Abstract
Aims/hypothesis
Rapamycin impairs glucose tolerance and insulin sensitivity. Our previous study demonstrated that rapamycin significantly increases the production of gastric ghrelin, which is critical in the regulation of glucose metabolism. Here, we investigated whether ghrelin contributes to derangements of glucose metabolism induced by rapamycin.
Methods
The effects of rapamycin on glucose metabolism were examined in mice receiving ghrelin receptor antagonist or with Ghsr1a gene knockout. Changes in GLUT4, c-Jun N-terminal kinase (JNK) and phosphorylated ribosomal protein S6 (pS6) were investigated by immunofluorescent staining or western blotting. Related hormones were detected by radioimmunoassay kits.
Results
Rapamycin impaired glucose metabolism and insulin sensitivity not only in normal C57BL/6J mice but also in both obese mice induced by a high fat diet and db/db mice. This was accompanied by elevation of plasma acylated ghrelin. Rapamycin significantly increased the levels of plasma acylated ghrelin in normal C57BL/6J mice, high-fat-diet-induced obese mice and db/db mice. Elevation in plasma acylated ghrelin and derangements of glucose metabolism upon administration of rapamycin were significantly correlated. The deterioration in glucose homeostasis induced by rapamycin was blocked by d-Lys3-GHRP-6, a ghrelin receptor antagonist, or by deletion of the Ghsr1a gene. Ghrelin receptor antagonism and Ghsr1a knockout blocked the upregulation of JNK activity and downregulation of GLUT4 levels and translocation in the gastrocnemius muscle induced by rapamycin.
Conclusions/interpretation
The current study demonstrates that ghrelin contributes to derangements of glucose metabolism induced by rapamycin via altering the content and translocation of GLUT4 in muscles.
Similar content being viewed by others
Introduction
Ghrelin, a gastric 28 amino acid peptide hormone, is the endogenous ligand for the growth hormone secretagogue receptor (GHSR) [1]. Ghrelin is the only currently identified circulating hormone that is able to initiate food intake [2]. A variety of other physiological processes are known to be regulated by ghrelin in addition to ingestive behaviour, including effects on glucose metabolism [3]. Systemic administration of exogenous ghrelin has been reported to elevate blood glucose levels in humans [4] and rodents [5]. This effect is blocked by the ghrelin receptor antagonist, d-Lys3-growth-hormone-releasing peptide-6 (d-Lys3-GHRP-6) [5]. Deletion of the ghrelin gene in mice results in a phenotype with lower levels of circulating glucose and altered glucose tolerance upon exposure to a high fat diet [6]. Ghsr null mice fed a high fat diet demonstrate increased insulin sensitivity [7]. While both ghrelin and its receptor are expressed in human [8] and rat pancreatic islets [9], the mechanisms by which ghrelin produces these effects are unknown.
Rapamycin is a macrolide fungicide, first used as an immunosuppressant [10], which is also employed to explore the role of the mammalian target of rapamycin (mTOR) system in control of metabolic processes [11]. The mTOR signalling system is widely recognised to be operant in the hypothalamus where it is crucial to the central control of food intake [11–13]. Effects of rapamycin on blood glucose, serum triacylglycerol, NEFA and ketone bodies have also been reported in both animals and humans [14–16]. Chronic application of rapamycin has been associated with new-onset diabetes in patients with organ transplantation [17]. Impaired glucose tolerance and new-onset diabetes are among the most serious metabolic complications of solid organ transplantation [18, 19]. Increased risk of diabetes in transplant recipients is largely due to the immunosuppressive agents used to treat transplant recipients [20]. There are two mTOR complexes: mTORC1 and mTORC2. mTORC1 complex is sensitive to rapamycin and includes mTOR, regulatory associated protein of mTOR (raptor), mammalian LST8/G-protein β-subunit like protein (mLST8/GβL), proline-rich Akt substrate of 40 kDa (PRAS40) and DEP-domain-containing mTOR-interacting protein (DEPTOR). mTORC1 is involved in the anabolic effect of insulin through activation of ribosomal protein S6 kinase (S6K)1/2 and inhibition of translation initiation factor 4E binding protein (4E-BP)1 and 4E-BP2 [21]. In obesity and diabetes, mTORC1/S6K signalling is chronically activated [22]. This chronic activation promotes insulin resistance by a negative feedback mechanism involving serine phosphorylation and degradation of IRS1 as well as inhibition of IRS1 transcription [23, 24]. Several genetically modified mice have been engineered to study the implication of mTORC1 in the regulation of insulin sensitivity. S6k1 (also known as Rps6k1) knockout mice are protected against obesity and insulin resistance as a result of elevated energy expenditure and the loss of IRS1 serine phosphorylation by S6K1 [25, 26]. Global invalidation of 4E-BP1 and 4E-BP2 leads to the opposite phenotype [27]. Mice with adipose-specific raptor invalidation mainly recapitulate the phenotype of global S6k1 knockout mice [28]. These observations suggest that the mTOR signalling system may be an important factor in the regulation of glucose metabolism. While previous studies of mTOR signalling have extensively focused on insulin secretion by islet cells and its signalling pathways in the insulin targeted tissues, little has been known about its effect on hormones critical for energy metabolism. We have reported that the mTOR signalling system regulates gastric mucosal production of ghrelin [29, 30]. Systemic administration of the mTOR inhibitor rapamycin stimulated the transcription and translation of gastric ghrelin, increased circulating levels of ghrelin and stimulated feeding behaviour [30]. In the present study, we test the hypothesis that ghrelin plays a role in disordered glucose metabolism induced by rapamycin in normal and obese mice.
Methods
Materials
Rapamycin, mouse anti-glyceraldehyde-3-phosphate dehydrogenase (GAPDH) antibody and goat anti-mouse Texas Red-conjugated IgG were purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA). DMSO was from Sigma Chemical (St Louis, MO, USA). d-Lys3-GHRP-6 was from Phoenix Pharmaceuticals (Burlingame, CA, USA). Aprotinin was from Amersham Biosciences (Pittsburgh, PA, USA). Phosphorylated ribosomal protein S6 (pS6; ser235/236) rabbit antibody, S6 ribosomal mouse antibody, mouse anti-phospho-stress-activated protein kinase (SAPK)/c-Jun N-terminal kinase (JNK) (Thr183/Tyr185) and mouse anti-GLUT4 were from Cell Signaling Technology (Beverly, MA, USA). IRDye-conjugated affinity purified anti-rabbit and anti-mouse IgGs were purchased from Rockland (Gilbertsville, PA, USA). TRIzol reagent and the reverse transcription (RT) system were from Invitrogen (Carlsbad, CA, USA). Acylated ghrelin and insulin radioimmunoassay kits were from Linco Bioscience Institute (St Charles, MO, USA).
