Abstract
Aims/hypothesis
Presentation of peptide epitopes derived from beta-cell autoantigens, such as insulin and its precursor molecules, by MHC class II molecules to autoreactive T-cells is believed to play a role in the development of Type 1 diabetes. However, little is known about the interaction between peptides of (prepro)insulin and MHC class II molecules permissive and protective for Type 1 diabetes. In this study therefore, peptides spanning the human preproinsulin sequence were assessed for their binding characteristics to Type 1 diabetes-protective and -permissive HLA molecules.
Methods
HLA-DR2, -DQ6.2 (Type 1 diabetes-protective) and HLA-DR4, -DQ8 (Type 1 diabetes permissive) molecule binding affinity for overlapping synthetic 20mer peptides spanning human preproinsulin was measured in a direct competition binding assay against a biotinylated indicator peptide.
Results
All HLA molecules tested showed similarity in their binding characteristics across the preproinsulin molecule, with regions of the insulin A-chain showing the highest affinity and C-peptide regions the lowest affinity for all HLA molecules tested. Furthermore, an insulin peptide implicated as a major CD4+ T-cell target in disease pathogenesis (B9-23) had high affinity binding to both protective and permissive HLA molecules but did not represent the highest affinity region of (prepro)insulin identified in either case.
Conclusion/interpretation
The results suggest that peptide binding affinity alone is unlikely to be the major determinant of disease susceptibility in relation to interactions between (prepro)insulin epitopes and HLA molecules. The identification of epitopes derived from beta-cell autoantigens that bind promiscuously to diabetes-permissive HLA molecules could be important in the design of peptide-based immunotherapeutic strategies for the prevention of Type 1 diabetes.
Similar content being viewed by others
The major contribution of genetic susceptibility to Type 1 diabetes mellitus (T1DM) is conferred by the major histocompatibility complex (MHC) gene cluster which accounts for approximately 45% of the inheritable diabetes risk in humans [1]. Disease susceptibility is strongly associated with the HLA-DRB1*04-DQB1*0302 and DRB1*0301-DQB1*0201 haplotypes and these alleles are found in the majority of Caucasian Type 1 diabetes patients [2]. Conversely, a dominant protective effect for Type 1 diabetes is conferred by the DRB1*1501-DQB1*0602 haplotype [3]. Given the fundamental role played by MHC molecules in thymic T-cell selection, as well as in peripheral T-cell regulation and activation, it seems likely that presentation of epitopes derived from pancreatic beta-cell autoantigens to autoreactive T-cells plays a pivotal role in Type 1 diabetes pathogenesis [4].
The mechanisms by which protective and permissive MHC molecules exert their effects on Type 1 diabetes remain unknown. Low affinity binding of autoantigenic peptide epitopes to permissive MHC molecules in the thymus has been suggested as a mechanism by which autoreactive T-cells escape negative selection [5]. Alternatively, protective MHC molecules could positively select a regulatory T-cell population [6]. An alternative, though not mutually exclusive hypothesis is that Type 1 diabetes-permissive MHC molecules bind certain diabetogenic epitopes of a beta-cell autoantigen with high affinity in the pancreas during the inflammatory disease process. The resulting long half-life of an MHC-diabetogenic peptide complex on the cell surface could promote efficient presentation to autoreactive T-cells. Such an epitope could constitute a pathogen-derived peptide, which activates T-cells cross-reactive with an autoantigenic epitope through molecular mimicry [7]. Finally it has been proposed that protective and permissive MHC class II molecules might compete for overlapping epitopes within an autoantigen [8, 9]. The affinity of epitopes for MHC molecules during antigen processing would dictate whether a "diabetogenic" or "non-diabetogenic" epitope is presented on the antigen presenting cell surface. One prediction from these models is that permissive and protective MHC molecules should vary measurably in their ability to bind disease-related peptide epitopes. However, few such epitopes have been identified with certainty in man. For this reason we have chosen to study the interaction of the whole preproinsulin molecule with the Type 1 diabetes-permissive HLA-DR4 (B1*0401) and HLA-DQ8 (A1*0301, B1*0302) molecules, and the Type 1 diabetes-protective HLA-DR2 (B1*1501) and HLA-DQ6.2 (A1*0102, B1*0602) molecules using a direct competition binding assay. Our studies were designed to identify regions of preproinsulin that differ in their binding characteristics to Type 1 diabetes-permissive and -protective HLA molecules.
