Abstract
Aims/hypothesis
We evaluated the insulinotropic and antihyperglycaemic actions of glucokinase activators (GKAs), especially through acute and subchronic studies in rodent diabetes models with (2R)-2-(4-cyclopropanesulphonylphenyl)-N-(5-fluorothiazol-2-yl)-3-(tetrahydropyran-4-yl)propionamide (PSN-GK1), a novel and potent GKA.
Materials and methods
The action of PSN-GK1 on or in the following were investigated: (1) on human liver glucokinase, insulin secretion from MIN6 cells and 2-deoxy-d-[3H]glucose (2-DG) uptake into rat hepatocytes; and (2) in Zucker diabetic fatty rats and in non-diabetic C57Bl/6, diabetic db/db and ob/ob mice.
Results
At 5 mmol/l glucose, PSN-GK1 activated glucokinase (4.3-fold, median effective concentration [EC50] 130 nmol/l), increased MIN6 insulin secretion (26-fold, EC50 267 nmol/l) and 2-DG hepatocytic uptake (threefold, EC50 1 μmol/l); at higher glucose concentrations, EC50s and fold-effectiveness were both lower. In C57Bl/6 mice, PSN-GK1 reduced blood glucose at 1 and 10 mg/kg (by mouth), but insulin was increased significantly at only the higher dose. In hyperinsulinaemic 10-mmol/l glucose clamps, PSN-GK1 increased 2-DG incorporation into liver glycogen sixfold, directly demonstrating liver effects. PSN-GK1 improved glycaemic profiles in db/db mice and Zucker diabetic fatty rats, diabetic animal models in which GKA efficacy has not previously been described, without causing hypoglycaemia. In ob/ob mice, it dose-dependently reduced excursions in OGTTs. Moreover, after subchronic administration, no tachyphylaxis was evident and glycaemia was improved without alterations to lipid levels, liver weight, glycogen content or body weight.
Conclusions/interpretation
PSN-GK1 was potently antihyperglycaemic through its effects on insulin release and hepatic glucose metabolism. It is one of the most potent GKAs described in the literature and is active in diabetic animal models where GKAs have not been reported to show efficacy to date. Ongoing human trials are investigating the potential of this novel therapeutic approach.
Similar content being viewed by others
Introduction
The incidence of type 2 diabetes is increasing dramatically worldwide, largely due to the ongoing obesity epidemic. At present, no single agent is capable of achieving acceptable, long-lasting blood glucose control in the majority of patients [1]. Although combinations of available drugs can give superior glycaemic control [2], they tend to lose efficacy over time and produce unwanted side effects, such as weight gain. Thus, there is a pressing need for safe, novel drugs with improved efficacy [3].
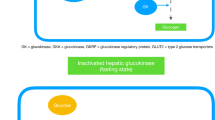
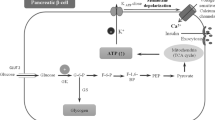
Because of its key role in glucose homeostasis, glucokinase is a potential target for small-molecule type 2 diabetes therapeutics [4, 5]. Its pivotal position in blood glucose control is determined by its actions in pancreas and liver [6], although it is expressed in numerous other cell types that complete the glucose-sensing network [7, 8]. In beta cells, glucokinase is the glucose sensor that dictates the threshold for insulin secretion, while in hepatocytes it is rate-determining for glucose metabolism. Additionally, this enzyme plays a crucial role in neuronal glucosensing in the brain [9] and is also produced in incretin-releasing K and L cells in the gut [10], as well as in the pituitary [11]. Deactivating glucokinase mutations lead to maturity-onset diabetes of the young type 2, a condition characterised by elevated plasma glucose resulting from glucokinase haploinsufficiency [12, 13]. On the other hand, individuals with activating glucokinase mutations [14] have hyperinsulinaemic hypoglycaemia [15], a disorder attributed to a decreased threshold for glucose-stimulated insulin release (GSIR) and possibly also to elevated hepatic glucose use, although effects on liver glucokinase flux remain uninvestigated. The existence of patients with hyperinsulinaemic hypoglycaemia suggests that small-molecule glucokinase activators (GKAs) could exhibit powerful antihyperglycaemic properties both by augmenting GSIR and by altering hepatic glucose balance [16, 17]. Thus, GKAs could combine [18] the glucose-lowering effects of insulin secretagogues with biguanide-like, hepatic glucose-lowering actions to provide enhanced glycaemic control.
Interest in glucokinase is intensifying [19] following the discovery of Ro-28-1675 [20]. This compound activates glucokinase by increasing affinity for glucose (substrate concentration at half maximal velocity, S 0.5) and maximal velocity (V max). It enhances GSIR from isolated rat pancreatic islets, increases hepatocyte glucose uptake and demonstrates antihyperglycaemic effects in various rodent models. Moreover, chronic administration of Ro-28-1675 prevents the development of hyperglycaemia in diet-induced obese mice [21]. Like Ro-28-1675, other GKAs reported to date [22–25] bind an allosteric site found where the activating mutations cluster [26, 27].
Here, we evaluate the GKA (2R)-2-(4-cyclopropanesulphonylphenyl)-N-(5-fluorothiazol-2-yl)-3-(tetrahydropyran-4-yl)propionamide (PSN-GK1) [28] (Fig. 1) and the translation of this compound’s improved activity and excellent pharmacokinetic profile into potent acute and subchronic antihyperglycaemic effects in rodents. Importantly, these antihyperglycaemic effects do not appear to be accompanied by adverse events, such as hypoglycaemia or hyperlipidaemia.