Animals and treatments
Animals
Twelve-week-old male C57BL/6J mice, high-fat-diet-induced obese (DIO) mice, Ghsr1a knockout mice and 12- to 16-week-old male db/db mice were used in the present study. Ghsr1a gene knockout mice in which exon 1 and exon 2 had been deleted were obtained from the Shanghai Research Center for Biomodel Organisms (Shanghai, People’s Republic of China) [31]. Deletion of the Ghsr1a gene fragment was confirmed by the absence of relative gene products examined by RT-PCR in the hypothalamus and skeletal muscle, in which Ghsr1a would be normally expressed. Mice were housed in standard plastic rodent cages and maintained in a regulated environment (24°C, 12 h light–dark cycle, with lights on at 07:00 hours). Regular chow and water were available ad libitum unless specified otherwise. In some experiments, rapamycin (1 mg/kg) or d-Lys3-GHRP-6 (10 μmol/kg) was injected i.p. for 6 days. Control animals received normal saline with the same concentration of DMSO (0.1%).
Diets
Where indicated, 4-week-old mice were assigned to receive standard laboratory chow or a high fat diet (45% fat, D12451; Research Diets, New Brunswick, NJ, USA) for 8 weeks. All animal protocols were approved by the Animal Care and Use Committee of Peking University.
Glucose tolerance test and insulin tolerance test
For the oral glucose tolerance tests, mice were fasted for 12 h before the gastric administration of glucose (3 g/kg body weight) by gavage. For insulin tolerance tests, mice were fasted for 4 h, followed by i.p. injection of insulin at a dose of 1 U/kg. Blood was drawn from a cut at the tip of the tail at 0, 30, 60, 90 and 120 min, and glucose concentrations were detected immediately with Glucotrend from Roche Diagnostics (Mannheim, Germany) according to the manufacturer’s instructions.
Tissue sample preparations and immunofluorescent analysis
C57BL/6J mice were deeply anaesthetised using pentobarbital, and perfused transcardially with 20 ml 0.1 mol/l PBS (pH 7.4), followed by 20 ml 4% paraformaldehyde in PBS. The gastrocnemius muscle and pancreas were quickly removed and rinsed thoroughly with PBS. The tissues were postfixed in 4% paraformaldehyde, dehydrated, embedded in wax and sectioned at 6 μm. Paraffin-embedded sections were de-waxed, rehydrated and rinsed in PBS. After boiling for 10 min in 0.01 mol/l sodium citrate buffer (pH 6.0), tissue sections were blocked in 5% goat pre-immune serum or 1% BSA in PBS for 1 h at room temperature, then incubated overnight with mouse monoclonal antibody to GLUT4 (1:100) or mouse anti-phospho-SAPK/JNK (Thr183/Tyr185) (1:400) (for gastrocnemius muscle) and goat anti-insulin (1:100) (for pancreas) antibodies. Tissue sections were then incubated at room temperature for 1 h with the following secondary antibodies: goat anti-mouse Texas Red-conjugated IgG or donkey anti-goat Texas Red-conjugated IgG (1:100). Controls included substituting primary antibodies with mouse or goat IgG. Computerised image analysis (Model Leica Q550CW, Leica, Qwin, Germany) was performed to quantify the immunostaining signals of GLUT4 and phospho-SAPK/JNK (Thr183/Tyr185) from mouse gastrocnemius muscle or insulin from pancreas.
Measurements of plasma acyl ghrelin and insulin
Blood samples were immediately transferred to chilled polypropylene tubes containing EDTA-2Na (1 mg/ml) and aprotinin (1,000 U/ml) and centrifuged at 4°C. The plasma was separated and stored at −70°C before use. Acylated ghrelin and insulin were measured using radioimmunoassay kits according to the manufacturer’s instructions. Concentrated HCl was added to the plasma to a final concentration of 0.1 mmol/l and the acidified plasma was diluted with an equal volume of 0.9% NaCl solution. The anti-acylate ghrelin antiserum or anti-insulin antibody were used at final dilutions of 1/100,000. All assays were performed in duplicate.
Cell culture, transfection, treatment and immunofluorescent staining
C2C12 cells were maintained in DMEM containing 4.5 g/l glucose supplemented with 10% FBS. Cells were then transfected with haemagglutinin (HA)-GLUT4 (4 μg) or GFP (4 μg) using Lipofectamine reagent (Invitrogen, Grand Island, NY, USA) according to the manufacturer’s instructions. After transfection, cells were switched to differentiation medium containing DMEM supplemented with 2% fetal calf serum, 1% penicillin-streptomycin, 1% sodium pyruvate and 1% glutamine. After 6 days of culture, cells were treated with ghrelin (10 nmol/l for 30 min), d-Lys3-GHRP-6 (1 μmol/l for 30 min), insulin (10 nmol/l for 10 min) or d-Lys3-GHRP-6 added 5 min before ghrelin and/or insulin stimulation.
After treatment, cells were washed with PBS, fixed with 3.7% paraformaldehyde for 10 min at room temperature, then treated with 0.1% Triton X-100 in PBS for 5 min. After thorough washing, cells were blocked with 1% BSA in PBS for 30 min. Cells were next incubated with the mouse anti-HA Tag primary antibody (1:1,000) overnight at 4°C, washed with PBS, then incubated with goat-anti-mouse Texas Red-conjugated IgG (1:100) for 1.5 h in the dark. Nuclei were visualised by staining with Hoechst 33254 for 15 min. Cells were mounted with 90% glycerol-PBS media and examined by confocal laser scanning microscopy (Leica). Computerised image analysis (Leica Q550CW) was performed to quantify the immunostaining signals of HA-GLUT4.
Western blot analysis
Gastric fundus and gastrocnemius muscle were isolated and homogenised in lysis buffer. Proteins were subjected to SDS-PAGE with a 10% running gel, then transferred to a polyvinylidene fluoride membrane. Membranes were incubated for 1 h at room temperature with 5% fat-free milk in Tris buffered saline containing Tween 20, followed by incubation overnight at 4°C with primary antibodies. Specific reaction was detected using IRDye-conjugated second antibody and visualised using the Odyssey infrared imaging system (LI-COR Biosciences, Lincoln, NE, USA).