Methods
Cell lines
As a source of HLA-DR4 (B1*0401) and HLA-DQ8 (A1*0301,B1*0302) molecules Preiss Epstein Barr virus (EBV)-transformed B cells, homozygous for these alleles, were used [10]. As a source of HLA-DR2 (B1*1501) and HLA-DQ6.2 (A1*0102, B1*0602) the homozygous PGF EBV B cell line was used. Cells were grown in RPMI 1640 (Life Technologies, Paisley, UK) supplemented with 10% heat-inactivated foetal calf serum (PAA Laboratories, Yeovil, UK), 1% penicillin/streptomycin (Life Technologies) at 37°C, 5% CO2. When cells reached a density of 1–2×106/ml they were pelleted and stored at −80°C.
Purification of HLA-DR and HLA-DQ molecules
HLA class II molecules were purified from cell pellets as described previously [11]. Briefly, cell pellets were homogenized in lyzing buffer and a crude membrane fraction solubilized in 4% NP-40 (Genaxis biotech, Saint-Cloud, France). Detergent solubilized membrane fractions were passed over a series of immunoaffinity columns with monoclonal antibodies specific for HLA-DR (clone L243) and HLA-DQ (clone SPVL3) coupled to protein A-Sepharose. MHC proteins were eluted with 50 mmol·l−1 glycine, pH 11.5, 0.1% sodium deoxycholate and immediately neutralized with 2 mol·l−1 glycine, pH 2 before being dialyzed against 10 mmol·l−1 Tris, pH 8 overnight. Dialyzed eluate was subsequently concentrated to 1 ml by ultrafiltration (Centricon 10; Millipore, Watford, UK) and purified on a gel-filtration column (7.8×300 mm Protein-Pak; Waters, Hemel Hempstead, UK). HLA-class II molecule purity and quantity was assessed by SDS-PAGE. All HLA-class II molecules were more than 98% pure.
Peptides
All synthetic peptides were purchased from Interactiva (Ulm, Germany). An overlapping 20mer peptide panel offset by eight amino acids spanning the human preproinsulin sequence was generated as well as an additional 15mer peptide spanning residues 9–23 of the insulin B-chain. For purposes of comparison with other studies on proinsulin binding to HLA-DR2 and -DR4 [12], we also obtained two additional synthetic peptides, insulin α-chain 1–17 (GIVEQCCTSICSLYQLE) and β-chain 16–30 (YLVCGERGFFYTPKT). Peptides were dissolved in 100% dimethyl sulfoxide (DMSO) and the peak associated with each peptide was quantified by area-under-curve analysis during RP-HPLC (absorbance at 210 nm, 2.1×150 mm Nova-Pak C18 column; Waters). All peptides showed over 70% purity by RP-HPLC and MALDI-TOF mass spectrometry. Peptides were stored at −20°C until use.
Peptide binding assays
Synthetic preproinsulin peptides were assessed for their ability to bind soluble HLA-class II molecules in vitro in a direct competition binding assay against a biotinylated indicator peptide. These indicator peptides comprised residues 98–117 of the MHC class II invariant chain peptide (PKPPKPVSKMRMATPLLMQA, for HLA-DR4 and -DQ6.2) [13], residues 430–444 of the HSV-2 transcriptional activator VP16 (EEVDMTPADALDDFD, for HLA-DQ8) [14] and residues 307–319 of influenza haemagglutinin (PKYVKQNTLKLAT, for HLA-DR2) [12]. We then incubated 12 µg of immunoaffinity-purified HLA class II protein with 2.5 µmol·l−1 biotinylated indicator peptide and test peptide or non-biotinylated indicator peptide at a range of concentrations (0.1–100 µmol·l−1) in a final DMSO concentration of 20% in 20 mmol·l−1 2-[N-morpholino]ethanesulfonic acid, 1% w/v n-octylglucoside, 140 mmol·l−1 sodium chloride, 0.05% sodium azide, pH 5, for 20 h at room temperature. Peptide mixtures were transferred to wells of a Maxisorp plate (Nalge Nunc, Hereford, UK) that had been pre-coated for 20 h at room temperature with 100 µl of either anti-HLA-DR (L243) or anti-HLA-DQ (SPVL3) capture antibody at 10 µg·ml−1 in phosphate buffered saline (PBS), blocked with 3% non-fat dried milk and 3% bovine serum albumin (BSA) for 30 min each and washed five times in Tris buffered saline (TBS)/0.1% Tween-20 (all chemicals from Sigma Chemical Co., Poole, Dorset, UK). Plates were incubated for a further 1 h at room temperature and washed five times in TBST. Europium-conjugated streptavidin (Perkin Elmer Ltd., Hounslow, UK) was added at 1 µg·ml−1 in dissociation-enhanced time-resolved fluoroimmunoassays (DELFIA) assay buffer (Wallac Oy, Turku, Finland) and incubated for 45 min at room temperature. Wells were washed a further five times in TBST and 100 µl Delfia enhancement solution added to each well. Fluorescent intensity was measured in a Delfia fluorimeter. Binding assays were carried out in triplicate and the entire peptide panel tested simultaneously on each separate occasion.
