Abstract
Objective
To identify factors associated with in-hospital outcome of adult patients admitted to the ICU with infective endocarditis (IE).
Design and setting
Retrospective study performed in the two medical ICUs of a teaching hospital.
Patients and participants
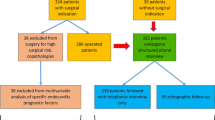
The charts of all 228 consecutive patients aged 18 years or older admitted with infective IE between January 1993 and December 2000 were reviewed. All patients satisfied the modified Duke’s criteria for definite IE.
Measurements and results
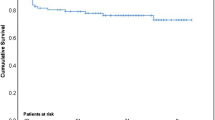
There were 146 episodes of native valve endocarditis and 82 of prosthetic valve endocarditis. Staphylococcus aureus was the predominant causative micro-organism. Most complications occurred early during the course of IE. One-half of the patients underwent cardiac surgery during the same hospitalization and had a better outcome than nonoperated patients. The overall in-hospital mortality rate was 45% (102/228). Multivariate analysis revealed the following clinical factors in patients with native valve IE as independently associated with outcome: septic shock (odds ratio 4.81), cerebral emboli (3.00), immunocompromised state (2.88), and cardiac surgery (0.475); in patients with prosthetic valve IE the factors were: septic shock (4.07), neurological complications (3.1), and immunocompromised state (3.46).
Conclusions
IE still carries high morbidity and mortality rates for the subset of patients requiring ICU admission. Most complications occur early making the decision process for optimal medical and surgical management more difficult. Surgical treatment appears to improve in-hospital outcome.


Similar content being viewed by others
References
Hoen B, Alla F, Selton-Suty C, Beguinot I, Bouvet A, Briancon S, Casalta JP, Danchin N, Delahaye F, Etienne J, Lemoing V, Leport C, Mainardi JL, Ruimy R, Vandenesch F (2002) Changing profile of infective endocarditis. Results of a 1-year survey in France. JAMA 288:75–81
Bayer AS, Bolger AF, Taubert KA, Wilson W, Steckelberg J, Karchmer AW, Levison M, Chamber HF, Dajani AS, Gewitz MH, Newburger JW, Gerber MA, Shulman ST, Pallasch TJ, Gage TW, Ferrieri P (1998) Diagnosis and management of infective endocarditis and its complications. Circulation 98:2936–2948
Mylonakis E, Calderwood SB (2001) Infective endocarditis in adults N Engl J Med 345:1318–1330
Cabell CH, Jollis JG, Peterson GE, Corey GR, Anderson DJ, Sexton DJ, Woods CW, Reller CB, Ryan T, Fowler VG Jr (2002) Changing patient characteristics and the effect on mortality in endocarditis. Arch Intern Med 162:90–94
Calderwood SB, Swinski LA, Karchmer AW, Waternaux CM, Buckley MJ (1986) Prosthetic valve endocarditis: analysis of factors affecting outcome of therapy. J Thorac Cardiovasc Surg 92:776–783
Hasbun R, Vikram HR, Barakat LA, Buenconsejo J, Quagliarello VJ (2003) Complicated left-sided native valve endocarditis in adults. Risk classification for mortality. JAMA 289:1933–1940
Karth GD, Koreny M, Binder T, Knapp S, Zauner C, Valentin A, Honninger R, Heinz G, Siostrzonek C (2002) Complicated infective endocarditis necessitating ICU admission: clinical course and prognosis. Crit Care 6:149–154
Wolff M, Witchitz S, Chastang C, Régnier B, Vachon F (1995) Prosthetic valve endocarditis in the ICU. Prognostic factors of overall survival in a series of 122 cases and consequences for treatment decision. Chest 108:688–694
Gouello JP, Asfar P, Brenet O, Kouatchet A, Berhelot G, Alquier P (2000) Nosocomial endocarditis in the intensive care unit: an analysis of 22 cases. Crit Care Med 28:377–382
Li JS, Sexton DJ, Mick N, Nettles R, Fowler VG Jr, Ryan T, Bashore T, Corey GR (2000) Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis. Clin Infect Dis 30:633–638
Le Gall JR, Lemeshow S, Saulnier F (1993) A new simplified acute physiology score (SAPS II) based on an European/North American mulicenter study. JAMA 270:2957–2963
Fagon JY, Chastre J, Novara A, Medioni P, Gibert C (1993) Characterization of intensive care unit patients using a model based on the presence or absence of organ dysfunction and/or infection: the ODIN model. Intensive Care Med 19:137–144
Fernandez-Guerrero ML, Verdejo, C Azofra J, de Gorgolas M (1995) Hospital-acquired infectious endocarditis not associated with cardiac surgery: an emerging problem. Clin Infect Dis 20:16–23
