Abstract
Objective
Measurements from the pulmonary pressure-volume (PV) curve have been proposed to adjust ventilator settings. We investigated the effects of repeated construction of an inflation PV curve implemented in a standard ventilator on recruitment or derecruitment in acutely injured lungs.
Design and setting
Prospective experimental animal study in eight anesthetized and mechanically ventilated pigs.
Interventions
Acute lung injury was induced by lung lavage and animals were ventilated in volume controlled mode with PEEP 10 cmH2O. The PV curve was constructed five times repeatedly by constant pressure rise, after which ventilation with the preset PEEP was resumed immediately. Studies of hemodynamics, lung mechanics, blood gases and computed tomography were carried out before and after maneuvers.
Measurements and results
Derecruitment was assessed as an increase in nonaerated lung volume (VNON), and VPEEP was the end-expiratory volume difference between PEEP and ZEEP. There was a significant decrease in PaO2 from 90.4±33.3 to 70.9±36.3 mmHg and a rise in venous admixture from 47.8±12.7 to 59.1±16.6%. VPEEP was reduced from 244 to 202 ml. A corresponding decrease in normally aerated lung volume was observed, while regression analysis revealed increase in VNON depending on the amount of preexisting atelectasis.
Conclusions
Repeated generation of the PV curve with a readily available tool resulted in worsened oxygenation. Derecruitment of the lungs occurred with loss of PEEP at the start of the maneuver, which could not be recovered by a maximum inflation pressure of 40 cmH2O. Repeated use of the investigated tool should be cautioned, and users should consider measures to preserve aerated lung volumes.
Similar content being viewed by others
Introduction
Construction of the pulmonary pressure-volume (PV) curve has been proposed to adjust ventilator settings to a potentially less injurious ventilation strategy [1, 2]. Despite controversy over selection of the right level of positive end-expiratory pressure (PEEP) many clinicians agree on the importance of preventing end-expiratory closure of alveoli prone to atelectasis formation to prevent alveolar cycling [2, 3]. In experimental models of lung injury the setting of PEEP above the lower inflection point (LIP) lowered systemic inflammatory response [4].
Dynamic inflation and static occlusion methods have been investigated for PV curve construction. While there is no standard procedure to construct the PV curve, the maneuver can be performed either manually (supersyringe technique [5] or increasing continuous positive airway pressure levels [6]) or by customized, computer-driven ventilators [7, 8]. In this investigation we tested a “P-V tool,” a built-in module to construct a PV curve in a commercially available ventilator (Galileo Gold, Hamilton Medical, Rhäzüns, Switzerland). PV curve measurement is conventionally carried out starting at zero end-expiratory pressure (ZEEP), which has the potential for derecruitment [9, 10]. On the other hand, inflating the lung to higher transpulmonary pressures than during tidal ventilation serves as a recruitment maneuver [11]. A potential for recruitment above the LIP has been demonstrated [11, 12] if PEEP is maintained. This study investigated whether repeated generation of inflation PV curves leads to recruitment in acutely injured lungs. We furthermore investigated the effects of repeated application of the new P-V tool with a fixed algorithm on hemodynamics and oxygenation.
Methods
Subjects
The study protocol was approved by governmental Committee for Animal Use and Care and conducted according to the National Institutes of Health [13] convention. Eight female pigs (race DL, 31.3±1.9 kg) were endotracheally intubated after induction of anesthesia with ketamine and pentobarbital, followed by a continuous infusion of pentobarbital, fentanyl, and pancuronium for maintenance. Ventilation was set to volume controlled mode with 8 ml/kg tidal volume (VT), inspiratory/expiratory ratio of 1:1, PEEP of 10 cmH2O, and FIO2 1.0 (Galileo Gold). Animals were kept in supine position throughout the experiment. The respiratory rate was set to target a PaCO2 of 35–40 mmHg before induction of lung injury. In previous investigations with the same model this had resulted in PaCO2 values below 60 mmHg after induction of lung injury with only slight adoptions in ventilator settings [14, 15]. The femoral artery was cannulated for invasive pressure monitoring and the femoral vein to advance a pulmonary artery catheter (SP5107, 7.5F, Becton Dickinson, Heidelberg, Germany), which was placed under transduced pressure guidance. All animals received an initial fluid bolus of 500 ml hydroxyethyl starch 200/0.5 10% followed by a continuous infusion of Ringer’s solution at 5 ml/kg per hour.