Whole protein HLA binding assay
Binding affinities of intact whole proinsulin (Eli Lilly, Hampshire, UK) and insulin (Novo Nordisk, Crawley, UK) molecules for HLA-DR2, HLA-DR4, HLA-DQ6.2 and HLA-DQ8 were tested in the same assay used to assess overlapping peptide binding affinities and at equivalent concentrations (0.1–100 µmol·l−1). For HLA-DQ8 bio-CLIP was used as an indicator peptide in the insulin and proinsulin binding assays.
Calculation of relative binding affinities of test peptides and proteins for HLA-class II molecules
The binding affinity of each test peptide was expressed as an inhibitory concentration 50 (IC50), calculated as the concentration of peptide required to inhibit binding of 2.5 µmol·l−1 biotinylated indicator peptide by 50%. IC50 values were calculated from standard curves in which peptide concentration was plotted against fluorescent units. Assays were carried out in triplcate and the binding affinity of each test peptide was expressed as the mean of triplicate IC50 values. IC50 variability between assays was minimal for all peptides tested.
Statistical analysis
The relationship between binding of different HLA molecules to preproinsulin peptides was analyzed by the Spearman rank correlation test. A p value of less than 0.5 was considered statistically significant.
Results
Preproinsulin peptide binding to diabetes-susceptible HLA-DR4 (B1*0401) and diabetes-protective HLA-DR2 (B1*1501) molecules
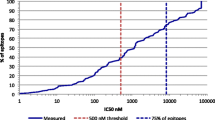
A 12-residue overlapping 20mer peptide panel spanning the entire human preproinsulin sequence, and an additional peptide representing residues 9–23 of the insulin B-chain were tested in triplicate for binding to soluble HLA-DR4 and HLA-DR2. For each peptide tested a binding curve was plotted and a peptide IC50 value extrapolated from this (Fig. 1).
Representative HLA-DR4 peptide binding curves of A: non-biotinylated indicator peptide and B: 20mer peptide consisting of residues 81–100 of preproinsulin. The concentration at which the test peptide curve crosses the horizontal dashed line representing 50% binding inhibition of 2.5 µmol·l−1 biotinylated indicator peptide is the test peptide IC50 value. A non-biotinylated indicator peptide IC50 value close to 2.5 µmol·l−1 indicates high assay accuracy (A)
Of the thirteen 20mer peptides tested, four inhibited binding of biotinylated indicator peptide to HLA-DR4 with an IC50 less than 1 µmol·l−1 and were classified as high affinity binders (Fig. 2A). A further four peptides had an IC50 value between 1 and 10 µmol·l−1 and were graded as having an intermediate HLA-DR4 binding affinity. Of the remaining five low affinity peptides, with an IC50 value greater than 10 µmol·l−1, four failed to inhibit indicator peptide binding by 50%, even when tested at 100 µmol·l−1, and therefore IC50 values could not be calculated. Higher affinity preproinsulin peptides tended to be located within the insulin A- and B-chains and the preproinsulin signal peptide whereas the majority of the lower affinity peptides were located within the proinsulin C-peptide and at the B-chain/C-peptide junction.