RT-PCR
Total RNA was isolated from mouse hypothalamus and gastrocnemius muscle using TRIzol reagent. RT was performed using the RT system according to the manufacturer’s instructions. The PCR programme was as follows: hold at 95°C for 5 min, then 95°C for 30 s, 60°C for 30 s and 72°C for 1 min for 35 cycles. The nucleotide sequences of sense and antisense primers used are listed in the electronic supplementary material (ESM) Table 1.
A 20 μl aliquot of the RT-PCR samples was loaded onto 1.5% agarose gel. For negative controls, PCR reactions were performed for the primer pairs in the absence of transcript.
Statistical analysis
Data were expressed as mean ± SEM and analysed by repeated-measures ANOVA, one-way ANOVA, the Student–Newman–Keuls test (comparisons between multiple groups), or unpaired Student’s t test (between two groups) as appropriate, using GraphPad Prism software. p < 0.05 was considered significant. Pearson’s correlation analysis was performed to determine the strength of the linear relationship between plasma concentration of acylated ghrelin and derangements of glucose metabolism or insulin resistance induced by rapamycin expressed as total AUC.
Results
Hyperglycaemia, derangements of glucose metabolism and hyperghrelinaemia induced by rapamycin
Because we have previously demonstrated that the mTOR signalling pathway is important in ghrelin production and secretion [30], studies were performed using the mTOR pathway inhibitor rapamycin. Mice treated with rapamycin demonstrated hyperglycaemia, impaired glucose metabolism and glucose disposal curves typifying insulin resistance. These alterations were observed in normal C57BL/6J mice, as well as in DIO mice and db/db obese mice (Fig. 1a–f). Disturbances of glucose homeostasis were accompanied by elevations in plasma acyl ghrelin. Significant increases of plasma acyl ghrelin in response to rapamycin administration were observed in normal C57BL/6J mice (27.6 ± 2.7 to 42.1 ± 5.8 pmol/l, p < 0.05), in DIO mice (15.0 ± 1.4 to 22.0 ± 1.3 pmol/l, p < 0.01) and in db/db mice (20.0 ± 1.5 to 27.8 ± 2.3 pmol/l, p < 0.05; Fig. 1g–i). Pearson’s analysis demonstrated positive correlations between plasma acyl ghrelin and rapamycin-induced derangements of glucose metabolism and insulin sensitivity in normal C57BL/6J mice (r = 0.922 and 0.925, respectively, p < 0.01), DIO obese mice (r = 0.943 and 0.960, respectively, p < 0.01) and db/db obese mice (r = 0.857and 0.907, respectively, p < 0.01). Systemic administration of rapamycin significantly decreased the phosphorylation of S6 protein, a downstream target of mTOR signalling, in the gastric fundus (Fig. 1j–l).
Hyperglycaemia, derangements of glucose metabolism and hyperghrelinaemia induced by rapamycin (grey squares) and not by DMSO control (black squares). Oral glucose tolerance tests for normal C57BL/6J mice (a), DIO mice (b) and db/db mice (c). Insulin tolerance tests for normal (d), DIO (e) and db/db (f) mice. Plasma acyl ghrelin levels for normal (g), DIO (h) and db/db (i) mice following administration of rapamycin (Rapa) or control (DMSO). Western blot analysis of gastric S6 and phospho-S6 levels in normal (j), DIO (k) and db/db (l) mice. Data are expressed as mean ± SEM; six mice were examined for each condition. *p < 0.05 vs control mice
Effect of ghrelin receptor antagonism on rapamycin-induced impairment of glucose metabolism
If elevation in plasma acyl ghrelin is mechanistically linked to derangements of glucose metabolism induced by rapamycin, blockade of acyl ghrelin activity would be predicted to reverse the effects of rapamycin. The effects of d-Lys3-GHRP-6, a GHSR1a antagonist, were examined in C57BL/6J mice. Twelve-week-old male C57BL/6J mice were divided into four groups and received the following treatments for 6 days: control (DMSO), rapamycin (1 mg/kg i.p.), d-Lys3-GHRP-6 (10 μmol/kg i.p.) or d-Lys3-GHRP-6, administered 2 min before rapamycin. As shown in Fig. 2a and b, d-Lys3-GHRP-6 blocked the effects of rapamycin on oral glucose tolerance and on insulin sensitivity even though plasma acyl ghrelin levels were significantly higher relative to controls (Fig. 2g).
Effect of ghrelin receptor antagonism or Ghsr1a knockout on rapamycin-induced impairment of glucose metabolism. Results of OGTT (a) and ITT (b) in male C57BL/6J mice receiving DMSO (black circles), rapamycin (Rapa; 1 mg/kg, white circles), d-Lys3-GHRP-6 (GHRP6; 10 μmol/kg, black triangles) or d-Lys3-GHRP-6 plus rapamycin (grey triangles). * p < 0.05 vs DMSO, OGTT (c) and ITT (d) in wild-type (WT) receiving DMSO (solid line, black circles), rapamycin (Rapa; 1 mg/kg, solid line, white circles) and Ghsr1a null mice receiving DMSO (dashed line, black triangles), rapamycin (Rapa; 1 mg/kg, dashed line, grey triangles) fed a normal chow diet. OGTT (e) and ITT (f) in WT (solid lines, black circles for DMSO and white circles for Rapa) and Ghsr1a null mice (dashed lines, black triangles for DMSO and grey triangles for Rapa) fed a high fat diet for 8 weeks. * p < 0.05 vs WT receiving DMSO. (g) Plasma acyl ghrelin levels in C57BL/6J mice receiving DMSO, rapamycin, d-Lys3-GHRP-6 or d-Lys3-GHRP-6 plus rapamycin. * p < 0.05 vs DMSO. (h) Plasma acyl ghrelin levels in WT and Ghsr1a knockout mice receiving DMSO or rapamycin. * p < 0.05 vs DMSO. (i) Western blot results for gastric pS6 and gastric total S6 in the presence of various treatments. Results are expressed as mean ± SEM. Six mice were examined for each condition. * p < 0.05 vs control, † p < 0.05 vs d-Lys3-GHRP-6 treatment. Western blot for gastric pS6 and gastric S6 for WT and Ghsr1a knockout mice receiving DMSO or rapamycin in the presence of normal chow diet (NCD) (j) or high fat diet (HFD) (k). Results are expressed as mean ± SEM. Six mice were examined for each condition. *p < 0.05 vs control mice, † p < 0.05 vs Ghsr1a knockout mice without rapamycin administration. Total AUCs are calculated with y values set as zero. Results are expressed as mean ± SEM. *p < 0.05 vs control (DMSO) mice
Effect of Ghsr1a knockout on rapamycin-induced alterations in glucose metabolism
To further confirm that ghrelin contributes to disturbance of glucose metabolism induced by rapamycin, a Ghsr1a gene knockout mouse model was used. When fed standard chow, rapamycin caused significant shifts in oral glucose tolerance and insulin sensitivity curves in wild-type littermates, but not in Ghsr1a gene knockout mice (Fig. 2c, d). These changes were proportionately greater in animals maintained on a high fat diet (Fig. 2e, f). Rapamycin-induced derangements of glucose metabolism and insulin sensitivity were significantly less severe in Ghsr1a knockout mice relative to wild-type littermates (Fig. 2e, f) although similar trends were shown in changes in ghrelin levels after glucose administration (ESM Fig. 1a).
