Abstract
Objective
Measurement of functional residual capacity (FRC) during mechanical ventilation is important to standardise respiratory system compliance and adjust the ventilator settings to optimise lung recruitment. In the present study we compared three methods to measure FRC.
Design
The bias flow nitrogen washout technique (FRCN2MC), the multiple breath nitrogen washout (FRCMBNW) and the multiple breath sulphur-hexafluoride washout using the molar mass signal of an ultrasonic flow meter (FRCMBSF6) were compared in six adult monkeys after endotracheal intubation and during spontaneous breathing and mechanical ventilation at three different positive end-expiratory pressure (PEEP) levels of 0, 5 and 10 cmH2O.
Setting
Animal research laboratory.
Results
We found good agreement between all three methods and they all accurately measured changes in FRC when PEEP was increased. The coefficients of variance of the three measurement techniques were in the same range (1.3–9.2%).
Conclusion
The measurement of the tracer gas concentration with the molar mass signal of the ultrasonic flow meter provides a good and simple alternative to respiratory mass spectrometer for FRC measurements in ventilated subjects.
Similar content being viewed by others
Introduction
Functional residual capacity (FRC) is an important lung volume without which lung mechanics such as dynamic lung compliance and resistance are difficult to interpret during mechanical ventilation [1]. The empirical titration of positive end-expiratory pressure (PEEP) to optimise lung volume and, hence, lung recruitment in diseased lungs is usually based only on clinical judgement such as blood gas analysis, chest expansion on X-ray and the interpretation of pressure-volume loops [2].
There are several techniques available to measure FRC in mechanically ventilated patients: the closed-circuit helium dilution technique, the open-circuit nitrogen washout or the open-circuit sulphur-hexafluoride (SF6) wash-in/washout. The helium dilution technique is very cumbersome and sensitive to leaks in the ventilatory system [3]. Nitrogen washout techniques can be divided into bias flow and breath-by-breath washout systems. The bias flow nitrogen washout method uses a mixing chamber (MCN2), whereas the multiple breath nitrogen washout (MBNW) technique measures the instantaneous nitrogen concentration and air flow during each breath at the airway opening. MCN2 allows very accurate measurement of FRC [4] but is limited to patients at FiO2 less than 0.7 since, for accurate volume measurement, the technique requires a change in the tracer gas (N2) of more than 0.3 [5]. Recently, newer techniques using sulphur hexafluoride (SF6) as a tracer gas have been developed [6, 7, 8, 9]. SF6 is an inert gas which is fed into the inspiratory limb of the ventilator circuit. The concentration of SF6 is measured breath-by-breath using a respiratory mass spectrometer [10] or an infrared analyser [8], the former having a high, and the latter having a low, signal-to-noise ratio. Alternatively, the SF6 concentration can be measured by the molar mass signal (MM) of an ultrasonic flowmeter at the same time as flow (and hence volume) is recorded. The molar mass method has been shown to be highly accurate and reproducible in a mechanical lung model [11] and sensitive to changes in FRC secondary to alterations of positive end-expiratory pressure (PEEP) in ventilated rabbits [6] and in spontaneously breathing healthy infants [7].
The aim of the study was to compare the molar mass method (FRCMM) with the bias flow nitrogen washout technique using a mixing chamber (FRCMCN2) and also with the multiple breath nitrogen washout (FRCMBNW) in mechanically ventilated adult rhesus monkeys.