Measurements
Cardiac output was determined by thermal dilution technique as the mean of three measurements (S5 compact monitor, Datex Ohmeda, Duisburg, Germany). Gas flow and pressure were measured between the tracheal tube and the Y-piece of the ventilator circuit by a membrane differential pressure transducer connected to the ventilator (Hamilton Medical, range −999 to +999 l/min, accuracy ±5%). VT was derived from the integrated flow signal. The static compliance of the respiratory system (CRS) was measured as described previously [16].
The relatively fixed algorithm provides an inflation pressure ramp (to be set at 2 or 3 cmH2O/s) up to a maximum pressure of 20–40 cmH2O, at which the maneuver is terminated and ventilation continued as set before. Pressure is reduced to previously set PEEP, with a total expiration time of three time constants, estimated by airway resistance and respiratory system compliance calculated from a preinflation control hub. The low flow inflation technique has been compared to static occlusion methods in terms of comparability between respiratory mechanics values obtained [7, 17]. When a low inflation flow less than 10 l/min was used, no difference was found between methods [18]. Low flow inflation generally has the advantage of not needing to disconnect the patient from the ventilator as with supersyringe method, or time-consuming multiple occlusion techniques must be used [19]. No differences have been observed whether the inflation flow is controlled by inspiratory constant flow or by pressure increase [6, 20].
Since the maneuver is started at ZEEP, the ventilator displays the PEEP-related volume obtained by switching from the preset PEEP level (VPEEP). The VPEEP theoretically corresponds to the difference between end expiratory lung volume during mechanical ventilation and the functional residual capacity (obtained through a prolonged expiration at ZEEP; referred to elsewhere as ΔEELV [21]). A mean of 4.5 s after normal expiration was allowed for complete exhalation to relaxation volume until cessation of expiratory flow, before the PV curve maneuver was started. VMAX is the end-inflation volume. The inspiratory PV curve is displayed on the ventilator, and two cursors can be moved on the graph to construct a tangent. We defined LIP as the greatest increase in upward slope, and the upper inflection point (UIP) as the greatest decrease in slope towards the upper asymptote. Graphically, the respective pressures are obtained by the intersection of a tangent through the linear middle part of the curve and the lower and upper asymptote, respectively. CMAX was defined as the maximum slope of the PV curve, and CTOT as the slope from ZEEP to maximum pressure.
Arterial, mixed venous and gaseous samples were collected simultaneously and analyzed immediately (ABL 510, Radiometer, Copenhagen, Denmark). Oxygen-saturated hemoglobin was measured with a species adjusted co-oximeter (OSM3, Radiometer). Venous admixture (QVA/Qt) was calculated according to Berggren’s formula. Expiratory gases were collected in a 10 l heated box and mixed expired PCO2 was measured for calculation of physiological dead space (VD/Vt) according to the modified Bohr equation.
Whole-lung computed tomography (CT) measurements (contiguous axial spiral CT, 4-mm slices reconstructed, window −1024 to +3074 HU; Sensation 16, Siemens, Erlangen, Germany) were taken at expiratory and inspiratory hold by pressing the respective ventilator button. Parenchyma aeration was analyzed as reported before [22, 23]. Briefly, lung outline was delineated manually along the inner pleura for every slice from apical to basal. The cross-sectional area of each slice was computed and slice volumes calculated by multiplying with slice thickness. The frequency distribution in HU was calculated in 100-HU segments for each slice and the respective gas plus tissue volumes obtained by multiplying the fraction of each with the slice volume. Lung volumes were classified hyperinflated from −1000 to −-900 HU, aerated for −900 to −500 HU, poorly aerated for −500 to −100 HU, and nonaerated for −100 to +100 HU [24, 25, 26, 27, 28, 29, 30]. The respective volumes were calculated for each slice and summed (VTOT, VHYP, VAER, VPOOR, VNON, respectively) for each scan.