Consistent with these observations, rapamycin stimulated food intake only in wild-type littermates but not in Ghsr1a null mice (ESM Fig. 2a–c) despite similar elevations in plasma acylated ghrelin for both Ghsr1a null mice (34.7 ± 2.5 pg/ml for DMSO vs 43.3 ± 2.1 pmol/l for rapamycin, p < 0.05) and wild-type littermates (27.3 ± 5.7 pg/ml for DMSO control vs 43.8 ± 1.6 pmol/l for rapamycin, p < 0.05) when fed with standard chow (Fig. 2h). Rapamycin abolished S6 phosphorylation despite concurrent administration of d-Lys3-GHRP-6 or Ghsr1a gene deletion (Fig. 2i–k).
Effects on insulin secretion and islet cells
No significant difference in plasma insulin was observed in mice treated with rapamycin in either control mice (70.42 ± 7.744 vs 67.43 ± 8.07 pmol/l, p = 0.8) or d-Lys3-GHRP-6-treated mice (161.3 ± 37.44 vs 142.4 ± 32.3 pmol/l, p = 0.7; ESM Fig. 3a). Similarly, no significant difference in plasma insulin was observed in mice treated with rapamycin relative to control in either wild-type littermates (91.78 ± 11.05 vs 122.9 ± 17.83 pmol/l, p = 0.2) or Ghsr1a gene knockout mice (226.2 ± 49.15 vs 151.7 ± 24.86 pmol/l, p = 0.2) (ESM Fig. 3b). Furthermore, similar trends in change were shown in insulin levels after glucose administration (ESM Fig. 1b). Analysis of pancreatic islets by haematoxylin and eosin staining and immunofluorescent staining showed no significant difference in islet morphology (ESM Fig. 4) and islet insulin immunoreactivity (ESM Fig. 5) between mice treated with or without rapamycin. This observation suggests that islet morphology and function are not significantly altered by rapamycin.
Ghrelin receptor and JNK phosphorylation
Because the stress-responsive JNK pathway in muscle may account for insulin resistance induced by rapamycin [18], we next examined the effect of ghrelin receptor antagonism on JNK phosphorylation in gastrocnemius muscle. As shown in Fig. 3a, rapamycin significantly increased levels of phosphorylated JNK. Pretreatment of mice with d-Lys3-GHRP-6 to block the ghrelin receptor markedly attenuated upregulation of JNK induced by rapamycin. The role of ghrelin in the regulation of JNK phosphorylation induced by rapamycin was further examined in Ghsr1a null mice. As shown in Fig. 3c, rapamycin failed to increase phosphorylation of JNK in gastrocnemius muscle of Ghsr1a null mice, while wild-type littermates remained sensitive to the effects of this agent.
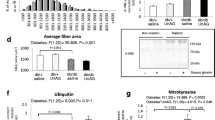
Effect of ghrelin receptor antagonism or Ghsr1a knockout on JNK activity in skeletal muscle. a Immunofluorescent staining for phospho-JNK (pJNK; red) in gastrocnemius muscle from mice treated with DMSO, rapamycin (Rapa; 1 mg/kg), d-Lys3-GHRP-6 (10 µmoL/kg) or d-Lys3-GHRP-6 plus rapamycin for 6 days. Nuclei were stained with Hoechst dye. Controls included substituting primary antibodies with mouse IgG. Representative results from six individual experiments are shown. The middle panels are results from mice treated with insulin (2 U/kg, i.p.) 10 min before harvest of tissues. b, Fluorescent area and intensity of JNK staining were measured to quantify changes in phospho-JNK and expressed as mean ± SEM. Representative results from six individual experiments are shown. *p < 0.05 vs DMSO. c Immunofluorescent staining for phospho-JNK (red) in gastrocnemius muscle derived from Ghsr1a gene null mice or wild-type (WT) littermates treated with DMSO or rapamycin (1 mg/kg). d Fluorescent area and intensity of JNK staining were measured to quantify changes in phospho-JNK and expressed as mean ± SEM. Representative results from six individual experiments are shown. *p < 0.05 vs WT receiving DMSO
Effect of ghrelin receptor antagonism and Ghsr1a knockout on glucose transport in muscle
Glucose transport into most tissues occurs through the action of members of a family of facilitative diffusion glucose transport proteins designated as GLUT1–5 and 7. GLUT1 is ubiquitously distributed and has been proposed to act as a constitutive transport protein. In contrast, the GLUT4 isoform is expressed almost exclusively in adipose cells and gastrocnemius muscle and is responsible for insulin-stimulated glucose transport [32–34]. As shown in Fig. 4a, rapamycin inhibited gastrocnemius muscle GLUT4 membrane translocation, both in the basal status and after insulin injection, while ghrelin antagonism rescued the suppression of GLUT4 translocation induced by rapamycin. As shown in Fig. 4c, experiments using Ghsr1a knockout mice confirmed that ghrelin suppresses GLUT4 translocation induced by rapamycin. The average area and intensity of GLUT4 staining signals were nearly unaffected by rapamycin in Ghsr1a null mice, while significant reductions in these variables were observed in wild-type mice. Similar results were also observed in C2C12 myocytes transfected with HA-Glut4 (ESM Fig. 6).
