Abstract
Aims/hypothesis
Insulin and exercise stimulate skeletal muscle glycogen synthase (GS) activity by dephosphorylation and changes in kinetic properties. The aim of this study was to investigate the effects of insulin, exercise and post-exercise insulin stimulation on GS phosphorylation, activity and substrate affinity in obesity and type 2 diabetes.
Methods
Obese men with type 2 diabetes (n = 13) and weight-matched controls (n = 14) underwent euglycaemic–hyperinsulinaemic clamps in the rested state and 3 h after 60 min of cycling (70% maximal pulmonary oxygen uptake [\( \overset{.}{V}{\mathrm{O}}_{2 \max } \)]). Biopsies from vastus lateralis muscle were obtained before and after clamps, and before and immediately after exercise.
Results
Insulin-stimulated glucose uptake was lower in diabetic patients vs obese controls with or without prior exercise. Post exercise, glucose partitioning shifted away from oxidation and towards storage in both groups. Insulin and, more potently, exercise increased GS activity (fractional velocity [FV]) and substrate affinity in both groups. Both stimuli caused dephosphorylation of GS at sites 3a + 3b, with exercise additionally decreasing phosphorylation at sites 2 + 2a. In both groups, changes in GS activity, substrate affinity and dephosphorylation at sites 3a + 3b by exercise were sustained 3 h post exercise and further enhanced by insulin. Post exercise, reduced GS activity and substrate affinity as well as increased phosphorylation at sites 2 + 2a were found in diabetic patients vs obese controls.
Conclusions/interpretation
Exercise-induced activation of muscle GS in obesity and type 2 diabetes involves dephosphorylation of GS at sites 3a + 3b and 2 + 2a and enhanced substrate affinity, which is likely to facilitate glucose partitioning towards storage. Lower GS activity and increased phosphorylation at sites 2 + 2a in type 2 diabetes in the recovery period imply an impaired response to exercise.
Similar content being viewed by others
Introduction
In type 2 diabetes, insulin-mediated glucose uptake is reduced by about 40% compared with weight-matched control individuals, with the defect largely accounted for by reduced glycogen synthesis in skeletal muscle [1–3]. In accordance, insulin activation of glycogen synthase (GS), the key enzyme in the regulation of glycogen synthesis, has consistently been found defective in muscle of patients with type 2 diabetes and obese insulin-resistant individuals [3–7].
Exercise plays a fundamental role in the prevention and treatment of type 2 diabetes [8, 9]. Beneficial effects of a single bout of moderate-intensity exercise include an immediate increase in muscle glucose uptake [10]. This is followed by a more prolonged (<48 h) increase in insulin sensitivity to stimulate glucose uptake in both healthy, insulin-resistant and type 2 diabetic individuals [11–13]. Both basal and insulin-stimulated muscle GS activity is elevated in recovery from exercise, indicating that GS indirectly mediates glucose uptake after exercise [7, 14] and facilitates glycogen replenishment. In line, correlation between insulin-stimulated glucose storage and GS activity at recovery from exercise has been reported [12]. Interestingly, glycogen-lowering exercise also increases GS activity per se [15]. This regulation does not seem to be impaired in insulin-resistant muscle [16, 17], indicating differential regulation of GS by insulin and exercise.
The activity of GS is regulated both by its allosteric activator glucose 6-phosphate (G6P) and covalently by phosphorylation of at least nine serine residues, of which sites 2, 2a, 3a and 3b are considered the most important [18, 19]. Dephosphorylation promotes activation of GS [20]. Insulin stimulation induces GS dephosphorylation at sites 3a + 3b as well as sites 2 + 2a in muscle of healthy individuals [6, 21, 22]. Impaired insulin activation of GS in insulin-resistant conditions such as obesity and type 2 diabetes is associated with dysregulation of GS dephosphorylation in skeletal muscle, in particular at sites 2 + 2a [4–6]. Also, the activation of GS during endurance exercise is associated with dephosphorylation of sites 3a and 3b but seemingly unchanged phosphorylation at sites 2 and 2a [15, 16]. Interestingly, glycogen content is tightly associated with GS activity, and glycogen depletion by exercise is associated with decreased phosphorylation of sites 2 + 2a [15]. GS affinity for its substrate uridine diphosphate-glucose (UDP-glucose) is regulated by phosphorylation, and assessment of both substrate affinity and traditional measurements of GS activity may provide more comprehensive insights to GS function [23]. A recent study of GS kinetic properties and phosphorylation in skeletal muscle indicates that the response to exercise and exercise recovery is preserved in obesity and type 2 diabetes [16]. However, that study neither compared the effect of acute exercise with that of insulin nor investigated the effect of insulin in recovery from exercise.
The present study was undertaken to investigate whether dysregulation of GS by insulin in type 2 diabetes is influenced by prior exercise. In a well-matched cohort of type 2 diabetic patients and obese control individuals, we investigated GS activity, phosphorylation and kinetic properties in response to acute moderate-intensity exercise and physiological insulin stimulation. In addition, these properties of GS were investigated in the insulin-stimulated state during recovery from exercise.
Methods
Participants
Thirteen obese male patients with type 2 diabetes and 14 obese healthy male control individuals, matched for age, BMI and physical activity level, participated in the study (Table 1). Medication details and eligibility criteria are given in the electronic supplementary material (ESM) Methods. Informed consent was obtained from all participants before participation. The study was approved by the local ethics committee and was performed in accordance with the Helsinki Declaration.