Experimental protocol
Acute lung injury (ALI) was induced by repeated lung lavage [31]. ALI was considered stable after a constant PaO2/FiO2 ratio below 100 mmHg for at least 60 min. The first set of measurements were taken for hemodynamics and oxygenation parameters, followed by CT and lung mechanics.
Pressure increase in the P-V tool was set to 2 cmH2O/s and maximum pressure to 40 cmH2O, which gives a total time of 20 s for the maneuver. The maneuver was performed five times in series, and the values were recorded each time as explained. A period of 60 s was allowed between maneuvers, which is longer than the ventilator lock-out time (five ventilation cycles). Between maneuvers tidal ventilation was resumed as set before with a PEEP of 10 cmH2O (Fig. 1). Five minutes after completion of the last PV curve a second set of measurements including CT were taken.
Statistics
Values are given as mean ±SD. Before/after maneuver data were analyzed by Wilcoxon’s rank sum test. For parameters exhibiting significant changes the fractional change was calculated as Δ=(after/before)−1. Changes in PV curve parameters were analyzed by Friedman’s procedure for repeated measurements. Regression analysis was used to further characterize changes in lung volumes. Statistical significance was accepted at p<0.05 (SPSS WIN 11.01, SPSS, Chicago, Ill, USA).
Results
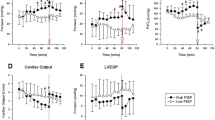
A mean of 10.2±2.3 l (maximum 16) of saline lavage was used to induce ALI, and experiments were started on average within 5.5±1.0 h after induction of anesthesia. Ventilator settings were identical before and after the maneuvers with no changes in RR, VTEX, or TiTOT, but peak inspiratory pressure increased (Table 1). No significant hemodynamic changes were observed after repeated P-V tool application. There was no change in physiological dead space, but a rise in PaCO2 (p<0.01). There was a continuous and significant reduction in VPEEP and VMAX from each PV curve construction to the next (p=0.012; Fig. 1), resulting in decreased oxygenation and increasing venous admixture (Tables 1, 2). In two animals there was a partial recovery of lost volume in the last of the repeated PV curves (Fig. 1). Since UIP was present in only one-half of the curves, it was omitted from analysis. There were no changes in LIP or CMAX and static compliance of the respiratory system. The fractional changes showed a deterioration in oxygenation and an increase in venous admixture and PCO2, indicating worsening of ventilation/perfusion mismatch (Fig. 2).
Fractional change in gas exchange parameters before and after repeated PV curve generation. Lines Median; boxes 25–75 quartile; whiskers outliers. PaO 2 Partial arterial oxygen pressure; HbO 2 oxygen saturated hemoglobin; Q VA /Q T venous admixture; PaCO 2 partial arterial carbon dioxide pressure; V D /V T physiological dead space; MIP mean inspiratory pressure *p<0.05 for before vs. after 5× PV curve generation
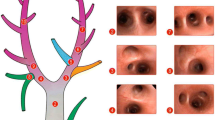
Regarding CT measurements, the loss of total lung volume after repeated PV curve generation did not reach statistical significance (p=0.089). There was a reduction in all aerated lung parenchyma (p=0.049), which was caused by a loss of VAER (p=0.049), but not by changes in VPOOR (p=0.108; Fig. 3A). Figure 4 presents the CT of one representative animal. VHYP increased significantly (p=0.013). Overall analysis of VNON showed no significant increase in atelectatic lung (p=0.056). Regression analysis of VNON revealed a significant relationship between measurements before and after. Until the point of equality (27.7% nonaerated lung of VTOT) there was an increase in VNON after repeated PV-construction, which included 81% of measurements. Animals with a greater portion of nonaerated lung were thus more likely to experience derecruitment (Fig. 5A). With VPOOR 63% of data were distributed to the right of the point of equality (22.9% of VTOT, Fig. 5B), indicating volume loss. For analysis of VAER inspiration and expiration showed different regression slopes (Fig. 5C, D), with the regression line running parallel to the bisecting line at expiration.
