Abstract
Objective
To evaluate the role of palliative stereotactic body radiation therapy (SBRT) in Barcelona Clinic Liver Cancer stage‑C (BCLC-C) hepatocellular carcinoma (HCC) patients who are not suitable for other loco-regional therapies.
Materials and methods
It is an observational retrospective study done between May 2020 and September 2021. The data were collected from 35 patients of advanced HCC who underwent SBRT. Patients of Child Pugh status (CPs) A5-B7 and with a liver reserve of ≥ 700cc were included. Local control (LC), overall survival (OS) and adverse events including decompensation were carefully recorded.
Results
In the cohort, Portal vein and IVC tumor thrombosis were present in 33 (94.3%) and 8 (22.85%) patients, respectively. Lung and nodal metastasis were found in 11 (31.4%) and 21 (60%) of patients, respectively. The median gross tumor volume (GTV) was 563cc (range 80–1925cc). The median SBRT dose prescription was 35 Gy (range 25–40 Gy) in 5–10 fractions. Post radiation therapy, there was improvement in pain and discomfort in 24 out of 29 (82.75%) and 18 out of 23 (78%) patients respectively. Also bone metastasis related pain was improved in all 3 (100%) patients.
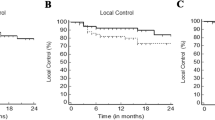
One year LC, and OS were 80% and 30% respectively. On multivariate analysis, the GTV volume > 750cc and PIVKA-II > 8000 mAU/ml remained the predictor factor for poor OS. Post SBRT, change in child-pugh score by 1 point was observed in 7 patients (20%) which was managed conservatively.
Conclusion
SBRT is a safe and feasible option for BCLC‑C HCC. It not only improves the quality of life by symptom control but also results in good LC and OS with acceptable toxicity. SBRT should be considered in a multidisciplinary fashion for patients presenting with advanced HCCs.



Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71(3):209–249. https://doi.org/10.3322/caac.21660
Kudo M, Izumi N, Kubo S, Kokudo N, Sakamoto M, Shiina S et al (2020) Report of the 20th Nationwide follow-up survey of primary liver cancer in Japan. Hepatol Res 50:15–46
Cheng S, Yang J, Shen F, Zhou W, Wang Y, Cong W et al (2016) Multidisciplinary management of hepatocellular carcinoma with portal vein tumor thrombus—Eastern Hepatobiliary Surgical Hospital consensus statement. Oncotarget 7(26):40816–40829. https://doi.org/10.18632/oncotarget.8386
Que J, Wu HC, Lin CH, Huang CI, Li LC, Ho CH (2020) Comparison of stereotactic body radiation therapy with and without sorafenib as treatment for hepatocellular carcinoma with portal vein tumor thrombosis. Medicine (Baltimore) 99(13):e19660. https://doi.org/10.1097/MD.0000000000019660
Pérez-Romasanta LA, González-Del Portillo E, Rodríguez-Gutiérrez A, Matías-Pérez Á (2021) Stereotactic radiotherapy for hepatocellular carcinoma, radiosensitization strategies and radiation-immunotherapy combination. Cancers (Basel) 13(2):192. https://doi.org/10.3390/cancers13020192
Su TS, Lu HZ, Cheng T, Zhou Y, Huang Y, Gao YC et al (2016) Long-term survival analysis in combined transarterial embolization and stereotactic body radiation therapy versus stereotactic body radiation monotherapy for unresectable hepatocellular carcinoma >5 cm. BMC Cancer 16(1):834. https://doi.org/10.1186/s12885-016-2894-9
Shui Y, Yu W, Ren X, Guo Y, Xu J, Ma T, Zhang B, Wu J, Li Q, Hu Q, Shen L, Bai X, Liang T, Wei Q (2018) Stereotactic body radiotherapy based treatment for hepatocellular carcinoma with extensive portal vein tumor thrombosis. Radiat Oncol 13(1):188. https://doi.org/10.1186/s13014-018-1136-5
Choi CKK, Ho CHM, Wong MYP, Leung RWK, Wong FCS, Tung SY et al (2021) Long-term results of palliative stereotactic radiotherapy of barcelona clinic liver cancer stage C hepatitis B–related hepatocellular carcinoma. Hong Kong J Radiol 24:81–86
Dawson LA, Zhu A, Knox J et al (2012) Radiation therapy oncology group Rtog 1112 randomized phase iii study of sorafenib versus stereotactic body radiation therapy followed by sorafenib in hepatocellular carcinoma
Cancer Institute N (2017) Common Terminology Criteria for Adverse Events (CTCAE) v5.0. https://www.meddra.org/. Accessed 4 Nov 2018
Lencioni R, Llovet JM (2010) Modified RECIST (mRECIST) assessment for hepatocellular carcinoma. Semin Liver Dis 30(1):52–60. https://doi.org/10.1055/s-0030-1247132
