Abstract
Aims/hypothesis
Although the variable number tandem repeat (VNTR) minisatellite 5′ to the insulin gene is among the most studied polymorphisms in diabetes, the relationships between VNTR variation, diabetes-related traits and predisposition to type 2 diabetes remain unclear. Since inadequate sample size is likely to have been an obstacle to reliable inference, we examined the relationship between VNTR variation and a range of diabetes-related traits in a cohort of 5,753 Finnish adults.
Materials and methods
VNTR genotypes were derived, by typing at the −23HphI variant site, for 5,646 individuals from the Northern Finland Birth Cohort 1966. Associations were sought between these genotypes and a range of anthropometric (BMI, WHR), physiological (blood pressure) and biochemical (fasting glucose, insulin, lipids, indices of insulin sensitivity and beta cell function) measures obtained at clinical examination at 31 years.
Results
We found no evidence that VNTR genotype was significantly associated with measures of insulin secretion, insulin sensitivity, glycaemia, adiposity or blood pressure.
Conclusions/interpretation
Despite evidence from several relatively small studies suggesting that INS-VNTR genotypes are associated with predisposition to type 2 diabetes, reduced beta cell function and measures of adiposity, the present study failed to detect any association with a range of diabetes-related traits. Taken with other recent studies in large population-based cohorts, these data suggest that previous studies have, at the very least, overestimated the influence of the INS-VNTR on type 2 diabetes-related traits. The effects of INS-VNTR variation on insulin transcription observed in vitro appear not to translate into detectable differences in basal insulin secretion in humans.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In the search for variants that influence susceptibility to type 2 diabetes and related physiological traits, few candidate genes have stronger biological credentials than the insulin gene itself. Disordered insulin secretion is one of the cardinal features of this condition and sequence variants within the insulin gene coding region are known to cause one rare form of diabetes [1]. In efforts to identify common variation that might explain a greater proportion of phenotypic variation at the population level, focus has been directed towards the variable number tandem repeat (VNTR) minisatellite element ~500 bp upstream of the insulin gene [2]. Sequence and length diversity within this element modifies insulin transcription in vitro [3, 4], and, in type 1 diabetes, VNTR composition clearly influences disease susceptibility, most likely through modulation of thymic insulin expression [5]. Recent studies have emphasised that, for type 1 diabetes at least, the major (and probably sole) susceptibility variant in the region is the VNTR itself, the shorter class III alleles being protective [2, 6].
In contrast, attempts to relate VNTR variation to type 2 diabetes and related traits paint a much less clear picture. Early case-control studies supported an association between class III alleles and type 2 diabetes [2], a finding consistent with in vitro data relating class III alleles to reduced pancreatic expression of insulin [3, 4]. Further support for this association has come from studies showing excess class III transmission from heterozygous fathers to diabetic offspring [7]; increased risk of glucose intolerance in elderly men with class III homozygosity [8]; and evidence that individuals with the class III allele have disordered insulin secretion [9, 10]. However, other (larger) studies have failed to corroborate these associations [11, 12]. Most recently, Hansen and colleagues found no association with type 2 diabetes in a study of 1,462 cases and 4,931 glucose-tolerant controls [12]. A similar pattern of confusing and often mutually contradictory findings has been reported for analyses of the associations between the VNTR and birthweight [11, 13–16], polycystic ovary syndrome [17–20] and obesity [12, 15, 21–24].
Much of the inconsistency of genetic association studies can be attributed to the consequences of inadequate sample size [25], and this is likely to have been a contributory factor in many of the studies listed above. In the present study, we report analyses of the insulin VNTR and its relationship to multiple adult metabolic traits in a sample of 5,753 Finns from a large birth cohort examined at age 31 years.
