Abstract
Objective
This study aimed to assess the level of agreement of both intermittent cardiac output monitoring by the lithium dilution technique (COLi) and continuous cardiac output monitoring (PulseCOLi) using the arterial pressure waveform with intermittent thermodilution using a pulmonary artery catheter (COPAC).
Design
Prospective, single-center evaluation.
Setting
University Hospital Intensive Care Unit.
Patients
Patients (n = 23) receiving liver transplantation.
Intervention
Pulmonary artery catheters were placed in all patients and COPAC was determined using thermodilution. COLi and PulseCOLi measurements were made using the LiDCO system.
Measurements and main results
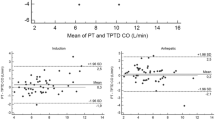
Data were collected after intensive care unit admission and every 8 h until the 48th hour. A total of 151 COPAC, COLi and PulseCOLi measurements were analysed. Bias and 95% limit of agreement were 0.11 lmin–1 and –1.84 to + 2.05 lmin–1 for COPAC vs. COLi (r = 0.88) resulting in an overall percentage error of 15.6%. Bias and 95% limit of agreement for COPAC vs. PulseCOLi were 0.29 lmin–1 and –1.87 to + 2.46 lmin–1 (r = 0.85) with a percentage error of 16.8%. Subgroup analysis revealed a percentage error of 15.7% for COPAC vs. COLi and 15.1% for COPAC vs. PulseCOLi for data pairs less than 8 lmin–1, and percentage errors of 15.5% and 18.5% respectively for data pairs higher than 8 lmin–1.
Conclusion
In patients with hyperdynamic circulation, intermittent and continuous CO values determined using the LiDCO system showed good agreement with those obtained by intermittent pulmonary artery thermodilution.



Similar content being viewed by others
References
Eisenberg PR, Jaffe AS, Schuster DP (1984) Clinical evaluation compared to pulmonary artery catheterization in the hemodynamic assessment of critically ill patients. Crit Care Med 12:549–553
De Wolf A (1993) Hemodynamic monitoring during orthotopic liver transplantation. Transplant Proc 25:1863–1864
Della Rocca G, Costa MG, Pompei L, Coccia C, Pietropaoli P (2002) Continuous and intermittent cardiac output measurement: pulmonary artery catheter vs. aortic transpulmonary technique. Br J Anaesth 88:350–356
Bottiger BW, Sinner B, Motsch J, Bach A, Bauer H, Martin E (1997) Continuous vs. intermittent thermodilution cardiac output measurement during orthotopic liver transplantation. Anaesthesia 52:207–214
Boldt J, Menges T, Wollbruck M, Hammermann H, Hempelmann G (1994) Is continuous cardiac output measurement using thermodilution technique reliable in the critically ill patients? Crit Care Med 22:1913–1918
Yeldermann ML (1990) Continuous measurement of cardiac output with the use of stochastic system identification techniques. J Clin Monit 6:322–332
Rodig G, Prasser C, Keyl A, Liebold A, Hobbhahn J (1999) Continuous cardiac output measurement: pulse contour analysis vs. thermodilution technique in cardiac surgical patients. Br J Anaesth 82:525–530
Linton RA, Band DM, Haire KM (1993) A new method of measuring cardiac output using lithium dilution. Br J Anaesth 71:262–266
Linton RA, Band DM, O'Brien TK, Jonas M, Leach R (1997) Lithium dilution cardiac output measurement: a comparison with thermodilution. Crit Care Med 25:1796–1800
Band DM, Linton RAF, O'Brien TK, Jonas MM, Linton NW (1997) The shape of indicator dilution curves for cardiac output measurement in man. J Physiol (Lond) 498:225–229
Kurita T, Morita K, Kato S, Kikura M, Horie M, Ikeda K (1997) Comparison of the accuracy of the lithium dilution technique with the thermodilution technique for measurement of cardiac output. Br J Anaesth 79:770–775
Mason D, O'Gray M, Woods JP, McDonell W (2001) Assessment of lithium dilution cardiac output as technique for measurement of cardiac output in dogs. Am J Vet Res 62:1255–1261
Linton RA, Young LE, Marlin DJ, Blissitt KJ, Brearley JC, Jonas MM, O'Brien TK, Linton NW, Band DM, Hollingworth C, Jones RS (2000) Cardiac output measured by lithium dilution, thermodilution and transesophageal Doppler echocardiography in anesthetized horses. Am J Vet Res 61:731–737