Methods
Subjects
Six adult rhesus monkey with a mean body weight of 10.9±2.7 kg were studied. Analgesia for intubation was achieved intramuscularly with ketamine (40 mg/kg) and for the duration of the experiment anaesthesia was maintained with intravenous infusion of thiopentone sodium (8.0 mg/kg per h). After oral intubation of the trachea, the cuff was inflated sufficiently to prevent any air leak detectable by auscultation when the lungs were inflated to +40 cmH2O pressure. The animals breathed spontaneously for the first set of experiments and were mechanically ventilated at modest settings to keep the PETCO2 in the 35–40 mmHg range in the second set. The animals were placed supine. Heart rate was monitored with a three-lead continual electrocardiogram (Sirecust Model 1281, Siemens, Erlangen, Germany) and transcutaneous haemoglobin saturation (SpO2) was obtained with pulse oximetry (Nellcor Type B, Hayward, CA). Animals were maintained in an in-house colony at Novartis, Basel, Switzerland, under the full-time care of an experienced primate veterinarian and his staff. All experimental protocols conformed to international standards of animal welfare and were approved and periodically reviewed by the Kantonale Tierversuchs-Kommission von Basel-Stadt und Baselland, Switzerland.
Equipment
The experimental set-up is shown in Fig. 1. Two ventilators of the same manufacturer with the same settings were used during the measurements (Hamilton Medical, Rhäzuns, CH). In order to perform the nitrogen washout, a sliding valve triggered by a computer was used to switch the monkeys from the first ventilator (FiO2 =0.21) to the second (washout) ventilator (FiO2 =0.95, FiSF6 =0.05) at the end of the last expiration before the washout. An ultrasonic flowmeter (Spiroson, Ecomedics, Dürnten, Switzerland) was directly connected to the endotracheal tube without any airway filter and was maintained in situ for the whole experiment. The same flow sensor was used for N2 and SF6 washout. The flow meter has a flow range of ±1500 ml/s and a dead space of 3.5 ml. FRC of the nitrogen-washout (FRCMCN2 and FRCMBNW) was calculated using the nitrogen signal of a respiratory mass spectrometer (MGA 3000, Morgan Medical, Biggin Hill, UK). FRCMCN2 was determined by the mixing chamber nitrogen washout technique [4, 5] utilising a computer-based data acquisition system (2600, SensorMedics Anaheim, CA). The N2 signal for FRCMBNW was acquired with the integrated AD-board of the Spiroson unit. Exhaled nitrogen volume was calculated by integrating the measured flow and by multiplying the instantaneous nitrogen fraction with the corresponding exhaled volume. FRCMBNW was then obtained by dividing this exhaled nitrogen volume with the nitrogen concentration of the breathing gas prior to the washout. Corrections were made for changes in gas viscosity and delay time of the mass spectrometry signal [10, 12]. Dedicated software written in LabView 5.0 was used for analysis. Equipment dead space was subtracted for all FRC measurements techniques.
Principles of ultrasonic flow meter
Flow and molar mass of the inhaled and exhaled gas were measured with the ultrasonic flow meter [13]. Technique and mathematical models for ultrasonic flow and gas density measurement have been described previously [6, 7, 13] and are available as electronic supplementary material.
In the present study we used 5% SF6 and 95% oxygen as the washout gas rather than 100% oxygen, because 5% SF6 results in a greater change of molar mass than using pure oxygen alone (changes in molar mass are 7.3 and 3.15 g/mol, respectively), and the gas mixture has a higher signal-to-noise ratio. Using the MM, the difference between the instantaneous inspiratory SF6-O2 fraction and the SF6-O2 fraction at the end of the wash-in was obtained and the SF6-O2 flow was calculated as the product of instantaneous airflow and the difference. The SF6-O2 flow was then integrated over time to give the inspired SF6-O2 volume. The FRC of the SF6-O2 wash-in was obtained by dividing the measured inspired SF6-O2 volume with the end tidal SF6-O2 concentration of the SF6-O2 at the end of the wash-in.
All signal data were acquired at a sampling rate of 200 Hz. Analysis of the data was done offline using adapted software.