Subjects, materials and methods
Subjects
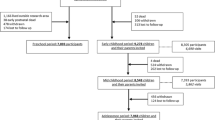
The study sample comprised individuals from the Northern Finnish Birth Cohort 1966 (NFBC 1966). This study originally identified 96% of all women in the northernmost two provinces of Finland expected to deliver during 1966 (12,058 live births, all of European Caucasian origin), and included longitudinal follow-up of the offspring [26]. At 31 years, all offspring still living in northern Finland or the Helsinki area (n=8,463) were recontacted and invited for clinical examination (response rate 71%) and DNA sampling (5,753 samples available). At this examination, standard anthropometric and blood pressure measures were made and fasting samples taken for assays of glucose, insulin and lipids. Characteristics of the study population are given in Table 1. Phenotyping procedures and biochemical assays are detailed elsewhere [16, 27, 28]. Paired fasting glucose and insulin levels were used to generate measures of beta cell function and insulin sensitivity using the homeostatic model assessment (HOMA) of beta cell function (HOMA%B) and insulin sensitivity (HOMA%S) [29]. The study was conducted with approval of the ethics committee of the universities of Oulu and Oxford and in accordance with the principles of the Declaration of Helsinki.
Genotyping
The −23HphI variant (rs689) was typed as a surrogate for VNTR class: in Finns, as in other non-African populations, these are in tight linkage disequilibrium [30]. Genotyping was performed in duplicate, using both a PCR-RFLP and a mass-spectrometry assay, with discrepant calls resolved using a four-primer ARMS (amplification–refractory mutation system)-PCR assay [16]. In addition, TT (i.e. class III homozygote) genotypes were reconfirmed (with no discrepancies detected) by ARMS-PCR, direct sequencing and/or pyrosequencing. A final round of ARMS-PCR, retyping of 384 samples identified only one genotype discrepancy compared with the assigned genotype. Thus, we estimate our overall error rate as ∼0.1%. Assay design and genotyping quality control data are described in greater detail elsewhere [16].
Statistical analysis
The relationship between −23HphI genotype and phenotypes of interest was examined by multiple linear regression modelling using SAS (version 8.2; ASA, Cary, NC, USA) and SPSS (version 11.5 for Windows; SPSS, Chicago, IL, USA) programs. We considered three genotype models: recessive (TT vs A/−); dominant (AA vs T/−); and additive (assuming a linear relationship between number of T alleles and the trait of interest). Variables were logarithmically transformed where appropriate. For all biochemical measures, we excluded individuals who were not fasted (n=236): in addition, analyses of glucose, insulin and HOMA measures excluded those receiving treatment for diabetes (n=34, of whom 19 were also non-fasting). Analyses were optionally adjusted for confounding and/or other explanatory or contributory variables, including sex and BMI, WHR, smoking, alcohol consumption and socioeconomic status (as assessed at age 31). Adjusted analyses included between 4,863 and 5,365 individuals. Where BMI or WHR were outcomes, neither was included in the adjustments. The full list of variables included in these adjustments is as shown in Table 1. Unless otherwise stated, all significance values reported are those for the fully adjusted analyses. Given indications that the phenotypic consequences of INS-VNTR variation may be influenced by early life events [8, 13, 14], the longitudinal nature of the cohort allowed us to repeat analyses after stratification by postnatal growth realignment [13] and birth order [14]. The former divided subjects into ‘non-changers’, ‘change-downers’ and ‘change-uppers’ based on comparison of sex- and gestational age-adjusted SD scores for weight at birth and 1 year (the latter available for 4,788 individuals). The boundaries for each stratum were set at a change in SD score of ±0.67 [13]. Stratification by parity considered first-borns and those from second or subsequent pregnancies.
Results
Genotypes were obtained for 5,646 individuals (98% of the available sample), 3,859 of whom (68.3%) were homozygous for A (equivalent to VNTR class I), 1,646 (29.2%) heterozygous and 141 (2.5%) homozygous for T (VNTR class III). These genotype frequencies did not deviate significantly from Hardy–Weinberg equilibrium. As previously noted [31, 32], the class III allele frequency is lower in Finns than other European populations.
