Abstract
Purpose
The new Medical Licensing Regulations 2025 (Ärztliche Approbationsordnung, ÄApprO) require the development of competence-oriented teaching formats. In addition, there is a great need for high-quality teaching in the field of radiation oncology, which manifests itself already during medical school. For this reason, we developed a simulation-based, hands-on medical education format to teach competency in performing accelerated partial breast irradiation (APBI) with interstitial multicatheter brachytherapy for early breast cancer. In addition, we designed realistic breast models suitable for teaching both palpation of the female breast and implantation of brachytherapy catheters.
Methods
From June 2021 to July 2022, 70 medical students took part in the hands-on brachytherapy workshop. After a propaedeutic introduction, the participants simulated the implantation of single-lead catheters under supervision using the silicone-based breast models. Correct catheter placement was subsequently assessed by CT scans. Participants rated their skills before and after the workshop on a six-point Likert scale in a standardized questionnaire.
Results
Participants significantly improved their knowledge-based and practical skills on APBI in all items as assessed by a standardized questionnaire (mean sum score 42.4 before and 16.0 after the course, p < 0.001). The majority of respondents fully agreed that the workshop increased their interest in brachytherapy (mean 1.15, standard deviation [SD] 0.40 on the six-point Likert scale). The silicone-based breast model was found to be suitable for achieving the previously defined learning objectives (1.19, SD 0.47). The learning atmosphere and didactic quality were rated particularly well (mean 1.07, SD 0.26 and 1.13, SD 0.3 on the six-point Likert scale).
Conclusion
The simulation-based medical education course for multicatheter brachytherapy can improve self-assessed technical competence. Residency programs should provide resources for this essential component of radiation oncology. This course is exemplary for the development of innovative practical and competence-based teaching formats to meet the current reforms in medical education.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The further development of medical studies within the framework of the new Medical Licensing Regulations 2025 includes an orientation from fact-based to competence-based learning and focuses on practical, longitudinal, and interdisciplinary training [1]. The specialty of radiation oncology and radiation therapy, as an integral part of therapeutic oncology, represents an interdisciplinary interface and should be adequately addressed in medical education because of its public health importance [2, 3]. Consequently, there is a great need for high-quality teaching and training in radiation oncology to continue during medical school as well as during residency training [4,5,6,7,8].
In this regard, structured training in brachytherapy techniques is particularly suited to teach practical radiation oncology skills. To date, such courses are rarely offered, although they provide graduates with more confidence and experience in the use of the method [9].
For example, training workshops using a phantom-based simulator have been established for brachytherapy of prostate cancer [10]. In addition to teaching ultrasound-guided treatment planning and implantation techniques, the CT simulation images allow subsequent calculation of the resulting spatial dose distribution, thus providing participants with direct feedback on the quality of catheter positioning [11, 12].
For multicatheter brachytherapy in breast cancer, there are no published results of simulation-based workshops in medical education. Therefore, the aim of the present work was to develop a feasible model for teaching and training practical skills in multicatheter brachytherapy of the breast.
Accelerated partial breast irradiation (APBI) using multicatheter interstitial brachytherapy is a highly effective treatment option for early breast cancer [13,14,15]. The treatment is characterized by precise delivery of a high dose to the target volume while minimizing the dose to organs at risk [16]. However, despite the advantages of this technique, many authors report a decline in brachytherapy due in part to lack of time and inadequate education and training [17].
Materials and methods
We have (1) developed a new breast model that enables the acquisition of practical skills in multicatheter brachytherapy of the breast and (2) evaluated its feasibility in an education workshop teaching and training students in brachytherapy techniques.
Breast model
For the simulation workshop, a silicone breast model consisting of a soft inner core and an outer skin was used. Therefore, silicone basis component and catalyzation component (SF00-RTV2 Silicone [silicone rubber], SILIKONFABRIK.DE) were mixed in a ratio of 1:1, then silicone oil (SF-V50, SILIKONFABRIK.DE) and Alginat (Protesil ®, ISO 21563) were added. Finally, a color paste (European‑3, FPHE3; Silikonfabrik.de, Ahrensburg, Deutschland) was used to give the model an authentic skin-colored tone. To ensure the soft texture of the inner core, salt and semolina were added to the mixture. The prepared inner core mixture was cast in a ceramic mold with a wire-fixed Styrodur® sphere of approximately 2 cm in diameter, which was supposed to simulate the tumor bed (Fig. 1). After the silicone had cured, the inner core was transferred to a breast-shaped plaster mold treated with silicone removal agent by keeping a gap of 1.5 cm between the inner core and mold, which was filled with the silicone mixture for the outer skin. After a second curing period, the whole breast could be gently removed from the mold.