Effect of ghrelin receptor antagonism or Ghsr1a knockout on glucose transport in skeletal muscle. a Immunofluorescent staining for GLUT4 (red) in gastrocnemius muscle derived from mice treated with DMSO, rapamycin (Rapa; 1 mg/kg), d-Lys3-GHRP-6 (10 µmoL/kg) or d-Lys3-GHRP-6 plus rapamycin for 6 days. Nuclei were stained with Hoechst dye. Controls included substituting primary antibodies with mouse IgG. Representative results from six individual experiments are shown. The middle panels are results from mice treated with insulin (2 U/kg, i.p.) 10 min before harvest of tissues. b Fluorescent area and intensity of GLUT4 staining in gastrocnemius muscle membrane were measured to quantify GLUT4 and expressed as mean ± SEM. Representative results from six individual experiments are shown. *p < 0.05 vs DMSO. c Images depict immunofluorescent staining for GLUT4 (red) in gastrocnemius muscle derived from Ghsr1a knockout mice or wild-type (WT) littermates treated with DMSO or rapamycin (1 mg/kg). d Fluorescent area and intensity of GLUT4 staining in gastrocnemius muscle membrane were measured to quantify GLUT4 and expressed as mean ± SEM. Representative results from six individual experiments are shown. *p < 0.05 vs WT receiving DMSO
Expression of ghrelin receptor in muscle
Des-acyl ghrelin failed to significantly alter blood glucose levels, which indicates that ghrelin increases blood glucose via a specific interaction with GHSR1a [35]. Thus the relative tissue distribution of Ghsr1a mRNA and protein were examined. High levels of Ghsr1a mRNA were detected in the hypothalamus and gastrocnemius muscle in wild-type mice, but not in Ghsr1a null mice (Fig. 5).
Expression of Ghsr1a mRNA. Ghsr1a mRNA was detected by RT-PCR using total RNA extracted from various mouse tissues as described in the Methods section. Gapdh mRNA was used as an internal control. The negative control used reaction product without RT. The results of four individual experiments are shown
Discussion
The major finding of this study is that an increased concentration of ghrelin contributes to derangements of glucose metabolism induced by rapamycin. These effects were induced by exposure to rapamycin, indicating a critical role of the mTOR signalling system in ghrelin secretion and glucose homeostasis. This general conclusion is supported by the following observations: (1) there exists a positive correlation between circulating plasma acyl ghrelin levels and derangements of glucose metabolism induced by rapamycin; (2) either ghrelin receptor antagonism or Ghsr1a knockout improves derangements of glucose metabolism induced by rapamycin; (3) upregulation of JNK phosphorylation induced by rapamycin is blocked by ghrelin receptor antagonism or gene deletion; (4) ghrelin receptor antagonism or gene deletion stimulates GLUT4 expression and translocation, and blocks the suppression of GLUT4 induced by rapamycin; (5) ghrelin receptor antagonism and Ghsr1a deletion inhibits gastrocnemius muscle JNK activity; and (6) ghrelin decreases membrane GLUT4 in differentiated C2C12 cells, while ghrelin receptor antagonism significantly increases the amount of GLUT4 under either basal condition or insulin stimulation.
The mTOR signalling system is regulated independently by insulin, amino acids and energy sufficiency [36]. It integrates signals from growth factors, hormones and nutrients, and cellular energy levels to regulate processes as diverse as protein translation, cell growth, proliferation and survival [36]. mTOR is therefore a critical molecule linking many cellular activities with overall energy status at the organism level [13]. Several lines of evidence suggest that dysregulated mTOR signalling may link nutrient excess with obesity and insulin resistance. Aberrant mTOR activity has been reported during the development of obesity and diabetes [37]. Significant elevation of mTOR signalling has been observed in the liver and skeletal muscle of insulin-resistant obese rats maintained on a high fat diet [22]. In vitro experiments have demonstrated that mTOR signalling may operate a negative feedback loop toward phosphoinositide 3 (PI3)-kinase/Akt by increasing inhibitory serine phosphorylation of IRS-1 [38]. Studies by Bell et al suggest that rapamycin has deleterious effects on min-6 cells, and rat or human islets [15]. Our study confirms that systemic rapamycin causes hyperglycaemia in normal mice and worsens hyperglycaemia in both DIO mice and db/db obese mice.
The mechanism underlying rapamycin-induced hyperglycaemia is complicated and may involve both insulin secretion from pancreatic islet cells and insulin sensitivity in the liver, muscle or adipose tissue [6]. While rapamycin has been associated with an increase in apoptosis in pancreatic beta cells and reduction in beta cell mass, insulin secretion has also been reported to be unchanged in rats or in cultured islet cells [18]. Our study shows that rapamycin does not alter levels of serum insulin, islet morphology or islet insulin immunoreactivity, suggesting that hyperglycaemic effects may rather involve impaired glucose metabolism in insulin-sensitive tissues. Skeletal muscle is a major site of glucose uptake after insulin administration. Insulin stimulation leads to an uptake of glucose through Akt-mediated translocation of GLUT-4 to the cell surface [39]. Our study provides evidence that skeletal muscle is one of the main targets of rapamycin and contributes to the derangements of glucose metabolism induced by this agent. Upon treatment with rapamycin, skeletal muscle showed a marked increase in JNK phosphorylation, and a significant reduction in GLUT4 membrane expression.
The evidence as to whether rapamycin exerts its effect on skeletal muscle by a direct or indirect mechanism is conflicting. Studies by Tremblay and Marette show that rapamycin acts directly on cultured skeletal muscle to prevent the insulin-resistant effects of nutrient excess on insulin-mediated glucose transport [38]. The current study reveals a novel mechanism for rapamycin-induced derangements of glucose metabolism. This study demonstrates that ghrelin contributes to the development of derangements of glucose metabolism induced by rapamycin. Hyperglycaemia induced by rapamycin was highly correlated with levels of plasma acylated ghrelin in both lean mice and obese animals. Rapamycin-induced derangements of glucose metabolism were blocked by ghrelin receptor antagonism or Ghsr1a knockout. Increase of JNK phosphorylation induced by rapamycin in skeletal muscle was significantly attenuated by ghrelin receptor antagonism or Ghsr1a knockout. In addition, ghrelin receptor antagonism or Ghsr1a gene deletion reversed the downregulation of GLUT4 induced by rapamycin in skeletal muscle. Together with our previous report [30] that rapamycin inhibits mTOR signalling in gastric mucosa and stimulates transcription and translation of ghrelin, this study indicates that rapamycin may act on the stomach to regulate the production of acylated ghrelin, which, in turn, causes impairment of glucose transport in skeletal muscle. While direct evidence is still absent and requires the conditional deletion of mTOR signalling molecules in gastric ghrelin secreting cells, a line of findings [30] supports the direct effect of rapamycin on gastric ghrelin secreting cells: (1) mTOR signalling molecules are selectively expressed in gastric ghrelin secreting cells and mTOR activity is reciprocally related to energy levels; (2) a reciprocal relationship exists between gastric mTOR activity and the production and secretion of ghrelin during changes in energy status; (3) inhibition of gastric mTOR signalling leads to increased production of ghrelin and circulating ghrelin, while activation of gastric mTOR signalling suppresses its production and secretion; and (4) overexpression of mTOR decreases ghrelin promoter activity, while blocking mTOR signalling by tuberous sclerosis protein (TSC)1 or TSC2 increases its activity.