Study design
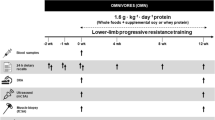
One week prior to the first trial, participants underwent blood screening tests, including plasma glucose, HbA1c and lipids, ECG and exercise tests [24] to determine maximal pulmonary oxygen uptake (see ESM Methods). Subsequently, participants underwent two experimental tests, a baseline (‘baseline day’) and a post-exercise (‘exercise day’) euglycaemic–hyperinsulinaemic clamp, separated by 4–8 weeks (ESM Fig. 1). All medications were withdrawn 1 week prior to both test days (see ESM Methods), and individuals were instructed to refrain from strenuous exercise for 48 h before each test.
Baseline euglycaemic–hyperinsulinaemic clamp
After an overnight fast, participants underwent a euglycaemic–hyperinsulinaemic clamp with tracer glucose (2 h basal period and 4 h insulin infusion, 40 mU m−2 min−1) combined with indirect calorimetry (see ESM Methods) to assess total glucose disposal rates (GDR), rates of glucose and lipid oxidation, and non-oxidative glucose disposal (NOGD) as described previously [4, 6, 25]. Muscle biopsies were obtained from vastus lateralis muscle before and after insulin (see ESM Methods).
At 4–8 weeks after the baseline clamp, the participants returned to the clinic after an overnight fast. They were rested for 30 min in the supine position, and two incisions (4–5 cm apart) were made in the same leg. A first biopsy was obtained from vastus lateralis muscle through the lower incision (pre-exercise biopsy). The participants then exercised on a cycle ergometer for 60 min at an intensity (~70% maximal pulmonary oxygen uptake [\( \overset{.}{V}{\mathrm{O}}_{2 \max } \)]), which has been shown to increase insulin sensitivity immediately after and up to 48 h afterwards [11]. On completion of exercise, a second muscle biopsy was obtained through the upper incision (exercise biopsy). Participants then rested in bed for 1 h, after which a post-exercise euglycaemic–hyperinsulinaemic clamp study identical to the previous clamp was started. Muscle biopsies (4–5 cm apart) were then taken from the other leg before (3 h into recovery) and after insulin stimulation (7 h into recovery including 4 h insulin infusion). Muscle homogenates were prepared as described in ESM Methods.
GS activity and Km value
All GS activity measurements were performed in 96 well microtitre plates as previously described [6]. The fractional velocity (FV) of GS was determined in the presence of 0.1 mmol/l (FV0.1) and 1.67 mmol/l (FV1.67) UDP-glucose. The FV was calculated as: 100 × activity in the presence of 0.17 mmol/l G6P/activity at 8 mmol/l G6P. The activity of GS independent of G6P (I-form) was determined in the presence of 1.67 mmol/l UDP and calculated as: 100 × activity in the presence of 0.02 mmol/l G6P/activity at 8 mmol/l G6P. The affinity of GS for UDP-glucose (expressed as the K m, i.e. an inverse measure of enzyme affinity for substrate) was analysed in the presence of 0.17 mmol/l G6P and the following concentrations of UDP-glucose: 0.1, 0.3, 0.7 and 1.67 mmol/l. Data were analysed as Eadie–Hofstee plots, with K m calculated as the reciprocal to the slope.
Glycogen content
Muscle glycogen content was measured in muscle homogenates (150 μg protein) as glycosyl units after acid hydrolysis determined by a fluorometric method [26].
SDS-PAGE and western blotting
Protein levels and phosphorylation patterns were measured using SDS-PAGE with self-cast Tris-HCl gels (7.5%). Proteins were transferred by semidry transfer to polyvinylidene difluoride (PVDF) membranes (Immobilion Transfer Membrane; Millipore, Billerica, MA, USA). The membranes were blocked by incubation in 3% skimmed milk (15 min, room temperature). After primary (overnight, 4°C) and secondary antibody treatment (45 min, room temperature), membranes were incubated in a chemiluminescent substrate (Immobilon Western Chemilum HRP Substrate; Millipore). The primary antibodies used were as previously described [6].
Statistics
Statistical analyses were performed by SigmaStat version 3.5 (Systat Software, San Jose, CA, USA). Baseline characteristics of diabetic and control individuals were compared via Student’s unpaired t tests. Separate two-way repeated measures analysis of variance (two-way RM ANOVA) was performed to evaluate the effect of insulin (‘baseline day’, ‘exercise day’) and exercise/recovery (pre-exercise, exercise and 3 h recovery data on the exercise day). Significant main effects or interactions were further analysed by the Student–Newman–Keul post-hoc test. The linear dependence between different groups of data was assessed by Spearman’s rank correlation coefficient. Data are presented as means ± SEM. Significance was accepted at p < 0.05.
