Abstract
Objective
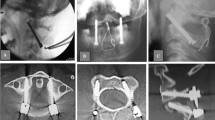
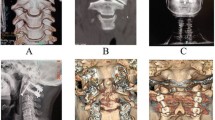
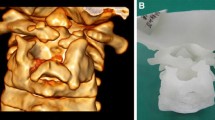
The purpose of this work is to evaluate the outcome of the transoral atlantoaxial pedicle screw technique for the treatment of irreducible atlantoaxial dislocation (IAAD).
Patients and methods
A total of 10 patients with IAAD were treated using the transoral atlantoaxial pedicle screw technique. We compared preoperative and postoperative JOA (Japanese Orthopedic Association) scores and observed bone graft fusion rate of the atlantoaxial joint, and examined whether our technique was suitable for the treatment of IAAD.
Results
The mean preoperative and postoperative JOA scores (9.2 ± 0.63 and 12.9 ± 0.73, respectively) were significantly different (P < 0.05). The atlantoaxial rigid bony fusion rate was 100 % in 10 cases. All cases were followed up for an average of 5.1 years (range 3.5–6 years).
Conclusion
The transoral atlantoaxial screw reconstruction plate technique is a novel surgical technique for the treatment of IAAD in upper cervical diseases.
Zusammenfassung
Ziel
Evaluiert werden soll das Outcome nach Therapie einer irreduziblen atlantoaxialen Dislokation (IAAD) mittels transoraler atlantoaxialer Pedikelverschraubung.
Patienten und Methoden
Insgesamt 10 Patienten mit IAAD wurden mit transoral eingebrachten atlantoaxialen Pedikelschrauben behandelt. Wir verglichen prä- und postoperative JOA(Japanese Orthopedic Association)-Scores, beobachteten die Fusionsrate beim Knochengraft am Atlantoaxialgelenk und überprüften die Eignung der verwendeten Methode für die Behandlung einer IAAD.
Ergebnisse
Die Unterschiede zwischen den durchschnittlichen prä- und postoperativen JAO-Scores (9,2 ± 0,63 bzw. 12,9 ± 0,73) waren statistisch signifikant. Die rigide atlantoaxiale knöcherne Fusionsrate betrug 100 % in allen 10 Fällen. Im Durchschnitt lag die Follow-up-Zeit bei 5,1 (3,5–6) Jahren.
Schlussfolgerung
Die Methode der atlantoaxialen Schrauben-Platte-Rekonstruktion mit transoralem Zugang ist eine neue chirurgische Methode zur Behandlung der IAAD bei Erkrankungen der oberen Halswirbelsäule.






Similar content being viewed by others
References
Dean CL, Lee MJ, Robbin M, Cassinelli EH (2009) Correlation between computed tomography measurements and direct anatomic measurements of the axis for consideration of C2 laminar screw placement. Spine J 9:258–262
Jeon SW, Jeong JH, Choi GH, Moon SM, Hwang HS, Choi SK (2012) Clinical outcome of posterior fixation of the C1 lateral mass and C2 pedicle by polyaxial screw and rod. Clin Neurol Neurosurg 114(6):539–544
Yin Q, Ai F, Zhang K, Chang Y, Xia H, Wu Z, Quan R, Mai X, Liu J (2005) Irreducible anterior atlantoaxial dislocation: one-stage treatment with a transoral atlantoaxialreduction plate fixation and fusion. Report of 5 cases and review of the literature. Spine (Phila Pa 1976) 30(13):E375–E381
Yin YH, Qiao GY, Yu XG et al (2013) Posterior realignment of irreducible atlantoaxial dislocation with C1-C2 screw and rod system: a technique of direct reduction and fixation. Spine J 13(12):1864–1871
Wang S, Wang C, Yan M, Zhou H, Dang G (2013) Novel surgical classification and treatment strategy for atlantoaxial dislocations. Spine (Phila Pa 1976) 38(21):E1348–E1356
Wu ZH, Zheng Y, Yin QS, Ma XY, Yin YH (2014) Anterior pedicle screw fixation of C2: an anatomic analysis of axis morphology and simulated surgical fixation. Eur Spine J 23(2):356–361
Yin QS, Ai FZ, Zhang K, Mai XH, Xia H, Wu ZH (2010) Transoral atlantoaxial reduction plate internal fixation for the treatment of irreducible atlantoaxial dislocation: a 2- to 4- year follow-up. Orthop Surg 2(2):149–155
Chandra PS, Kumar A, Chauhan A et al (2013) Distraction, compression, and extension reduction of basilar invagination and atlantoaxial dislocation: a novel pilot technique. Neurosurgery 72(6):1040–1053
Liu T, Li F, Xiong W, Du X et al (2010) Video-assisted anterior transcervical approach for the reduction of irreducible atlantoaxialdislocation. Spine (Phila Pa 1976) 35(15):1495–1501
Xu R, Bydon M, Macki M et al (2014) Biomechanical impact of C2 pedicle screw length in an atlantoaxial fusion construct. Surg Neurol Int 5(Suppl 7):S343–S346
Liu GY, Mao L, XU RM et al (2014) Biomechanical comparison of pedicle screws versus spinous process screws in C2 vertebra. Indian J Orthop 48(6):550–554
Yadav YR, Madhariya SN, Parihar VS, Namdev H, Bhatele PR (2013) Endoscopic transoral excision of odontoid process in irreducible atlantoaxial dislocation: our experience of 34 patients. J Neurol Surg A Cent Eur Neurosurg 74(3):162–167
Yang J, Ma X, Xia H, Wu Z, Ai F, Yin Q (2014) Transoral anterior revision surgeries for basilar invagination with irreducible atlantoaxialdislocation after posterior decompression: a retrospective study of 30 cases. Eur Spine J 23(5):1099–1108
Ai FZ, Yin QS, Wang ZY, Xia H, Chang YB, Wu ZH, Liu JF (2006) The anatomical study of transoral atlantoaxial reduction plate internal fixation. Chin J Traumatol 9(1):8–13
Syre P III, Rodriguez-Cruz L, Desai R, Geeene KA, Hurst R, Schuster J, Malhotra NR, Marcotte P (2013) Civilian gunshot wounds to the atlantoaxial spine: a report of 10 cases treated using a multidisciplinary approach. J Neurosurg Spine 19(6):759–766
Xia H, Yin Q, Ai F, Ma X, Wang J, Wu Z, Zhang K, Liu J, Xu J (2014) Treatment of basilar invagination with atlantoaxial dislocation: atlantoaxial joint distraction and fixation with transoral atlantoaxial reduction plate (TARP) without odontoidectomy. Eur Spine J 23(8):1648–1655
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Y. Zheng, Z.-H. Wu, Y.-H. Yin, Q.-S. Yin, and K. Zhang state that there are no conflicts of interest.
All studies on humans described in the present manuscript were carried out with the approval of the responsible ethics committee and in accordance with national law and the Helsinki Declaration of 1975 (in its current, revised form). Informed consent was obtained from all patients included in studies.
Rights and permissions
About this article
Cite this article
Zheng, Y., Wu, ZH., Yin, YH. et al. Treatment of irreducible atlantoaxial dislocation using the transoral atlantoaxial pedicle screw technique. Orthopäde 45, 174–179 (2016). https://doi.org/10.1007/s00132-015-3219-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00132-015-3219-4