In addition to its orexigenic effect, ghrelin plays an important role in the regulation of glucose homeostasis [6]. Previous studies have demonstrated that ghrelin is able to suppress insulin secretion in several in vitro experimental models, including rodent islets [5], pancreatic cell lines [40] and perfused rat pancreas [41]. Ghrelin receptor antagonism or neutralisation of endogenous ghrelin significantly increases insulin release from perfused pancreas [5]. Ghrelin deficiency in ob/ob mice causes enhanced insulin secretion and improved insulin sensitivity [42]. Blockade of pancreatic islet-derived ghrelin enhances insulin secretion to prevent glucose intolerance in mice fed a high fat diet [7]. Ghrelin gene knockout mice demonstrate a significant increase in plasma insulin and a marked reduction of blood glucose levels [6]. In addition, the number of ghrelin-positive epsilon (ε) cells is greater in transgenic mouse models lacking functional Nkx2-2, Pax6 or Pax4, with reciprocal beta cell deficiency [43]. Taken together, these studies suggest that ghrelin may alter glucose homeostasis by modulating the secretion of insulin. Our study demonstrates, in addition, that endogenous ghrelin may contribute to derangements of glucose metabolism by impairing glucose transport in the skeletal muscle. While ghrelin has been shown to exercise its effect on energy metabolism via a central mechanism [3, 44], our study suggests that ghrelin may directly act through its receptor on myocytes to regulate their glucose transportation. These data are consistent with previous reports demonstrating that ghrelin regulates the differentiation of myocytes [45] and that acylation is critical for the effect of ghrelin on myogenesis [46]. Other studies may limit the validity of this conclusion. The existence of a novel ghrelin receptor subtype has been reported [2]. While the involvement of a novel ghrelin receptor other than GHSR1a in the rapamycin-induced derangements of glucose metabolism cannot be completely excluded, the following evidence indicates that ghrelin increases blood glucose via specific interaction with GHSR1a. The novel ghrelin receptor, if it exists, is activated by des-acyl ghrelin, which demonstrates no effect on blood glucose levels [35]. In addition, both circulating and duodenal lipids have been shown to regulate glucose homeostasis by activating neurons in the hypothalamus and/or midbrain, which subsequently inhibit glucose production in the liver [47]. These effects are probably mediated by protein kinase C [48, 49]. Since ghrelin has been reported to stimulate food intake by activation of its receptor in the hypothalamus, the possibility that ghrelin acts through a central neuronal mechanism to regulate hepatic glucose production and therefore mediates the effect of rapamycin-induced glucose dysfunction cannot be excluded.
In summary, our study demonstrates that direct modulation of acylated ghrelin secretion is a crucial mechanism accounting for the derangements of glucose metabolism induced by rapamycin. Antagonism of ghrelin may therefore provide a potential therapeutic strategy for new-onset diabetes mellitus associated with rapamycin treatment after transplantation.
Abbreviations
- 4E-BP:
-
Translation initiation factor 4E binding protein
- DIO:
-
High-fat-diet-induced obese [mice]
- D-Lys3-GHRP-6:
-
D-Lys3-growth-hormone-releasing peptide 6
- GAPDH:
-
Glyceraldehyde-3-phosphate dehydrogenase
- GHSR:
-
Growth hormone secretagogue receptor
- HA:
-
Haemagglutinin
- JNK:
-
c-Jun N-terminal kinase
- mTOR:
-
Mammalian target of rapamycin
- pS6:
-
Phosphorylated ribosomal protein S6
- Raptor:
-
Regulatory associated protein of mTOR
- RT:
-
Reverse transcription
- S6K:
-
S6 kinase
- SAPK:
-
Stress-activated protein kinase
- TSC:
-
Tuberous sclerosis protein
References
Kojima M, Hosoda H, Date Y, Nakazato M, Matsuo H, Kangawa K (1999) Ghrelin is a growth-hormone-releasing acylated peptide from stomach. Nature 402:656–660
Cummings DE, Foster-Schubert KE, Overduin J (2005) Ghrelin and energy balance: focus on current controversies. Curr Drug Targets 6:153–169
Kojima M, Kangawa K (2005) Ghrelin: structure and function. Physiol Rev 85:495–522
Vestergaard ET, Gormsen LC, Jessen N et al (2008) Ghrelin infusion in humans induces acute insulin resistance and lipolysis independent of growth hormone signaling. Diabetes 57:3205–3210
Dezaki K, Hosoda H, Kakei M et al (2004) Endogenous ghrelin in pancreatic islets restricts insulin release by attenuating Ca2+ signaling in beta-cells: implication in the glycemic control in rodents. Diabetes 53:3142–3151
Dezaki K, Sone H, Koizumi M et al (2006) Blockade of pancreatic islet-derived ghrelin enhances insulin secretion to prevent high-fat diet-induced glucose intolerance. Diabetes 55:3486–3493
Zigman JM, NakanoY CR et al (2005) Mice lacking ghrelin receptors resist the development of diet-induced obesity. J Clin Invest 115:3564–3572
Ueberberg B, Unger N, Saeger W, Mann K, Petersenn S (2009) Expression of ghrelin and its receptor in human tissues. Horm Metab Res 41:814–821
An W, Li Y, Xu G et al (2010) Modulation of ghrelin O-acyltransferase expression in pancreatic islets. Cell Physiol Biochem 26:707–716
Abraham RT, Wiederrecht GJ (1996) Immunopharmacology of rapamycin. Annu Rev Immunol 14:483–510
Polak P, Hall MN (2009) mTOR and the control of whole body metabolism. Curr Opin Cell Biol 21:209–218
Kahn BB, Myers MG Jr (2006) mTOR tells the brain that the body is hungry. Nat Med 12:615–617
Cota D, Proulx K, Smith KA et al (2006) Hypothalamic mTOR signaling regulates food intake. Science 312:927–930
Houde VP, Brule S, Festuccia WT et al (2010) Chronic rapamycin treatment causes glucose intolerance and hyperlipidemia by upregulating hepatic gluconeogenesis and impairing lipid deposition in adipose tissue. Diabetes 59:1338–1348