CT volumes before and after repeated generation of the PV curve. Volumes measured in whole-lung CT before and after 5× PV curve generation. Left Absolute volumes during expiratory hold with 10 cmH2O. Right Tidal volume calculated as difference between inspiration and expiration. V HYP Hyperinflated lung volume; V AER normally aerated lung volume; V POOR poorly aerated lung volume; V NON nonaerated lung volume
Regression of CT-derived parameters before and after repeated generation of the PV curve. All data expressed as percentage of total lung volume VTOT. Bisection line Equality of before/after values; equation regression line. A Nonaerated lung volume, intersection of regression with bisecting line at 27.7%. B Poorly aerated lung volume, intersection at 22.9%. C Normally aerated lung volume, at inspiration hold. D Normally aerated lung volume, at expiration hold
The distribution of ventilation, calculated as the difference between end-inspiratory and expiratory hold measurements, is shown in Fig. 4B. There was a trend towards increased tidal ventilation in hyperinflated and nonaerated parenchyma, which did not reach statistical significance (p=0.093). In conclusion, animals with large atelectasis and low normally aerated lung volume at the start of the experiment were less prone to further deterioration after a potential derecruitment maneuver. Changes occurred mainly in normally aerated and nonaerated parenchyma, while there were only subtle changes in poorly aerated lung volume.
Discussion
Repeated generation of an inspiratory PV curve to a maximum pressure of 40 cmH2O resulted in the loss of aerated lung volume and the increase in nonaerated volume in a model of experimental saline lavage lung injury. This happened despite of a period of 60 s between maneuvers, which was longer than the minimal lock-out time. As would be expected in volume controlled ventilation, total volumes did not change, but tidal ventilation changed to a more unfavorable distribution. This was reflected by a decrease in oxygenation and an increase in venous admixture. A corresponding loss in PEEP related volume was noted from the ventilator’s built-in measurement.
Regarding limitations of the study design, the validity of the model of repeated lung lavage for representing acute respiratory distress syndrome (ARDS) has been questioned. It seems quite impossible to include all the different possible pathophysiological conditions of the ARDS in a single model. However, in addition to atelectasis formation, the lavage model has been shown to cause lung inflammation [32], ventilation-perfusion mismatch equal to other models [33], and an increase in extravascular lung water and excess tissue [34]. Furthermore, CT has demonstrated the preferential distribution of atelectasis to the dependent lung regions in approx. one-third of ARDS patients [27]. A further limitation of the porcine model could be the special anatomy in the supine position, with a compression of the lower lobes by the abdomen and a relevant sternovertebral pressure gradient. However, this is also a common finding in different experimental models [25] and in ARDS patients [35] and might well present pathophysiological relevant conditions.
We speculated that repeated construction of the PV curve would lead to alveolar recruitment, as seen with periodically raising transpulmonary pressure to higher levels than those achieved during tidal ventilation [36, 37]. In view of the findings by Lee et al. [38] we were surprised that actually derecruitment took place. On the other hand, one might argue that repeated construction of the PV curve is not a clinical relevant issue. To our knowledge the Hamilton Galileo is the first ventilator equipped with a tool especially designed for measuring PV curves. While it is possible to perform such a maneuver on other ventilators with a graphic display (e.g., Taema Horus, Daeger Evita, Viasys Avea) by manual ventilator setting [39], users might be tempted to perform multiple measurements if the method is readily available, without necessarily being aware of the possible negative effects.
As regards lung CT morphometry, we examined real volumes of lung parenchyma with different aeration status, thus being able to identify changes in distribution of volumes rather than distribution in HU. In studying the effects of PEEP Vieira et al. [28] observed an increase in overdistended lung concomitant with alveolar recruitment and an increase in normally aerated lung. In our study distinct derecruitment caused an increase in hyperinflated lung by excluding dependent lung from ventilation, and derecruitment occurred mainly by conversion of normally aerated to non-aerated parenchyma. Some animals with severe atelectasis, however, behaved differently and showed a potential for recruitment, assuming that all recruitable units had been collapsed already at the begin of the study. Performing CT after each PV curve might have added additional information; however, performing inspiratory/expiratory hold maneuvers between these acquisitions may have affected the results.