There was no evidence (at the 5% significance level) that, after adjustment, VNTR genotype influenced any of the traits examined under any of the models tested (Table 2). Specifically, there was no association with measures of insulin secretion (fasting insulin, HOMA%B), of insulin sensitivity (fasting insulin, HOMA%S, fasting lipids), adiposity (BMI, WHR), glycaemia (fasting glucose) or blood pressure (systolic, diastolic). Though the analysis of WHR generated a nominally significant p value on the unadjusted analysis (p=0.02), any trends were abolished after adjustment for, or stratification by, sex (males, p=0.72, females, p=0.10).
Analyses of the same traits after stratification based on early growth trajectory or birth order failed to generate any consistent evidence for association (no individual p value <0.01, data not shown).
Discussion
In this study of over 5,500 Finns examined at age 31, we found no evidence that variation at the −23HphI site (and more pertinently, the VNTR with which it is in tight linkage disequilibrium) influences metabolic traits related to type 2 diabetes. These data help to resolve some of the remaining uncertainties about the role of this variant in the development of type 2 diabetes and population variation in diabetes-related quantitative metabolic traits.
While several small studies have suggested that class III individuals have reduced insulin levels [9], altered insulin pulsatility [10] and an increased risk of type 2 diabetes [2, 7], the findings from larger studies (likely to be less susceptible to sampling error and to selection and publication biases) have been less clear. In ∼2,000 subjects from the Northwick Park Study, Rodriguez and colleagues reported that class III-bearing haplotypes were associated with diverse features of insulin resistance, including elevated blood pressure, fat mass and triglyceride levels [24]. Class III homozygosity was also associated with a modest, nominally significant increase in BMI and insulin resistance in a study of 1,306 UK individuals [15]. We have been unable to substantiate these findings, and our findings are more in line with the only other very large study of this variant, which in 4,444 middle-aged Danish subjects, failed to detect any association whatsoever with a range of diabetes-related metabolic traits [12]. The design of the present study did not allow us to explore the role of INS-VNTR variation in type 2 diabetes susceptibility per se. It is worth noting that it has often proved surprisingly difficult to identify associations with diabetes-related intermediate traits, even for variants widely recognised to influence susceptibility to type 2 diabetes, such as P12A in PPARG [33, 34] and E23K in KCNJ11 [35, 36]. However, a recent study in Danes found no association between INS-VNTR genotype and type 2 diabetes in a comparison of 1,462 diabetic subjects and 4,931 normal glucose-tolerant controls [12].
There are several possible explanations for these discrepant findings. The accuracy and reliability of phenotyping is always an issue but the present study featured standardised and quality-controlled clinical examination by experienced investigators, and robust biochemical assays performed in a single laboratory. In addition, duplicate genotyping was used to minimise technical errors. Hence, neither genotyping nor phenotyping error is likely to explain our failure to detect associations seen in the other studies.
Similarly, ethnic differences in regional linkage disequilibrium patterns are unlikely to be relevant since these are known to be similar in all non-African groups [30]. While the lower frequency of class III alleles in the Finnish cohort compared with other Europeans (17% in the present study vs ∼30%) may have reduced our power to detect class III effects (particularly if restricted to class III homozygotes), this is compensated for by the greater sample size of the present study, in which absolute numbers of class III homozygotes are comparable with, or exceed, those reported by Hansen and colleagues [12] and Rodriguez and colleagues [24]. While it is conceivable that the appreciable ethnic differences in VNTR class frequency that are apparent even in non-African populations [30] may have rendered studies of this locus susceptible to the consequences of latent population stratification [37], available data comparing case-control and family-based association analyses do not support this concern [2, 7].