Bell E, Cao X, Moibi JA et al (2003) Rapamycin has a deleterious effect on MIN-6 cells and rat and human islets. Diabetes 52:2731–2739
Fraenkel M, Ketzinel-Gilad M, Ariav Y et al (2008) mTOR inhibition by rapamycin prevents beta-cell adaptation to hyperglycemia and exacerbates the metabolic state in type 2 diabetes. Diabetes 57:945–957
Johnston O, Rose CL, Webster AC, Gill JS (2008) Sirolimus is associated with new-onset diabetes in kidney transplant recipients. J Am Soc Nephrol 19:1411–1418
Friedman EA, Shyh TP, Beyer MM, Manis T, Butt KM (1985) Posttransplant diabetes in kidney transplant recipients. Am J Nephrol 5:196–202
Kasiske BL, Snyder JJ, Gilbertson D, Matas AJ (2003) Diabetes mellitus after kidney transplantation in the United States. Am J Transplant 3:178–185
Rodrigo E, Fernandez-Fresnedo G, Valero R et al (2006) New-onset diabetes after kidney transplantation: risk factors. J Am Soc Nephrol 17:S291–S295
Ma XM, Blenis J (2009) Molecular mechanisms of mTOR-mediated translational control. Nat Rev Mol Cell Biol 10:307–318
Khamzina L, Veilleux A, Bergeron S, Marette A (2005) Increased activation of the mammalian target of rapamycin pathway in liver and skeletal muscle of obese rats, possible involvement in obesity-linked insulin resistance. Endocrinology 146:1473–1481
Harrington LS, Findlay GM, Gray A et al (2004) The TSC1-2 tumor suppressor controls insulin-PI3K signaling via regulation of IRS proteins. J Cell Biol 166:213–223
Shah OJ, Wang Z, Hunter T (2004) Inappropriate activation of the TSC/ Rheb/mTOR/S6K cassette induces IRS1/2 depletion, insulin resistance, and cell survival deficiencies. Curr Biol 14:1650–1656
Um SH, Frigerio F, Watanabe M et al (2004) Absence of S6K1 protects against age- and diet-induced obesity while enhancing insulin sensitivity. Nature 431:200–205
Tremblay F, Brule S, Hee Um S et al (2007) Identification of IRS-1 Ser-1101 as a target of S6K1 in nutrient- and obesity-induced insulin resistance. Proc Natl Acad Sci U S A 104:14056–14061
Le Bacquer O, Petroulakis E, Paglialunga S et al (2007) Elevated sensitivity to diet-induced obesity and insulin resistance in mice lacking 4E-BP1 and 4EBP2. J Clin Invest 117:387–396
Polak P, Cybulski N, Feige JN, Auwerx J, Ruegg MA, Hall MN (2008) Adipose-specific knockout of raptor results in lean mice with enhanced mitochondrial respiration. Cell Metab 8:399–410
Xu G, Li Y, An W et al (2010) Regulation of gastric hormones by systemic rapamycin. Peptides 31:2185–2192
Xu G, Li Y, An W et al (2009) Gastric mammalian target of rapamycin signaling regulates ghrelin production and food intake. Endocrinology 150:3637–3644
Wang W, Wang Z, Zhang Y, Fei J, Zheng Q (2008) Generation of mouse embryonic stem cell clones for ghrelin receptor gene knock out. Chin J Bases Clin General Surg 15:733–736
Marette A, Richardson JM, Ramlal T et al (1992) Abundance, localization, and insulin-induced translocation of glucose transporters in red and white muscle. Am J Physiol 263:C443–C452
James DE, Strube M, Mueckler M (1989) Molecular cloning and characterization of an insulin-regulatable glucose transporter. Nature 338:83–87
Slot JW, Geuze HJ, Gigengack S, James DE, Lienhard GE (1991) Translocation of the glucose transporter GLUT4 in cardiac myocytes of the rat. Proc Natl Acad Sci U S A 88:7815–7819
Dezaki K, Sone H, Yada T (2008) Ghrelin is a physiological regulator of insulin release in pancreatic islets and glucose homeostasis. Pharmacol Ther 118:239–249
Yang Q, Guan KL (2007) Expanding mTOR signaling. Cell Res 17:666–681
Dann SG, Selvaraj A, Thomas G (2007) mTOR Complex1-S6K1 signaling: at the crossroads of obesity, diabetes and cancer. Trends Mol Med 13:252–259
Tremblay F, Marette A (2001) Amino acid and insulin signaling via the mTOR/p70 S6 kinase pathway. A negative feedback mechanism leading to insulin resistance in skeletal muscle cells. J Biol Chem 276:38052–38060
Santos JM, Ribeiro SB, Gaya AR, Appell HJ, Duarte JA (2008) Skeletal muscle pathways of contraction-enhanced glucose uptake. Int J Sports Med 29:785–794
Wang Y, Nishi M, Doi A et al (2010) Ghrelin inhibits insulin secretion through the AMPK-UCP2 pathway in beta cells. FEBS Lett 584:1503–1508
Egido EM, Rodriguez-Gallardo J, Silvestre RA, Marco J (2002) Inhibitory effect of ghrelin on insulin and pancreatic somatostatin secretion. Eur J Endocrinol 146:241–244
Sun Y, Asnicar M, Saha PK, Chan L, Smith RG (2006) Ablation of ghrelin improves the diabetic but not obese phenotype of ob/ob mice. Cell Metab 3:379–386
Prado CL, Pugh-Bernard AE, Elghazi L, Sosa-Pineda B, Sussel L (2004) Ghrelin cells replace insulin-producing beta cells in two mouse models of pancreas development. Proc Natl Acad Sci U S A 101:2924–2929
Perez-Tilve D, Hofmann SM, Basford J et al (2010) Melanocortin signaling in the CNS directly regulates circulating cholesterol. Nat Neurosci 13:877–882
Filigheddu N, Gnocchi VF, Coscia M et al (2007) Ghrelin and des-acyl ghrelin promote differentiation and fusion of C2C12 skeletal muscle cells. Mol Biol Cell 18:986–994
Zhang W, Zhao L, Mulholland MW (2007) Ghrelin stimulates myocyte development. Cell Physiol Biochem 20:659–664
Wang PY, Caspi L, Lam CK et al (2008) Upper intestinal lipids trigger a gut-brain-liver axis to regulate glucose production. Nature 452:1012–1016
Kokorovic A, Cheung GW, Breen DM, Chari M, Lam CK, Lam TK (2011) Duodenal mucosal protein kinase C-δ regulates glucose production in rats. Gastroenterology 141:1720–1727
Ross R, Wang PY, Chari M et al (2008) Hypothalamic protein kinase C regulates glucose production. Diabetes 57:2061–2065
Funding
This work was supported by grants from the National Natural Science Foundation of China (81030012, 81170795, 30971434, 30871194, 30890043 and 30971085) the Major National Basic Research Program of the People’s Republic of China (No. 2010CB912504) and National Institute of Health grant RO1DK043225.
