Abstract
Aims/hypothesis
We studied dietary factors and their association with blood glucose control in type 1 diabetic children and adolescents using intensive insulin treatment.
Materials and methods
A total of 550 children and adolescents with type 1 diabetes mellitus (age 2–19 years) recorded their diet for 4 days in pre-coded food diaries. Of the study group, 34% used insulin pumps, 43% used four or more injections and 16% three injections per day. HbA1c was related to targets of optimal blood glucose control defined by the International Society for Pediatric and Adolescent Diabetes (ISPAD).
Results
Adolescents with optimal glucose control (HbA1c ≤ 7.5%) had a lower intake of added sugar (7.7 vs 9.1% of energy intake, p = 0.004), a higher intake of fibre (19.3 vs 17.0 g/day, p = 0.01) and a higher intake of fruits and vegetables (257 vs 227 g/day, p = 0.04) than those with suboptimal metabolic control (HbA1c > 7.5%). Multiple regression analysis in adolescents showed that fibre and meal pattern were significantly associated with blood glucose control (effect fibre intake = −0.02, p = 0.04, effect having breakfast regularly = −0.89, p = 0.009). In children meal pattern was associated with blood glucose control (effect having dinner regularly = −0.66, p = 0.02, effect having supper regularly = −0.78, p = 0.03).
Conclusions/interpretation
In diabetic adolescents both intake of fibre and having a regular meal pattern are associated with blood glucose control. Lower intake of added sugar and sugar-sweetened soft drinks and higher intake of fruits and vegetables are observed among those with optimal compared with those with suboptimal blood glucose control. Dietary guidance should be intensified during adolescence to improve dietary intake and blood glucose control.
Similar content being viewed by others
Introduction
Poor blood glucose control is frequently reported in diabetic children and adolescents [1–5]. Several studies have explored predictors of blood glucose control [2, 6–9], and several factors have been identified, e.g. age [2], insulin dosage [7, 8], diabetes duration [7] and number of clinical visits [8, 9]. However, few studies have looked in detail at dietary intake and its effects on blood glucose control in children and adolescents [1, 4, 10, 11]; moreover, those that have done so had small sample sizes [1, 4, 11].
A more flexible meal pattern is possible in parallel with the introduction of more intensified insulin regimens. At the same time, dietary recommendations for children and adolescents have changed considerably since the 1980s. Recommendations now favour the intake of more carbohydrate and less protein and fat [12]. The intake of carbohydrate is recommended to consist of whole grain foods, fruits and vegetables, with no more than 10% of energy intake from added sugar [12]. Furthermore diabetic patients are recommended to eat a high fibre diet to facilitate control of blood glucose [12]. Several studies have demonstrated that intensive insulin treatment both delays the onset and slows the progression of microvascular [13–16] and macrovascular complications [16, 17]. Thus, addressing and outlining risk factors for poor blood glucose control might have a large impact on diabetes-related complications. Our hypothesis was that a high intake of fibre, low intake of added sugar and a regular meal pattern would all help improve HbA1c in children and adolescents with type 1 diabetes.
Materials and methods
Participants
The participants were recruited from participants in the Norwegian Childhood Diabetes and Quality project (NCDQ) [18]. This is a prospective population-based study for research and quality improvement by means of benchmarking, and includes all children and adolescents with type 1 diabetes mellitus in Norway, taken from 24 of 25 Norwegian Paediatric Departments. The classification of type 1 diabetes mellitus is made by measurements of autoantibodies (insulin, GAD, protein tyrosine phosphatase) and C-peptide at diagnosis. Children with type 2 diabetes mellitus were not included.
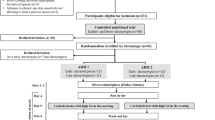
Participants were recruited in 2004 and 2005. The number of NCDQ project participants in 2004 and 2005 was 1,417 and 1,655 respectively. The total number of participants over these 2 years was 1935. Of these, 658 children and adolescents recorded their diet for 4 days, 457 in 2004 and 201 in 2005. This gives a participation rate of 34%. Three participants were excluded because they participated both years (2005 data excluded). For 550 of the 655 participants, data were available on centralised measurement of HbA1c from the NCDQ project for the year they recorded their diet. This was therefore the number included in the present analyses.