Concerning PV curve generation, current concepts of low flow inflation to generate the pulmonary PV curve include starting the maneuver at ZEEP. Several studies have shown the detrimental effect of eliminating PEEP on atelectasis formation in the acutely injured lung [9], and obviously the technically limited maximum pressure of 40 cmH2O was not enough to recruit those alveoli collapsed after the removal of PEEP. Pelosi and coworkers [25] have demonstrated that much higher pressures are needed to effectively open up atelectatic lung regions. Also, sustained inflation is often needed, and recruitment maneuvers of 45 cmH2O for 40 s have been shown to result in improved oxygenation [11, 40]. Importantly, we observed significant volume loss even after the first maneuver, although PEEP was preserved at 10 cmH2O with baseline ventilation between maneuvers (Table 2). The safety of PV curve construction has been investigated previously [38]. PV curves were repeatedly constructed up to three times in patients with ARDS/ALI. Only a small drop in saturation was noted, and some patients even improved after PV curve generation. However, there are some major differences compared to our study. Firstly, all patients had been ventilated with ZEEP for 15 min before PV curve generation, and thus any loss of volume related to PEEP reduction would have not been detected. Secondly, several minutes of baseline ventilation was allowed between maneuvers. Thirdly, the maneuver characteristic differed, as the maximum pressure was 45 cmH2O, and a 3 s inspiratory plateau was allowed for each step, leading to a total maneuver time of 60–90 s. This may have acted as a recruitment maneuver and could reflect an advantage over constant inflation technique. We speculate that changing the maneuver characteristic to an inflation/deflation curve with an inspiratory plateau pause leads to less derecruitment and recommend this for further developments.
Conclusions
We evaluated a readily available PV tool implemented in a commercial ventilator and found the potential for derecruitment and worsening of gas exchange. The design of the investigated tool as a fixed algorithm should caution uncritical use and the lock-out time should be increased between measurements. Since the loss of lung volume was found even after the first PV curve construction, measures to preserve aerated lung volume should be considered. Further research should be undertaken to investigate whether a different maneuver characteristic would result in less adverse effects.
References
Amato MB, Barbas CS, Medeiros DM, Magaldi RB, Schettino GP, Lorenzi FG, Kairalla RA, Deheinzelin D, Munoz C, Oliveira R et al (1998) Effect of a protective-ventilation strategy on mortality in the acute respiratory distress syndrome. N Engl J Med 338:347–354
Ranieri VM, Suter PM, Tortorella C, De Tullio R, Dayer JM, Brienza A, Bruno F, Slutsky AS (1999) Effect of mechanical ventilation on inflammatory mediators in patients with acute respiratory distress syndrome: a randomized controlled trial. JAMA 282:54–61
Uhlig S (2002) Ventilation-induced lung injury and mechanotransduction: stretching it too far? Am J Physiol Lung Cell Mol Physiol 282:L892–L896
Herrera MT, Toledo C, Valladares F, Muros M, Diaz-Flores L, Flores C, Villar J (2003) Positive end-expiratory pressure modulates local and systemic inflammatory responses in a sepsis-induced lung injury model. Intensive Care Med 29:1345–1353
Janney CD (1959) Super syringe. Anesthesiology 20:709–711
Albaiceta GM, Piacentini E, Villagra A, Lopez-Aguilar J, Taboada F, Blanch L (2003) Application of continuous positive airway pressure to trace static pressure-volume curves of the respiratory system. Crit Care Med 31:2514–2519