Pearse RM, Ikram K, Barry J (2004) Equipment review: an appraisal of the LiDCO™ Plus method of measuring cardiac output. Crit Care 8:190–195
Linton RA, Jonas MM, Tibby SM, Murdoch IA, O'Brien TK, Linton NWF, Band DM (2000) Cardiac output measured by lithium dilution and transpulmonary thermodilution in patients in a paediatric intensive care unit. Intensive Care Med 26:1507–1511
Pittman J, Bar-Yosef S, SumPing J, Sherwood M, Mark J (2005) Continuous cardiac output monitoring with pulse contour analysis: a comparison with lithium indicator dilution cardiac output measurement. Crit Care Med 33:2015–2021
Hamilton TT, Huber LM, Jessen ME (2002) PulseCO™: A less-invasive method to monitor cardiac output from arterial pressure after cardiac surgery. Ann Thorac Surg 74:S1408–S1412
Costa MG, Lugano M, Coccia C, Della Rocca G (2004) Continuous and intermittent lithium dilution cardiac output measurements. Eur J Anaesthesiol 21:A88
Hourani JM, Bellamy PE, Tashkin DP, Batra P, Simmons MS (1991) Pulmonary dysfunction in advanced liver disease: frequent occurrence of an abnormal diffusing capacity. Am J Med 90:693–700
Rhodes A, Sunderland R (2005) Arterial pulse power analysis: the LiDCO™ Plus System. Functional hemodynamic monitoring. In: Pinsky M, Payen D (eds) Update in intensive care and emergency medicine. Springer, Berlin Heidelberg New York, pp 183–192
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Critchley LAH, Critchley JAJH (1999) A meta-analysis of studies using bias and precision statistics to compare cardiac output measurement techniques. J Clin Monitor 15:85–91
Mantha S, Roizen MF, Fleisher LA, Thisted R, Foss J (2000) Comparing methods of clinical measurement: reporting standards for Bland and Altman analysis. Anesth Analg 90:593–602
Ma Z, Lee S (1996) Cirrhotic cardiomyopathy: getting to the heart of the matter. Hepatology 24:451–459
Nasraway SA, Klein RD, Spanier TB, Rohrer RJ, Freeman RB, Rand WM, Benotti PN (1995) Haemodynamic correlates of outcome in patients undergoing orthotopic liver transplantation. Evidence for early postoperative myocardial depression. Chest 107:218–224
Soni N (1996) Swan song for the Swan-Ganz catheter? The use of pulmonary artery catheter probably needs re-evaluation, but they should not be banned. BMJ 313:173–174
Dalen JE (2001) The pulmonary artery catheter–friend, foe, or accomplice? J Am Med Assoc 286:348–350
Harvey S, Harrison DA, Singer M, Ashcroft J, Jones CM, Elbourne D, Brampton W, Williams D, Young D, Rowan K (2005) Assessment of the clinical effectiveness of pulmonary artery catheters in management of patients in intensive care (PAC-Man): a randomised controlled trial. Lancet 366:472–477
Antonelli M, Levy M, Andrews PJD, Chastre J, Hudson LD, Manthous C, Meduri GU, Moreno RP, Putensen C, Stewart T, Torres A (2006) Hemodynamic monitoring in shock and implications for management. Intensive Care Med 33:575–590
Kim JJ, Dreyer J, Chang AC, Breinhot III JP, Grifka RG (2006) Arterial pulse wave analysis: an accurate means of determining cardiac output in children. Crit Care Med 7:532–535
Pearse R, Dawson D, Fawcett J, Rhodes A, Grounds RM, Bennett ED (2005) Early goal-directed therapy after major surgery reduces complications and duration of hospital stay. A randomised, controlled trial. Crit Care 9:R687–R693
Acknowledgements
We thank Dr. L. Scudeller (MD, Clinic of Infectious Diseases, University of Udine), who performed the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
Descriptor: 34 Cardiovascular Monitoring
Rights and permissions
About this article
Cite this article
Costa, M.G., Della Rocca, G., Chiarandini, P. et al. Continuous and intermittent cardiac output measurement in hyperdynamic conditions: pulmonary artery catheter vs. lithium dilution technique. Intensive Care Med 34, 257–263 (2008). https://doi.org/10.1007/s00134-007-0878-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-007-0878-6