The dietary data collection was carried out from January to April 2004 and 2005 and is described in detail elsewhere [19]. Written information and food diaries were sent to the participants and they were told to record their diet for three specific weekdays and one specific weekend day. All participants were either asked to start recording on the next Sunday or Wednesday. On the second day of recording they were phoned by a nutritionist to encourage them to finish the study. The time for the dietary study was chosen to coincide as closely as possible with the time of yearly visit for NCDQ project. The median time difference from the clinical visit to the time when recording started was 2 weeks. Ninety per cent of the participants recorded their diet within 2 weeks before or 2 weeks after the clinical visit and HbA1c measurement.
The study protocols were approved by the National Committee for Research Ethics in Norway and the Norwegian Social Science Data Services. Informed consent was obtained from the parents and from the participants who were older than 12 years of age.
Questionnaires
Participants filled in a questionnaire, which included questions on meal frequency (missing values = 5%) and parents’ education (missing values = 14%) (for further details see [20]). The meal frequency variable was recoded, and having breakfast, dinner and supper regularly was defined as having the meal more than five times a week. Information on BMI (missing = 1%), insulin dose per kg body weight (missing values = 30%), diabetes duration (missing values = 12%), insulin regimen (missing values = 6%) was obtained from the case record forms used in the NCDQ project. To estimate the prevalence of overweight, the international cut-off points for BMI (kg/m2) for overweight were used [21]. Intensive insulin treatment was defined as using an insulin pump or needing three or more injections per day, but some patients may have used one to two injections per day during the early phase of the disease (remission period).
HbA1c
We determined HbA1c by an HPLC method (Variant; BioRad, Richmond, CA, USA) standardised in line with The Diabetes Control and Complication Trial recommendations [22]. All samples were sent to the same central laboratory at Aker University Hospital, Oslo. Normal reference was 4.1% to 6.4% (2 SD) and intra-assay CV was <3%. Optimal blood glucose control was defined as having HbA1c ≤ 7.5% and suboptimal control as having HbA1c > 7.5%. These targets of optimal blood glucose control have been defined by the International Society for Pediatric and Adolescent Diabetes (ISPAD) [23] to reduce the risk of cardiovascular disease and microvascular complications.
Food diary
The participants recorded their food intake for four consecutive days, in food diaries. The diary has lists of 277 drinks, food items and dishes grouped together according to a typical Norwegian diet. Food amounts are presented in predefined household units or as portions estimated from pictures in a photographic booklet [24] (for further details see [19]). The food diary and the photographic booklet have been validated [24–26]. Validation of the food diary among 9-year-olds showed that there were no significant differences in energy intakes on different recording days. However, when comparing under-reporters and actual reporters, under-reporters had a significantly lower energy intake for the last 2 days of the recording period than did actual reporters [26].
Calculations of dietary intake
The data entry was made by scanning, using Teleform program 6.0 and 8.1 (Datascan, Oslo, Norway). Daily intake of foods, energy and nutrients were computed using a food database and software system developed at the Department of Nutrition, University of Oslo (for further details see [19]). When the term added sugar is used it refers to refined or industrially produced sugar (not including naturally occurring mono- and disaccharides) used as an ingredient in processed or prepared food. Furthermore, day-to-day variation in nutrient intake is presented and expressed as the CV (CV = SD × 100/mean) [27].
Statistical analysis
Demographic and clinical data and nutrient intakes are presented as means with SDs for those with optimal and suboptimal blood glucose control (Table 1). The data for all analyses are separated into two age groups: children (2–10 years old) and adolescents (11–19 years old). This grouping was chosen to separate the pubertal from the pre-pubertal participants. Ninety-three per cent of the children were at stage 1 in Tanner’s puberty score, while eight children were at stage 2 and one at stage 3. Intake of foods and drinks is presented as medians with first and third quartile (Q1, Q3). When comparing continuous variables Student’s t test was used for normally distributed data and Mann–Whitney U test for not normally distributed data. The χ 2 test was used to compare different HbA1c groups regarding overweight, insulin regimen, parents’ education and meal frequencies. Simple and multiple linear regression analyses were used to study possible factors associated with HbA1c. All macronutrients, relevant clinical variables and puberty, and diabetes duration were tested in the unadjusted analysis, while only variables with p < 0.1 were presented and included in the multivariate analysis. Sex and mothers’ education were included even when p > 0.1, only for adjustment in the multivariate analysis. Data on insulin dose and body weight insulin per kg were missing for 30% of the participants and insulin per kg body weight was not included in the regression analysis.
