Abstract
Objective
Central venous catheter (CVC)-related infections may be caused by micro-organisms introduced from the skin surface into deeper tissue at the time of CVC insertion. The optimal disinfection regimen to avoid catheter-related infections has not yet been defined. This study compares three different approaches.
Design
Prospective randomised trial.
Setting
A tertiary care hospital.
Patients and participants
One hundred nineteen patients scheduled electively to receive 140 CVCs.
Interventions
Skin disinfection was performed with either povidone-iodine 10% (PVP-iodine), chlorhexidine 0.5%/propanol 70%, or chlorhexidine 0.5%/propanol 70% followed by PVP-iodine 10%. Prior to disinfection, a swab from the site of insertion was taken for culture. CVCs were removed if no longer needed or infection was suspected. All catheters were cultured quantitatively after removal.
Measurement and results
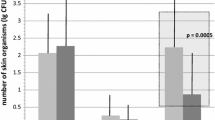
Bacteria could be isolated from 20.7% of the catheter tips. Bacterial growth was found in 30.8% of the catheters placed after skin disinfection with povidone-iodine, in 24.4% after disinfection with propanol/chlorhexidine and in 4.7% after disinfection with propanol/chlorhexidine followed by povidone-iodine (p=0.006). In 15 cases, the same organism was isolated from the skin swab and the catheter tip. Ten of these paired isolates showed the same pattern in a pulsed-field gel electrophoresis analysis.
Conclusions
Skin disinfection with propanol/chlorhexidine followed by PVP-iodine was superior in the prevention of microbial CVC colonisation compared to either of the regimens alone. These results support the concept that catheter infections can originate from bacterial translocation at the time of catheter insertion.


Similar content being viewed by others
References
Pearson ML (1996) Guidelines for prevention of intravascular device-related infections. Part I: Intravascular device-related infections: an overview. Infection control Practices Advisory committee. Am J Infect Control 24:262–277
Grady NP, Alexander M, Dellinger EP, Gerberding JL, Heard SO, Maki DG, Masur H, McCormick RD, Mermel LA, Pearson ML, Raad II, Randolph A, Weinstein RA (2002) Guidelines for prevention of intravascular catheter-related infections. Healthcare infection control practices advisory committee. MMWR 51/RR-10:1–32
Maki DG, Stolz SM, Wheeler S, Mermel LA (1997) Prevention of central venous catheter related infections by use of an antiseptic impregnated catheter. A randomized controlled study. Ann Intern Med 127:257–266
Raad I, Darouiche R, Dupuis J, Abi-Said D, Gabrielli A, Hachem R, Wall M, Harris R, Jones J, Buzaid A, Robertson C, Shenaq S, Curling P, Burke T, Ericsson C (1997) Central venous catheters coated with minocyclin and rifampin for the prevention of catheter-related colonization and bloodstream infections: a randomized double-blind trial. Ann Intern Med 127:267–274
Arnow PM, Quimosing EM, Brech M (1993) Consequences of intravascular catheter sepsis. Clin Infect Dis 16:778–784
Pittet D, Tarara D, Wenzel RP (1994) Nosocomial bloodstream infection in critically ill patients: excess length of stay, extra costs and attributable mortality. JAMA 271:1598–1601
Smith RL. Meixler SM, Simberkoff MS (1991) Excess mortality in critically ill patients with nosocomial bloodstream infections. Chest 100:164–167
Renaud B, Brun-Buisson C, for the ICU-Bacteremia Study Group (2001) Outcomes of primary and catheter-related bacteremia. A cohort and case-control study in critically ill patients. Am J Respir Crit Care Med 163:1584–1590
Rello J, Ochagavia A, Sabanes E, Roque M, Mariscal D, Reynaga E, Valles J (2000) Evaluation of outcome of intravenous catheter-related infections in critically ill patients. Am J Respir Crit Care Med 162:1027–1030
Pearson ML (1996) Guidelines for prevention of intravascular device-related infections. Part II: Recommendations for the prevention of nosocomial intravascular device-related infections. Infection control practices advisory committee. Am J Infect Control 24:277–293
Lacour M, Gastmeier P, Rüden H, Daschner F (1998) Prävention von Infektionen durch intravasale Katheter. Intensivmed 35:585–592
Safdar N, Kluger DM, Maki DG (2002) A review of risk factors for catheter-related bloodstream infection caused by percutaneously inserted, noncuffed central venous catheters: implications for preventive strategies. Medicine (Baltimore) 81:466–479
