Abstract
Purpose
Attention-deficit hyperactivity disorder (ADHD) is associated with increased use of health, social and education services. There is a lack of data to quantify the economic burden of ADHD in the UK. The aim of this study was to estimate additional education, health and social care costs amongst adolescents in the UK diagnosed with ADHD.
Methods
Participants were 143, 12- to 18-year-olds from the Cardiff longitudinal ADHD study. Service use relating to mental health over the previous year was measured using the children’s service interview. Individual resource use was combined with unit cost data, from national sources, to calculate costs per patient and subsequently the mean cost per patient. Mean costs, 95 % confidence intervals and median use were calculated using nonparametric bootstrapping methods.
Results
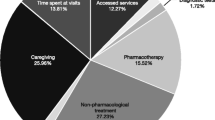
The mean cost per adolescent for NHS, social care and education resources used in a 12-month period related to ADHD was £5,493 (£4,415.68, £6,678.61) in 2010 prices and the median was £2,327. Education and NHS resources accounted for approximately 76 and 24 %, respectively. Estimated annual total UK costs are £670 million.
Conclusions
The additional costs to the NHS and education system of treating adolescents remain substantial for several years after the initial ADHD diagnosis. There exists a need to develop and evaluate early interventions which have the potential to reduce the longer-term burden, particularly on education resource use.


Similar content being viewed by others
References
Ford T, Goodman R, Meltzer H (2003) The British Child and Adolescent Mental Health Survey 1999: the prevalence of DSM-IV disorders. J Am Acad Child Adolesc Psychiatry 42(10):1203–1211
Polanczyk M, Silva de Lima M, Biederman J, Rohde L (2007) The worldwide prevalence of ADHD: a systematic review and metaregression analysis. Am J Psychiatry 164(6):942–948
Biederman J, Faraone S, Milberger S, Curtis S, Chen L, Marrs A et al (1996) Predictors of persistence and remission of ADHD into adolescence: results from a four-year perspective follow-up study. J Am Acad Child Adolesc Psychiatry 35(3):343–351
Hinshaw S (1994) Attention deficits and hyperactivity in children. Sage, Thousand Oaks
Barkley R, Fischer M, Smallish L, Fletcher K (2002) The persistence of attention-deficit/hyperactivity disorder into young adulthood as a function of reporting sources and definition of disorder. J Abnorm Psychol 111:279–289
Faraone SV, Biederman J, Mick E (2006) The age dependent decline of attention deficit hyperactivity disorder: a meta-analysis of follow-up studies. Psychol Med 36:159–165
Ford T, Fowler T, Langley K, Whittinger N, Thapar A (2008) Five years on: public sector service use related to mental health in young people with ADHD or hyperkinetic disorder 5 years after diagnosis. Child Adolesc Mental Health 13(3):122–129
Pelham W, Foster M, Robb J (2007) The economic impact of attention-deficit/hyperactivity disorder in children and adolescents. J Pediatr Psychol 32(6):711–727
Langley K, Fowler T, Ford T, Thapar A, Van den Bree M, Harold G et al (2010) Adolescent clinical outcomes for young people with attention-deficit hyperactivity disorder. Brit J Psychiat 196:235–240
Ford T, Hamilton H, Dosani S, Burke L, Goodman R (2007) The children’s services interview: validity and reliability. Soc Psychiatry Psychiatr Epidemiol 42(1):36–49
British Medical Association and Royal Pharmaceutical Society of Great Britain (2010) British National Formulary (Sept. issue). BMJ Books and Pharmaceutical Press, London
Curtis L (2010) Unit costs of health and social care. Personal Social Services Research Unit, Canterbury
Federation of Ophthalmic and Dispensing Opticians (2010) Optics at a glance 2009. http://www.aop.org.uk/uploads/uploaded_files/optics_at_a_glance_2009.pdf. Accessed 23 June 2011
Department for Education. Education and training expenditure since 1995–96 (Internet only). EXCEL (total school based expenditure per pupil (1995–96 to 2003–04)—real terms (2004–05 prices)). http://www.education.gov.uk/rsgateway/DB/SBU/b000612/index.shtml. Accessed 24 June 2011
National Association of Schoolmasters/Union of Women Teachers. Teachers’ salaries (England and Wales) 2008–2011. http://www.nasuwt.org.uk/TrainingEventsandPublications/NASUWTPublications/Publications/TeachersSalaries2007-2010/index.htm. Accessed 24 June 2011
Curtis L, Netten A (2004) Unit costs of health and social care. Personal Social Services Research Unit, Canterbury
Efron B, Tibshirani R (1993) An introduction to the bootstrap. Chapman and Hall/CRC, Boca Raton
Leibson C, Katusie S, Barbaresi W, Ransom J, O’Brien P (2001) Use and costs of medical care for children and adolescents with and without attention-deficit/hyperactivity disorder. JAMA 285(1):60–66
Ford T, Hamilton H, Meltzer H, Goodman R (2007) Child mental health is everybody’s business; the prevalence of contacts with public sector services by type of disorder among British school children in a three-year period. Child Adolesc Mental Health 12(1):13–20
Weare K, Nind M (2010) Identifying evidence-based work on mental health promotion in schools in Europe: an interim report on the DataPrev project. Adv Sch Mental Health Promot 3(2):36–44
Abbott R, O’Donnell J, Hawkins D, Hill K, Kosterman R, Catalano R (1998) Changing teaching practices to promote achievement and bonding to school. Am J Orthopsychiat 68:542–552
Rimm-Kaufman S, Chiu Y (2007) Promoting social and academic competence in the classroom: an intervention study examining the contribution of the “Responsive Classroom” approach. Psychol Schools 44:397–413
Office for National Statistics (2010) Mid year population estimates 2009: 24/06/10. http://www.statistics.gov.uk/statbase/product.asp?vlnk=15106. Accessed 23 Sept 2011
DiScala C, Lescohier I, Barthel M, Li G (1998) Injuries to children with attention deficit hyperactivity disorder. Pediatrics 102:1415–1421
Szatmari P, Offord D, Boyle M (1989) Correlates, associated impairments and patterns of service utilization of children with attention deficit disorder: findings from the Ontario Child Health Study. J Child Psychol Psychiatry 30:205–217
Acknowledgments
Colin Green and Stuart Logan received research support from the National Institute for Health Research (NIHR) through the Peninsula Collaboration for Leadership in Applied Health Research and Care. This report/article presents independent research commissioned by the NIHR. The views expressed in this publication are those of the authors and not necessarily those of the NHS, the NIHR or the Department of Health. The original study was funded by the Wellcome Trust, Action Medical Research and the Department of Health (England). We are grateful to Dr Marianne van den Bree, Dr Tom Fowler, Professor Michael Owen and Professor Michael O’Donovan for their input to the CLASS study.
Conflict of interest
The authors have no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Telford, C., Green, C., Logan, S. et al. Estimating the costs of ongoing care for adolescents with attention-deficit hyperactivity disorder. Soc Psychiatry Psychiatr Epidemiol 48, 337–344 (2013). https://doi.org/10.1007/s00127-012-0530-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-012-0530-9