Servillo G, Svantesson C, Beydon L, Roupie E, Brochard L, Lemaire F, Jonson B (1997) Pressure-volume curves in acute respiratory failure: automated low flow inflation versus occlusion. Am J Respir Crit Care Med 155:1629–1636
Servillo G, De Robertis E, Coppola M, Blasi F, Rossano F, Tufano R (2000) Application of a computerised method to measure static pressure volume curve in acute respiratory distress syndrome. Intensive Care Med 26:11–14
Rouby JJ, Lu Q, Goldstein I (2002) Selecting the right level of positive end-expiratory pressure in patients with acute respiratory distress syndrome. Am J Respir Crit Care Med 165:1182–1186
Richard JC, Brochard L, Vandelet P, Breton L, Maggiore SM, Jonson B, Clabault K, Leroy J, Bonmarchand G (2003) Respective effects of end-expiratory and end-inspiratory pressures on alveolar recruitment in acute lung injury. Crit Care Med 31:89–92
Richard JC, Maggiore SM, Jonson B, Mancebo J, Lemaire F, Brochard L (2001) Influence of tidal volume on alveolar recruitment. Respective role of PEEP and a recruitment maneuver. Am J Respir Crit Care Med 163:1609–1613
Jonson B, Richard JC, Straus C, Mancebo J, Lemaire F, Brochard L (1999) Pressure-volume curves and compliance in acute lung injury: evidence of recruitment above the lower inflection point. Am J Respir Crit Care Med 159:1172–1178
Drummond JC, Todd MM, Saidman LJ (1996) Use of neuromuscular blocking drugs in scientific investigations involving animal subjects. The benefit of the doubt goes to the animal. Anesthesiology 85:697–699
Henzler D, Dembinski R, Bensberg R, Hochhausen N, Rossaint R, Kuhlen R (2004) Ventilation with biphasic positive airway pressure in experimental lung injury: influence of transpulmonary pressure on gas exchange and haemodynamics. Intensive Care Med 30:935–943
Dembinski R, Max M, Bensberg R, Rossaint R, Kuhlen R (2002) Pressure support compared with controlled mechanical ventilation in experimental lung injury. Anesth Analg 94:1570–1576
D’Angelo E, Robatto FM, Calderini E, Tavola M, Bono D, Torri G, Milic-Emili J (1991) Pulmonary and chest wall mechanics in anesthetized paralyzed humans. J Appl Physiol 70:2602–2610
Ranieri VM, Giuliani R, Fiore T, Dambrosio M, Milic-Emili J (1994) Volume-pressure curve of the respiratory system predicts effects of PEEP in ARDS: “occlusion” versus “constant flow” technique. Am J Respir Crit Care Med 149:19–27
Blanc Q, Sab JM, Philit F, Langevin B, Thouret JM, Noel P, Robert D, Guerin C (2002) Inspiratory pressure-volume curves obtained using automated low constant flow inflation and automated occlusion methods in ARDS patients with a new device. Intensive Care Med 28:990–994
Sydow M, Burchardi H, Zinserling J, Ische H, Crozier TA, Weyland W (1991) Improved determination of static compliance by automated single volume steps in ventilated patients. Intensive Care Med 17:108–114
Pasero DC, Belliato M, Zanierato M, Mediani TS, Mojoli F, Franzoso B, Iotti GA, Braschi A (2002) Pressure-volume curve of the respiratory system: Linear pressure ramp vs. low constant flow method. Intensive Care Med 28[Suppl], 176
Rossi A, Gottfried SB, Higgs BD, Zocchi L, Grassino A, Milic-Emili J (1985) Respiratory mechanics in mechanically ventilated patients with respiratory failure. J Appl Physiol 58:1849–1858
Gattinoni L, Caironi P, Pelosi P, Goodman LR (2001) What has computed tomography taught us about the acute respiratory distress syndrome? Am J Respir Crit Care Med 164:1701–1711
Quintel M, Pelosi P, Caironi P, Meinhardt JP, Luecke T, Herrmann P, Taccone P, Rylander C, Valenza F, Carlesso E, Gattinoni L (2004) An increase of abdominal pressure increases pulmonary edema in oleic acid-induced lung injury. Am J Respir Crit Care Med 169:534–541
Crotti S, Mascheroni D, Caironi P, Pelosi P, Ronzoni G, Mondino M, Marini JJ, Gattinoni L (2001) Recruitment and derecruitment during acute respiratory failure: a clinical study. Am J Respir Crit Care Med 164:131–140