Measurement protocol
Two different sets of measurements were performed. (1) in six rhesus monkeys, three measurements each of FRCMCN2, FRCMBNW and FRCMM were measured during spontaneous breathing via the endotracheal tube. (2) After starting mechanical ventilation, FRCMCN2, FRCMBNW and FRCMM were measured in six monkeys at three different levels of positive end-expiratory pressure (0 cmH2O,5 cmH2O and at 10 cmH2O). The measurements were repeated at least three times at each level. The nitrogen signal of the respiratory mass spectrometer could only be used either for FRCMCN2 or FRCMBNW and, therefore, only one of each could be compared to FRCMM simultaneously.
Statistics
Values are presented as means ± SD. Reproducibility of the methods was evaluated by calculating the coefficient of variation. The accuracy of the measurements (limits of agreement) between the different FRC measurement methods were assessed with the difference of the measured volumes plotted against their mean [14]. Because of the relatively small sample size in each group a Wilcoxon signed rank test was used to compare paired FRC values at different PEEP levels. A p value of less than 0.05 was considered significant.
Results
Three measurements in each of the six monkeys were performed during spontaneous breathing via the endotracheal tube and FRCMCN2 and FRCMM were calculated (Table 1). FRCMM was statistically significantly lower than FRCMCN2 but the measured difference of 7 ml (less than 5%) is clinically not relevant. In Table 1 all measured FRCMCN2 and FRCMM during mechanical ventilation at 0, 5 and 10 cmH2O PEEP are given. Some of these measured FRC values were significantly different, but again the differences are clinically not relevant (<5%).
Figure 2 displays, in the upper panel, the relationship between all FRCMCN2 and FRCMM (measured during spontaneous breathing and mechanical ventilation) and, in the lower panel, the mean difference of the two measurements against their mean. The mean offset of all measured FRCMCN2 and FRCMM was −4.3±24.4 ml (p=0.3). FRCMBNW measured during spontaneous breathing was equal to FRCMM (Table 2). Table 2 lists all measured FRCMBNW and FRCMM at 0, 5 and 10 cmH2O PEEP.
Figure 3 displays, in the upper panel, all measured FRCMBNW and FRCMM (measured during spontaneous breathing and mechanical ventilation) and, in the lower panel, the mean difference of FRCMBNW and FRCMM against their mean. The mean offset of all measured FRCMBNW and FRCMM was 10.0±14.8 ml (p<0.01).
Discussion
The concentration of an inert gas such as SF6 can be estimated from the molar mass signal (MM) of an ultrasonic flow meter and, thus, FRC can be calculated during an inert gas wash-in or washout. In the present study we demonstrated that, in mechanically ventilated monkeys, the inert gas wash-in technique using the MM is not significantly different to the “gold standard”, the nitrogen washout technique using a mixing chamber [4] or the multiple breath nitrogen washout technique [12, 15]. All three methods have similar intra-individual variations and detect changes of FRC accurately when PEEP is changed from 0 to 5 and 10 cmH2O.
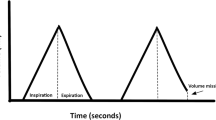
All three methods have their limitations. The mixing chamber bias flow technique is highly accurate [4, 5] and well established to measure lung volumes [16], but needs bulky equipment and is limited to subjects with an oxygen requirement of FiO2 less than 0.7. FRC is calculated from the area under the curve of the nitrogen signal measured with a respiratory mass spectrometer sampling from the output of a mixing chamber. The nitrogen signal has a pyramidal shape with a slightly prolonged tail at the end of the washout. In the case of severe maldistribution of ventilation, this tail becomes more prolonged and the signal-to-noise ratio is low, which leads to difficulties in calculating FRC accurately.