Bone RC, Sibbald WJ, Sprung CL (1992) The ACCP-SCCM consensus conference on sepsis and organ failure. Chest 101:1481–1483
Wilson WR, Karchmer AW, Dajani AS, Taubert KA, Bayer AS, Kaye D, Bisno AL, Ferrieri P, Shulman ST, Durack DT (1995) Antibiotic treatment of adults with infective endocarditis due to streptococci, enterococci, staphylococci, and HACEK microorganisms. JAMA 274:1706–1713
Pettersson G, Carbon C and the Endocarditis Working Group of the International Society of Chemotherapy (1998) Recommendations for the surgical treatment of endocarditis. Clin Microb Infect 4 [Suppl 3]:3S34–3S46
Francioli PB (1997) Complications of infective endocarditis. In: Scheld WM, Whitley RJ, Durack DT (eds) Infections of the central nervous system. Lippincott-Raven, Philadelphia, pp 523–553
Anderson DJ, Goldstein LB, Wilkinson WE, Corey GR, Cabell CH, Sanders LL, Sexton DJ (2003) Stroke location, characterization, severity, and outcome in mitral vs aortic valve endocarditis. Neurology 61:1341–1346
Heiro M, Nikoskelainen J, Engblom E, Kotilainen E, Marttila R, Kotilainen P (2000) Neurologic manifestations of infective endocarditis. A 17-year experience in a teaching hospital in Finland. Arch Intern Med 160:2781–2787
Roder BL, Wandall DA, Espersen F, Frimodt-Moller N, Skinhoj P, Rosdahl VT (1997) Neurologic manifestations in Staphylococcus aureus endocarditis: a review of 260 bacteremic cases in nondrug addicts. Am J Med 102:379–386
Steckelberg JM, Murphy JG, Ballard D, Bailley K, Tajik AJ, Taliercio CP, Guliani ER, Wilson WR (1991) Emboli in infective endocarditis: the prognostic value of echocardiography. Ann Intern Med 114:635–640
Di Salvo G, Habib G, Pergola V, Aviernos JF, Philip E, Casalta JP, Vailloud JM, Derumeaux G, Gouvernet J, Ambrosi P, Lambert M, Ferracci A, Raoult D (2001) Echocardiography predicts embolic events in infective endocarditis. J Am Coll Cardiol 37:1069–1076
Vilacosta I, Graupner C, San Roman Alberto J, Sarria C, Ronderos R, Fernandez C, Mancini L, Sanz O Sanmartin JV, Stoermann W (2002) Risk of embolization after institution of antibiotic therapy for infective endocarditis. J Am Coll Cardiol 39:1489–1495
Hecht S, Berger M (1992) Right-sided endocarditis in intravenous drug users. Prognostic features in 102 cases. Ann Intern Med 117:560–566
Akowuah EF, Davies W, Oliver S, Stephens J, Riaz I, Zadk P, Cooper G (2003) Prosthetic valve endocarditis: early and late outcome following medical or surgical treatment. Heart 89:269–272
John MD, Hibberd PL, Karchmer AW, Sleeper LA, Calderwood SB (1998) Staphylococcus aureus prosthetic valve endocarditis: optimal management and risk factors for death. Clin Infect Dis 26:1302–1309
Alexiou C, Langley SM, Stafford H, Lowes JA, Livesey SA, Monro JC (2000) Surgery for active culture-positive endocarditis: determinants of early and late outcome. Ann Thorac Surg 69:1448–1454
Tornos P, Almirante B, Mirabet S, Permanyer G, Pahissa A, Soler-Soler J (1999) Infective endocarditis due to Staphylococcus aureus. Deleterious effect of anticoagulant therapy. Arch Intern Med 159:473–475
Vickram HR, Buenconsejo J, Hasbun R, Quagliarello VJ (2003) Impact of valve surgery on 6-month mortality in adults with complicated left-sided native valve endocarditis. JAMA 290:3207–3214
Eishi K, Kawazoe K, Kuryama Y, Kitoh Y, Kawaschima Y, Omae T (1995) Surgical management of infective endocarditis associated with cerebral complications: multicenter retrospective study in Japan. J Thorac Cardiovasc Surg 110:1745–1755
Parrino PE, Kron IL, Ross SD, Shockey KS, Kron AM, Towler MA, Tribble CG (1999) Does a focal neurological deficit contraindicate operation in a patient with endocarditis? Ann Thorac Surg 67:59–64
Rubinovitch B, Pittet D (2002) Infective endocarditis: too ill to be operated? Crit Care 6:106–107
Moreillon P, Que YA (2004) Infective endocarditis. Lancet 363:139–149
Acknowledgements
We are indebted to Mrs. Janet Jacobson for assistance in the preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
Rights and permissions
About this article
Cite this article
Mourvillier, B., Trouillet, JL., Timsit, JF. et al. Infective endocarditis in the intensive care unit: clinical spectrum and prognostic factors in 228 consecutive patients. Intensive Care Med 30, 2046–2052 (2004). https://doi.org/10.1007/s00134-004-2436-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-004-2436-9