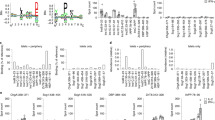
Binding of overlapping preproinsulin 20mer peptides to HLA-DR and -DQ molecules. Binding affinities are expressed as IC50 values i.e. the amount of overlapping preproinsulin peptide required to inhibit binding of 2.5 µmol·l−1 indicator peptide by 50%. IC50 values <1 µmol·l−1 classify peptides binding with high affinity. IC50 values >10 µmol·l−1 classify peptides binding with low affinity. IC50 values shown are means of triplicate assays. Error bars indicate standard deviation. Overlapping peptides are denoted by reference to the preproinsulin chain and residues covered (S= preproinsulin signal peptide). * indicates peptide binds with too low an affinity to ascertain an IC50 at the concentrations tested
Measurement of binding affinities of overlapping peptides for HLA-DR2 showed that 4 of the 13 overlapping peptides bound with an IC50 less than 1 µmol·l−1 and, as with HLA-DR4, these sequences were located within the insulin A- and B- chains and the preproinsulin signal peptide (Fig. 2B). Furthermore, the four peptides with the lowest affinity for HLA-DR2 spanned the proinsulin C-peptide.
Statistical analysis of the relationship between binding of overlapping peptides to HLA-DR4 and HLA-DR2 has shown the correlation to be significant (Fig. 3A; p<0.0001).
In order to make comparisons between our own results and those of others, we also obtained two additional synthetic peptides, insulin α-chain 1–17 and β-chain 16–30. Binding affinity of these peptides for HLA-DR molecules has been reported in a previous study. The α-chain peptide was previously reported as a moderate binder to both HLA-DR2 and -DR4 (IC50 14 µmol·l−1 and 4 µmol·l−1, respectively). In our hands, this peptide also bound similarly to DR2 and DR4 (IC50 0.8 µmol·l−1 and 1.1 µmol·l−1, respectively). The β-chain peptide was previously reported to bind well to HLA-DR2 and poorly to HLA-DR4 (6 µmol·l−1 and 100 µmol·l−1, respectively). In our assay, the β-chain 16–30 peptide also bound moderately to DR2 (5.4 µmol·l−1) and with low affinity to HLA-DR4 (>10 µmol·l−1).
To further validate the performance of our HLA-DR binding assay, we also explored the relationship between measured binding to HLA-DR4 and binding predicted by the SYPEITHI programme (http://syfpeithi.bmi-heidelberg.com/), a widely used database of HLA ligands and peptide motifs. There was a clear relationship between high and low predicted binding scores for DR4 and our IC50 values (Fig. 4).
Relationship between predicted binding to HLA-DR4 (solid line, square symbols) and measured binding to HLA-DR4 (broken line, triangle) of overlapping preproinsulin peptides. Prediction of binding was made using the SYFPEITHI programme. Axis showing log of IC50 is reversed to allow comparison with SYFPEITHI score. Score given for each overlapping peptide is equal to the highest score for a 9-mer core within each 20-mer peptide
Preproinsulin overlapping peptide binding to diabetes-susceptible HLA-DQ8 (A1*0301,B1*0302) and diabetes-protective HLA-DQ6.2 (A1*0102, B1*0602) molecules
The same preproinsulin overlapping 20mer peptide panel was tested for binding to soluble HLA-DQ6.2 and HLA-DQ8 molecules in vitro in direct competition binding assays (Fig. 2C, D). Binding of the overlapping peptide panel to HLA-DQ8 showed that seven peptides inhibited binding of biotinylated competitor peptide with an IC50 less than 1 µmol·l−1 and three peptides bound with an IC50 value greater than 10 µmol·l−1. The regions of preproinsulin with the highest affinity for HLA-DQ8 were located within the insulin A- and B-chains. Lowest affinity regions were confined to the proinsulin C-peptide.
Binding affinities to HLA-DQ6.2 with an IC50 value less than 1 µmol·l−1 were observed for 5 of the 13 overlapping peptides tested and a further five bound with an IC50 greater than 10 µmol·l−1. As with HLA-DQ8, the highest binding affinities were focused within the insulin A- and B- chains and the regions of preproinsulin with the lowest affinity for HLA-DQ6.2 were located within the proinsulin C-peptide. Statistical analysis showed the correlation between binding of preproinsulin peptides to HLA-DQ6.2 and HLA-DQ8 to be highly significant (Fig 3B; p<0.0001).
A strong similarity in the overlapping peptide panel binding pattern was shared by all HLA-class II molecules tested with the highest affinity peptides being located within the insulin A- and B-chains and those spanning the proinsulin C-peptide with the lowest affinities relative to all peptides tested.