The breast model was evaluated by experienced radiation oncologists (MM, SD, SK) for its condition, safety, and suitability for training purposes prior to use.
Applicators
For the teaching course, we used stainless steel needles, 350 mm blind-ended flexible implant tubes, and fixation buttons, which were all sponsored for this workshop by the manufacturer (Varian, Palo Alto, CA, USA).
CT imaging of the breast cancer model
Imaging of the newly developed breast cancer model using CT scan visualized simulation of the hypointense tumor bed, normal breast tissue, skin, and subcutaneous adipose tissue (Fig. 1).
Design and learning objectives
The training course was aimed at medical students in advanced clinical training (6th–10th semesters) at the beginning of their training. The event was conducted in each case by two radiation oncologists and a student assistant.
We defined the following learning objectives for our hands-on workshop: trainees should be enabled to
-
correctly perform the clinical examination of the female breast, localize the tumor bed, and describe clinical findings in technical terms;
-
describe the principles of brachytherapy and its areas of application in breast cancer in consideration of alternative radiation techniques;
-
perform correctly the implantation of single-leader catheters in predefined positions for breast brachytherapy;
-
assess the accuracy of the catheter position a) relative to the tumor bed and b) relative to each other;
-
describe the target volume for breast cancer brachytherapy; and
-
evaluate the actual implanted catheter position in terms of the resulting dose distribution.
Workflow of the training course
Before the start of the course, participants were asked to fill out a questionnaire intended to assess their knowledge level (Table 1). The course was divided into a 30-minute propaedeutic introduction, including a definition of the learning objectives, and the 60-minute practical part, which consisted of three hands-on stations (Figs. 2 and 3). After the course, the participants were asked again to answer the questionnaire to track their knowledge progress, including a course evaluation.
Training course on breast cancer brachytherapy using the newly developed breast cancer model. Following an introductory lecture (a), residents and participants trained the implantation of single-lead catheters into the silicone breast model (b). CT scan evaluated the accuracy of applicator placement and CT-based contouring and treatment planning was demonstrated and trained (c, d)
The propaedeutic part included a lecture on the most important aspects relevant to the curriculum regarding diagnostics and standard guideline-guided therapy of early breast cancer, with a focus on the clinical evidence-based benefit of different radiotherapy techniques after breast-conserving therapy.
The indication for brachytherapy was then presented and the patient population eligible for multicatheter brachytherapy for breast carcinoma was characterized. Partial breast irradiation was then compared with percutaneous irradiation in terms of its advantages and disadvantages. The theoretical part was concluded with a clinical case report.
At the first station of the practical part, a clinical examination of the female breast was first demonstrated to the participants using a silicone breast model, which was then performed by the students under supervision.
Step-by-step catheter implantation was then demonstrated by the instructors. Participants were then requested to work in teams of two to implant three to four introducer catheters homogeneously into the tumor bed of the model simulated by a Styrodur® sphere. The models differed with respect to the sphere, requiring thorough prior palpation for localization. Additionally, CT images of the scanned breast models were presented to each team. After each team had implanted 3–4 applicators under constant supervision, all breast models were CT scanned at the second station of the workshop.
Here, participants were able to assess the accuracy of their applicator placement. In addition, postoperative processing, including catheter shortening and reconstruction in the Radiation Therapy Planning System (Eclipse©, Varian, Palo Alto, CA), of single-lead catheters was demonstrated by a medical physics expert.
At the third station, a representative CT-based contouring and treatment plan was explained and adapted live by a medical physicist. The specifics of 3D radiation planning and treatment flow in clinical practice were discussed. Together with the students, the irradiation plan was optimized. In particular, effects of a suboptimal catheter position on dosimetry and radiation therapy planning (under- and overdosing) were discussed.
At the end of the workshop, the reported clinical patient case was revisited and take-home messages were summarized. After the workshop, participants completed the questionnaire again. Finally, all participants received a handout with the key facts conveyed to consolidate the acquired knowledge at home.
Evaluation of the training workshop
Before and after the workshop, participants were asked to rate their skills and knowledge on APBI using a questionnaire on a six-point Likert scale (1—completely agree, 2—mostly agree, 3—tend to agree, 4—tend to disagree, 5—mostly disagree, 6—disagree completely). In addition, participants were required to complete a questionnaire after the course to evaluate the entire workshop. Optionally, there were two free questions, “What did you like best?” and “What could be improved?” Participation was anonymous.