All p values are two-sided; a 5% level of significance was used. All statistical analyses were performed with SPSS 14.0 (SPSS, Chicago, IL, USA).
Results
Characteristics of the participants are described in Table 1. Results are presented for those with optimal blood glucose control (HbA1c ≤ 7.5%) and those with suboptimal blood glucose control (HbA1c > 7.5%) in the two selected age groups (Table 1). The groups with low and high HbA1c were in general comparable regarding age, pubertal development, weight, BMI, overweight, insulin regimens and parent’s education. However, adolescents with poor glycaemic control had slightly longer diabetes duration, higher insulin dose, less hypoglycaemia and more pump-users.
Optimal blood glucose control was associated with eating a recommended diet and not skipping meals. In adolescents, unadjusted regression analysis showed that low intake of added sugar, high intake of fibre, having breakfast and supper regularly, together with shorter diabetes duration and less intensive insulin regimen, significantly improved HbA1c (crude values; Table 2). In the multiple regression model, high fibre intake, low BMI, having breakfast regularly, few clinical visits and short diabetes duration significantly improved HbA1c (Table 2). In the multiple analyses in children, lower HbA1c was significantly associated with low BMI and having dinner and supper regularly.
Table 3 shows details on intake of energy and macronutrients in the two age groups. Apart from intake of fat and fibre, which were higher and lower, respectively, than recommended, all intakes of macronutrients were adequate according to current recommendations [12]. Adolescents with optimal blood glucose control had a significantly lower intake of added sugar and significantly higher intake of fibre than adolescents with suboptimal blood glucose control. They also had a significantly lower intake of sugar-sweetened soft drinks and a higher total intake of fruits and vegetables. Among the children, no such significant differences were observed. Among the adolescents there were significantly more sugar-sweetened soft drink users among those with suboptimal blood glucose control than among those with optimal control (38% vs 26%, p = 0.03). This difference was not observed among the children (31% vs 37%, p = 0.33). No significant differences were found in the day-to-day variation (CV) of energy, carbohydrate, fibre and added sugar in relation to the HbA1c groups (Table 3).
Discussion
This study shows that an irregular meal pattern is significantly associated with poor blood glucose control in Norwegian children and adolescents with type 1 diabetes mellitus, even though more than 90% were on intensive insulin treatment. In adolescents a low intake of fibre was also associated with high HbA1c. When looking at adolescents with optimal blood glucose control, they have a lower intake of added sugar and sugar-sweetened soft drinks, plus a higher intake of fruits and vegetables than those with suboptimal blood glucose control.
Blood glucose control was associated with having breakfast, dinner and supper regularly. The introduction of insulin via pump and multiple insulin injections has made the timing of meals more flexible for diabetic patients [28], possibly making some more prone to skipping meals. Frey et al. [29] found that better blood glucose control was associated with eating three meals a day among adolescents. Moreover, among Finnish diabetic adolescents a large number of meals per day was related to good blood glucose control and reflected a good coordination between insulin regimen and diet [1]. Our results suggest that avoiding the skipping of meals would help improve blood glucose control in children and adolescents.
An association between dietary fibre and HbA1c was observed among the adolescents. This has previously been reported in one study among British adolescents from 1986 [11] and more recently among adults in EURODIAB [30], although not among north-western Europeans. The mechanism whereby increased fibre intake beneficially affects HbA1c presumably relates to reduced postprandial blood glucose peaks. Thus, increased fibre intake may contribute to an overall improvement of glycaemic control [30]. The reason why this observation is only seen among adolescents could be because there are more adolescents than children in the present study and that the adolescents had a greater range of HbA1c, making dietary influence easier to detect. Mean intake of fibre and fruits and vegetables was lower than recommended (fibre = 40 g/day; fruits and vegetables = 500 g/day [12, 31]) for all groups regardless of age and HbA1c in this study. However, among adolescents with optimal blood glucose control the intake was higher than in those with suboptimal blood glucose control.