Reig M, Forner A, Rimola J, Ferrer-Fàbrega J, Burrel M, Garcia-Criado Á et al (2021) BCLC strategy for prognosis prediction and treatment recommendation: The 2022 update. J Hepatol. https://doi.org/10.1016/j.jhep.2021.11.018
Apisarnthanarax S, Barry A, Cao M, Czito B, DeMatteo R, Drinane M et al (2022) External beam radiation therapy for primary liver cancers: an ASTRO clinical practice guideline. Pract Radiat Oncol 12(1):28–51. https://doi.org/10.1016/j.prro.2021.09.004
El-Serag HB, Rudolph KL (2007) Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology 132:2557–2576
Patidar Y, Garg L, Mukund A, Sarin SK (2019) Early experience of combination therapy of transarterial chemoembolization and radiofrequency ablation for hepatocellular carcinoma measuring 3–7 cm. Indian J Radiol Imaging 29(1):47–52. https://doi.org/10.4103/ijri.IJRI_352_18
Chopra S, George K, Engineer R, Rajamanickam K, Nojin S, Joshi K et al (2019) Stereotactic body radio therapy for inoperable large hepatocellular cancers: results from a clinical audit. Br J Radiol 92(1101):20181053. https://doi.org/10.1259/bjr.20181053
Yeoh KW, Prawir A, Bin Saad MZ, Lee KM, Lee EMH, Low GK et al (2020) Vinorelbine augments radiotherapy in hepatocellular carcinoma. Cancers 12:872
Bujold A, Massey CA, Kim JJ, Brierley J, Cho C, Wong RK et al (2013) Sequential phase I and II trials of stereotactic body radiotherapy for locally advanced hepatocellular carcinoma. J Clin Oncol 31:1631–1639
Ohri N, Tome WA, Mendez Romero A, Miften M, Ten Haken RK, Dawson LA et al (2021) Local control after stereotactic body radiation therapy for liver tumors. Int J Radiat Oncol Biol Phys 110(1):188–195. https://doi.org/10.1016/j.ijrobp.2017.12.288
Gkika E, Schultheiss M, Bettinger D, Maruschke L, Neeff HP, Schulenburg M et al (2017) Excellent local control and tolerance profile after stereotactic body radiotherapy of advanced hepatocellular carcinoma. Radiat Oncol. https://doi.org/10.1186/s13014-017-0851-7
Hammad AY, Robbins JR, Turaga KK, Christians KK, Gamblin TC, Johnston FM (2017) Palliative interventions for hepatocellular carcinoma patients: analysis of the National Cancer Database. Ann Palliat Med 6(1):26–35. https://doi.org/10.21037/apm.2016.11.02
Hawkins MA, Dawson LA (2006) Radiation therapy for hepatocellular carcinoma: from palliation to cure. Cancer 106:1653–1663
Yamashita H, Onishi H, Murakami N, Matsumoto Y, Matsuo Y, Nomiya T, Nakagawa K (2015) Japanese Radiological Society multi-institutional SBRT study group (JRS-SBRTSG). Survival outcomes after stereotactic body radiotherapy for 79 Japanese patients with hepatocellular carcinoma. J Radiat Res 56(3):561–567. https://doi.org/10.1093/jrr/rru130
Kuo H‑T, Que J, Lin L‑C, Yang C‑C, Koay L‑B, Lin C‑H (2017) Impact of tumor size on outcome after stereotactic body radiation therapy for inoperable hepatocellular carcinoma. Medicine 96:e9249. https://doi.org/10.1097/MD.0000000000009249
Klement RJ, Abbasi-Senger N, Adebahr S, Alheid H, Allgaeuer M, Becker G et al (2019) The impact of local control on overall survival after stereotactic body radiotherapy for liver and lung metastases from colorectal cancer: a combined analysis of 388 patients with 500 metastases. BMC Cancer 19(1):173. https://doi.org/10.1186/s12885-019-5362-5
Cheng AL, Kang YK, Chen Z, Tsao CJ, Qin S, Kim JS et al (2009) Efficacy and safety of sorafenib in patients in the Asia-Pacific region with advanced hepatocellular carcinoma: a phase III randomised, double-blind, placebo-controlled trial. Lancet Oncol 10(1):25–34. https://doi.org/10.1016/S1470-2045(08)70285-7
Nandennavar MI, Karpurmath SV, Mandakalatur G, Prasad AE (2017) Clinical profile of hepatocellular carcinoma and experience with sorafenib from a tertiary cancer centre in Southern India. Int J Res Med Sci 5:379–383
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
D. Sharma, D. Thaper, R. Kamal and H.P. Yadav declare that they have no competing interests.
Additional information
Data Availability Statement
Research data are stored in an institutional repository and will be shared upon request to the corresponding author.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sharma, D., Thaper, D., Kamal, R. et al. Role of palliative SBRT in barcelona clinic liver cancer-stage C hepatocellular carcinoma patients. Strahlenther Onkol 199, 838–846 (2023). https://doi.org/10.1007/s00066-023-02065-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-023-02065-x