Results
Euglycaemic–hyperinsulinaemic clamps
In the insulin-stimulated period of both clamps, euglycaemia (~5.5 mmol/l) and hyperinsulinaemia (~400 pmol/l) were achieved in each group (Table 2). During the baseline clamp, insulin-stimulated GDR, glucose oxidation and NOGD were lower in type 2 diabetic patients vs weight-matched obese controls (Table 2). Reduced NOGD accounted for ~70% of the reduction in insulin-stimulated GDR in diabetic patients. Similar differences between the groups were seen during the post-exercise clamp. When comparing the baseline day with the exercise day, neither basal nor insulin-stimulated GDR was altered by prior exercise in either group (Table 2). However, prior exercise did lower basal and insulin-stimulated glucose oxidation in both groups. In line, prior exercise increased basal and insulin-stimulated NOGD in diabetic patients. In obese controls previous exercise did not significantly alter NOGD when evaluated by two-way RM ANOVA. However, when evaluated by Student’s paired t test, basal NOGD was increased after exercise (p < 0.01). In response to exercise, plasma NEFA at the beginning of the basal clamp period increased from 543 ± 52 to 838 ± 63 and from 428 ± 26 to 842 ± 85 nmol/l in diabetic patients and obese controls, respectively (p < 0.001), and remained significantly elevated during the recovery period (p < 0.001) as well as 1 and 2 h into the following insulin-stimulated period (Fig. 1). During the last 2 h of the insulin-stimulated period, plasma NEFA were higher in diabetic patients vs obese controls (p < 0.05) both with and without prior exercise (Fig. 1).
Plasma NEFA levels in patients with type 2 diabetes (black circles/triangles) and controls (white circles/triangles) on: (1) the baseline day (triangles) during the basal (60–180 min) and insulin-stimulated (180–420 min) periods; and on (2) the exercise day (circles) during exercise (−60–0 min) and during the basal and insulin-stimulated periods post exercise. Insulin was infused at a rate of 40 mU m−2 min−1 for 4 h. Exercise consisted of 60 min cycling at 70% \( \overset{.}{V}{\mathrm{O}}_{2 \max } \). Data are means ± SEM. *** p < 0.001 vs baseline day (main effect day); † p < 0.05 type 2 diabetes vs controls on baseline day (main effect group); ‡ p < 0.05 type 2 diabetes vs controls on exercise day (main effect group); and §§ p < 0.01 vs NEFA levels at −60 min (main effect time)
Glycogen content
On the baseline day, muscle glycogen content was similar between groups (Fig. 2a). On the exercise day, exercise robustly decreased muscle glycogen content by ~50% (p < 0.001) in both groups. Glycogen content did not change during the 3 h recovery period. After subsequent insulin stimulation, glycogen content increased equally in the groups (p < 0.05). However, glycogen levels were not restored to pre-exercise levels (Fig. 2a).
Muscle glycogen content (a); GS FV assayed with 0.1 mmol/l (b) and 1.67 mmol/l UDP-glucose (c); GS I-form activity (d) and K m value assayed with 0.17 mmol/l of G6P (e) in skeletal muscle biopsies obtained from patients with type 2 diabetes (black bars) and obese controls (white bars) on the baseline day before and after insulin and on the exercise day before and after exercise and before and after insulin. Data are means ± SEM. (*) p < 0.10, * p < 0.05, ** p < 0.01 and *** p < 0.001 vs before insulin; †† p < 0.01 and ††† p < 0.001 vs before exercise; ‡ p < 0.05 vs after exercise; (§) p < 0.10 and § p < 0.05 vs controls; ¶ p < 0.05 and ¶¶¶ p < 0.001 vs after insulin. Basal, before insulin; Ins, after insulin; Pre-ex, before exercise; Ex, after exercise; 3 h rec, before insulin (3 h into recovery on exercise day); Ins + 7 h rec, after insulin (7 h into recovery on exercise day)
GS protein content
No differences in total GS protein content or GS total activities, either measured in the presence of 1.67 mmol/l (high) or 0.1 mmol/l (low) UDP-glucose, were found at any time or between groups (data not shown). Average total GS activity (n = 102) was 18.8 ± 0.6 nmol min−1 mg−1 at high and 6.5 ± 0.1 nmol min−1 mg−1 at low UDP-glucose concentration.
GS activity
On the baseline day, insulin stimulation increased GS activity measured as FV0.1, FV1.67 and I-form similarly in each group (Fig. 2b–d). Exercise robustly increased these measures of GS activity with no differences between groups. Activation of GS by exercise per se was markedly higher than the effect of insulin per se (p < 0.001). At 3 h into recovery, these measures of GS activity remained elevated in obese controls, but decreased in diabetic patients, so that the GS FV1.67, and I-form activities were lower in diabetic patients vs obese controls. Subsequent insulin stimulation increased all measures of GS activity in both groups, but GS FV0.1 and FV1.67 activities were still lower in the diabetic patients vs obese controls. The activities of GS FV0.1, FV1.67 and I-form were higher in the post-exercise clamp vs the baseline clamp in both groups (Fig. 2b–d).
GS affinity for UDP-glucose
On the baseline day, basal muscle GS affinity for UDP-glucose (assessed with a physiological [0.17 mmol/l] concentration of G6P) was similar between groups (K m ~ 1.5 mmol) (Fig. 2e). Insulin increased GS affinity for UDP-glucose as K m decreased to ~1.0 mmol/l in both groups (p < 0.001). Exercise also increased GS substrate affinity (p < 0.001) and in fact more potently than insulin per se to K m values around 0.4–0.5 mmol/l in both groups. After 3 h of recovery, K m remained decreased compared with pre-exercise in both groups.