Binding of insulin B-chain residues 9–23 to diabetes-susceptible and diabetes-protective HLA class II molecules
Due to the reported importance of residues 9–23 of the insulin B-chain as a target T-cell epitope in the pathogenesis of Type 1 diabetes in the nonobese diabetic mouse (NOD mouse) and in Type 1 diabetes in man, a synthetic peptide constituting these residues was assessed for binding to diabetes-susceptible and diabetes-protective soluble HLA-DR and DQ molecules(Fig. 2). The mean B9–23 IC50 values for HLA-DR4 and HLA-DR2 were 10 µmol·l−1 and 1.56 µmol·l−1, respectively. For both HLA-DR4 and HLA-DR2 therefore, this peptide bound with a moderate to low affinity relative to other preproinsulin peptides tested. The mean B9–23 IC50 values for HLA-DQ8 and HLA-DQ6.2 were 0.3 µmol·l−1 and 2.3 µmol·l−1, respectively. B9–23 did not contain the epitope of preproinsulin that binds with the highest affinity to HLA-DQ6.2 and similarly, although being amongst the peptides binding with high affinity to HLA-DQ8, residues B9–23 did not constitute the highest affinity region of the preproinsulin molecule.
Binding of whole insulin and proinsulin molecules to diabetes-susceptible and diabetes-protective HLA class II molecules
Whole intact proinsulin and insulin molecules were assessed for their ability to bind diabetes-susceptible and diabetes-protective soluble HLA-DR and HLA-DQ molecules in vitro (Fig. 5). Binding to HLA-DR molecules was weak. We observed detectable binding of proinsulin to HLA-DR4, but HLA-DR2 IC50 values could not be calculated for either insulin or proinsulin at the concentrations tested and therefore potential differences in HLA-DR2 binding affinity for these molecules could not be established. Binding of both whole proinsulin and insulin to HLA-DQ molecules was more readily detectable. For HLA-DQ6.2, binding to proinsulin and insulin was evident at similar levels of affinity. In contrast, HLA-DQ8 showed a much greater degree of binding to proinsulin than insulin, the difference in IC50 values being approximately 10-fold.
Binding of whole proinsulin (black bars) and insulin (white bars) to HLA-DR and-DQ molecules. IC50 values shown are the mean of triplicate assays. Error bars indicate standard deviation. * indicates that molecule bound with too low an affinity to ascertain an accurate IC50 value at the concentrations tested
Discussion
The aim of this study was to investigate whether Type 1 diabetes-permissive and -protective HLA class II molecules differ in their binding characteristics to the beta-cell autoantigen proinsulin, in order to gain a better understanding of disease-related functional differences between these molecules. The results show, however, a striking correlation between diabetes-permissive and diabetes-protective HLA class II molecules and the characteristics of their binding to regions of preproinsulin. Each of the HLA class II molecules examined had low affinity binding across the proinsulin C-peptide region and highest binding within the insulin A-chain relative to other peptides tested. In addition, each of the HLA class II molecules tested was able to bind the B9–23 region of the B-chain, proposed as an important epitope in human Type 1 diabetes and in the NOD mouse [15, 16]. Some differences in the binding characteristics of different HLA class II molecules were however detected. Notably, the HLA class II molecule most strongly associated with Type 1 diabetes, HLA-DQ8, has the greatest difference in its affinity for binding proinsulin and insulin, which could have relevance to the processing and presentation of autoantigenic epitopes to autoreactive T-cells.
Peptides bind HLA class II molecules via interactions between side chains of peptide anchor residues and specific pockets within the HLA peptide-binding groove [17]. The HLA binding groove is highly promiscuous and capable of accommodating a broad range of peptides, albeit at varying affinities. Residue requirements at defined anchor positions within the binding groove define the peptide-binding "motif" of a particular HLA allele and primary motifs for several Type 1 diabetes-protective and -permissive HLA class II molecules have been defined by a variety of experimental approaches [18, 19, 20, 21]. In light of these differing primary motifs HLA class II molecules might be expected to vary in their binding preferences to a panel of synthetic peptides. However, the existence of promiscuous peptides with the ability to bind multiple HLA molecules and with immunogenic potential has been reported [22, 23, 24]. Furthermore, peptides with promiscuous binding characteristics have been identified after sequencing of naturally processed peptides eluted from several HLA class II molecules, supporting the concept that degeneracy of peptide binding is a natural occurrence [18]. The ability of synthetic peptides within the insulin A- and B-chains and the preproinsulin signal peptide to bind all HLA class II molecules tested with relatively high affinity, compared to other peptides in the panel, is therefore consistent with previous studies.