In vitro activation of glucokinase by PSN-GK1. a Concentration-dependent activation of glucokinase by PSN-GK1 and structure of PSN-GK1. b Glucokinase kinetics with respect to glucose in the presence of different concentrations of PSN-GK1 (0.0 μmol/l, crosses; 0.1 μmol/l, circles; 0.4 μmol/l, squares; 1.0 μmol/l, triangles)
Materials and methods
Animals
Male C57Bl/6 (5–6 weeks), C57Bl/6 ob/ob (6–7 weeks) and female C57Bl/KsJ db/db (9 weeks) mice from Harlan Olac, Bicester, UK were housed under controlled conditions (21 ± 2°C; 45–65% humidity; 12-h light–dark cycle, lights on 08.00 h) with free access to rat and mouse no. 1 diet (Bantin and Kingman, Hull, UK). Female Zucker diabetic fatty (ZDF) rats (6 weeks old; Charles River, Manston, UK) were housed similarly, except that they were put on a 10/14-h light–dark cycle (lights off at 22.00 h) and had free access to high-fat diet D1245 (Research Diets, New Brunswick, NJ, USA) (45% of energy from fat) for 4 weeks prior to a meal-feeding regimen. For clamp studies, male C57Bl/6J mice (12 weeks) from Charles River were housed as above but fed pelleted chow (UAR, Nillemoison, France). Studies were approved by local ethical boards and animal husbandry and procedures carried out according to institutional guidelines.
Materials
PSN-GK1 was prepared [29], dissolved in DMSO and used in vitro at concentrations indicated with a final DMSO concentration of ≤5%. For mice studies, PSN-GK1 was dissolved in warm 90% water–10% Gelucire 44/14 (Gattefossé, Gennevilliers, France), with stirring and/or sonication at 0.1–2.0 mg/ml, for dosing at 1–20 mg/kg via oral gavage at 10 ml/kg. For ZDF rats, PSN-GK1 was administered at 10 mg 2 ml–1 kg–1 in warm 90% water–10% Gelucire 44/14. Recombinant human hexokinases I, II and III and glucokinase (liver form) were expressed as glutathione S-transferase (GST) fusion proteins in E. coli, purified by glutathione affinity chromatography to >98% purity and stored at –80 °C in 50 mmol/l Tris/HCl pH 7.4, 1 mmol/l dl-dithiothreitol, 50 mmol/l NaCl and 10% glycerol.
Enzyme assays
Glucokinase activity was measured in a coupled reaction with glucose-6-phosphate dehydrogenase (G6PDH) by monitoring NADPH production at A340 in a plate reader (SpectraMax 190; Molecular Devices, Wokingham, UK) after 15 min incubation at 24°C, in a final volume of 100 μl containing 25 mmol/l HEPES pH 7.1, 25 mmol/l KCl, 5 mmol/l glucose, 1 mmol/l ATP, 2 mmol/l MgCl2, 1 mmol/l dl-dithiothreitol, 1 mmol/l NADP, 2.5 U/ml G6PDH, 0.4 μg GST-glucokinase. These conditions were also used for hexokinases I to III, except that the glucose concentration was 0.25 mmol/l. We tested ten dilutions of PSN-GK1 from 0.004 to 100 μmol/l, calculating and fitting fold changes in activity vs controls to sigmoidal curves using a four-parameter logistic model. For effects on kinetic parameters (S 0.5, V max, Hill coefficient), a series of velocity plots at different PSN-GK1 and glucose concentrations (0.67–20 mmol/l) were fitted to the Hill equation using XLfit version 4.1 (IDBS, Guildford, UK).
Cell incubations and assays
MIN6 cells, a mouse pancreatic beta cell line, were cultured in DMEM containing 25 mmol/l glucose, 1 mmol/l sodium pyruvate, 50 μmol/l 2-mercaptoethanol, 15% heat-inactivated FCS, 50 U/ml penicillin, 50 μg/ml streptomycin. Culture and incubations were at 37°C. Cells were seeded at 4 × 105 cells per well in 12-well plates, cultured for 3 days, then washed twice with KRB containing 119 mmol/l NaCl, 4.74 mmol/l KCl, 2.54 mmol/l CaCl2, 1.19 mmol/l MgSO4, 1.19 mmol/l KH2PO4, 25 mmol/l NaHCO3, 10 mmol/l HEPES pH 7.4, 0.1% BSA and 5 mmol/l glucose. Cells were pre-incubated for 1 h in KRB, followed by 1 h static incubations with PSN-GK1 and glucose at indicated concentrations. Media samples were removed, cleared of debris by centrifugation at 1,000 g and insulin was measured in triplicate against standards using a rat insulin ELISA kit (Mercodia, Uppsala, Sweden). Cells were lysed in 150 mmol/l NaCl, 1% glycerol, 1% Triton X-100, 1 mmol/l EGTA, 50 mmol/l HEPES pH 7.5 supplemented with Complete Protease Inhibitor Cocktail (Roche Diagnostics, Penzberg, Germany) for protein measurement by bicinchoninic acid assay (Pierce, Rockford, IL, USA) with BSA standard.
Cryopreserved rat hepatocytes (XenoTech LLC, Lenexa, KS, USA) were centrifuged at 75 g over 25% Percoll and seeded at 2 × 105 to 4 × 105 cells per well in 12-well plates coated with collagen-I. Cells were attached, cultured and assayed for 2-deoxy-d-[3H]glucose (2-DG) uptake as described [30]. Media contained 5.55 mmol/l glucose and after 2 days of culture cells were incubated for 4 h in fresh media containing 74 kBq/ml 2-DG (Perkin Elmer, Beaconsfield, UK). Cells were washed three times, lysed and portions of lysates used for scintillation counting and protein measurement as above. Net uptake was calculated as pmol 2-DG per mg protein and expressed as a percentage of the basal value.