As a group, adolescents with optimal blood glucose control had a lower intake of added sugar and sugar-sweetened soft drinks and also fewer sugar-sweetened soft drink users than the group with suboptimal blood glucose control. Nutritional management of children with type 1 diabetes mellitus has traditionally emphasised the exclusion of refined carbohydrate [32]. In the 1980s and 1990s several randomised controlled trials demonstrated that small amounts of sucrose in the diet had no adverse effects on blood glucose control in adults [33, 34] and children [32, 35], leading to a more liberal approach [12]. According to current recommendations, it is acceptable for patients with type 1 diabetes mellitus to have a moderate intake of free sugars if desired and if blood glucose levels are satisfactory [12]. From our results it seems that a lower intake of sugar and a lower consumption of sugar-sweetened soft drinks can make it easier to achieve optimal blood glucose control.
In our study, HbA1c increased with increasing BMI in children, while the opposite was seen in adolescents, in whom HbA1c decreased with increasing BMI. The latter has been reported earlier [7]. High BMI may indicate a too high dose of insulin; it has also been shown that increase in body weight may reduce insulin action [1, 36], and this could explain our result among the children. Increased BMI is reported to be a side effect of intensive insulin treatment, explained by fear of hypoglycaemia that leads to overeating [37]. A high number of clinical visits in adolescents was associated with higher HbA1c, as has been described by others [8, 9]. The result probably reflects the practice of following patients with poor control more closely. Furthermore, in adolescents HbA1c increased with increasing diabetes duration, a finding that has been reported earlier [2, 6]. This could reflect the decline or end of endogenous insulin production [1, 6] or the fact that HbA1c often deteriorates with age in adolescents [1, 3].
In this study we used a food diary designed to be ideal for children and adolescents. This method captures much of the variability in food intake through extensive food lists and an open-ended approach [25]. The advantage of this method compared with those such as 24 h recall and dietary history is that intake is recorded as it is eaten, thus providing more accurate and more detailed information. Compared with weighed records it is also less time-consuming for the participants and the researcher to conduct [38]. The present study is a population-based study of dietary intake and measurements of HbA1c among children and adolescents with type 1 diabetes mellitus. Few studies have looked in detail at the relationship between dietary intake and blood glucose control in children and adolescents [1, 4, 10, 11, 39]. Most of these studies have smaller sample sizes than the present study. These previous studies [1, 4, 10, 11] have identified intake of fat [10, 39], saturated fat [4], fibre [1]) and day-to-day variations in energy intake [1, 10] to be related to HbA1c. However, fibre is the only factor replicated in this study. Among dietary factors, glycaemic index has also been studied, especially among adults [40], but also among children [41, 42], and was seen to have a rather small effect on blood glucose control in randomised control trials [40, 43, 44].
Insulin regimen was included in the regression analysis, but was not a significant factor. Among those who had poorer glucose control there were more insulin pump users, possibly reflecting the fact that patients with blood glucose control are asked to use insulin pumps to help improve their blood glucose control. There were only minor differences in dietary intake between the two groups (data not shown) and the results were therefore not separated according to pump use. Insulin dose per kg body weight was only a significant factor in adolescents (B = 1.2 [0.75, 1.74], p < 0.001), as reported by others [7, 8]. Insulin dose per kg was higher among participants with suboptimal blood glucose control than among those with optimal blood glucose control, a finding that might reflect both the use of higher insulin dosage to achieve better control and the lower insulin sensitivity resulting from high blood glucose.
It could be argued that the clinical relevance of our results are scarce because of the small, albeit significant regression coefficients for some variables, However, it has been recognised that it is impossible to estimate the dietary intake of individuals without error and that the high random error associated with estimates of nutrient intake biases the correlation coefficients and slopes of regression lines toward zero [45]. Thus, the effect on HbA1c of dietary intake is likely to be larger than estimated here.