Statistics
Statistics were performed by using IBM SPSS Statistics version 26 (IBM Deutschland GmbH, Ehningen, Germany). Only completely fulfilled surveys were included in the statistical analysis. We hypothesized that the workshop enables participants to enhance their knowledge-based competencies on brachytherapy. The participants assessed their skills on a six-point-Likert scale in a questionnaire consisting of nine items. In a descriptive analysis, mean values and standard error (SEM) for each item were compared before and after the workshop (Table 1). To test our hypothesis, sum scores of all items were calculated. A non-parametric statistical hypothesis test was performed by a paired t-test. A significance level below p = 0.05 was considered as significant.
Results
The brachytherapy breast cancer model
The newly developed breast cancer model was rated as realistic by the seniors involved in the publication with many years of experience in brachytherapy of breast cancer.
Trainees described the brachytherapy breast cancer model as suitable for achieving the previously defined learning objectives (1.16, standard deviation [SD] 0.41 on the six-point Likert scale) and successfully learned practical skills of implanting single-leader catheters into the breast model (5.8 to 1.9). The majority of respondents fully agreed that the workshop increased their interest in brachytherapy (1.15, SD 0.40). Moreover, they were able to describe the contouring principles of the target volume, the treatment planning process, and radiation fractionation schemes (4.9 to 2.1).
Workshop
Between June 2021 and July 2022, a total of 70 trainees participated in 11 sessions of 90 min each. 62 questionnaires were completed in full.
For all learning objectives, participants indicated that their theoretical and practical skills improved significantly as a result of the course (see Likert confidence scores, Table 1). Participants were able to improve their knowledge-based skills about aspects essential for radiation planning, the pre-radiotherapy process (4.0 at 1.8), and treatment (4.8 at 2.0) of early-stage breast cancer. They were able to expand their knowledge about different application fields of brachytherapy in general (4.0 to 1.6). The workshop raised the awareness of which patients could benefit from partial breast irradiation (5.0 to 1.8). Furthermore, the workshop enabled participants to provide patients with information about the treatment procedure (4.6 to 1.6) as well as the advantages and disadvantages in comparison to external beam irradiation techniques (4.5 to 1.7).
For statistical analysis of the described learning progress, we calculated sum scores based on the Likert confidence scores for all nine survey statements. Before the workshop, the mean sum score was 42.4, which corresponds to an average value of 4.7 on the Likert confidence score. After the workshop, the mean sum score was enhanced to 16.0, corresponding to a value of 1.8 on average. The participants underwent a striking learning process by attending this workshop and were able to improve their knowledge-based competencies on brachytherapy for breast cancer significantly (p < 0.001, tested by paired t-test).
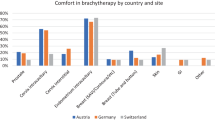
The training workshops were predominantly positive (Fig. 4). The breast model was described as suitable to achieve the previously defined learning objectives (1.16, SD 0.41).
According to the free-text answers, the participants appreciated the practical hands-on session, the well-structured workflow within the real clinical facilities, the appreciative supervision by the lecturer, the color-printed handout, the link between the propaedeutic and practical parts, and the learning and working atmosphere in general.
In the first seminars, the sluggishness of the catheter application due to the high resistance of the model was criticized several times. After optimizing the composition of the breast model, this point of criticism did not reoccur.
Discussion
This workshop is the first simulation-based hands-on workshop on interstitial multicatheter brachytherapy for breast cancer described in the literature. The simulation of catheter placement on the breast model enabled participants to achieve the predefined learning objectives. According to the self-assessment, participants benefited significantly from an increase in their competency-based knowledge measurable using the six-point Likert scale. Furthermore, the students appreciated the practical hands-on elements, their close integration with the theoretical content, and the insight into real clinical facilities.
The workshop follows a competency-based and interdisciplinary teaching approach. Thus, it is significantly oriented towards the current reform efforts of medical teaching in Germany, which are expressed in the Masterplan Medizinstudium 2020 and in the revision of the National Competence-Based Catalogue of Learning Objectives in Medicine (NKLM). Here, the demand for a consistent practice and competence orientation of teaching with a special focus on an understanding of effective interdisciplinary collaboration between different professions in health care is found. By synthesizing individual learning objectives, more practice-related competencies are to be taught. The acquisition of competencies not only includes pure knowledge aspects, but also requires additional manual and communicative skills in the application of the acquired knowledge. Lectures such as the brachytherapy workshop are particularly suitable for linking cognitive, psychomotor, and affective learning objectives [18,19,20]. These proclaimed educational principles afford a high potential for developing innovative teaching formats especially in radiation oncology, due to its multiprofessional and interdisciplinary nature [1, 7, 21].