Animal studies
C57Bl/6J mice
Food was withdrawn 5 h before dosing, while water was available throughout. A blood sample was taken from the tail tip under local anaesthetic for glucose and insulin measurement. Thereafter, mice were weighed and dosed orally with PSN-GK1 (1 or 10 mg/kg) or vehicle. Blood samples were taken 15, 30, 60, 120 and 240 min after dosing, samples (20 μl) for glucose being taken into disposable micro-pipettes and added to 480 μl haemolysis reagent. Duplicate 20-μl aliquots haemolysed blood were added to 180 μl Trinder’s glucose reagent (Sigma enzymatic colorimetric method) in a 96-well plate. After mixing, samples were left (room temperature) for 30 min before reading against standards; correction was made for haemoglobin. Samples for insulin (30 μl) were collected into heparin/Li-containing tubes, kept on ice for <30 min, centrifuged (2,800 g, 10 min, 4°C) and stored at −20°C for subsequent measurements using an insulin ELISA kit (Crystal Chem, Downers Grove, IL, USA) and SpectroMax 250 plate reader (Molecular Devices).
Hyperinsulinaemic–hyperglycaemic clamps
After 8 days acclimatisation, during which mice were periodically handled, an indwelling catheter was placed into the femoral vein under anaesthesia, sealed under the back skin and glued on top of the skull. After 4 to 5 days, mice were fasted for 6 h before dosing and throughout the remainder of the study. PSN-GK1 (10 mg/kg) or vehicle was administered orally 30 min before 180 min i.v. infusion of a steady rate of [3H]glucose (to ensure detectable glucose isotopic dilution into blood and measurable incorporation into liver glycogen) and of pharmacological insulin at 18 mU kg−1 min−1. Non-radiolabelled glucose infusion maintained plasma glucose at 10 mmol/l. Plasma glucose concentrations and [3H]glucose-specific activity were determined in 5 μl blood from the tail tip every 10 min during the last hour. For glucose turnover, [3H]glucose enrichments were determined in deproteinised blood by Zn(OH)2 precipitation; aliquots of the supernatant fraction were evaporated to dryness to determine radioactivity. In a second aliquot, glucose concentration was assessed by the glucose oxidase method. Plasma insulin was determined by ELISA (Mercodia) at study end to check that mice were stimulated comparably. Mice were killed by cervical dislocation. The liver glycogen synthesis rate was determined as described previously [31, 32] following extraction with 3% perchloric acid and precipitation with ethanol. The radioactive glycogen was counted and divided by the [3H] glucose-specific activity to determine the rate of synthesis.
C57Bl/KsJ db/db mice
Blood (20 μl) was obtained for glucose levels 45 min before dosing. Just prior to dosing, food was removed (free access to water), a further blood sample taken and mice dosed orally with PSN-GK1 (20 mg/kg) or vehicle, blood samples being removed 30, 60, 120, 180 and 300 min thereafter. Glucose was determined in whole blood as above.
ZDF rats
At age 10 to 11 weeks, rats were housed singly and fed high-fat diet (45% energy from fat, D1245; Research Diets) as follows during the 14-h dark phase: (1) free access (0–3 h); (2) food removed (3–7 h); (3) 8 g (7–14 h). After 30 days, the diet was changed to one in which 60% of energy was from fat (D12492; Research Diets). Treatment commenced at age 14 to 15 weeks and was conducted as follows: 1 h before lights out, a blood sample was obtained from the tail tip under local anaesthesia for basal glucose. Thirty minutes later, rats were dosed orally with PSN-GK1 (10 mg/kg) or vehicle. At the start of the dark phase, blood samples were taken for glucose, then the animals were fed as described above with hourly glucose sampling.
OGTTs in ob/ob mice
Food was withdrawn 5 h before OGTTs and throughout with free access to water provided. Blood (20 μl) was removed for basal glucose 45 min before OGTTs. Then mice were weighed and dosed orally with PSN-GK1 (3, 5 or 10 mg/kg) or vehicle 30 min before glucose (2 g/kg). Blood samples were taken 0, 30, 60, 90, 120, 180 and 240 min thereafter and glucose determined as above.
Subchronic study in ob/ob mice
On day 0, 23.5 h before first dose, blood glucose was determined and mice allocated to groups. The day after, an OGTT was performed as above, with oral PSN-GK1 (10 mg/kg) or vehicle administered at 11.30 h, 30 min before the glucose load (2 g/kg). After the OGTT, food was returned. PSN-GK1 or vehicle was dosed daily at 11.30 h. On days 3 and 6, glucose was measured in blood samples 15 min before and 60 min after dosing. Another OGTT was performed on day 8. On day 9, 3 h after dosing, terminal anaesthesia was induced and blood (500–600 μl) collected via the abdominal aorta into heparin/Li-containing tubes and kept on ice (<30 min), before centrifugation (2,800 g, 10 min, 4°C) to give plasma (≥300 μl), which was stored at −20°C for subsequent analysis (using kits) of fructosamine (Randox, Crumlin, Northern Ireland, UK), NEFA (Wako, Neuss, Germany), triacylglycerol (Thermotrace, VIC, Australia) and alanine aminotransferase (Randox). Livers were removed, freeze-clamped, weighed and stored (wrapped in foil) at −80°C for subsequent glycogen analysis by ethanol precipitation after alkali digestion and for glucosyl measurement after amyloglucosidase treatment.
Plasma PSN-GK1 concentrations
A satellite exposure study, linked to basal blood glucose-lowering/insulin secretion in C57Bl/6 mice, was performed, in which 12 mice were dosed with 10 mg/kg PSN-GK1. Following terminal anaesthesia, blood (500–600 μl) was collected from three animals via the abdominal aorta at 30, 60, 120 and 240 min after dosing. Blood was collected into heparin/Li-containing tubes and kept on ice (<30 min), before centrifugation (2,800 g, 10 min, 4°C) and storage at −20°C for subsequent compound measurement. A similar experiment was performed following a 5 mg/kg dose to ob/ob mice, with terminal blood collected after 30, 60, 150 and 270 min; these timepoints were used in a satellite exposure study paired with the OGTTs on days 1 and 8 (dosed daily) of the ob/ob study above.