It is important to notice some limitations of our study, which include the fact that dietary data were self-reported, which often results in under-reporting of energy intake [46]. According to Goldberg et al. [47], a ratio between energy intake and basal metabolic rate of less than 1.06 may indicate under-reporting. According to this, the total prevalence of under-reporting in our study was 20%, 28% among girls and 12% among boys. Many investigators have found that the most frequent under-estimated food items are ‘unhealthy’ ones such as sweets, desserts and snacks [48]. However, in a validation study of the food diary, the under-reporters did not under-report unhealthy food to a greater extent than they did healthy food groups [25]. Another limitation of our study was the low response rate (34%). A reason for the low response rate may be the considerable effort of detailed registration of food intake for 4 days. Of those who did not participate in the dietary study, HbA1c and BMI were available from the NCDQ for 1009 participants. Among those who participated in the dietary study, HbA1c was significantly lower (HbA1c mean difference = 0.24%; p < 0.001) than among non-participants in analysis adjusted for age and sex, while there was no significant difference in BMI (BMI mean difference = 0.05 kg/m2; p = 0.77). This could mean that our results are skewed in relation to HbA1c and that they represent the part of the young diabetic population with good blood glucose control and diet. The reduced range in HbA1c and dietary intake makes the regression analysis less sensitive. Furthermore, for more than 50% of the participants HbA1c was measured before the diet was recorded. HbA1c is a retrospective measurement for blood glucose control and so diet might not reflect the HbA1c at time of recording. However, NCDQ data show that mean HbA1c was stable over 3 years in this age group (data not shown) as is supported in the literature [49]. The median difference was 14 days, and we do not believe that much change in HbA1c could have occurred during this time.
Conclusion
Optimal blood glucose control was associated with eating a recommended diet and not skipping meals. This is still important even when intensive insulin treatment with insulin pumps and multiple injections are used. Our results show that a regular meal pattern and high fibre intake are factors that improve HbA1c in young diabetic patients. Among adolescents, moreover, lower intake of added sugar and sugar-sweetened soft drinks, as well as higher fruits and vegetables intake were observed among patients with optimal compared with suboptimal blood glucose control. Our results support the policy that dietary guidance should be intensified during adolescence to improve dietary intake, meal pattern and blood glucose control.
Abbreviations
- NCDQ:
-
The Norwegian Childhood Diabetes and Quality project
References
Virtanen SM (1992) Metabolic control and diet in Finnish diabetic adolescents. Acta Paediatr 81:239–243
Rosilio M, Cotton JB, Wieliczko MC et al (1998) Factors associated with glycemic control. A cross-sectional nationwide study in 2,579 French children with type 1 diabetes. The French Pediatric Diabetes Group. Diabetes Care 21:1146–1153
Weissberg-Benchell J, Glasgow AM, Tynan WD, Wirtz P, Turek J, Ward J (1995) Adolescent diabetes management and mismanagement. Diabetes Care 18:77–82
Pietilainen KH, Virtanen SM, Rissanen A, Rita H, Maenpaa J (1995) Diet, obesity, and metabolic control in girls with insulin dependent diabetes mellitus. Arch Dis Child 73:398–402
Mortensen HB, Hougaard P (1997) Comparison of metabolic control in a cross-sectional study of 2,873 children and adolescents with IDDM from 18 countries. The Hvidore Study Group on Childhood Diabetes. Diabetes Care 20:714–720
Dorchy H, Roggemans MP, Willems D (1997) Glycated hemoglobin and related factors in diabetic children and adolescents under 18 years of age: a Belgian experience. Diabetes Care 20:2–6
Scottish Study Group for the Care of the Young Diabetic (2001) Factors influencing glycemic control in young people with type 1 diabetes in Scotland: a population-based study (DIABAUD2). Diabetes Care 24:239–244
