Purpose:
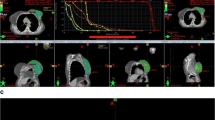
Investigation of the effects of breathing motion- and misregistration-induced errors on the superficial dose in the treatment of breast cancer using helical tomotherapy (HT).
Material and Methods:
Surface dose measurements were performed with thermoluminescence dosimetry (TLD). Two treatment plans with different planning target volume (PTV) definitions of the left breast were used: PTVskin had its ventral border exactly on skin level, while PTVair included also a 10-mm extension ventral to the PTVskin. With a thoracic static phantom, misregistration errors in an HT were simulated. A dynamic phantom was used to simulate a breathing patient during HT. Surface doses of breast cancer patients were measured both for an HT (179 points) and a conventional three-dimensional conformal treatment (70 points).
Results:
In the static phantom misregistration setup, dose deviations of –31.9% for PTVskin to +35.4% for PTVair could be observed. The dynamic phantom measurements resulted in surface dose deviations from those in a static position between 0.8% and 3.8% without a significant difference for the PTV definitions. The measured surface doses on patients averaged (mean ± standard deviation) 1.65 ± 0.13 Gy for the HT and 1.42 ± 0.11 Gy for the three-dimensional conformal treatment.
Conclusion:
HT enables a homogeneous and reproducible surface dose with small dose deviations in the treatment of breast cancer. HT is a feasible method to treat breast cancer under free shallow breathing of the patient using a treatment plan with a ventral PTV border on the skin level.
Ziel:
Untersuchung der Effekte von atembewegungs- und fehlpositionierungsbedingten Störungen auf die Oberflächendosis in der Behandlung des Mammakarzinoms mit helikaler Tomotherapie (HT).
Material und Methodik:
Die Oberflächendosismessungen wurden mit Thermolumineszenzdosimetrie (TLD) durchgeführt. Zwei Bestrahlungspläne mit verschiedenen Planungszielvolumen-(PTV-)Definitionen der linken Brust wurden verwendet: PTVskin hatte seine ventrale Begrenzung exakt auf Hautniveau, während PTVair zusätzlich eine 10-mm-Erweiterung ventral von PTVskin enthielt. Mit einem statischen Thoraxphantom wurden verschiedene Fehlpositionierungen während einer HT simuliert. Ein dynamisches Phantom wurde verwendet, um eine atmende Patientin während einer HT zu simulieren. Die Oberflächendosen von Mammakarzinompatientinnen wurden sowohl bei HT (179 Messpunkte) als auch bei der dreidimensionalen konformalen Radiotherapie (70 Messpunkte) gemessen.
Ergebnisse:
Im Versuch des statischen Phantoms konnten Dosisunterschiede von –31,9% bei PTVskin bis +35,4% bei PTVair beobachtet werden. Die Messungen mit dem dynamischen Phantom ergaben Dosisunterschiede von den Dosen in statischer Position zwischen 0,8% und 3,8% ohne einen signifikanten Unterschied zwischen den PTV-Definitionen. Die gemessenen Oberflächendosen von Patientinnen lagen durchschnittlich bei (Mittelwert ± Standardabweichung) 1,65 ± 0,13 Gy bei HT und 1,42 ± 0,11 Gy bei der dreidimensionalen konformalen Behandlung.
Schlussfolgerung:
HT ermöglicht eine homogene und reproduzierbare Oberflächendosis mit geringen Abweichungen in der Behandlung des Mammakarzinoms. Die HT eignet sich zur Behandlung des Mammakarzinoms unter freier flacher Atmung der Patientin, wenn ein Bestrahlungsplan mit ventraler PTV-Begrenzung auf Hautniveau verwendet wird.
Similar content being viewed by others
References
Bauman G, Yartsev S, Rodrigues G, et al. A prospective evaluation of helical tomotherapy. Int J Radiat Oncol Biol Phys 2007;68:632–41.
Dawson LA, Sharpe MB. Image-guided radiotherapy: rationale, benefits, and limitations. Lancet Oncol 2006;7:848–58.
Ding C, Li X, Huq MS, et al. The effect of respiratory cycle and radiation beam-on timing on the dose distribution of free-breathing breast treatment using dynamic IMRT. Med Phys 2007;34:3500–9.