Aliquots (50 μl) of plasma calibration standards, quality controls, unknown samples and blanks were placed into a 96-well protein precipitation plate (Argonaut Technologies, Hengoed, Wales, UK). The plate was placed on a vacuum manifold over a 96-well, 1-ml collection plate and acetonitrile (200 μl) added to each well. The plate was left for precipitation to occur and supernatant fractions to drip through under gravity for 10 min. Vacuum was applied and the block removed and centrifuged (3,000 g, 10 min) prior to injection on to a liquid chromatography/mass spectrometry/mass spectrometry system, comprising an HPLC column (Hichrom RPB; Highchrom, Theale, Berkshire, UK), 50 × 2.1 mm column, mobile phase of acetonitrile– 10 mmol/l ammonium formate, flow rate 0.25 ml/min. The Micromass Quattro Micro spectrometer (Waters, Milford, MA, USA) was fitted with an electrospray ionisation interface. PSN-GK1 was detected by selected reaction monitoring of daughter ions in negative ion mode.
Statistics
Analyses consisted of one-way ANOVA coupled with t tests. In cases where normality tests failed, the Mann-Whitney U test was used.
Results
Glucokinase activation in vitro
PSN-GK1 raised the glucose phosphorylating activity of glucokinase at 5 mmol/l glucose by 4.3 ± 0.2-fold with an EC50 of 130 ± 10 nmol/l (Fig. 1a); 54 ± 6 nmol/l PSN-GK1 doubled activity. At 30 μmol/l, PSN-GK1 did not affect any of the related hexokinases. Glucokinase activation by PSN-GK1 can be ascribed primarily to reduced glucose S 0.5 values (Fig. 1b, Table 1), with some modest increases in V max. Glucokinase kinetics for Mg-ATP were unaltered. The approximately sevenfold reduction in S 0.5 with 1 μmol/l PSN-GK1 corresponds to effects on the glucose cooperativity and reductions in Hill coefficient (Table 1). Effects of PSN-GK1 on glucokinase resemble those of GKAs reported to bind at the proposed allosteric activator site [26, 27].
Actions in cells
Effects of PSN-GK1 on insulin secretion from MIN6 clonal mouse pancreatic beta cells [33] were measured at basal and raised glucose concentrations (Fig. 2a). Like pancreatic beta cells, these cells exclusively express the liver-type glucose transporter (GLUT2, also known as SLC2A2) [34], which allows normal glucose-sensing where glucose phosphorylation, not transport, is rate-limiting [35]. At 5 mmol/l glucose, PSN-GK1 increased secretion 25.9 ± 5.3-fold with an EC50 of 267 ± 84 nmol/l. It also produced stimulations above the effects of raised glucose at 10 and 15 mmol/l. Although EC50s were lower at higher glucose concentrations, corresponding fold increases were not as large.
Effects of PSN-GK1 on clonal pancreatic beta cells and cultured rat hepatocytes. a Insulin secretion in MIN6 pancreatic beta cells in the presence of glucose (5 mmol/l, closed circles; 10 mmol/l, squares; 15 mmol/l, triangles; 25 mmol/l, open circles) and the indicated concentrations of PSN-GK1. Data are from a representative experiment of three repeat experiments. b 2-DG net uptake in cultured primary rat hepatocytes in the presence of 5.55 mmol/l glucose and the indicated concentrations of PSN-GK1 (squares) or sorbitol (circles). Results are mean ± SEM of four independent experiments. *p < 0.05, **p < 0.01 vs basal 2-DG uptake. Average basal 2-DG uptake was 1.38 pmol 2-DG per mg cellular protein
Glucokinase exerts strong control over hepatic glucose metabolism and glycogen synthesis [36]. Hence, activation is expected to produce increases in glucose uptake/metabolism in cultured hepatocytes, which contain the high-capacity GLUT2 glucose transporter [37]. Effects of PSN-GK1 on 2-DG uptake in primary rat hepatocytes in 5.55 mmol/l glucose (Fig. 2b) were compared with those of sorbitol. Sorbitol activates glucokinase indirectly through its metabolite, fructose-1-phosphate, which promotes the enzyme’s dissociation from its regulatory protein [38]. Relative to basal (100%), PSN-GK1 enhanced uptake 300 ± 34% with an EC50 of 1.04 ± 0.05 μmol/l, while the corresponding values for sorbitol were 137 ± 9% and 34.8 ± 6.7 μmol/l. PSN-GK1 also increased uptake at 15 mmol/l glucose, but to a lesser degree (not shown).
Effects in non-diabetic mice
PSN-GK1 rapidly lowered basal blood glucose and increased insulin in non-diabetic C57Bl/6 mice at 10 mg/kg (Fig. 3a,b), effects that were associated with good exposure (median PSN-GK1 concentration in μmol/l, n = 3, at time points as specified: 30 min = 11.7; 60 min = 9.7; 120 min = 7.0; 240 min = 4.1). At a dose of 1 mg/kg PSN-GK1 also lowered glucose, but without altering insulin.