Comparison of K m values for the first three time points of the exercise day using two-way RM ANOVA showed significant effects of exercise (p < 0.001) and group (p < 0.05), with no significant interaction between group and exercise (p = 0.43). However, comparing only the exercise values with the 3 h recovery values demonstrated that K m was higher in diabetic patients vs obese controls 3 h into recovery, and actually increased during recovery in the diabetic patients. Post exercise, insulin tended to decrease K m further (p = 0.06 for main effect) with no significant differences between groups. These observations on GS substrate affinity (K m) are in line with the GS activity pattern described above. Finally, insulin-stimulated K m values were markedly lower in the post-exercise state than during the baseline condition in both groups (p < 0.001).
GS phosphorylation
Dephosphorylation of GS at sites 2 + 2a and 3a + 3b is an important mechanism by which GS is activated [18–20, 27]. On the baseline day, insulin decreased GS sites 3a + 3b phosphorylation in both groups (p = 0.008) (Fig. 3a). GS sites 3a + 3b phosphorylation was also robustly decreased in response to exercise (p < 0.001), and remained decreased 3 h into recovery in both groups (p < 0.001). Post-exercise insulin stimulation further decreased GS sites 3a + 3b phosphorylation vs 3 h into recovery (p = 0.012) causing reduced GS sites 3a + 3b phosphorylation compared with the baseline insulin-stimulated condition in both groups (p = 0.001). No differences in GS sites 3a + 3b phosphorylation were seen between diabetic patients and controls.
Phosphorylation of GS at sites 3a + 3b (a), sites 2 + 2a (b) and site 1a (c), and Ser9 phosphorylation of GSK3-β (d) and Thr172 phosphorylation of AMPK (e) in skeletal muscle biopsies obtained from patients with type 2 diabetes (black bars) and controls (white bars) on the baseline day and the exercise day (see Fig. 2). Representative immunoblots are shown in (f). Quantified data in the bar graphs are given in arbitrary units. Data are means ± SEM. * p < 0.05, ** p < 0.01 and *** p < 0.001 vs before insulin; †† p < 0.01 and ††† p < 0.001 vs before exercise; ‡ p < 0.05 vs after exercise; (§) p < 0.10 and § p < 0.05 vs controls and ¶¶¶ p < 0.001 vs after insulin. AU, arbitrary units; Basal, before insulin; Ins, after insulin; Pre-ex, before exercise; Ex, after exercise; 3 h rec, before insulin (3 h into recovery on exercise day); Ins + 7 h rec, after insulin (7 h into recovery on exercise day); T2D, type 2 diabetes
GS phosphorylation at sites 2 + 2a was similar between the groups on the baseline day and was not influenced by insulin (Fig. 3b). Exercise caused significant dephosphorylation of GS sites 2 + 2a (p < 0.01 vs pre-exercise), with no difference between groups. After 3 h of recovery, a significant (115%) increase in GS phosphorylation at sites 2 + 2a vs the level at exercise was observed in the diabetic patients (p = 0.02). On the exercise day, GS phosphorylation at sites 2 + 2a was again not affected by insulin in either group. GS site 1a phosphorylation was similar between groups at all time points (Fig. 3c). Whereas insulin did not affect this phosphorylation site on the baseline day, exercise caused significant GS site 1a dephosphorylation (p < 0.01), and it remained decreased 3 h into recovery. Post-exercise insulin stimulation increased GS site 1a phosphorylation (p < 0.01 vs recovery), with a tendency for this effect to be confined to the diabetic group (p = 0.09 for interaction between group and insulin). GS site 1b phosphorylation was similar in diabetic patients and obese controls at all time points and was unaffected by insulin or exercise (ESM Fig. 2).
Glycogen synthase kinase 3 (GSK3) and AMP-activated protein kinase (AMPK) are major upstream regulators of GS [27, 28]. Insulin stimulation inhibited GSK-3β activity by increasing Ser9 phosphorylation on both experimental days (p < 0.001). No effect of acute exercise was seen on GSK-3β Ser9 phosphorylation (Fig. 3d). GSK-3β Ser9 phosphorylation was slightly higher 3 h into recovery vs exercise, and tended to be increased in the diabetic group in the recovery period compared with obese controls (p = 0.099). AMPK phosphorylation at Thr172 (reflecting kinase activation) was increased modestly by exercise in both groups (p = 0.002) (Fig. 3e). AMPK phosphorylation decreased in recovery from exercise (p = 0.029) and was further decreased by insulin (p = 0.009) on the exercise day. Interestingly, AMPK phosphorylation was elevated in the post-exercise period in type 2 diabetic patients compared with obese controls (p = 0.03). Total protein levels of AMPK (α2 subunit) and GSK-3β were similar between groups and unaffected by interventions except for a small increase in GSK-3β protein by insulin on the baseline day (p < 0.001) (data not shown).
Correlation analysis
To explore possible mechanisms underlying the regulation of GS activity, phosphorylation and substrate affinity (K m) by insulin, exercise and insulin post exercise, we examined the relationship between these measures as well as glucose metabolism and glycogen content in the study cohort.
On the baseline day, insulin-stimulated GDR and NOGD correlated positively with GS FV0.l, FV1.67 and I-form (r = 0.41 to 0.66, all p < 0.05). No significant associations between these variables were seen on the exercise day.
On the baseline day, insulin-stimulated GS FV0.1, FV1.67 and GS I-form activities correlated inversely with GS phosphorylation at sites 3a + 3b and 2 + 2a (r = −0.48 to −0.61, all p < 0.01). K m correlated with GS phosphorylation at sites 2 + 2a (r = 0.50, p < 0.01) and tended to correlate with GS phosphorylation at sites 3a + 3b (r = 0.37, p = 0.06).