Elliott TSJ, Moss HA, Tebbs SE, Wilson IC, Bonser RS, Graham TR, Burke LP, Faroqui MH (1997) Novel approach to investigate a source of microbial contamination of central venous catheters. Eur J Clin Microbiol Infect Dis 16:210–213
Livesley MA, Tebbs SE, Moss HA, Faroqui MH, Lambert PA, Elliott TSJ (1998) Use of pulse field gel electrophoresis to determine the source of microbial contamination of central venous catheters. Eur J Clin Microbiol Infect Dis 17:108–112
Maki DG, Ringer M, Alvarado CJ (1991) Prospective randomised trial of povodine-iodine, alcohol and chlorhexidine for prevention of infection associated with central venous and arterial catheters. Lancet 338:339–343
Mimoz O, Pieroni L, Lawrence C, Edouard A, Costa Y, Samii K, Brun-Buisson C (1996) Prospective, randomized trial of two antiseptic solutions for prevention of central venous or arterial catheter colonization and infection in intensive care unit patients. Crit Care Med 24:1818–1823
Maki DG, Weise CE, Sarafin HW (1977) A semiquantitative culture method for identifying intravenous-catheter-related infection. N Engl J Med 296:1305–1309
Tenover F, Arbeit RD, Goering PA, Mickelsen PA, Murray BE, Persing DH, Swaminathan B (1995) Interpreting chromosomal DANN restriction patterns produced by pulsed-field gel electrophoresis: criteria for bacterial stain typing. J Clin Microbiol 33:2233–2239
Gautom RK (1997) Rapid pulsed-field gel electrophoresis protocol for typing of Escherichia coli O157:H7 and other gram-negative organisms in 1 day. J Clin Microbiol 35:2977–2980
Morrison D, Woodford N, Barrett SP, Sisson P, Cookson BD (1999) DNA banding pattern polymorphism in vancomycin-resistant Enterococcus faecium and criteria for defining strains. J Clin Microbiol 37:1084–1091
Turabelidze D, Kotetishvili M, Kreger J, Morris G, Sulakvelidze (2000) Improved pulsed-field gel electrophoresis for typing vancomycin-resistant enterococci. J Clin Microbiol 38:4242–4245
Sloos JH, Dijkshoorn L, Vogel L, van Boven CP (2000) Performance of phenotypic and genotypic methods to determine the clinical relevance of serial blood isolates of Staphylococcus epidermidis in patients with septicemia. J Clin Microbiol 38:2488–2493
Garland JS, Buck RK, Maloney P, Durkin DM, Toth-Lloyd S, Duffy M, Szocik P, McAuliffe TL, Goldmann D (1995) Comparison of 10% povidone-iodine and 0.5% chlorhexidine gluconate for the prevention of peripheral intravenous catheter colonization in neonates: a prospective trial. Pediatr Infect Dis J 14:510–516
Humar A, Ostromecki A, Direnfeld J, Marshall JC, Lazar N, Houston PC, Boiteau P, Conly JM (2000) Prospective randomized trial of 10% povidone-iodine versus 0.5% tincture of chlorhexidine as cutaneous antisepsis for prevention of central venous catheter infection. Clin Inf Dis 31:1001–1007
Mimoz O, Karim A, Mercat A, Cosseron M, Falissard B, Parker F, Richard C, Samii K, Nordmann P (1999) Chlorhexidine compared with povidone-iodine as skin preparation before blood culture. A randomized controlled trial. Ann Intern Med 121:834–837
Chaiyakunapruk N, Veenstra DL, Lipsky BA, Saint S (2002) Chlorhexidine compared with povidone-iodine solution for vascular catheter-site care: a meta-analysis. Ann Intern Med 136:792–801
Goldblum SE, Ulrich JA, Goldman RS, Reed WP, Avasthi PS (1983) Comparison of 4% chlorhexidine gluconate in a detergent base (Hibiclens) and povidone-iodine (Betadine) for the skin preparation of hemodialysis patients and personnel. Am J Kidney Dis 2:548–552
May SR, Roberts DP, DeClement FA, Still JM (1991) Reduced bacteria on transplantable allograft skin after preparation with chlorhexidine gluconate, povidone-iodine and isopropanol. J Burn Care Rehabil 12:224–228
Corona ML, Peters SG, Narr BJ, Thompson RL (1190) Infections related to central venous catheters. Mayo Clin Proc 65:979–986
Linares J, Dominguez MA, Martin R (1997) Current laboratory techniques in the diagnosis of catheter-related infections. Nutrition 13:10S–14S
Gebler H (1998) Tabellen für die pharmazeutische Praxis. Govi, Eschborn p 426
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Langgartner, J., Linde, HJ., Lehn, N. et al. Combined skin disinfection with chlorhexidine/propanol and aqueous povidone-iodine reduces bacterial colonisation of central venous catheters. Intensive Care Med 30, 1081–1088 (2004). https://doi.org/10.1007/s00134-004-2282-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-004-2282-9