Contribution statement
GX, ZL and HT performed the experiments and analysed data; all authors contributed to the design of the experiments, interpretation of data and the writing of the manuscript. GX, ZL, MM and WZ revised the manuscript. All the authors approved the final version of the paper.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Author information
Authors and Affiliations
Corresponding authors
Electronic Supplementary Materials
Below is the link to the electronic supplementary material.
ESM Figure 1
Dynamic change of plasma total ghrelin and insulin after glucose administration. Wild type (n = 7) and Ghsr1a knockout mice (n = 5) received rapamycin (1 mg/kg) for 6 days, mice were fasted for 12 h before the gastric administration of glucose (3 g/kg body weight) by gavage. Blood was drawn from canthus at 0, 15, 30, 60, and 90 min, and plasma total ghrelin (a) and insulin (b) concentrations were measured. Data expressed are mean ± SEM; *P < 0.05 vs. control mice (PDF 82 kb)
ESM Figure 2
Ghsr1a gene deletion blocks the orexigenic effect of rapamycin. Average food intake (a–c) in wild type or Ghsr1a knockout mice. Animals were divided into two groups and acclimated for six days before the following treatments: DMSO or rapamycin (1 mg/kg) intraperitoneal injection for six days. 3 h and 12 h food intake in dark cycle and 24 h (12:12 h light/dark) food intake were measured daily. Results were expressed as mean ± SEM. n = 6. *denotes P < 0.05 versus control (PDF 120 kb)
ESM Figure 3
Effects of rapamycin on plasma insulin. (a) Plasma insulin in normal male C57BL/6J mice receiving DMSO, rapamycin (Rapa; 1 mg/kg ip), D-Lys3-GHRP-6 (10 μmol/kg), or injection of ghrelin receptor antagonist D-Lys3-GHRP-6 (10 μmol/kg ip 2 min before rapamycin injection) and rapamycin. (b) Levels of plasma insulin in wild type littermate mice receiving DMSO, or rapamycin and Ghsr1a null mice receiving DMSO or rapamycin (Rapa; 1 mg/kg ip). Animals were fed with normal chow diet. Results were expressed as mean ± SEM. n = 6. *P < 0.05 vs. control mice (PDF 65 kb)
ESM Figure 4
Effect of ghrelin receptor antagonism or ghrelin receptor gene deletion on islets morphology. (a) Illustrates hematoxylin and eosin (H&E) staining in pancreas derived from mice treated with DMSO, rapamycin (1 mg/kg), D-Lys3-GHRP-6 (10 μmol/kg ip) or D-Lys3-GHRP-6 plus rapamycin for six days. (c) Depicts hematoxylin and eosin (H&E) staining in pancreas derived from Ghsr1a knockout mice or wild type littermates treated with DMSO or rapamycin (1 mg/kg). (b, d) Hematoxylin and eosin staining were measured to quantify changes in islets and expressed as mean ± SEM. Shown were representative results from six individual experiments (PDF 138 kb)
ESM Figure 5
Effect of ghrelin receptor antagonism or Ghsr1a knockout on insulin expression in pancreas. (a) Illustrates immunofluorescent staining for insulin (red) in pancreas derived from mice treated with DMSO, rapamycin (1 mg/kg), D-Lys3-GHRP-6 (10 μmol/kg ip) or D-Lys3-GHRP-6 plus rapamycin for 6 days. Nuclei were stained with Hochest dye. Controls include substituting primary antibodies with goat IgG. Shown are representative results from 6 individual experiments. (c) Depicts immunofluorescent staining for insulin (red) in pancreas derived from Ghsr1a knockout mice or wild type littermates treated with DMSO or rapamycin (1 mg/kg). Controls include substituting primary antibodies with goat IgG. (b, d) Fluorescent area and intensity of insulin staining were measured to quantify changes in insulin and expressed as mean ± SEM. Shown were representative results from six individual experiments (PDF 183 kb)
ESM Figure 6
Effect of ghrelin receptor antagonism on glucose transport in vitro. (a) Depicts immunofluorescent staining for HA-GLUT4 (red) in C2C12 myocytes treated with saline, ghrelin, D-Lys3-GHRP-6 or D-Lys3-GHRP-6 plus ghrelin. Nuclei were stained with Hochest dye. Controls include substituting primary antibodies with mouse IgG. Shown were representative results from three individual experiments. The middle panels are results from C2C12 cells treated with insulin (10 nmol) 10 min before harvest of cells. Controls include substituting primary antibodies with mouse IgG. (b) Fluorescent staining of HA-GLUT4 in C2C12 were measured to quantify HA-GLUT4 and expressed as mean ± SEM (n = 4). C2C12 cells were transfected with HA-GLUT4 or control plasmids two days before induction of differentiation (PDF 164 kb)
ESM Table 1
(PDF 43 kb)
Rights and permissions
About this article
Cite this article
Xu, G., Wang, Z., Li, Y. et al. Ghrelin contributes to derangements of glucose metabolism induced by rapamycin in mice. Diabetologia 55, 1813–1823 (2012). https://doi.org/10.1007/s00125-012-2509-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-012-2509-1