Peptide promiscuity implies the existence of overlapping core binding motifs within these regions of preproinsulin. Alternatively, the promiscuous preproinsulin peptides identified in our study could bind different HLA molecules via the same binding frame, using conserved anchor residues, or could lack allele-restricted contact sites at the major anchor positions. Such "supermotifs" have been described extensively for HLA class I molecules [25] and for HLA-DR molecules [26]. As yet, evidence of supermotifs capable of binding both HLA-DR and HLA-DQ is more limited [27]. The identification of peptides from beta-cell autoantigens that encompass supermotifs might be beneficial in the design of peptide-based immunotherapies aiming to restore immune tolerance in the outbred population in which multiple different HLA-DR and HLA-DQ alleles will be expressed by any given individual at risk of Type 1 diabetes [28].
Autoreactive T-cell responses to residues B9-23 of the insulin B-chain are associated with the development of diabetes in the NOD mouse [15]. Recently, interferon-gamma producing B9-23 reactive T-cells have been detected in recent onset Type 1 diabetes patients and pre-diabetic individuals [16]. Previous reports have suggested that B9-23 peptide binds weakly to the NOD mouse HLA-DQ8 homologue I-Ag7 and that such complexes are unstable at the cell surface, with a fast off-rate [14, 29]. It has been proposed that as a consequence, there is a failure of clonal deletion of B9-23 reactive T-cells in the thymus of NOD mice, contributing to disease pathogenesis [5]. In contrast, the results of our binding assay show, consistent with previous reports [14] and the crystal structure of a HLA-DQ8/B9-23 peptide complex [30], that B9-23 peptide binds with high affinity to HLA-DQ8. However, other regions of preproinsulin also bound HLA-DQ8 with comparable or higher affinity. Further studies will be required to show which regions of this autoantigen are naturally processed and presented by this Type 1 diabetes permissive HLA class II molecule in vivo, as we [11] and others have shown that the relationship between binding affinity, processing and presentation is complex. However, our binding data suggest that naturally processed epitopes are unlikely to arise from the C-peptide region, which had low or undetectable binding to all HLA class II molecules tested and has also been shown by others to contain poorly binding sequences for several different HLA-DR molecules [12].
Our study shows that B9-23 peptide also binds with high affinity to both Type 1 diabetes protective and permissive HLA-DQ molecules. This finding raises the question as to whether HLA-DQ6.2 molecules could exert their dominant protective effect through determinant capture [8, 9]. It is proposed that in this process, binding of disease-related epitopes to a permissive HLA class II molecule is by a co-expressed, protective HLA class II molecule with higher affinity for the same region of the autoantigen. However, our binding assay is based on relative affinity of test peptide for a single HLA class II molecule, in competition with a selected indicator peptide. This precludes direct comparisons of binding affinities of individual peptides for different HLA class II molecules, and therefore other approaches will be required to examine this hypothesis.
Other investigators have examined binding of proinsulin peptides to HLA-DR and HLA-DQ molecules. One such study examined binding of overlapping peptides of proinsulin to a range of different HLA-DR molecules, and the concordance between their results and our own in relation to binding to HLA-DR2 and -DR4 molecules in the C-peptide region has been discussed above [12]. Concordance in other areas of the molecule is difficult to judge, since the overlapping peptide sets were different, but our analysis of two peptides from the aforementioned study, insulin α-chain 1–17 and β-chain 16–30, shows broadly similar results. Differences are likely to be attributable to differences in peptide sets and the use of different indicator peptides.
For binding of proinsulin peptides to HLA-DQ, in contrast, our study is the first to measure direct binding of test peptide to the HLA-DQ groove. A previous study to examine binding to HLA-DQ8 and HL-DQ6.2 [20] used a whole cell lysate assay, and found that B9-23 bound slightly better to HLA-DQ6.2 than to HLA-DQ8. However, the assay did not involve competitive displacement by test peptide of an indicator peptide and it remains uncertain, therefore, whether the binding detected is HLA peptide binding groove-specific. Others have examined differences in T-cell response to proinsulin peptides after immunization of HLA-DQ8 and -DQ6 transgenic mice [31]. However, the observed differences in recognition of different proinsulin peptides in that study were modest, and might reflect parameters other than peptide affinity, such as peptide solubility and TCR avidity.