Nordly S, Mortensen HB, Andreasen AH, Hermann N, Jorgensen T (2005) Factors associated with glycaemic outcome of childhood diabetes care in Denmark. Diabet Med 22:1566–1573
Urbach SL, LaFranchi S, Lambert L, Lapidus JA, Daneman D, Becker TM (2005) Predictors of glucose control in children and adolescents with type 1 diabetes mellitus. Pediatr Diabetes 6:69–74
Forsander G, Malmodin B, Eklund C, Persson B (2003) Relationship between dietary intake in children with diabetes mellitus type I, their management at diagnosis, social factors, anthropometry and glycaemic control. Scand J Nutr 47:75–84
Hackett AF, Court S, Mccowen C, Parkin JM (1986) Dietary survey of diabetics. Arch Dis Child 61:67–71
Mann JI, De Leeuw I, Hermansen K et al (2004) Evidence-based nutritional approaches to the treatment and prevention of diabetes mellitus. Nutr Metab Cardiovasc Dis 14:373–394
Dahl-Jorgensen K (1987) Near-normoglycemia and late diabetic complications. The Oslo Study. Acta Endocrinol Suppl (Copenh) 284:1–38
The Diabetes Control and Complications Trial Research Group (1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. The Diabetes Control and Complications Trial Research Group. N Engl J Med 329:977–986
Diabetes Control and Complications Trial Research Group (1994) Effect of intensive diabetes treatment on the development and progression of long-term complications in adolescents with insulin-dependent diabetes mellitus: Diabetes Control and Complications Trial. Diabetes Control and Complications Trial Research Group. J Pediatr 125:177–188
Larsen J, Brekke M, Sandvik L, Arnesen H, Hanssen KF, Dahl-Jorgensen K (2002) Silent coronary atheromatosis in type 1 diabetic patients and its relation to long-term glycemic control. Diabetes 51:2637–2641
Nathan DM, Cleary PA, Backlund JY et al (2005) Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes. N Engl J Med 353:2643–2653
Margeirsdottir HD, Larsen JR, Brunborg C, Dahl-Jørgensen K (2006) Nation-wide improvement in HbA1c and complication screening in a Benchmarking project in childhood diabetes. A prospective national quality study. Pediatr Diabetes 7(Suppl 5):OP-4 (Abstract)
Overby NC, Flaaten V, Veierod MB et al (2007) Children and adolescents with type 1 diabetes eat a more atherosclerosis-prone diet than healthy control subjects. Diabetologia 50:307–316
Overby NC, Lillegaard IT, Johansson L, Andersen LF (2004) High intake of added sugar among Norwegian children and adolescents. Public Health Nutr 7:285–293
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH (2000) Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 320:1240–1243
Little RR, Rohlfing CL, Wiedmeyer HM, Myers GL, Sacks DB, Goldstein DE (2001) The national glycohemoglobin standardization program: a five-year progress report. Clin Chem 47:1985–1992
Swift PGF (2007) ISPAD guidelines 2000. Medforum, Zeist, The Netherlands
Lillegaard IT, Overby NC, Andersen LF (2005) Can children and adolescents use photographs of food to estimate portion sizes? Eur J Clin Nutr 59:611–617
Lillegaard IT, Andersen LF (2005) Validation of a pre-coded food diary with energy expenditure, comparison of under-reporters v. acceptable reporters. Br J Nutr 94:998–1003
Lillegaard IT, Loken EB, Andersen LF (2007) Relative validation of a pre-coded food diary among children, under-reporting varies with reporting day and time of the day. Eur J Clin Nutr 61:61–68
Wolever TM, Hamad S, Chiasson JL et al (1999) Day-to-day consistency in amount and source of carbohydrate associated with improved blood glucose control in type 1 diabetes. J Am Coll Nutr 18:242–247
Sullivan-Bolyai S, Knafl K, Tamborlane W, Grey M (2004) Parents’ reflections on managing their children’s diabetes with insulin pumps. J Nurs Scholarsh 36:316–323
Frey MA, Ellis D, Naar-King S, Greger N (2004) Diabetes management in adolescents in poor metabolic control. Diabetes Educ 30:647–657
Buyken AE, Toeller M, Heitkamp G et al (1998) Relation of fibre intake to HbA1c and the prevalence of severe ketoacidosis and severe hypoglycaemia. EURODIAB IDDM Complications Study Group. Diabetologia 41:882–890