The multiple breath nitrogen washout technique during mechanical ventilation needs two ventilators and is therefore, like the mixing chamber technique, not suitable for daily routine bedside FRC measurement. The nitrogen concentration is measured at the airway opening and can be displayed breath-by-breath on the computer screen. The nitrogen signal of the respiratory mass spectrometer has a variable delay time to the flow signal. Therefore the flow and nitrogen signals need to be aligned carefully [10, 12, 15]. Pressure changes within the ventilator circuit considerably shorten or prolong the delay time of the nitrogen signal, which makes good alignment of the nitrogen and the flow signals difficult. Any nitrogen washout technique using oxygen as a washout gas has the potential disadvantage that the washout gas participates in gas exchange. This effect is negligible in healthy subjects and during positive pressure ventilation, but in spontaneously breathing infants it has been shown that pure oxygen rebreathing changes breathing pattern and creates atelectasis [15].
With the ultrasonic flow meter a new method is introduced to measure flow, volume and gas concentration all in one sensor. In previous studies we have shown that the tracer gas (SF6) can be fed into the circuit of the ventilator through a side port and thus only one ventilator is necessary for FRC measurement [6, 7, 8, 9]. In the present study, however, we used an experimental set-up with two ventilators in order to compare simultaneously the nitrogen washout and the molar mass technique. FRCMM measurements were on average slightly higher than FRCMCN2 or FRCMBNW, but these differences are clinically not relevant and may be partly explained by the fact that SF6 does not interfere with gas exchange. The reproducibility of all three methods were within the same range.
The user of the ultrasonic flow meter has to be aware of several important methodological issues. The ultrasonic flow meter has a low dead space (3.5 ml) and provides an all-in-one sensor for the flow and gas concentration (by molar mass) measurements. In order to compute the molar mass, the temperature along the sound transmission path is computed using a combination of a mathematical model and temperature measurements. If the measurements are performed during mechanical ventilation using humidified and heated air (BTPS conditions), the corrections of the MM are negligible. However, if measured under ATPS conditions (e.g. as with spontaneous breathing in room air) the temperature corrections have considerable effects on flow measurements. The MM needs to be further corrected for the wash-in/washout process occurring in the two side chambers. A step-response function assuming exponential gas mixing in the side chamber was used. This correction depends on the length of the diffusion path within the side chamber and the effusion constant α of the tracer gas.
In ventilated patients, the molar mass of the inhaled and exhaled gas is not constant. The molar mass of exhaled CO2 is 36 g/mol, of oxygen 32 g/mol and of nitrogen 28 g/mol. The effusion constants of these gases are different. We therefore calculated the FRC based on the change of molar mass (delta MM) in respect to the baseline value prior to the SF6 wash-in/washout and not in absolute terms. Using the delta MM, an almost perfect matching can be obtained if the MM is superimposed onto the SF6 signal of the respiratory mass spectrometer (Fig. 4). The ultrasonic flow meter has not been validated under more extreme conditions such as rapid changes in breathing pattern, high respiratory rate and high ventilation pressures. In a previous work [6] we showed that the molar mass, but not the flow signal, of the ultrasonic flowmeter is pressure sensitive. Using delta MM, however, the effect of pressure changes on the MM is eliminated. The ultrasonic measurement technique presented has only been validated in a small volume range of 50–650 ml and therefore cannot been directly generalised to adult humans with lung disease.
The respiratory mass spectrometer signal measuring the SF6 concentration is superimposed on the molar mass signal. Both signals were measured simultaneously. The black signal represents the molar mass signal, which has been converted to % concentration, the grey signal is the SF6 signal of the respiratory mass spectrometer
In conclusion, we have demonstrated that lung volumes (FRC) can be accurately measured with an ultrasonic flow meter if compared to standard methods such as the bias flow nitrogen washout using a mixing chamber or the multiple breath nitrogen washout. The ultrasonic flowmeter may be a clinically very helpful tool to adjust PEEP for optimal ventilation at normal FRC levels and may be valuable for more precise interpretation of pressure-volume loops. The equipment to measure FRC with the ultrasonic flow meter is simple, it requires only a small laptop computer, the switching valve and a small cylinder containing pure SF6. In addition, breath-by-breath systems provide the potential advantage of assessing gas distribution and ventilatory efficiency [6, 7, 9, 15] that cannot be measured by the bias flow washout systems.