On the exercise day, GS FV0.1, FV1.67 and I-form activities after exercise correlated inversely with GS sites 3a + 3b phosphorylation (r = −0.55 to −0.68, all p < 0.01) and at sites 2 + 2a (r = −0.41 to −0.56, all p < 0.05). K m correlated with GS sites 3a + 3b phosphorylation (r = 0.42, p = 0.03) and tended to correlate with GS phosphorylation at sites 2 + 2a (r = 0.35, p = 0.08). During recovery, GS FV0.1, FV1.67 and I-form activities all showed an inverse correlation with GS phosphorylation at sites 3a + 3b and 2 + 2a (r = −0.64 to −0.83, all p < 0.001), whereas K m correlated with GS phosphorylation at both sites 3a + 3b and sites 2 + 2a (r = 0.61 to 0.71, p < 0.001).
On the exercise day, the changes (∆ values) in muscle glycogen content in response to exercise correlated inversely with the changes in GS FV0.1, FV1.67 and I-form activities (r = −0.43 to 0.56, all p < 0.05), and positively with the changes in K m (r = 0.53, p < 0.01) and with the changes in the corresponding phosphorylation of GS at sites 3a + 3b (r = 0.56, p < 0.01) and sites 2 + 2a (r = 0.41, p = 0.03).
Discussion
In the present study, we demonstrate that moderate-intensity exercise reduces muscle glycogen, increases muscle GS activity and substrate affinity, and dephosphorylates GS at sites 3a + 3b and 2 + 2a to a similar degree in type 2 diabetic patients and well-matched controls. These effects may explain the observed increase in glucose partitioning toward storage and away from oxidation. Importantly, we show that, 3 h into exercise recovery and during insulin stimulation post exercise, GS activity and substrate affinity in muscle are reduced in diabetic patients compared with controls concomitant with increased phosphorylation of GS at sites 2 + 2a. This dysregulation of muscle GS in type 2 diabetes implies some degree of impaired response to recovery from exercise.
Our findings on the effects of exercise on GS activity, substrate affinity and sites 3a + 3b phosphorylation are in accordance with a recent study that reported similar changes in these variables and with comparable efficacy in lean, obese and type 2 diabetic individuals [16]. In contrast to our results, Jensen et al could not demonstrate an effect of acute exercise on GS phosphorylation at sites 2 + 2a or differences in measures of GS activity and phosphorylation 3.5 h into recovery between the diabetic and control groups [16]. However, in that study the post-exercise muscle biopsies were only available from four diabetic participants, which may explain the inability to detect such changes. This, together with differences in sex composition and a lower baseline \( \overset{.}{V}{\mathrm{O}}_{2 \max } \), may explain these discordant findings. Mutational studies [18, 19] as well as analysis on muscle biopsies from humans [15, 21, 22, 29] have found phosphorylation of GS at sites 2 + 2a and 3a + 3b to be the most important for GS activity. In accordance, we demonstrate an inverse correlation between both insulin- and exercise-induced measures of GS activity and GS phosphorylation at these sites. This also suggests that the increased phosphorylation at GS sites 2 + 2a caused the reduced GS activities in our diabetic cohort in the recovery period.
Glycogen is a proposed regulator of GS activity [30] and GS phosphorylation at sites 2 + 2a [28]. Consistent with this, the exercise-associated decrease in muscle glycogen content has been shown to be a factor involved in GS activation [30–32]. Recently, a positive correlation between muscle glycogen levels and GS phosphorylation at sites 2 + 2a, 3a, and 3a + 3b was reported in pooled data from healthy young volunteers before, during and after glycogen-depleting exercise [15]. We extend these findings to a cohort of obese individuals with or without type 2 diabetes, reporting a positive correlation between changes in muscle glycogen content during moderate-intensity exercise and changes in phosphorylation of GS at sites 2 + 2a and 3a + 3b. In skeletal muscle of both normal and insulin-resistant rats, contraction-induced glycogen utilisation is associated with dephosphorylation of GS on sites 2 + 2a [33, 34]. It is, therefore, interesting that GS phosphorylation at sites 2 + 2a increased 3 h into recovery in our patients with type 2 diabetes despite a sustained depletion of glycogen. This suggests that in type 2 diabetes, recovery from exercise is associated with activation of kinases and/or inhibition of phosphatases acting on muscle GS. Our data suggest that increased activation of the stress-activated kinase AMPK during exercise recovery might be associated with enhanced GS site 2 + 2a phosphorylation in the type 2 diabetic patients compared with obese controls. The pattern of GSK-3β regulation does not support a direct role for this kinase in the differential GS regulation during the post-exercise period between the groups.
Several studies have found insulin sensitivity, as assessed by the euglycaemic–hyperinsulinaemic clamp technique, to be increased for a prolonged period after a single bout of moderate- to strenuous-intensity cycle exercise [11, 12]. An enhanced post-exercise insulin sensitivity has been demonstrated both for glucose-tolerant individuals and for various insulin-resistant populations, including patients with type 2 diabetes, with the change mainly accounted for by an increase in NOGD [11–13]. As glycogen synthesis is the primary pathway of NOGD [1], these changes favour glycogen replenishment after exercise [13, 17, 35–37].