In addition, it is important to point out that in the present study we did not, in the absence of parental DNA, have the opportunity to test for parent-of-origin effects. Significant parent-of-origin effects have previously been detected at the INS-VNTR in relation to PCOS [38], type 1 diabetes [2], type 2 diabetes [7] and childhood obesity [22], and are consistent with known imprinting in this region [39]. While the size of the present study provides reasonable power to detect biologically relevant association effects even if these are restricted to alleles transmitted from one parent alone, the variable capacity to test for such effects may have contributed to some of the inconsistency in the literature.
An important related question is whether variants at the IGF2-INS-TH locus other than the insulin gene VNTR are involved in the modulation of metabolic risk. The evidence from type 1 diabetes points ever more strongly to the VNTR as the underlying susceptibility variant [6], but this does not necessarily imply that the same holds in type 2 diabetes. Indeed, the Southampton group have suggested in several studies (albeit on a single cohort) that variants within the IGF2 gene may also contribute to variation in adiposity and other insulin-resistance traits [21, 40]. However, their most recent study on this cohort, featuring an extensive haplotypic analysis of the IGF2-INS-TH region [24], suggests that much of the evidence for IGF2 association resides on class III-bearing haplotypes, once again focusing attention on the VNTR. Further large-scale studies of the full IGF2-INS-TH region will be necessary to gain a robust estimate of the specific consequences of variation within the IGF2 gene, but the present study, along with the study by Hansen and colleagues [12], certainly casts serious doubt on the importance of the VNTR as a determinant of adult metabolic function.
In this respect, the present findings coincide with data from other recent large-scale studies that have failed to substantiate the role of the VNTR as a source of human phenotypic variation. Recently, in the same Finnish cohort, we could detect no association between VNTR genotype and birthweight and other early growth variables [16], in contrast to earlier positive studies in UK and Pima samples (though these had reported effects in the opposite direction to each other) [11, 13]. Similarly, as described above, the only large case-control study for type 2 diabetes has failed to corroborate earlier positive findings [12].
In a recent meta-analysis, small sample size was shown to be a significant risk factor for the generation of association results that could not be replicated on subsequent examination [25]. These recent findings from large-scale studies of the INS-VNTR minisatellite seem likely to provide additional examples of the potential dangers of inadequate sample size in complex trait association studies.
Abbreviations
- ARMS:
-
amplification–refractory mutation system
- HOMA:
-
homeostatic model assessment
- HOMA%B:
-
homeostatic model assessment of beta cell function
- HOMA%S:
-
homeostatic model assessment of insulin sensitivity
- VNTR:
-
variable number tandem repeat
References
Gabbay KH (1980) The insulinopathies. N Engl J Med 302:165–167
Bennett ST, Todd JA (1996) Human type 1 diabetes and the insulin gene: principles of mapping polygenes. Annu Rev Genet 30:343–370
Bennett ST, Wilson AJ, Cucca F et al (1996) IDDM2-VNTR-encoded susceptibility to type 1 diabetes: dominant protection and parental transmission of alleles of the insulin gene-linked minisatellite locus. J Autoimmun 9:415–421
Vafiadis P, Bennett ST, Colle E et al (1996) Imprinted and genotype-specific expression of genes at the IDDM2 locus in pancreas and leucocytes. J Autoimmun 9:397–403