Fiorino C, Dell’Oca I, Pierelli A, et al. Simultaneous integrated boost (SIB) for nasopharynx cancer with helical tomotherapy. A planning study. Strahlenther Onkol 2007;183:497–505.
Kanagaki B, Read PW, Molloy JA, et al. A motion phantom study on helical tomotherapy: the dosimetric impacts of delivery technique and motion. Phys Med Biol 2007;52:243–55.
Kinoshita R, Shimizu S, Taguchi H, et al. Three-dimensional intrafractional motion of breast during tangential breast irradiation monitored with high-sampling frequency using a real-time tumor-tracking radiotherapy system. Int J Radiat Oncol Biol Phys 2008;70:931–4.
Kissick MW, Fenwick J, James JA, et al. The helical tomotherapy thread effect. Med Phys 2005;32:1414–23.
Kissick MW, Flynn RT, Westerly DC, et al. On the impact of longitudinal breathing motion randomness for tomotherapy delivery. Phys Med Biol 2008;53:4855–73.
Mackie TR, Balog J, Ruchala K, et al. Tomotherapy. Semin Radiat Oncol 1999;9:108–17.
Mackie TR, Holmes T, Swerdloff S, et al. Tomotherapy: a new concept for the delivery of dynamic conformal radiotherapy. Med Phys 1993;20:1709–19.
Moeckly SR, Lamba M, Elson HR. Respiratory motion effects on whole breast helical tomotherapy. Med Phys 2008;35:1464–75.
Mutic S, Low DA. Superficial doses from serial tomotherapy delivery. Med Phys 2000;27:163–5.
Ramsey CR, Seibert RM, Robison B, et al. Helical tomotherapy superficial dose measurements. Med Phys 2007;34:3286–93.
Robertson MA. Characteristics of TLD. In: Robertson MA, ed. Identification and reduction of errors in thermoluminescence dosimetry systems. Weybridge: Pittman, 1981:6–10.
Rochet N, Sterzing F, Jensen A, et al. Helical tomotherapy as a new treatment technique for whole abdominal irradiation. Strahlenther Onkol 2008;184:145–9.
Ruchala KJ, Olivera GH, Schloesser EA, et al. Megavoltage CT on a tomotherapy system. Phys Med Biol 1999;44:2597–621.
Sterzing F, Herfarth K, Debus J. IGRT with helical tomotherapy - effort and benefit in clinical routine. Strahlenther Onkol 2007;183:Special Issue 2:35–7.
Sterzing F, Schubert K, Sroka-Perez G, et al. Helical tomotherapy. Experiences of the first 150 patients in Heidelberg. Strahlenther Onkol 2008;184:8–14.
Thilmann C, Sroka-Perez G, Krempien R, et al. Inversely planned intensity modulated radiotherapy of the breast including the internal mammary chain: a plan comparison study. Technol Cancer Res Treat 2004;3:69–75.
Thilmann C, Zabel A, Milker-Zabel S, et al. Number and orientation of beams in inversely planned intensity-modulated radiotherapy of the female breast and the parasternal lymph nodes. Am J Clin Oncol 2003;26:e136–43.
Thilmann C, Zabel A, Nill S, et al. Intensity-modulated radiotherapy of the female breast. Med Dosim 2002;27:79–90.
Tournel K, Verellen D, Duchateau M, et al. An assessment of the use of skin flashes in helical tomotherapy using phantom and in-vivo dosimetry. Radiother Oncol 2007;84:34–9.
Welsh JS, Patel RR, Ritter MA, et al. Helical tomotherapy: an innovative technology and approach to radiation therapy. Technol Cancer Res Treat 2002;1:311–6.
Yu CX, Jaffray DA, Wong JW. The effects of intra-fraction organ motion on the delivery of dynamic intensity modulation. Phys Med Biol 1998;43:91–104.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zibold, F., Sterzing, F., Sroka-Perez, G. et al. Surface Dose in the Treatment of Breast Cancer with Helical Tomotherapy. Strahlenther Onkol 185, 574–581 (2009). https://doi.org/10.1007/s00066-009-1979-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-009-1979-7