Zhang ZG, Eliceiri BP, Jiang Q, Boccia AD, Zhang RL, Chopp M, Cheresh DA (2001) Src deficiency or blockade of Src activity in mice provides cerebral protection following stroke. Nat Med 7:222–227
Lennmyr F, Ericsson A, Gerwins P, Akterin S, Ahlstrom H, Terent A (2004) Src family kinase-inhibitor PP2 reduces focal ischemic brain injury. Acta Neurol Scand 110:175–179
Takeishi Y, Huang Q, Wang T, Glassman M, Yoshizumi M, Baines CP, Lee JD, Kawakatsu H, Che W, Lerner-Marmarosh N, Zhang C, Yan C, Ohta S, Walsh RA, Berk BC, Abe J (2001) Src family kinase and adenosine differentially regulate multiple MAP kinases in ischemic myocardium: modulation of MAP kinases activation by ischemic preconditioning. J Mol Cell Cardiol 33:1989–2005
Weis S, Shintani S, Weber A, Kirchmair R, Wood M, Cravens A, McSharry H, Iwakura A, Yoon YS, Himes N, Burstein D, Doukas J, Soll R, Losordo D, Cheresh D (2004) Src blockade stabilizes a Flk/cadherin complex, reducing edema and tissue injury following myocardial infarction. J Clin Invest 113:885–894
Cursio R, Miele C, Filippa N, Van Obberghen E, Gugenheim J (2006) Alterations in protein tyrosine kinase pathways in rat liver following normothermic ischemia-reperfusion. Transplant Proc 38:3362–3365
Takikita-Suzuki M, Haneda M, Sasahara M, Owada MK, Nakagawa T, Isono M, Takikita S, Koya D, Ogasawara K, Kikkawa R (2003) Activation of Src kinase in platelet-derived growth factor-B-dependent tubular regeneration after acute ischemic renal injury. Am J Pathol 163:277–286
Baldwin C, Chen ZW, Bedirian A, Yokota N, Nasr SH, Rabb H, Lemay S (2006) Upregulation of EphA2 during in vivo and in vitro renal ischemia-reperfusion injury: role of Src kinases. Am J Physiol Renal Physiol 291:F960–F971
Severgnini M, Takahashi S, Tu P, Perides G, Homer RJ, Jhung JW, Bhavsar D, Cochran BH, Simon AR (2005) Inhibition of the Src and Jak kinases protects against lipopolysaccharide-induced acute lung injury. Am J Respir Crit Care Med 171:858–867
Fung S-Y, Oyaizu T, Yang H, Han B, Keshavjee S, Liu M (2011) The potential of nanoscale combination of self-assembling peptide and amino acids of the Src tyrosine kinase inhibitor in acute lung injury. Biomaterials 32:4000–4008
Keshavjee S, Zhang XM, Fischer S, Liu M (2000) Ischemia reperfusion-induced dynamic changes of protein tyrosine phosphorylation during human lung transplantation. Transplantation 70:525–531
Sakiyama S, dePerrot M, Han B, Waddell TK, Keshavjee S, Liu M (2003) Ischemia-reperfusion decreases protein tyrosine phosphorylation and p38 mitogen-activated protein kinase phosphorylation in rat lung transplants. J Heart Lung Transpl 22:338–346
Khadaroo RG, He R, Parodo J, Powers KA, Marshall JC, Kapus A, Rotstein OD (2004) The role of the Src family of tyrosine kinases after oxidant-induced lung injury in vivo. Surgery 136:483–488
Okutani D, Han B, Mura M, Waddell TK, Keshavjee S, Liu M (2007) High-volume ventilation induces pentraxin 3 expression in multiple acute lung injury models in rats. Am J Physiol Lung Cell Mol Physiol 292:L144–L153
He X, Han B, Mura M, Li L, Cypel M, Soderman A, Picha K, Yang J, Liu M (2008) Anti-human tissue factor antibody ameliorated intestinal ischemia reperfusion-induced acute lung injury in human tissue factor knock-in mice. PLoS One 3:e1527
Han B, Haitsma JJ, Zhang Y, Bai X, Rubacha M, Keshavjee S, Zhang H, Liu M (2011) Long pentraxin PTX3 deficiency worsens LPS-induced acute lung injury. Intensive Care Med 37:334–342