It was thus somewhat surprising that we did not find an effect of prior exercise on insulin-stimulated GDR in either diabetic or obese control individuals. Indeed, the observed exercise-induced increase in plasma NEFA, which was sustained at least 3 h into recovery in both groups as shown previously [38], is a physiological response that might explain the lack of increase in whole-body insulin-stimulated glucose metabolism by both changes in substrate preferences and perhaps signalling mechanisms [39–41]. Moreover, NEFA levels remained elevated during the post-exercise clamp in the diabetic individuals. This indicates that insulin resistance at the level of adipose tissue is not ameliorated in response to exercise. Nevertheless, prior exercise did in fact direct basal and insulin-stimulated glucose uptake toward storage and away from oxidation within both groups, in accordance with previous observations [42].
Glucose storage has consistently been reported to correlate with GS activity [6, 7, 12]. In accordance with the effect of exercise on intracellular glucose metabolism, we observed increased basal and insulin-stimulated values for GS activity and substrate affinity after exercise in both diabetic and obese individuals. As noted by Jensen et al [16], with a GS K m value (in the mmol/l range) far above the physiological concentration of UDP-glucose (estimated to ~0.03 mmol/l in resting muscle), an increase in substrate affinity would be likely to increase the rate of glucose storage into glycogen after exercise. Correspondingly, we demonstrate a reduction in the GS K m at a physiological concentration of G6P (0.17 mmol/l) from above 1 mmol/l in the rested state to < 0.5 mmol/l after exercise in both study groups.
Previously, we have found GS hyperphosphorylation or lack of dephosphorylation on sites 2 + 2a together with impaired GS activation by insulin in muscle of patients with type 2 diabetes compared with lean and obese controls in some [4, 5], but not all studies [6]. However, in the present study, we could not demonstrate these differences between patients with type 2 diabetes and weight-matched obese controls in the baseline rested state. In line with previous studies of insulin-resistant conditions including individuals with obesity, PCOS and type 2 diabetes [4–6, 25, 29], we did, however, observe a lack of insulin-induced dephosphorylation of GS at sites 2 + 2a in both type 2 diabetes and obesity. These phosphosites have previously been found to be responsive to insulin stimulation in a number of healthy lean participant populations [4, 25, 43].
Although impaired insulin activation of muscle GS represents one of the more consistent defects found in insulin-resistant cohorts with obesity, polycystic ovary syndrome (PCOS) and type 2 diabetes [4, 6, 7, 25], not all studies have been able to detect a difference between type 2 diabetic and weight-matched obese individuals [6, 17, 44]. In the present study, the insulin-stimulated GDR in the type 2 diabetic patients was 51–77% higher than values reported in our previous studies [6, 44]. This could be explained by the higher cardiorespiratory fitness (\( \overset{.}{V}{\mathrm{O}}_{2 \max } \)) in this diabetic cohort compared with cohorts in previous studies [5, 45], and may have contributed to higher insulin-stimulated GS activity in the rested state. Nevertheless, our data also demonstrate that changes in GS activity, substrate affinity and phosphorylation cannot explain all the differences in whole-body insulin sensitivity between type 2 diabetic patients and weight-matched controls, indicating a role for other factors, e.g. those involved in glucose delivery (capillary recruitment) or glucose transport (Glut4 recruitment) and phosphorylation (hexokinase II activation).
In summary, the present study demonstrates that a single bout of exercise stimulates muscle GS activity with similar efficiency in type 2 diabetic patients and weight-matched controls. This effect involves GS dephosphorylation and enhanced substrate affinity. In both groups these exercise-induced effects on GS were sustained 3 h into recovery. Thus, the subsequent enhanced insulin-stimulated responses may contribute to increased glucose partitioning towards storage and away from oxidation in the period after exercise. Interestingly, compared with obese controls, increased phosphorylation of GS at sites 2 + 2a in concert with impaired GS activation was observed in the diabetic group during recovery from exercise. Further studies are needed to establish to what extent these post-exercise defects in the regulation of GS leave type 2 diabetic patients refractory to post-exercise recovery. Although not fully illuminated, our data suggest that elevated AMPK activity in the post-exercise recovery period might be part of the mechanisms involved.