Vafiadis P, Ounissi-Benkalha H, Palumbo M et al (2001) Class III alleles of the variable number of tandem repeat insulin polymorphism associated with silencing of thymic insulin predispose to type 1 diabetes. J Clin Endocrinol Metab 86:3705–3710
Barratt BJ, Payne F, Lowe CE et al (2004) Remapping the insulin gene/IDDM2 locus in type 1 diabetes. Diabetes 53:1884–1889
Huxtable SJ, Saker PJ, Haddad L et al (2000) Analysis of parent–offspring trios provides evidence for linkage and association between the insulin gene and type 2 diabetes mediated exclusively through paternally transmitted class III variable number tandem repeat alleles. Diabetes 49:126–130
Ong KK, Phillips DI, Fall C et al (1999) The insulin gene VNTR, type 2 diabetes and birth weight. Nat Genet 21:262–263
Cocozza S, Riccardi G, Monticelli A et al (1988) Polymorphism at the 5′ end flanking region of the insulin gene is associated with reduced insulin secretion in healthy individuals. Eur J Clin Invest 18:582–586
Ahmed S, Bennett ST, Huxtable SJ et al (1999) INS VNTR allelic variation and dynamic insulin secretion in healthy adult non-diabetic Caucasian subjects. Diabet Med 16:910–917
Lindsay RS, Hanson RL, Wiedrich C et al (2003) The insulin gene variable number tandem repeat class I/III polymorphism is in linkage disequilibrium with birth weight but not Type 2 diabetes in the Pima population. Diabetes 52:187–193
Hansen SK, Gjesing AP, Rasmussen SK et al (2004) Large-scale studies of the HphI insulin gene variable-number-of-tandem-repeats polymorphism in relation to Type 2 diabetes mellitus and insulin release. Diabetologia 47:1079–1087
Dunger DB, Ong KK, Huxtable SJ et al (1998) Association of the INS VNTR with size at birth. ALSPAC Study Team. Avon Longitudinal Study of Pregnancy and Childhood. Nat Genet 19:98–100
Ong KK, Petry CJ, Barratt BJ et al (2004) Maternal–fetal interactions and birth order influence insulin variable number of tandem repeats allele class associations with head size at birth and childhood weight gain. Diabetes 53:1128–1133
Mitchell SM, Hattersley AT, Knight B et al (2004) Lack of support for a role of the insulin gene variable number of tandem repeats minisatellite (INS-VNTR) locus in fetal growth or type 2 diabetes-related intermediate traits in United Kingdom populations. J Clin Endocrinol Metab 89:310–317
Bennett AJ, Sovio U, Ruokonen A et al (2004) Variation at the insulin gene VNTR (variable number tandem repeat) polymorphism and early growth: studies in a large Finnish birth cohort. Diabetes 53:2126–2131
Waterworth DM, Bennett ST, Gharani N et al (1997) Linkage and association of insulin gene VNTR regulatory polymorphism with polycystic ovary syndrome. Lancet 349:986–990
Urbanek M, Legro RS, Driscoll DA et al (1999) Thirty-seven candidate genes for polycystic ovary syndrome: strongest evidence for linkage is with follistatin. Proc Natl Acad Sci U S A 96:8573–8578
Calvo RM, Telleria D, Sancho J, San Millan JL, Escobar-Morreale HF (2002) Insulin gene variable number of tandem repeats regulatory polymorphism is not associated with hyperandrogenism in Spanish women. Fertil Steril 77:666–668
Michelmore K, Ong K, Mason S et al (2001) Clinical features in women with polycystic ovaries: relationships to insulin sensitivity, insulin gene VNTR and birth weight. Clin Endocrinol (Oxf) 55:439–446
O’Dell SD, Bujac SR, Miller GJ, Day IN (1999) Associations of IGF2 ApaI RFLP and INS VNTR class I allele size with obesity. Eur J Hum Genet 7:821–827
Le Stunff C, Fallin D, Bougneres P (2001) Paternal transmission of the very common class I INS VNTR alleles predisposes to childhood obesity. Nat Genet 29:96–99
Le Stunff C, Fallin D, Schork NJ, Bougneres P (2000) The insulin gene VNTR is associated with fasting insulin levels and development of juvenile obesity. Nat Genet 26:444–446