He X, Han B, Bai X, Zhang Y, Cypel M, Mura M, Keshavjee S, Liu M (2010) PTX3 as a potential biomarker of acute lung injury: supporting evidence from animal experimentation. Intensive Care Med 36:356–364
Mura M, Andrade CF, Han B, Seth R, Zhang Y, Bai XH, Waddell TK, Hwang D, Keshavjee S, Liu M (2007) Intestinal ischemia-reperfusion-induced acute lung injury and oncotic cell death in multiple organs. Shock 28:227–238
Mura M, Binnie M, Han B, Li C, Andrade CF, Shiozaki A, Zhang Y, Ferrara N, Hwang D, Waddell TK, Keshavjee S, Liu M (2010) Functions of type II pneumocyte-derived vascular endothelial growth factor in alveolar structure, acute inflammation, and vascular permeability. Am J Pathol 176:1725–1734
dos Santos CC, Okutani D, Hu P, Han B, Crimi E, He X, Keshavjee S, Greenwood C, Slutsky AS, Zhang H, Liu M (2008) Differential gene profiling in acute lung injury identifies injury-specific gene expression. Crit Care Med 36:855–865
Shiozaki A, Lodyga M, Bai X, Nadesalingam J, Oyaizu T, Winer D, Asa SL, Keshavjee S, Liu M (2011) XB130, a novel adaptor protein, promotes thyroid tumor growth. Am J Pathol 178:391–401
Cardella JA, Keshavjee SH, Bai XH, Yeoh JS, Granton JT, Meade MO, Matte-Martyn A, Waddell TK, Liu M (2004) Increased expression of nitric oxide synthase in human lung transplants after nitric oxide inhalation. Transplantation 77:886–890
Sagan D, Eckardt-Schupp F, Eichholtz-Wirth H (2008) Reduced expression of SRC family kinases decreases PI3K activity in NBS1−/− lymphoblasts. Biochem Biophys Res Commun 377:181–186
Schabbauer G, Tencati M, Pedersen B, Pawlinski R, Mackman N (2004) PI3K-Akt pathway suppresses coagulation and inflammation in endotoxemic mice. Arterioscler Thromb Vasc Biol 24:1963–1969
dos Santos CC, Han B, Andrade CF, Bai X, Uhlig S, Hubmayr R, Tsang M, Lodyga M, Keshavjee S, Slutsky AS, Liu M (2004) DNA microarray analysis of gene expression in alveolar epithelial cells in response to TNFalpha, LPS, and cyclic stretch. Physiol Genomics 19:331–342
Garcia R, Bowman TL, Niu G, Yu H, Minton S, Muro-Cacho CA, Cox CE, Falcone R, Fairclough R, Parsons S, Laudano A, Gazit A, Levitzki A, Kraker A, Jove R (2001) Constitutive activation of Stat3 by the Src and JAK tyrosine kinases participates in growth regulation of human breast carcinoma cells. Oncogene 20:2499–2513
Aggarwal BB, Kunnumakkara AB, Harikumar KB, Gupta SR, Tharakan ST, Koca C, Dey S, Sung B (2009) Signal transducer and activator of transcription-3, inflammation, and cancer: how intimate is the relationship? Ann N Y Acad Sci 1171:59–76
Acknowledgments
Drs. Takeshi Oyaizu and Atsushi Shiozaki were recipients of Research Fellowship awards from the Uehara Memorial Foundation, Japan, and the International Society for Heart and Lung Transplantation. Dr. Shan-Yu Fung was a recipient of Fellowship award from the Ministry of Research and Innovation of Ontario. This study was supported by research grants from the Canadian Institutes of Health Research (MOP-13270, MOP-42546) and Multi Organ Transplantation Academic Enhancement Funds of University Health Network.
Conflicts of interest
The authors have no financial conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
T. Oyaizu and S.-Y. Fung contribution equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Oyaizu, T., Fung, SY., Shiozaki, A. et al. Src tyrosine kinase inhibition prevents pulmonary ischemia–reperfusion-induced acute lung injury. Intensive Care Med 38, 894–905 (2012). https://doi.org/10.1007/s00134-012-2498-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-012-2498-z