Abbreviations
- AMPK:
-
AMP-activated protein kinase
- FV(0.1/1.67) :
-
Fractional velocity (at 0.1/1.67 mmol/l UDP-glucose)
- G6P:
-
Glucose 6-phosphate
- GDR:
-
Glucose disposal rate
- GS:
-
Glycogen synthase
- GSK3:
-
Glycogen synthase kinase 3
- I-form:
-
Glycogen synthase activity independent of G6P
- NOGD:
-
Non-oxidative glucose disposal
- RM ANOVA:
-
Repeated measures ANOVA
- UDP-glucose:
-
Uridine diphosphate-glucose
- \( \overset{.}{V}{\mathrm{O}}_{2 \max } \) :
-
Maximal pulmonary oxygen uptake
References
DeFronzo RA, Tripathy D (2009) Skeletal muscle insulin resistance is the primary defect in type 2 diabetes. Diabetes Care 32(Suppl 2):157–163
Højlund K (2014) Metabolism and insulin signaling in common metabolic disorders and inherited insulin resistance. Dan Med J 61:B4890
Shulman GI, Rothman DL, Jue T, Stein P, DeFronzo RA, Shulman RG (1990) Quantitation of muscle glycogen synthesis in normal subjects and subjects with non-insulin-dependent diabetes by 13C nuclear magnetic resonance spectroscopy. N Engl J Med 322:223–228
Højlund K, Staehr P, Hansen BF et al (2003) Increased phosphorylation of skeletal muscle glycogen synthase at NH2-terminal sites during physiological hyperinsulinemia in type 2 diabetes. Diabetes 52:1393–1402
Vind BF, Pehmoller C, Treebak JT et al (2011) Impaired insulin-induced site-specific phosphorylation of TBC1 domain family, member 4 (TBC1D4) in skeletal muscle of type 2 diabetes patients is restored by endurance exercise-training. Diabetologia 54:157–167
Højlund K, Birk JB, Klein DK et al (2009) Dysregulation of glycogen synthase COOH- and NH2-terminal phosphorylation by insulin in obesity and type 2 diabetes mellitus. J Clin Endocrinol Metab 94:4547–4556
Cusi K, Maezono K, Osman A et al (2000) Insulin resistance differentially affects the PI 3-kinase- and MAP kinase-mediated signaling in human muscle. J Clin Invest 105:311–320
Helmrich SP, Ragland DR, Leung RW, Paffenbarger RS Jr (1991) Physical activity and reduced occurrence of non-insulin-dependent diabetes mellitus. N Engl J Med 325:147–152
Madden KM (2013) Evidence for the benefit of exercise therapy in patients with type 2 diabetes. Diabetes Metab Syndr Obes 6:233–239
Martin IK, Katz A, Wahren J (1995) Splanchnic and muscle metabolism during exercise in NIDDM patients. Am J Physiol 269:583–590
Mikines KJ, Sonne B, Farrell PA, Tronier B, Galbo H (1988) Effect of physical exercise on sensitivity and responsiveness to insulin in humans. Am J Physiol 254:248–259
Bogardus C, Thuillez P, Ravussin E, Vasquez B, Narimiga M, Azhar S (1983) Effect of muscle glycogen depletion on in vivo insulin action in man. J Clin Invest 72:1605–1610
Devlin JT, Hirshman M, Horton ED, Horton ES (1987) Enhanced peripheral and splanchnic insulin sensitivity in NIDDM men after single bout of exercise. Diabetes 36:434–439
Wojtaszewski JF, Hansen BF, Kiens B, Richter EA (1997) Insulin signaling in human skeletal muscle: time course and effect of exercise. Diabetes 46:1775–1781
Prats C, Helge JW, Nordby P et al (2009) Dual regulation of muscle glycogen synthase during exercise by activation and compartmentalization. J Biol Chem 284:15692–15700
Jensen J, Tantiwong P, Stuenaes JT et al (2012) Effect of acute exercise on glycogen synthase in muscle from obese and diabetic subjects. Am J Physiol Endocrinol Metab 303:82–89
Christ-Roberts CY, Pratipanawatr T, Pratipanawatr W, Berria R, Belfort R, Mandarino LJ (2003) Increased insulin receptor signaling and glycogen synthase activity contribute to the synergistic effect of exercise on insulin action. J Appl Physiol 95:2519–2529
Skurat AV, Roach PJ (1995) Phosphorylation of sites 3a and 3b (Ser640 and Ser644) in the control of rabbit muscle glycogen synthase. J Biol Chem 270:12491–12497
Skurat AV, Dietrich AD, Roach PJ (2000) Glycogen synthase sensitivity to insulin and glucose-6-phosphate is mediated by both NH2- and COOH-terminal phosphorylation sites. Diabetes 49:1096–1100
Beck-Nielsen H (2012) The role of glycogen synthase in the development of hyperglycemia in type 2 diabetes: 'To store or not to store glucose, that's the question'. Diabetes Metab Res Rev 28:635–644
Friedrichsen M, Birk JB, Richter EA et al (2013) Akt2 influences glycogen synthase activity in human skeletal muscle through regulation of NH2-terminal (sites 2 + 2a) phosphorylation. Am J Physiol Endocrinol Metab 304:631–639
Poulsen P, Wojtaszewski JF, Petersen I et al (2005) Impact of genetic versus environmental factors on the control of muscle glycogen synthase activation in twins. Diabetes 54:1289–1296
Jensen J, Lai YC (2009) Regulation of muscle glycogen synthase phosphorylation and kinetic properties by insulin, exercise, adrenaline and role in insulin resistance. Arch Physiol Biochem 115:13–21
Astrand I (1960) Aerobic work capacity in men and women with special reference to age. Acta Physiol Scand (Suppl 49):1–92
Vind BF, Birk JB, Vienberg SG et al (2012) Hyperglycaemia normalises insulin action on glucose metabolism but not the impaired activation of AKT and glycogen synthase in the skeletal muscle of patients with type 2 diabetes. Diabetologia 55:1435–1445
Lowry O, Passanneau JV (1972) A flexible system of enzyme analysis. Academic, London, pp 1–291
Cohen P, Alessi DR, Cross DA (1997) PDK1, one of the missing links in insulin signal transduction? FEBS Lett 410:3–10