PSN-GK1 lowers blood glucose levels through pancreatic and hepatic mechanisms. Blood glucose concentrations (a) and plasma insulin levels (b) following oral administration of vehicle (open circles) or PSN-GK1 (1 mg/kg, squares; 10 mg/kg, closed circles) to 5-h-fasted male C57Bl/6 mice. c Effect of vehicle (open bar) and PSN-GK1 (10 mg/kg by mouth; black bar) on liver glycogen biosynthesis rate under hyperinsulinaemic–hyperglycaemic conditions. *p < 0.05; **p < 0.01; ***p < 0.001 vs vehicle control
Effects of PSN-GK1 on liver glycogen biosynthesis were evaluated in a hyperinsulinaemic–hyperglycaemic clamp, with insulin at 18 mU kg−1 min−1 and glucose maintained at 10 mmol/l, employing a radiolabelled glucose tracer to monitor incorporation into liver glycogen. Glucose infusion rates at 150 to 210 min after vehicle or 10 mg/kg PSN-GK1 were 124.9 ± 4.8 and 139.1 ± 7.9 mg kg−1 min−1, respectively; at study end, plasma insulin values were 1,844 ± 213 and 1,803 ± 239 pmol/l, respectively. PSN-GK1 markedly raised the liver glycogen biosynthesis rate (Fig. 3c) (5.41 ± 1.40; vehicle: 0.89 ± 0.21 ng g tissue−1 min−1, p < 0.01), a phenomenon attributed directly to liver glucokinase activation.
Effects in db/db mice and ZDF rats
PSN-GK1 at 20 mg/kg produced rapid and significant antihyperglycaemia in fed (food removed immediately before dosing) db/db mice, compared with controls (Fig. 4). After 180 min, PSN-GK1 lowered blood glucose (from 20.5 ± 1.5 mmol/l to 5.8 ± 0.5 mmol/l) compared with controls (from 17.9 ± 1.4 to 13.0 ± 1.5 mmol/l).
PSN-GK1 (20 mg/kg by mouth; closed circles) attenuates hyperglycaemia compared with vehicle (open circles) in female db/db mice. a Blood glucose profile. b Delta delta blood glucose (ΔΔBG) profiles reflecting the difference between the change in blood glucose concentrations from time 0 min within each experimental group (ΔBG) and the change in blood glucose concentrations from time 0 min in the vehicle-treated arm (ΔBGvehicle). Thus, ΔΔBG = ΔBG–ΔBGvehicle. *p < 0.05; **p < 0.01; ***p < 0.001 vs vehicle control
ZDF rats were trained to a two-meal paradigm to monitor effects on glucose control over multiple meals. Following a single 10 mg/kg dose, PSN-GK1 lowered glycaemia at all time points during both meals and at nearly all time points between (Fig. 5), indicating an extended duration of action; blood glucose was 3.3–4.8 mmol/l and 3.4–4.0 mmol/l lower than vehicle-treated counterparts during the first and second meals, respectively.
The anti-hyperglycaemic effects of PSN-GK1 (10 mg/kg by mouth; closed circles) compared with vehicle (open circles) endure over two distinct meals in female ZDF rats. a Blood glucose profile. b Delta blood glucose values, which reflect the change in blood glucose from time 0 min within each experimental group, i.e. ΔBG = BGtime–BG0 min. *p < 0.05; **p < 0.01 vs vehicle control
OGTTs and subchronic effects in ob/ob mice
PSN-GK1 (5 mg/kg) improved glucose tolerance when administered 30 min before the glucose load (Fig. 6a). Glucose administration coincided with the PSN-GK1 maximum plasma concentration (median concentrations in μmol/l, n = 3, at specified time points: 30 min = 4.1; 60 min = 2.5; 150 min = 1.5; 270 min = 0.8). Effects were dose-dependent, 10 mg/kg reducing glucose excursions to a greater degree than doses of 3 and 5 mg/kg (not shown).
PSN-GK1 attenuates hyperglycaemia subchronically in ob/ob mice. a Blood glucose profile from an OGTT, in which PSN-GK1 (5 mg/kg by mouth; closed circles) and vehicle (open circles) were administered orally to male ob/ob mice 30 min prior to an oral glucose load (2 g/kg). b Effects of dosing 10 mg kg−1 day−1 PSN-GK1 (closed circles) and vehicle (open circles) to male ob/ob mice for nine consecutive days at T = 0 min each day. *p < 0.05; **p < 0.01 vs vehicle control
PSN-GK1 (10 mg/kg) was dosed once daily for 9 days. Comparable antihyperglycaemic effects were observed in OGTTs on days 1 and 8, where compound exposures were similar (Table 2). PSN-GK1 improved glucose profiles throughout vs controls (Fig. 6b). After 9 days, there were no significant differences (Table 2) between PSN-GK1- and vehicle-treated groups in body weight, plasma lipids, liver weights, liver glycogen, liver function (alanine aminotransferase levels) or plasma fructosamine, an index of medium- to long-term glucose control; however, the study may have been too short to reveal fructosamine differences.
Discussion
PSN-GK1 is a potent activator of glucokinase in vitro, possessing enhanced activity relative to the archetypal GKA Ro-28-1675. At 5 mmol/l glucose, PSN-GK1 at 0.05 μmol/l doubles glucokinase activity, whereas 0.18 μmol/l Ro-28-1675 increases activity only by 1.5-fold [21]. Although the recently disclosed GKA50 has an EC50 of 0.03 μmol/l [24, 39], no fold-activation data are available. Thus, PSN-GK1 is one of the most potent GKAs described to date. Like Ro-28-1675 and GKA50, PSN-GK1 principally increases catalytic effectiveness, expressed as the V max:S 0.5 ratio, by lowering S 0.5, as indicated by the fact that V max increases were modest. As expected, PSN-GK1 does not activate other hexokinases that do not possess glucokinase’s allosteric activator site [26].
PSN-GK1 markedly increases GSIR from MIN6 cells, most notably at lower glucose concentrations, where basal secretion is lower. However, effects are also observed at 10 and 15 mmol/l glucose, values more typical of the diabetic condition. Here, concentration-responses for PSN-GK1 are left-shifted, suggesting that, at higher glucose concentrations, smaller doses would still provide maximum secretion. The fact that higher PSN-GK1 concentrations are required to stimulate secretion at lower glucose concentrations may provide GKAs with an inbuilt safety mechanism that glucose-insensitive sulfonylureas [40] do not have. At 25 mmol/l glucose, PSN-GK1 does not augment secretion, consistent with a mechanism chiefly involving reduction in S 0.5 rather than increased V max.