References
Sivan Y, Deakers TW, Newth CJL (1991) Effect of positive end-expiratory pressure on respiratory compliance in children with acute respiratory failure. Pediatr Pulmonol 11:103–107
Rimensberger PC, Bryan AC (1999) Measurement of functional residual capacity in the critically ill. Relevance for the assessment of respiratory mechanics during mechanical ventilation. Intensive Care Med 25:540–542
Tepper RS, Merth IT, Newth CJL, Gerhart T (1996) Measurement of functional residual capacity in infants by helium and nitrogen washout techniques. In: Stocks J, Sly PD, Tepper RS, Morgan WJ (eds) Infant respiratory function testing. Wiley, New York, pp 165–189
Sivan Y, Deakers TW, Newth CJL (1990) An automated bedside method for measuring functional residual capacity by N2 washout in mechanically ventilated children. Pediatr Res 28:446–450
Sivan Y, Deakers TW, Newth CJL (1990) Functional residual capacity in ventilated infants and children. Pediatr Res 28:451–454
Schibler A, Henning R (2001) Measurement of functional residual capacity in rabbits and children using an ultrasonic flow meter. Pediatr Res 49:581–588
Schibler A, Henning R (2002) Positive end-expiratory pressure and ventilation inhomogeneity in mechanically ventilated children. Pediatr Crit Care Med 3:124–128
Schüller A, Schaller P. Topfer A, Kirplani H (1994) Measurement of functional residual capacity by sulfur hexafluoride in small-volume lungs during spontaneous breathing and mechanical ventilation. Pediatr Res 35:494–499
Vilstrup CT, Björkulund J, Larsson A, Lachmann B, Werner O (1992) Functional residual capacity and ventilation inhomogeneity in mechanically ventilated small neonates. J Appl Physiol 73 (1):276–283
Brunner JX, Wolff G, Cumming G, Langenstein H (1985) Accurate measurement of N2-volumes during N2 washout requires dynamic adjustment of delay time. J Appl Physiol 59 (3):1008–1012
Wauer J, Leier TU, Henschen M, Wauer RR, Schmalisch G (2003) In vitro validation of an ultrasonic flowmeter in order to measure the functional residual capacity in newborns. Physiol Meas 24(2):355–365
Wrigge H, Sydow M, Zinserling J, Neumann P, Hinz J, Buchardi H (1998) Determination of functional residual capacity (FRC) by multibreath nitrogen washout in a lung model and in mechanically ventilated patients. Intensive Care Med 24:487–493
Buess C, Burger R, Guggenbühl W (1991) Ultrasonic respiration analysis. IEEE 1597–1598
Altman DG, Bland JM (1983) Measurement in medicine: the analysis of method comparison studies. Statistician 32:307–317
Schibler A, Schneider M, Frey U, Kraemer R (2000) Moment ratio analysis of multiple breath nitrogen washout in infants with lung disease. Eur Respir J 15:1094–1101
Hammer J, Numa A, Newth CJL (1998) Total lung capacity by N2 washout from high and low lung volumes in ventilated infants and children. Am J Respir Crit Care Med 158:526–531
Acknowledgements
Our gratitude to Novartis and Dr. John Fozard for permission to do the studies in their facility, and for providing the animals. Particular thanks to Dr. Lazzaro Mazzoni and Mr. Heinz Büscher for their technical and organisational assistance. Also, thanks to Hamilton Medical Company, Rhäzüns, Switzerland for providing the ventilators and associated equipment.
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
Rights and permissions
About this article
Cite this article
Schibler, A., Hammer, J., Isler, R. et al. Measurement of lung volume in mechanically ventilated monkeys with an ultrasonic flow meter and the nitrogen washout method. Intensive Care Med 30, 127–132 (2004). https://doi.org/10.1007/s00134-003-2028-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-003-2028-0