The multiprofessional design of the workshop will provide participants with a profound understanding about brachytherapeutic work and treatment processes as well as interdisciplinary collaboration in radiation oncology. A profound understanding of multiprofessional cooperation in radiation oncology care is instrumental for improved patient outcome and should therefore be further promoted through multiprofessionally designed teaching opportunities [22].
Simulation-based training, based on active learning theories in cognitive and learning sciences, is increasingly demanded for modern medical teaching across disciplines [23]. According to Dale’s Cone of Experiences, active learning processes are significantly more effective than passive ones and allow learners to remember up to 90% of what they learn [24]. Complex cognitive processes result from the interaction between declarative and procedural knowledge. The acquisition of high-quality professional competencies therefore requires the essential integration of practical components into teaching. Especially for medical education, it has been shown that simulation-based teaching concepts are superior to purely theoretical lessons [25, 26]. The positive effects were not only shown with regard to the acquisition of technical knowledge and practical skills, but were even associated with an improvement in patient care, which should be seen as a groundbreaking advantage in view of the intention of medical teaching [27,28,29,30,31]. Furthermore, it has already been demonstrated that simulation-based training achieves particularly sustainable and long-term learning effects [23, 32].
Our results are congruent with observations from other simulation-based workshops on brachytherapy for prostate and gynecologic cancer. Here, it was consistently shown that simulation-based brachytherapy training led to increased confidence in using the method [9, 11, 12]. Despite its advantages, the clinical use of brachytherapy has been declining for years [17]. Conducting such hands-on teaching sessions for residents could be an approach to strengthen the awareness and entrenchment of brachytherapy in radiation oncology.
Recently, it has been reported that there is a great demand for more practical lessons in the training of radiation oncology professionals [33]. While it has been demonstrated that simulation-based education has a high benefit in radiation oncology, it mainly addresses the teaching of contouring. Hence, there is a big gap to fill regarding other specific competencies such like communication or technical skills [34]. Educational training methods like the workshop are a promising approach to meet these needs.
Despite the didactic advantages, only few simulation-based teaching concepts have been established in radiation oncology so far, which is possibly also related to the required personnel, time, and financial burdens. In addition, techniques such as multicatheter brachytherapy of breast carcinoma are not even available at all university centers.
The participants of our workshop particularly appreciated the integration of our workshop into the real clinical setting with participation of the professional groups involved in everyday treatment. They reported being able to better estimate the complexity of the radiotherapeutic treatment chain, with the consequences to be derived from the various treatment steps. From the perspective of cognitive science, the situational learning theory is applied here, according to which learning is understood as a context-dependent process. The content and meaning of what is learned is largely dependent on the environment in which it is taught. Therefore, it is advisable to integrate technical courses into the real-life professional environment [23, 35, 36].
Learning about the various radiotherapeutic procedures, especially interventional techniques such as brachytherapy, could stimulate interest in the entire field of radiation oncology [6, 8]. Although not explicitly recorded in the evaluation form, the majority of students indicated that the workshop increased their interest in the topic.
In addition to the positive results of the workshop described here, some limitations also become apparent. The monocentric nature of this study limits its validity. This is especially true for the questionnaire, which was developed specifically for the study and thus does not represent an established, standardized measurement instrument. Similarly, the number of study participants forms only a small sample size. Furthermore, not all participants completed the questionnaire in full. The voluntary workshop participation of the medical students results in a selection bias, as it is possible that primarily students interested in radiation oncology attended the workshop, which limits a transfer of the results to the general public of medical students. To assess the achievement of the predefined learning objectives, an exam (e.g., as a lightning round or elevator pitch) could be conducted at the end of the event. Likewise, no statement can be made about the long-term learning effect achieved. Further follow-up studies would be necessary for this.
The comparability of the breast model, including the Styrofoam ball as a tumor bed, with a real breast is limited. The consistency of the material was found to be stiffer compared to real breast tissue. A clinical examination of the breast can only be reproduced to a limited extent with the aid of the model, but this was also not the leading intention of this course.