The antihyperglycaemic properties of GKAs may also be mediated through enhanced hepatic glucose utilisation, so that activation will cause increases in uptake of glucose or other glucokinase substrates, such as non-metabolisable 2-DG. Glucokinase activation in hepatocytes, either pharmacologically or by adenoviral overexpression, results in increased 2-DG uptake [22, 30]. Stimulation of hepatic glucose phosphorylation by sorbitol, a precursor to the indirect GKA fructose-1-phosphate [38], has been reported with an EC50 of 20–30 μmol/l and stimulation of ∼1.5-fold [41], values similar to those seen in our hands in rat primary hepatocytes. PSN-GK1 has a substantially greater effect on 2-DG uptake, indicating that glucokinase activation occurs by a different mechanism.
In vitro effects in pancreatic and hepatic cells are translated in vivo in non-diabetic mice, where PSN-GK1 stimulated insulin secretion, reduced blood glucose and raised liver glycogen biosynthesis. The increased potency of PSN-GK1 compared with Ro-28-1675 is evident in this model: 15 mg/kg Ro-28-1675 maximally raised insulin ∼1.5-fold [21], while 10 mg/kg PSN-GK1 induced an approx. threefold increase. As mentioned, the hypoglycaemia provoked by GKAs in a non-diabetic setting may be more manageable than that resulting from sulfonylureas [40] because the glucose-lowering effected by GKAs is glucose-dependent [42, 43]. At 1 mg/kg, PSN-GK1 reduced blood glucose without hypoglycaemia, indicating that there is a reasonable window between glucose-lowering and severe hypoglycaemia. At this dose, no effects on insulin secretion were apparent, indicating that severe hypoglycaemic actions may be associated with insulinotropic effects. However, the fact that this dose was able to decrease blood glucose possibly indicates a hepatic action, although insulin levels were raised in view of the prevailing low glucose. Hyperinsulinaemic–hyperglycaemic clamps directly confirmed the hepatic contribution (Fig. 3c).
To date, there have been no reports of GKAs displaying antihyperglycaemic actions in db/db mice. Indeed, some GKAs, such as Ro-28-1675, lose their effectiveness in older db/db mice with blood glucose ∼16.7 mmol/l and hypoinsulinaemia [20]. In our study, by contrast, PSN-GK1 normalised blood glucose in db/db mice with initial blood glucose >20 mmol/l without hypoglycaemia. The potential of GKAs to control blood glucose is underscored by the fact that a single dose of PSN-GK1 can elicit antihyperglycaemic effects in high-fat-diet-fed female ZDF rats over multiple ‘meals’ and an extended time period without hypoglycaemia. To our knowledge, PSN-GK1 is the first GKA to show efficacy in this model.
PSN-GK1 improved glucose tolerance dose-dependently in ob/ob mice, again without hypoglycaemia. Like Ro-28-1675, PSN-GK1 appears to normalise blood glucose in rodent type 2 diabetes models, even though it produces hypoglycaemia in non-diabetic animals. It has been postulated [21] that GKAs do not provoke hypoglycaemia in diabetic rodents because of underlying defects in glucose homeostasis. The results seen acutely in OGTTs translate into subchronic efficacy, comparable antihyperglycaemic actions being noted at the beginning and end of the 9-day experiment, i.e. PSN-GK1’s effects did not appear to suffer from tachyphylaxis. Moreover, although PSN-GK1 improved blood glucose throughout this study, it did not alter liver glycogen, suggesting that GKAs lower blood glucose principally by a mechanism unrelated to increased glycogen storage.
One concern with GKAs is the possibility that they could increase lipid levels. In normal rodents, chronic glucokinase overexpression leads to raised hepatic lipogenesis and circulating lipids [44, 45]. However, humans with activating glucokinase mutations have normal lipids [15], hinting that long-term glucokinase activation may not produce adverse lipid effects. Effects of other GKAs on lipids following repeated administration have not been described. In our study, subchronic administration of PSN-GK1 did not affect plasma lipids, indicating that concerns surrounding GKAs and increased lipogenesis may be unfounded. However, longer term studies will be required ultimately to ensure that GKAs are safe in this regard. It was also discovered that PSN-GK1 did not induce changes in liver weight or plasma alanine aminotransferase, an indicator of liver toxicity and steatosis.
In summary, we have demonstrated that PSN-GK1’s ability to activate glucokinase results in robust hypoglycaemic effects in normal mice and antihyperglycaemic actions in diabetic rodents. The overall efficacy, plus the fact that no adverse events were observed subchronically, further supports the premise that GKAs may be among the next generation of oral glucose-lowering therapies. In contrast to current therapies that target a single organ, e.g. sulfonylureas (pancreas) or metformin (liver), GKAs could achieve greater efficacy by targeting multiple sites in the body. Several GKAs are now in human clinical trials. Results from these trials will determine whether they can distinguish themselves from the widely prescribed sulfonylureas, which are associated with increased mortality [46] as a result of raised cardiovascular risk [47] and may accelerate beta cell apoptosis and exhaustion [48, 49].
