Abstract
Objective. To determine if the rapid waveform profile of the activated partial thromboplastin time (aPTT) assay, which detects lipoprotein-complexed C reactive protein (LCCRP) formation, predicts sepsis and mortality in critically ill patients.
Design. Observational, cohort study.
Setting. General intensive therapy unit (ITU) of a tertiary care hospital.
Patients and participants. A total of 1187 consecutive patients admitted to the ITU.
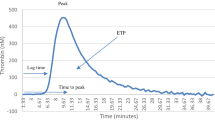
Intervention. Activated partial thromboplastin time transmittance waveform analysis was performed within the first hour of admission to the ITU. The degree of change causing a biphasic waveform was quantified through the drop in light transmittance level.
Measurements and results. Three hundred forty-six patients had a biphasic waveform on admission to the ITU with a mortality rate of 44% compared with 26% for those with normal waveforms. Logistic regression models showed direct correlation between the likelihood for sepsis and in-patient mortality with increasing waveform abnormalities. The mortality fraction was 0.3 with normal waveforms versus 0.6 when the light transmittance decreased by 30%. The odds ratio (OR) for mortality and sepsis were 4.5 and 11, respectively, from the most abnormal to normal aPTT waveforms. These were comparable with APACHE II scores and superior to those estimated by CRP for mortality (OR 2.3) / sepsis (OR 6.4) prediction.
Conclusion. Waveform analysis within the first hour of ITU admission is a single, simple and rapid method of identifying the risks of mortality and sepsis. Its measure of LCCRP formation shows superior prediction over CRP alone and it warrants further assessment as a tool to triage and target prompt, appropriate treatment in the ITU.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Electronic Publication
Rights and permissions
About this article
Cite this article
Toh, C., Ticknor, L.O., Downey, C. et al. Early identification of sepsis and mortality risks through simple, rapid clot-waveform analysis. Intensive Care Med 29, 55–61 (2003). https://doi.org/10.1007/s00134-002-1557-2
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00134-002-1557-2