The demand for practice-oriented teaching formats to impart manual skills is countered by the development of an increasing number of digital teaching formats, partly driven by the coronavirus pandemic [37]. While certain elements of the workshop can only be conducted in classroom teaching under supervision (e.g., catheter implantation), some parts are also feasible in digital format. A further development of the course could be the integration of digital technologies as a hybrid format [2]. It would be conceivable to establish a flipped classroom format as preparation for the workshop with the aid of digital teaching materials [38].
The multiprofessional, competence- and practice-based approach of the hands-on workshop is significantly oriented towards the reform movements in the German medical curriculum and could be exemplary for future teaching concepts in radiation oncology.
Conclusion
The simulation-based medical education course for multicatheter brachytherapy can improve self-assessed technical competence and increase enthusiasm for brachytherapy. Residency programs should provide resources for this essential component of radiation oncology. This course is exemplary for the development of innovative practical and competence-based teaching formats to meet the current reforms of medical education in Germany.
References
Dapper H et al (2022) Integration of radiation oncology teaching in medical studies by German medical faculties due to the new licensing regulations : an overview and recommendations of the consortium academic radiation oncology of the German society for radiation oncology (DEGRO). Strahlenther Onkol 198(1):1–11
Vorwerk H, Engenhart-Cabillic R (2022) Students’ learning behavior in digital education for radiation oncology. Strahlenther Onkol 198(1):12–24
Mäurer MA, Mäurer I, Kamp MA (2022) Can neuro-oncology teaching contribute to educate medical doctors better? A reflection on the value of neuro-oncology for student teaching. Chin Neurosurg J 8(1):23
Zaorsky NG et al (2016) What are medical students in the United States learning about radiation oncology? Results of a multi-institutional survey. Int J Radiat Oncol Biol Phys. https://doi.org/10.1016/j.ijrobp.2015.10.008
Mäurer MA et al (2022) Erstmalige interdisziplinäre DKK-Programmplanung durch Zusammenschluss onkologischer Nachwuchsgruppen. Forum 37(1):19–23
Sandhu N et al (2020) Virtual radiation oncology clerkship during the COVID-19 pandemic and beyond. Int J Radiat Oncol Biol Phys 108(2):444–451
Linde P et al (2022) Teaching in radiation oncology: now and 2025—results of a focus group with medical students. Strahlenther Onkol. https://doi.org/10.1007/s00066-022-01997-0
Oertel M et al (2020) Quality of teaching radiation oncology in Germany-where do we stand? : results from a 2019 survey performed by the working group “young DEGRO” of the German society of radiation oncology. Strahlenther Onkol 196(8):699–704
Singer L et al (2019) Development and implementation of a simulation-based educational workshop on gynecological brachytherapy: pilot study at a national meeting. Pract Radiat Oncol 9(5):E465–E472
Mesko S et al (2020) Development, implementation, and outcomes of a simulation-based medical education (SBME) prostate brachytherapy workshop for radiation oncology residents. Brachytherapy 19(6):738–745
Thaker NG et al (2014) Establishing high-quality prostate brachytherapy using a phantom simulator training program. Int J Radiat Oncol Biol Phys 90(3):579–586
Frank SJ et al (2020) The American brachytherapy society prostate brachytherapy LDR/HDR simulation workshops: hands-on, step-by-step training in the process of quality assurance. Brachytherapy 19(6):787–793
Correa C et al (2017) Accelerated partial breast irradiation: executive summary for the update of an ASTRO evidence-based consensus statement. Pract Radiat Oncol 7(2):73–79
Polgár C et al (2013) Breast-conserving therapy with partial or whole breast irradiation: ten-year results of the Budapest randomized trial. Radiother Oncol 108(2):197–202
Strnad V et al (2016) 5‑year results of accelerated partial breast irradiation using sole interstitial multicatheter brachytherapy versus whole-breast irradiation with boost after breast-conserving surgery for low-risk invasive and in-situ carcinoma of the female breast: a randomised, phase 3, non-inferiority trial. Lancet 387(10015):229–238
Polgár C et al (2017) Late side-effects and cosmetic results of accelerated partial breast irradiation with interstitial brachytherapy versus whole-breast irradiation after breast-conserving surgery for low-risk invasive and in-situ carcinoma of the female breast: 5‑year results of a randomised, controlled, phase 3 trial. Lancet Oncol 18(2):259–268