Andersen LF, Overby N, Lillegaard IT (2004) Intake of fruit and vegetables among Norwegian children and adolescents. Tidsskr Nor Laegeforen 124:1396–1398
Loghmani E, Rickard K, Washburne L, Vandagriff J, Fineberg N, Golden M (1991) Glycemic response to sucrose-containing mixed meals in diets of children with insulin-dependent diabetes mellitus. J Pediatr 119:531–537
Slama G, Haardt MJ, Jean-Joseph P et al (1984) Sucrose taken during mixed meal has no additional hyperglycaemic action over isocaloric amounts of starch in well-controlled diabetics. Lancet 2:122–125
Bornet F, Haardt MJ, Costagliola D, Blayo A, Slama G (1985) Sucrose or honey at breakfast have no additional acute hyperglycaemic effect over an isoglucidic amount of bread in type 2 diabetic patients. Diabetologia 28:213–217
Schwingshandl J, Rippel S, Unterluggauer M, Borkenstein M (1994) Effect of the introduction of dietary sucrose on metabolic control in children and adolescents with type I diabetes. Acta Diabetol 31:205–209
Yki-Jarvinen H, Koivisto VA (1986) Natural course of insulin resistance in type I diabetes. N Engl J Med 315:224–230
Craig ME, Handelsman P, Donaghue KC et al (2002) Predictors of glycaemic control and hypoglycaemia in children and adolescents with type 1 diabetes from NSW and the ACT. Med J Aust 177:235–238
Andersen LF, Pollestad ML, Jacobs DR Jr, Lovo A, Hustvedt BE (2005) Validation of a pre-coded food diary used among 13-year-olds: comparison of energy intake with energy expenditure. Public Health Nutr 8:1315–1321
Lodefalk M, Aman J (2006) Food habits, energy and nutrient intake in adolescents with Type 1 diabetes mellitus. Diabet Med 23:1225–1232
Brand-Miller J, Hayne S, Petocz P, Colagiuri S (2003) Low-glycemic index diets in the management of diabetes: a meta-analysis of randomized controlled trials. Diabetes Care 26:2261–2267
Gilbertson HR, Brand-Miller JC, Thorburn AW, Evans S, Chondros P, Werther GA (2001) The effect of flexible low glycemic index dietary advice versus measured carbohydrate exchange diets on glycemic control in children with type 1 diabetes. Diabetes Care 24:1137–1143
Mohammed NH, Wolever TM (2004) Effect of carbohydrate source on post-prandial blood glucose in subjects with type 1 diabetes treated with insulin lispro. Diabetes Res Clin Pract 65:29–35
Brand-Miller JC, Petocz P, Colagiuri S (2003) Meta-analysis of low-glycemic index diets in the management of diabetes: response to Franz. Diabetes Care 26:3363–3364
Gilbertson HR, Thorburn AW, Brand-Miller JC, Chondros P, Werther GA (2003) Effect of low-glycemic-index dietary advice on dietary quality and food choice in children with type 1 diabetes. Am J Clin Nutr 77:83–90
Beaton GH (1994) Approaches to analysis of dietary data: relationship between planned analyses and choice of methodology. Am J Clin Nutr 59:253S–261S
Black AE, Goldberg GR, Jebb SA, Livingstone MBE, Cole TJ, Prentice AM (1991) Critical evaluation of energy-intake data using fundamental principles of energy physiology. 2. Evaluating the results of published surveys. Eur J Clin Nutr 45:583–599
Goldberg GR, Black AE, Jebb SA et al (1991) Critical evaluation of energy-intake data using fundamental principles of energy physiology. 1. Derivation of cutoff limits to identify under-recording. Eur J Clin Nutr 45:569–581
Svendsen M, Tonstad S (2006) Accuracy of food intake reporting in obese subjects with metabolic risk factors. Br J Nutr 95:640–649
Jorde R, Sundsfjord J (2000) Intra-individual variability and longitudinal changes in glycaemic control in patients with type 1 diabetes mellitus. Diabet Med 17:451–456
Acknowledgements
The authors would like to thank all the participants in the Norwegian Childhood Diabetes and Quality project. This project was financed with the aid of EXTRA funds from the Norwegian Foundation for Health and Rehabilitation.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Øverby, N.C., Margeirsdottir, H.D., Brunborg, C. et al. The influence of dietary intake and meal pattern on blood glucose control in children and adolescents using intensive insulin treatment. Diabetologia 50, 2044–2051 (2007). https://doi.org/10.1007/s00125-007-0775-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-007-0775-0