Abstract
Purpose
To describe outcome and changes in clotting and inflammatory parameters in an uncontrolled case series of consecutive patients with severe sepsis who received protein C concentrate soon after cardiac surgery.
Methods
From January 2007 to January 2008 nine consecutive adult patients with severe sepsis or septic shock and two or more organ failure after cardiac surgery received protein C concentrate, 50 IU/kg as a bolus followed by continuous infusion of 3 IU/kg per hour for 72 h.
Results
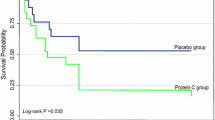
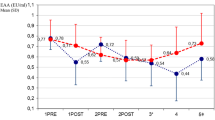
The increase in protein C levels was accompanied by an early drop in interleukins and near-normalization of prothrombin time, activated partial thromboplastin time, antithrombin and thrombin–antithrombin complex levels (p ≤ 0.03). No patient experienced drug-related side effects. Thirty-day mortality was 11% (1 patient) compared to the expected mortality of 68%.
Conclusions
In this pilot, uncontrolled study of nine patients with sepsis-induced double organ failure following cardiac surgery, treatment with protein C concentrate was associated with significant improvement in clinical, inflammatory and clotting parameters, no bleeding and low 30-day mortality.


Similar content being viewed by others
References
Bernard GR, Vincent JL, Laterre PF, LaRosa SP, Dhainaut JF, Lopez-Rodriguez A, Steingrub JS, Garber GE, Helterbrand JD, Ely EW, Fisher CJ Jr, Recombinant human protein C Worldwide Evaluation in Severe Sepsis (PROWESS) study group (2001) Efficacy and safety of recombinant human activated protein C for severe sepsis. N Engl J Med 344:699–709
Dellinger RP, Levy MM, Carlet JM, Bion J, Parker MM, Jaeschke R, Reinhart K, Angus DC, Brun-Buisson C, Beale R, Calandra T, Dhainaut JF, Gerlach H, Harvey M, Marini JJ, Marshall J, Ranieri M, Ramsay G, Sevransky J, Thompson BT, Townsend S, Vender JS, Zimmerman JL, Vincent JL (2008) Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock: 2008. Intensive Care Med 34:17–60 Erratum in: Intensive Care Med 34:783–785
Fisher CJ Jr, Yan SB (2000) Protein C levels as prognostic indicator of outcome in sepsis and related diseases. Crit Care Med 28(9 Suppl):S49–S56
Macias WL, Nelson DR (2004) Severe protein C deficiency predicts early death in severe sepsis. Crit Care Med 32(5 Suppl):S223–S228
White B, Livingstone W, Murphy C, Hodgson A, Rafferty M, Smith OP (2000) An open-label study of the role of adjuvant hemostatic support with protein C replacement therapy in purpura fulminans-associated meningococcemia. Blood 96:3719–3724
Clarke RC, Johnston JR, Mayne EE (2000) Meningococcal septicaemia: treatment with protein C concentrate. Intensive Care Med 26:471–473
de Kleijn ED, de Groot R, Hack CE, Mulder PG, Engl W, Moritz B, Joosten KF, Hazelzet JA (2003) Activation of protein C following infusion of protein C concentrate in children with severe meningococcal sepsis and purpura fulminans: a randomized, double-blinded, placebo-controlled, dose-finding study. Crit Care Med 31:1839–1847
Schellongowski P, Bauer E, Holzinger U, Staudinger T, Frass M, Laczika K, Locker GJ, Quehenberger P, Rabitsch W, Schenk P, Knöbl P (2006) Treatment of adult patients with sepsis-induced coagulopathy and purpura fulminans using a plasma-derived protein C concentrate (Ceprotin). Vox Sang 90:294–301
Rintala E, Kauppila M, Seppälä OP, Voipio-Pulkki LM, Pettilä V, Rasi V, Kotilainen P (2000) Protein C substitution in sepsis-associated purpura fulminans. Crit Care Med 28:2373–2378
Baratto F, Michielan F, Meroni M, Dal Palù A, Boscolo A, Ori C (2008) Protein C concentrate to restore physiological values in adult septic patients. Intensive Care Med 34:1707–1712
Crivellari M, Marino G, Landoni G, Belloni I, Bigami E, Zangrillo A (2008) Administration of human protein C concentrates in patients with double organ failure and severe sepsis after cardiac surgery. Minerva Anestesiol 74:48–49
Vincent JL, Bernard GR, Beale R, Doig C, Putensen C, Dhainaut JF, Artigas A, Fumagalli R, Macias W, Wright T, Wong K, Sundin DP, Turlo MA, Janes J (2005) Drotrecogin alfa (activated) treatment in severe sepsis from the global open-label trial ENHANCE: further evidence for survival and safety and implications for early treatment. Crit Care Med 33:2266–2277
Liaw PC, Ferrell G, Esmon CT (2003) A monoclonal antibody against activated protein C allows rapid detection of activated protein C in plasma and reveals a calcium ion dependent epitope involved in factor Va inactivation. J Thromb Haemost 1:662–670
Bakhtiari K, Meijers JC, de Jonge E, Levi M (2004) Prospective validation of the international society of thrombosis and haemostasis scoring system for disseminated intravascular coagulation. Crit Care Med 32:2416–2421
Zangrillo A, Landoni G, Fumagalli L, Bove T, Bellotti F, Sottocorna O, Roberti A, Marino G (2006) Methicillin-resistant Staphylococcus species in a cardiac surgical intensive care unit: a 5-year experience. J Cardiothorac Vasc Anesth 20:31–37
Esmon CT (2006) Inflammation and the activated protein C anticoagulant pathway. Semin Thromb Hemost 32(Suppl 1):S49–S60
Mosnier LO, Zlokovic BV, Griffin JH (2007) The cytoprotective protein C pathway. Blood 109:3161–3172
Bae JS, Yang L, Manithody C, Rezaie AR (2007) The ligand occupancy of endothelial protein C receptor switches the protease-activated receptor 1-dependent signaling specificity of thrombin from a permeability-enhancing to a barrier-protective response in endothelial cells. Blood 110:3909–3916
Acknowledgments
We thank Dr. Charles and Naomi Esmon for their kind gift of the monoclonal antibody HAPC-1555. We are also indebted to Mariano Fichera, RN, Isotta Virzo, RN, Cristiano Chiappa, RN, Giuseppe Giardina, RN, and Giulio Cozzuto, RN, for their appreciated contribution to this work.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Crivellari, M., Della Valle, P., Landoni, G. et al. Human protein C zymogen concentrate in patients with severe sepsis and multiple organ failure after adult cardiac surgery. Intensive Care Med 35, 1959–1963 (2009). https://doi.org/10.1007/s00134-009-1584-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-009-1584-3