The only difference between Type 1 diabetes-permissive and -protective HLA class II molecules that we could identify in this study was in their differences in binding affinity for intact proinsulin and insulin molecules. For HLA-DQ8 the IC50 value of proinsulin was almost a log-fold higher than that of insulin whereas HLA-DQ6.2 bound both molecules with a very similar affinity. The higher affinity of HLA-DQ8 for proinsulin over insulin suggests that HLA-DQ8 binds regions unique to proinsulin, i.e. within the C-peptide or at the C-peptide/A-chain and C-peptide/B-chain junctions. Since binding to peptides representing the C-peptide was generally poor, it is likely that exposed junctional regions have the capacity for direct binding to HLA-DQ8. The mechanism through which enhanced binding of proinsulin to HLA-DQ8 might influence Type 1 diabetes susceptibility is not clear. However, one speculation would be that such properties could enhance processing and presentation of proinsulin epitopes located within these regions of the molecule. The open ends of class II MHC molecules are well suited to capture of unfolded antigen domains, and it is thought that this could be essential to avoid excessive destruction of T-cell epitopes by over-digestion by processing enzymes [32]. Several studies have indicated that long processing products, up to 7 kDa, could be generated [33] strongly suggesting that interaction between MHC class II molecule and antigen can be an early event, preceding much of the proteolytic destruction of antigens. In this scenario, the ability of HLA-DQ8 to bind intact proinsulin would provide a greater opportunity for peptide presentation and might skew the peptides shown towards those in more "exposed" regions of the molecule. Further data on natural processing will be required to add to these observations.
Abbreviations
- MHC:
-
major histocompatibility complex
- HLA:
-
human leukocyte antigen
- EBV:
-
Epstein Barr virus
- IC50 :
-
inhibitory concentration 50
References
Buzzetti R, Quattrocchi CC, and Nistico L (1998) Dissecting the genetics of type 1 diabetes: relevance for familial clustering and differences in incidence. Diabetes Metab Rev 14:111–128
She JX (1996) Susceptibility to type I diabetes: HLA-DQ and DR revisited. Immunol Today 17:323–329
Thorsby E (1997). Invited anniversary review: HLA associated diseases. Hum Immunol 53:1–11
Kreuwel HT, Sherman LA (2001). The T-cell repertoire available for recognition of self-antigens. Curr Opin Immunol 13:639–643
Ridgway WM Fasso M Fathman CG (1999) A new look at MHC and autoimmune disease. Science 284:749–751
Luhder F, Katz J, Benoist C, Mathis D (1998) Major histocompatibility complex class II molecules can protect from diabetes by positively selecting T-cells with additional specificities. J Exp Med 187:379–387
Atkinson MA, BowmanMA, Campbell L, Darrow BL, Kaufman DL, Maclaren NK (1994) Cellular immunity to a determinant common to glutamate decarboxylase and coxsackie virus in insulin-dependent diabetes. J Clin Invest 94:2125–2129
Nepom GT (1990). A unified hypothesis for the complex genetics of HLA associations with IDDM. Diabetes 39:1153–1157
Deng H, Apple R, Clare-Salzler M, et al. (1993) Determinant capture as a possible mechanism of protection afforded by major histocompatibility complex class II molecules in autoimmune disease. J Exp Med 178:1675–1680
Gorga JC, Horejsi V, Johnson DR, Raghupathy R, Strominger JL (1987) Purification and characterization of class II histocompatibility antigens from a homozygous human B cell line. J Biol Chem 262:16087–16094
Peakman M, Stevens EJ, Lohmann T, et al. (1999) Naturally processed and presented epitopes of the islet cell autoantigen IA-2 eluted from HLA-DR4. J Clin Invest 104:1449–1457
Geluk A, Meijgaarden KE van, Schloot NC, Drijfhout JW, Ottenhoff TH, Roep BO (1998) HLA-DR binding analysis of peptides from islet antigens in IDDM. Diabetes 47:1594–1601
Chicz RM, Urban RG, Lane WS et al. (1992) Predominant naturally processed peptides bound to HLA-DR1 are derived from MHC-related molecules and are heterogeneous in size. Nature 358:764–768