Petereit DG et al (2015) Brachytherapy: where has it gone? J Clin Oncol 33(9):980–982
Frobenius W (2021) Nationaler Kompetenzbasierter Lernzielkatalog Medizin (NKLM) Version 2.0
Bundesministerium für Bildung und Forschung (2017) Masterplan Medizinstudium 2020
Ärzteblatt (2019) Medizinische Fakultäten wollen sich bei Neustrukturierung des Medizinstudiums engagieren. Deutscher Ärzteverlag GmbH
Oertel M et al (2019) Successful integration of radiation oncology in preclinical medical education : experiences with an interdisciplinary training project. Strahlenther Onkol 195(12):1104–1109
Winter IP, Ingledew PA, Golden DW (2019) Interprofessional education in radiation oncology. J Am Coll Radiol 16(7):964–971
Patel VL, Yoskowitz NA, Arocha JF (2009) Towards effective evaluation and reform in medical education: a cognitive and learning sciences perspective. Adv Health Sci Educ Theory Pract 14(5):791–812
Sprawls P (2008) Evolving models for medical physics education and training: a global perspective. Biomed Imaging Interv J 4(1):e16
Kamp MA et al (2021) Proposed definition of competencies for surgical neuro-oncology training. J Neurooncol 153(1):121–131
Bi M et al (2019) Comparison of case-based learning and traditional method in teaching postgraduate students of medical oncology. Med Teach 41(10):1124–1128
McGaghie WC et al (2011) Does simulation-based medical education with deliberate practice yield better results than traditional clinical education? A meta-analytic comparative review of the evidence. Acad Med 86(6):706–711
Akaike M et al (2012) Simulation-based medical education in clinical skills laboratory. J Med Invest 59(1):28–35
Cook DA et al (2011) Technology-enhanced simulation for health professions education: a systematic review and meta-analysis. JAMA 306(9):978–988
Griswold-Theodorson S et al (2015) Beyond the simulation laboratory: a realist synthesis review of clinical outcomes of simulation-based mastery learning. Acad Med 90(11):1553–1560
Cook DA et al (2013) Comparative effectiveness of instructional design features in simulation-based education: systematic review and meta-analysis. Med Teach 35(1):e867–98
Jiang G et al (2011) Learning curves and long-term outcome of simulation-based thoracentesis training for medical students. BMC Med Educ 11:39
Dubois N et al (2022) Training of radiotherapy professionals: status, content, satisfaction and improvement suggestions in the greater region. BMC Med Educ 22(1):485
Rooney MK et al (2018) Simulation as more than a treatment-planning tool: a systematic review of the literature on radiation oncology simulation-based medical education. Int J Radiat Oncol Biol Phys 102(2):257–283
Merriam SB (2010) Adult learning. International encyclopedia of education. Elsevier
Stein D (1998) Situated learning in adult education. ERIC Digest 195:1–7
Dapper H et al (2021) Radiation oncology as part of medical education—current status and possible digital future prospects. Strahlenther Onkol 197(6):528–536
Oertel M et al (2022) Digital transfer in radiation oncology education for medical students—single-center data and systemic review of the literature. Strahlenther Onkol 198(9):765–772
Acknowledgements
We would like to thank Varian for the supply of professional products for brachytherapy. We would also like to thank all colleagues of our Department of Radiation Oncology who were involved in teaching or development and preparation of the workshop.
Funding
Matthias Mäurer was funded by the Deutsche Forschungsgemeinschaft (DFG, German Research Foundation) Clinician Scientist Program OrganAge (funding number 413668513) and by the Interdisciplinary Center of Clinical Research of the Medical Faculty Jena. Georg Wurschi receives funding from the Clinician Scientist Program of the Interdisciplinary Center for Clinical Research, Jena University Hospital (grant no.: CSP-11).
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M.A. Mäurer, S. Drozdz, J. Ehrenpfordt, M. Schwedas, M. Friedlein, N. Hille, C. Riede, S. Schrott, M. Graf, G. Wurschi, M.A. Kamp, A. Wittig, and S. Knippen declare that they have no competing interests.
Ethical standards
The present study was performed in accordance with the Declaration of Helsinki and with approval by the institutional review board of the Medical Faculty, Friedrich-Schiller-University (registration number: 2022-2730-Bef).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mäurer, M.A., Drozdz, S., Ehrenpfordt, J. et al. Development, implementation, and results of a simulation-based hands-on brachytherapy workshop for medical students. Strahlenther Onkol 199, 370–378 (2023). https://doi.org/10.1007/s00066-023-02058-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-023-02058-w