Pelosi P, Goldner M, McKibben A, Adams A, Eccher G, Caironi P, Losappio S, Gattinoni L, Marini JJ (2001) Recruitment and derecruitment during acute respiratory failure: an experimental study. Am J Respir Crit Care Med 164:122–130
Gattinoni L, Pelosi P, Crotti S, Valenza F (1995) Effects of positive end-expiratory pressure on regional distribution of tidal volume and recruitment in adult respiratory distress syndrome. Am J Respir Crit Care Med 151:1807–1814
Puybasset L, Cluzel P, Gusman P, Grenier P, Preteux F, Rouby JJ (2000) Regional distribution of gas and tissue in acute respiratory distress syndrome. I. Consequences for lung morphology. CT Scan ARDS Study Group. Intensive Care Med 26:857–869
Vieira SR, Puybasset L, Richecoeur J, Lu Q, Cluzel P, Gusman PB, Coriat P, Rouby JJ (1998) A lung computed tomographic assessment of positive end-expiratory pressure-induced lung overdistension. Am J Respir Crit Care Med 158:1571–1577
Lu Q, Rouby JJ (2000) Measurement of pressure-volume curves in patients on mechanical ventilation: methods and significance. Crit Care 4:91–100
Rouby JJ, Puybasset L, Nieszkowska A, Lu Q (2003) Acute respiratory distress syndrome: lessons from computed tomography of the whole lung. Crit Care Med 31:S285–S295
Lachmann B, Robertson B, Vogel J (1980) In vivo lung lavage as an experimental model of the respiratory distress syndrome. Acta Anaesthesiol Scand 24:231–236
Kaisers U, Max M, Walter J, Kuhlen R, Pappert D, Falke KJ, Rossaint R (1997) Partial liquid ventilation with small volumes of FC 3280 increases survival time in experimental ARDS. Eur Respir J 10:1955–1961
Neumann P, Hedenstierna G (2001) Ventilation-perfusion distributions in different porcine lung injury models. Acta Anaesthesiol Scand 45:78–86
Luecke T, Roth H, Herrmann P, Joachim A, Weisser G, Pelosi P, Quintel M (2003) PEEP decreases atelectasis and extravascular lung water but not lung tissue volume in surfactant-washout lung injury. Intensive Care Med 29:2026–2033
Pelosi P, D’Andrea L, Vitale G, Pesenti A, Gattinoni L (1994) Vertical gradient of regional lung inflation in adult respiratory distress syndrome. Am J Respir Crit Care Med 149:8–13
Foti G, Cereda M, Sparacino ME, De Marchi L, Villa F, Pesenti A (2000) Effects of periodic lung recruitment maneuvers on gas exchange and respiratory mechanics in mechanically ventilated acute respiratory distress syndrome (ARDS) patients. Intensive Care Med 26:501–507
Rimensberger PC, Pristine G, Mullen BM, Cox PN, Slutsky AS (1999) Lung recruitment during small tidal volume ventilation allows minimal positive end-expiratory pressure without augmenting lung injury. Crit Care Med 27:1940–1945
Lee WL, Stewart TE, MacDonald R, Lapinsky S, Banayan D, Hallett D, Mehta S (2002) Safety of pressure-volume curve measurement in acute lung injury and ARDS using a syringe technique. Chest 121:1595–1601
Lu Q, Vieira SR, Richecoeur J, Puybasset L, Kalfon P, Coriat P, Rouby JJ (1999) A simple automated method for measuring pressure-volume curves during mechanical ventilation. Am J Respir Crit Care Med 159:275–282
Grasso S, Mascia L, del Turco M, Malacarne P, Giunta F, Brochard L, Slutsky AS, Marco RV (2002) Effects of recruiting maneuvers in patients with acute respiratory distress syndrome ventilated with protective ventilatory strategy. Anesthesiology 96:795–802
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported in part by an unrestricted research grant from Hamilton Medical, Rhäzüns, Switzerland
Rights and permissions
About this article
Cite this article
Henzler, D., Mahnken, A., Dembinski, R. et al. Repeated generation of the pulmonary pressure-volume curve may lead to derecruitment in experimental lung injury. Intensive Care Med 31, 302–310 (2005). https://doi.org/10.1007/s00134-004-2512-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-004-2512-1