Yu B, Gauthier L, Hausmann DH, Wucherpfennig KW (2000) Binding of conserved islet peptides by human and murine MHC class II molecules associated with susceptibility to type I diabetes. Eur J Immunol 30:2497–2506
Daniel D, Wegmann DR (1996) Protection of nonobese diabetic mice from diabetes by intranasal or subcutaneous administration of insulin peptide B-(9-23). Proc Natl Acad Sci USA 93:956–960
Alleva DG, Crowe PD, Jin L, et al. (2001) A disease-associated cellular immune response in type 1 diabetics to an immunodominant epitope of insulin. J Clin Invest 107:173–180
Germain RN (1994) MHC-dependent antigen processing and peptide presentation: providing ligands for T lymphocyte activation. Cell 76:287–299
Chicz RM, Urban RG, Gorga JC, Vignali DA, Lane WS, Strominger JL (1993) Specificity and promiscuity among naturally processed peptides bound to HLA-DR alleles. J Exp Med 178:27–47
Hammer J, Valsasnini P, Tolba K, et al. (1993) Promiscuous and allele-specific anchors in HLA-DR-binding peptides. Cell 74:197–203
Ettinger RA, Kwok WW (1998) A peptide binding motif for HLA-DQA1*0102/DQB1*0602, the class II MHC molecule associated with dominant protection in insulin-dependent diabetes mellitus. J Immunol 160:2365–2373
Godkin AJ, Davenport MP, Willis A, Jewell DP, Hill AV (1998) Use of complete eluted peptide sequence data from HLA-DR and -DQ molecules to predict T-cell epitopes, and the influence of the nonbinding terminal regions of ligands in epitope selection. J Immunol 161:850–858
Alexander J, Sidney J, Southwood S, et al. (1994) Development of high potency universal DR-restricted helper epitopes by modification of high affinity DR-blocking peptides. Immunity 1:751–761
O'Sullivan D, Arrhenius T, Sidney J, et al. (1991) On the interaction of promiscuous antigenic peptides with different DR alleles. Identification of common structural motifs. J Immunol 147:2663–2669
Sette A, Sidney J, Oseroff C, del Guercio MF, Southwood S, Arrhenius T, Powell MF, Colon SM, Gaeta FC, Grey HM (1993) HLA DR4w4-binding motifs illustrate the biochemical basis of degeneracy and specificity in peptide-DR interactions. J Immunol 151:3163–3170
Sette A, Sidney J (1998) HLA supertypes and supermotifs: a functional perspective on HLA polymorphism. Curr Opin Immunol 10:478–482
Southwood S, Sidney J, Kondo A, et al. (1998) Several common HLA-DR types share largely overlapping peptide binding repertoires. J Immunol 160:3363–3373
Raddrizzani L, Sturniolo T, Guenot J, et al. (1997) Different modes of peptide interaction enable HLA-DQ and HLA-DR molecules to bind diverse peptide repertoires. J Immunol 159:703–711
Peakman M, Dayan CM (2001) Antigen-specific immunotherapy for autoimmune disease: fighting fire with fire? Immunology 104:361–366
Carrasco-Marin E, Shimizu J, Kanagawa O, Unanue ER (1996) The class II MHC I-Ag7 molecules from non-obese diabetic mice are poor peptide binders. J Immunol 156:450–458
Lee KH, Wucherpfennig KW, Wiley DC (2001) Structure of a human insulin peptide-HLA-DQ8 complex and susceptibility to type 1 diabetes. Nat Immunol 2:501–507
Raju R, Munn SR, David CS (1997) T-cell recognition of human pre-proinsulin peptides depends on the polymorphism at HLA DQ locus: a study using HLA DQ8 and DQ6 transgenic mice. Hum Immunol 58:21–29
Watts C (2001) Antigen processing in the endocytic compartment. Curr Opin Immunol 13:26–31
Castellino F, Zappacosta F, Coligan JE, Germain RN (1998) Large protein fragments as substrates for endocytic antigen capture by MHC class II molecules. J Immunol 161:4048–4057
Acknowledgements
This work was supported by Diabetes UK and the Joint Research Committee (JRC) of King's College Hospital. M.Peakman is a Diabetes UK Senior Clinical Research Fellow. T.P. Astill received a JRC studentship.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Astill, T.P., Ellis, R.J., Arif, S. et al. Promiscuous binding of proinsulin peptides to Type 1 diabetes-permissive and -protective HLA class II molecules. Diabetologia 46, 496–503 (2003). https://doi.org/10.1007/s00125-003-1070-3
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-003-1070-3