Abbreviations
- 2-DG:
-
2-deoxy-d-[3H]glucose
- EC50 :
-
median effective concentration
- G6PDH:
-
glucose-6-phosphate dehydrogenase
- GKA:
-
glucokinase activator
- GSIR:
-
glucose-stimulated insulin release
- GST:
-
glutathione S-transferase
- PSN-GK1:
-
(2R)-2-(4-cyclopropanesulphonylphenyl)-N-(5-fluorothiazol-2-yl)-3-(tetrahydropyran-4-yl)propionamide
- S 0.5 :
-
substrate concentration at half maximal velocity
- V max :
-
maximal velocity
- ZDF:
-
Zucker diabetic fatty
References
Gershell L (2005) Type 2 diabetes market. Nature Rev Drug Discov 4:367–368
Bell DSH (2004) A comparison of agents used to manage type 2 diabetes mellitus: need for reappraisal of traditional approaches. Treat Endocrinol 3:67–76
Wagman AS, Nuss JM (2001) Current therapies and emerging targets for the treatment of diabetes. Curr Pharmaceut Design 7:417–450
Kietzmann T, Ganjam GK (2005) Glucokinase: old enzyme, new target. Expert Opin Therap Patents 15:705–713
Printz RL, Granner DK (2005) Tweaking the glucose sensor: adjusting glucokinase activity with activator compounds. Endocrinology 146:3693–3695
Magnuson MA, Matschinsky FM (2004) Glucokinase as a glucose sensor: past, present, and future. In: Matschinsky FM, Magnuson MA (eds) Glucokinase and glycemic disease: from basics to novel therapeutics. Karger, Basel, pp 1–17
Matschinsky FM, Magnuson MA, Zelent D et al (2006) The network of glucokinase-expressing cells in glucose homeostasis and the potential of glucokinase activators for diabetes therapy. Diabetes 55:1–12
Baltrusch S, Tiedge M (2006) Glucokinase regulatory network in pancreatic β-cells and liver. Diabetes 55(Suppl 2):S55–S64
Kang L, Dunn-Meynell AA, Routh VH et al (2006) Glucokinase is a critical regulator of ventromedial hypothalamic neuronal glucosensing. Diabetes 55:412–420
Theodorakis MJ, Carlson O, Michopoulos S et al (2006) Human duodenal enteroendocrine cells: source of both incretin peptides, GLP-1 and GIP. Am J Physiol Endocrinol Metab 290:E550–E559
Zelent D, Golson ML, Koeberlein B et al (2006) A glucose sensor role for glucokinase in anterior pituitary cells. Diabetes 55:1923–1929
Velho G, Froguel P, Gloyn A, Hattersley A (2004) Maturity onset diabetes of the young type 2. In: Matschinsky FM, Magnuson MA (eds) Glucokinase and glycemic disease: from basics to novel therapeutics. Karger, Basel, pp 42–64
Sagen JV, Odili S, Bjørkhaug L et al (2006) From clinicogenetic studies of maturity-onset diabetes of the young to unraveling complex mechanisms of glucokinase regulation. Diabetes 55:1713–1722
Heredia VV, Carlson TJ, Garcia E, Sun S (2006) Biochemical basis of glucokinase activation and the regulation by glucokinase regulatory protein in naturally occurring mutations. J Biol Chem 281:40201–40207
Christesen HBT, Herold K, Noordam K, Gloyn AL (2004) Glucokinase-linked hypoglycemia: Clinical aspects of activating glucokinase mutations. In: Matschinsky FM, Magnuson MA (eds) Glucokinase and glycemic disease: from basics to novel therapeutics. Karger, Basel, pp 75–91
Al-Hasani H, Tschöp MH, Cushman SW (2003) Two birds with one stone: Novel glucokinase activator stimulates glucose-induced pancreatic insulin secretion and augments hepatic glucose metabolism. Mol Interventions 3:367–370
Leighton B, Atkinson A, Coghlan MP (2005) Small molecule glucokinase activators as novel anti-diabetic agents. Biochem Soc Trans 33:371–374
Van Gaal LF, De Leeuw IH (2003) Rationale and options for combination therapy in the treatment of Type 2 diabetes. Diabetologia 46(Suppl 1):M44–M50
Guertin KR, Grimsby J (2006) Small molecule glucokinase activators as glucose lowering agents: a new paradigm for diabetes therapy. Curr Med Chem 13:1839–1843
Grimsby J, Sarabu R, Corbett WL et al (2003) Allosteric activators of glucokinase: potential role in diabetes therapy. Science 301:370–373
Grimsby J, Matschinsky FM, Grippo JF (2004) Discovery and actions of glucokinase activators. In: Matschinsky FM, Magnuson MA (eds) Glucokinase and glycemic disease: from basics to novel therapeutics. Karger, Basel, pp 360–378
Efanov AM, Barrett DG, Brenner MB et al (2005) A novel glucokinase activator modulates pancreatic islet and hepatocyte function. Endocrinology 146:3696–3701
Sarabu R, Grimsby J (2005) Targeting glucokinase activation for the treatment of type 2 diabetes—a status review. Curr Opin Drug Discov Dev 8:631–637
McKerrecher D, Allen JV, Caulkett PWR et al (2006) Design of a potent, soluble glucokinase activator with excellent in vivo efficacy. Bioorg Med Chem Lett 16:2705–2709
Futamura M, Hosaka H, Kadotani A et al (2006) An allosteric activator of glucokinase impairs the interaction of glucokinase and glucokinase regulatory protein and regulates glucose metabolism. J Biol Chem 281:37668–37674
Dunten P, Swain A, Kammlott U et al (2004) Crystal structure of human liver glucokinase bound to a small molecule allosteric activator. In: Matschinsky FM, Magnuson MA (eds) Glucokinase and glycemic disease: from basics to novel therapeutics. Karger, Basel, pp 145–154
Kamata K, Mitsuya M, Nishimura T, Eiki J-I, Nagata Y (2004) Structural basis for allosteric regulation of the monomeric allosteric enzyme human glucokinase. Structure 12:429–438