Jørgensen SB, Nielsen JN, Birk JB et al (2004) The alpha2-5'AMP-activated protein kinase is a site 2 glycogen synthase kinase in skeletal muscle and is responsive to glucose loading. Diabetes 53:3074–3081
Glintborg D, Højlund K, Andersen NR, Hansen BF, Beck-Nielsen H, Wojtaszewski JF (2008) Impaired insulin activation and dephosphorylation of glycogen synthase in skeletal muscle of women with polycystic ovary syndrome is reversed by pioglitazone treatment. J Clin Endocrinol Metab 93:3618–3626
Danforth WH (1965) Glycogen synthetase activity in skeletal muscle. Interconversion of two forms and control of glycogen synthesis. J Biol Chem 240:588–593
Jensen J, Jebens E, Brennesvik EO et al (2006) Muscle glycogen inharmoniously regulates glycogen synthase activity, glucose uptake, and proximal insulin signaling. Am J Physiol Endocrinol Metab 290:154–162
Wojtaszewski JF, Nielsen JN, Richter EA (2002) Invited review: effect of acute exercise on insulin signaling and action in humans. J Appl Physiol 93:384–392
Lai YC, Stuenaes JT, Kuo CH, Jensen J (2007) Glycogen content and contraction regulate glycogen synthase phosphorylation and affinity for UDP-glucose in rat skeletal muscles. Am J Physiol Endocrinol Metab 293:1622–1629
Lin FC, Bolling A, Stuenaes JT et al (2012) Effect of insulin and contraction on glycogen synthase phosphorylation and kinetic properties in epitrochlearis muscles from lean and obese Zucker rats. Am J Physiol Cell Physiol 302:1539–1547
Richter EA, Mikines KJ, Galbo H, Kiens B (1989) Effect of exercise on insulin action in human skeletal muscle. J Appl Physiol 66:876–885
Kjaer M, Hollenbeck CB, Frey-Hewitt B, Galbo H, Haskell W, Reaven GM (1990) Glucoregulation and hormonal responses to maximal exercise in non-insulin-dependent diabetes. J Appl Physiol 68:2067–2074
Burstein R, Epstein Y, Shapiro Y, Charuzi I, Karnieli E (1990) Effect of an acute bout of exercise on glucose disposal in human obesity. J Appl Physiol 69:299–304
Bahr R, Høstmark AT, Newsholme EA, Grønnerød O, Sejersted OM (1991) Effect of exercise on recovery changes in plasma levels of FFA, glycerol, glucose and catecholamines. Acta Physiol Scand 143:105–115
Boden G (2002) Interaction between free fatty acids and glucose metabolism. Curr Opin Clin Nutr Metab Care 5:545–549
Szendroedi J, Yoshimura T, Phielix E et al (2014) Role of diacylglycerol activation of PKCθ in lipid-induced muscle insulin resistance in humans. Proc Natl Acad Sci U S A 111:9597–9602
Høeg LD, Sjøberg KA, Jeppesen J et al (2011) Lipid-induced insulin resistance affects women less than men and is not accompanied by inflammation or impaired proximal insulin signaling. Diabetes 60:64–73
Pehmøller C, Brandt N, Birk JB et al (2012) Exercise alleviates lipid-induced insulin resistance in human skeletal muscle-signaling interaction at the level of TBC1 domain family member 4. Diabetes 61:2743–2752
Bienso RS, Ringholm S, Kiilerich K et al (2012) GLUT4 and glycogen synthase are key players in bed rest-induced insulin resistance. Diabetes 61:1090–1099
Damsbo P, Vaag A, Hother-Nielsen O, Beck-Nielsen H (1991) Reduced glycogen synthase activity in skeletal muscle from obese patients with and without type 2 (non-insulin-dependent) diabetes mellitus. Diabetologia 34:239–245
Ghanassia E, Brun JF, Fedou C, Raynaud E, Mercier J (2006) Substrate oxidation during exercise: type 2 diabetes is associated with a decrease in lipid oxidation and an earlier shift towards carbohydrate utilization. Diabetes Metab 32:604–610
Acknowledgements
We would like to thank L. Hansen, C. B. Olsen (Department of Endocrinology, Odense University Hospital, Denmark), J. B. Birk, B. Bolmgren, I. B. Nielsen and N. R. Andersen (Department of Nutrition, Exercise, and Sports, University of Copenhagen, Denmark) for their skilled technical assistance. Some of the data were presented as an abstract at the ADA meeting in 2014.
Funding
The study was supported by grants from the Danish Medical Research Council, the Danish Council for Independent Research (including Sapere Aude, DFF Starting Grant), the Novo Nordisk Foundation (including Excellence Grant 2009), the European Foundation for the Study of Diabetes (EFSD), and Odense University Hospital.
Duality of interest
MF is a shareholder of Novo Nordisk A/S. The remaining authors confirm there is no duality of interest associated with this manuscript.
Contribution statement
AJTP, KH and JFPW were responsible for the conception and design of the study. AJTP conducted the in vivo experiments and wrote the first version of the manuscript. JRH and MF conducted the laboratory experiments. AJTP, JRH MF, JMK and KH contributed to analysis of data. All contributed to the interpretation of the results, revised the manuscript and approved the final version. KH and JFPW are responsible for the integrity of the work as a whole.
Author information
Authors and Affiliations
Corresponding author
Additional information
Andreas J. T. Pedersen and Janne R. Hingst contributed equally to this study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM Methods
(PDF 68.8 kb)
ESM Fig. 1
(PDF 64 kb)
ESM Fig. 2
(PDF 93.3 kb)
Rights and permissions
About this article
Cite this article
Pedersen, A.J.T., Hingst, J.R., Friedrichsen, M. et al. Dysregulation of muscle glycogen synthase in recovery from exercise in type 2 diabetes. Diabetologia 58, 1569–1578 (2015). https://doi.org/10.1007/s00125-015-3582-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-015-3582-z