Rodriguez S, Gaunt TR, O’Dell SD et al (2004) Haplotypic analyses of the IGF2-INS-TH gene cluster in relation to cardiovascular risk traits. Hum Mol Genet 13:715–725
Ioannidis JP, Trikalinos TA, Ntzani EE, Contopoulos-Ioannidis DG (2003) Genetic associations in large versus small studies: an empirical assessment. Lancet 361:567–571
Rantakallio P (1988) The longitudinal study of the northern Finland birth cohort of 1966. Paediatr Perinat Epidemiol 2:59–88
Taponen S, Martikainen H, Jarvelin MR et al (2003) Hormonal profile of women with self-reported symptoms of oligomenorrhea and/or hirsutism: northern Finland birth cohort 1966 study. J Clin Endocrinol Metab 88:141–147
Taponen S, Martikainen H, Jarvelin MR et al (2004) Metabolic cardiovascular disease risk factors in women with self-reported symptoms of oligomenorrhea and/or hirsutism: northern Finland birth cohort 1966 study. J Clin Endocrinol Metab 89:2114–2118
Levy JC, Matthews DR, Hermans MP (1998) Correct homeostasis model assessment (HOMA) evaluation uses the computer program. Diabetes Care 21:2191–2192
Stead JD, Jeffreys AJ (2002) Structural analysis of insulin minisatellite alleles reveals unusually large differences in diversity between Africans and non-Africans. Am J Hum Genet 71:1273–1284
Metcalfe KA, Hitman GA, Fennessy MJ et al (1995) In Finland insulin gene region encoded susceptibility to IDDM exerts maximum effect when there is low HLA-DR associated risk. DiMe (childhood diabetes in Finland) Study Group. Diabetologia 38:1223–1229
Undlien DE, Bennett ST, Todd JA et al (1995) Insulin gene region-encoded susceptibility to IDDM maps upstream of the insulin gene. Diabetes 44:620–625
Altshuler D, Hirschhorn JN, Klannemark M et al (2000) The common PPARgamma Pro12Ala polymorphism is associated with decreased risk of type 2 diabetes. Nat Genet 26:76–80
Li S, Chen W, Srinivasan SR, Boerwinkle E, Berenson GS, The Bogalusa Heart Study (2003) The peroxisome proliferator-activated receptor-gamma2 gene polymorphism (Pro12Ala) beneficially influences insulin resistance and its tracking from childhood to adulthood: the Bogalusa Heart Study. Diabetes 52:1265–1269
Gloyn AL, Weedon MN, Owen KR et al (2003) Large scale association studies of variants in genes encoding the pancreatic beta-cell K-ATP channel subunits Kir6.2 (KCNJ11) and SUR1 (ABCC8) confirm that the KCNJ11 E23K variant is associated with increased risk of Type 2 diabetes. Diabetes 52:568–572
Weedon MN, Gloyn AL, Frayling TM, Hattersley AT, Davey Smith G, Ben-Shlomo Y (2003) Quantitative traits associated with the Type 2 diabetes susceptibility allele in Kir6.2. Diabetologia 46:1021–1023
Cardon LR, Palmer LJ (2003) Population stratification and spurious allelic association. Lancet 361:598–604
Bennett ST, Todd JA, Waterworth DM, Franks S, McCarthy MI (1997) Association of insulin gene VNTR polymorphism with polycystic ovary syndrome. Lancet 349:1771–1772
Moore GE, Abu-Amero SN, Bell G et al (2001) Evidence that insulin is imprinted in the human yolk sac. Diabetes 50:199–203
Gaunt TR, Cooper JA, Miller GJ, Day IN, O’Dell SD (2001) Positive associations between single nucleotide polymorphisms in the IGF2 gene region and body mass index in adult males. Hum Mol Genet 10:1491–1501
Acknowledgements
This study was conducted with the support of the Wellcome Trust (Grant 069224), the Academy of Finland and the European Commission (Framework 5 award QLG1-CT-2000-01643). We acknowledge the many subjects, technicians, nurses and physicians who contributed to the ascertainment of the various clinical samples used in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bennett, A., Sovio, U., Ruokonen, A. et al. No association between insulin gene variation and adult metabolic phenotypes in a large Finnish birth cohort. Diabetologia 48, 886–891 (2005). https://doi.org/10.1007/s00125-005-1737-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-005-1737-z