Fyfe MCT, Gardner LS, Nawano M et al (2004) Tri(cyclo) substituted amide compounds. International Patent Publication WO 2004/072031
Fyfe MCT, Naud F (2006) Fluorination process of protected aminothiazole. International Patent Publication WO 2006/016174
Yang R, Cao L, Gasa R, Brady MJ, Sherry AD, Newgard CB (2002) Glycogen-targeting subunits and glucokinase differentially affect pathways of glycogen metabolism and their regulation in hepatocytes. J Biol Chem 277:1514–1523
Massillon D, Chen W, Hawkins M, Liu R, Barzilai N, Rossetti L (1995) Quantitation of hepatic glucose fluxes and pathways of hepatic glycogen synthesis in conscious mice. Am J Physiol Endocrinol Metab 269:E1037–E1043
Perrin C, Knauf C, Burcelin R (2004) Intracerebroventricular infusion of glucose, insulin, and the adenosine monophosphate-activated kinase activator, 5-aminoimidazole-4-carboxamide-1-β-D-ribofuranoside, controls muscle glycogen synthesis. Endocrinology 145:4025–4033
Miyazaki J, Araki K, Yamato E et al (1990) Establishment of a pancreatic beta cell line that retains glucose inducible insulin secretion: special reference to expression of glucose transporter isoforms. Endocrinology 127:126–132
Leturque A, Brot-Laroche E, Le Gall M, Stolarczyk E, Tobin V (2006) The role of GLUT2 in dietary sugar handling. J Physiol Biochem 61:529–538
Tal M, Wu Y, Leiser M et al (1992) [Val12]HRAS downregulates GLUT2 in β cells of transgenic mice without affecting glucose homeostasis. Proc Natl Acad Sci U S A 89:5744–5748
Agius L (1998) The physiological role of glucokinase binding and translocation in hepatocytes. Adv Enzyme Regul 38:303–331
Zheng Q, Levitsky LL, Mink K, Rhoads DB (1995) Glucose regulation of glucose transporters in cultured adult and fetal hepatocytes. Metabolism 44:1553–1558
Veiga-Da-Cunha M, Van Schaftingen E (2002) Identification of fructose 6-phosphate- and fructose 1-phosphate-binding residues in the regulatory protein of glucokinase. J Biol Chem 277:8466–8473
Coope GJ, Atkinson AM, Allott C et al (2006) Predictive blood glucose lowering efficacy by glucokinase activators in high fat fed female Zucker rats. Br J Pharmacol 149:328–335
Light PE (2002) The ABCs of sulfonylurea receptors, islet KATP channels and the control of insulin secretion. Can J Diabetes 26:223–231
Brocklehurst KJ, Payne VA, Davies RA et al (2004) Stimulation of hepatocyte glucose metabolism by novel small molecule glucokinase activators. Diabetes 53:535–541
Matschinsky FM, Glaser B, Magnuson MA (1998) Pancreatic β-cell glucokinase: closing the gap between theoretical concepts and experimental realities. Diabetes 47:307–315
Zelent D, Najafi H, Odili S et al (2005) Glucokinase and glucose homeostasis: proven concepts and new ideas. Biochem Soc Trans 33:306–310
O’Doherty RM, Lehman DL, Telemaque-Potts S, Newgard CB (1999) Metabolic impact of glucokinase overexpression in liver. Lowering of blood glucose in fed rats is accompanied by hyperlipidemia. Diabetes 48:2022–2027
Ferre T, Riu E, Franckhauser S, Agudo J, Bosch F (2003) Long-term overexpression of glucokinase in the liver of transgenic mice leads to insulin resistance. Diabetologia 46:1662–1668
Simpson SH, Majumdar SR, Tsuyuki RT, Eurich DT, Johnson JA (2006) Dose–response relation between sulfonylurea drugs and mortality in type 2 diabetes mellitus: a population-based cohort study. Can Med Assoc J 174:169–174
Bell DSH (2006) Do sulfonylurea drugs increase the risk of cardiac events? Can Med Assoc J 174:185–186
Donath MY, Ehses JA, Maedler K et al (2005) Mechanisms of β-cell death in type 2 diabetes. Diabetes 54(Suppl 2):S108–S113
Del Prato S, Pulizzi N (2006) The place of sulfonylureas in the therapy for type 2 diabetes mellitus. Metab Clin Exp 55(Suppl 1):S20–S27
Acknowledgements
We are grateful to F. Naud of Solvias (Basel, Switzerland) for the synthesis of PSN-GK1 and to Gattefossé (Gennevilliers, France) for generously supplying us with Gelucire 44/14. The MIN6 cells were kindly supplied by J. Miyazaki of Osaka University Graduate School of Medicine, Osaka, Japan. We also acknowledge M. Cawthorne, M. Sennitt and D. Hislop from Buckingham University for in vivo pharmacology experiments, as well as L. Bertram, C. Rasamison, V. Shah and G. Williams from (OSI)Prosidion (Oxford, UK) for technical support. The following are thanked for helpful discussion: K. Lindhardt and M. Thomsen from (OSI)Prosidion, R. Burcelin from University Paul Sabatier (Toulouse, France) and A. Cherrington and D. Granner from Vanderbilt University School of Medicine, USA.
Duality of interest
E. Wargent, R. L. Printz and T. Sulpice conducted studies on a fee-for-service basis. M. C. T. Fyfe, J. R. White, A. Taylor, R. Chatfield, M. J. Procter, C. Reynet, J. G. McCormack, P. S. Widdowson and P. Wong-Kai-In are all employed by (OSI)Prosidion and own stock or have stock options in (OSI)Pharmaceuticals (Melville, NY, USA).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fyfe, M.C.T., White, J.R., Taylor, A. et al. Glucokinase activator PSN-GK1 displays enhanced antihyperglycaemic and insulinotropic actions. Diabetologia 50, 1277–1287 (2007). https://doi.org/10.1007/s00125-007-0646-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-007-0646-8